Abstract
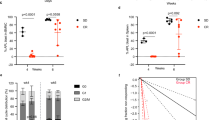
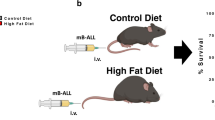
New therapeutic approaches are needed to treat leukemia effectively. Dietary restriction regimens, including fasting, have been considered for the prevention and treatment of certain solid tumor types. However, whether and how dietary restriction affects hematopoietic malignancies is unknown. Here we report that fasting alone robustly inhibits the initiation and reverses the leukemic progression of both B cell and T cell acute lymphoblastic leukemia (B-ALL and T-ALL, respectively), but not acute myeloid leukemia (AML), in mouse models of these tumors. Mechanistically, we found that attenuated leptin-receptor (LEPR) expression is essential for the development and maintenance of ALL, and that fasting inhibits ALL development by upregulation of LEPR and its downstream signaling through the protein PR/SET domain 1 (PRDM1). The expression of LEPR signaling-related genes correlated with the prognosis of pediatric patients with pre-B-ALL, and fasting effectively inhibited B-ALL growth in a human xenograft model. Our results indicate that the effects of fasting on tumor growth are cancer-type dependent, and they suggest new avenues for the development of treatment strategies for leukemia.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Hursting, S.D., Lavigne, J.A., Berrigan, D., Perkins, S.N. & Barrett, J.C. Calorie restriction, aging, and cancer prevention: mechanisms of action and applicability to humans. Annu. Rev. Med. 54, 131–152 (2003).
Fontana, L. & Partridge, L. Promoting health and longevity through diet: from model organisms to humans. Cell 161, 106–118 (2015).
Mihaylova, M.M., Sabatini, D.M. & Yilmaz, O.H. Dietary and metabolic control of stem cell function in physiology and cancer. Cell Stem Cell 14, 292–305 (2014).
Bordone, L. & Guarente, L. Calorie restriction, SIRT1 and metabolism: understanding longevity. Nat. Rev. Mol. Cell Biol. 6, 298–305 (2005).
Longo, V.D. & Mattson, M.P. Fasting: molecular mechanisms and clinical applications. Cell Metab. 19, 181–192 (2014).
Kalaany, N.Y. & Sabatini, D.M. Tumours with PI3K activation are resistant to dietary restriction. Nature 458, 725–731 (2009).
Di Biase, S. et al. Fasting-mimicking diet reduces HO-1 to promote T cell-mediated tumor cytotoxicity. Cancer Cell 30, 136–146 (2016).
Pietrocola, F. et al. Caloric restriction mimetics enhance anticancer immunosurveillance. Cancer Cell 30, 147–160 (2016).
Cheng, C.W. et al. Prolonged fasting reduces IGF-1/PKA to promote hematopoietic-stem-cell-based regeneration and reverse immunosuppression. Cell Stem Cell 14, 810–823 (2014).
Lee, C. et al. Fasting cycles retard growth of tumors and sensitize a range of cancer cell types to chemotherapy. Sci. Transl. Med. 4, 124ra27 (2012).
Döhner, H., Weisdorf, D.J. & Bloomfield, C.D. Acute myeloid leukemia. N. Engl. J. Med. 373, 1136–1152 (2015).
Inaba, H., Greaves, M. & Mullighan, C.G. Acute lymphoblastic leukaemia. Lancet 381, 1943–1955 (2013).
Ntziachristos, P., Lim, J.S., Sage, J. & Aifantis, I. From fly wings to targeted cancer therapies: a centennial for notch signaling. Cancer Cell 25, 318–334 (2014).
Kocabas, F. et al. Meis1 regulates the metabolic phenotype and oxidant defense of hematopoietic stem cells. Blood 120, 4963–4972 (2012).
Simsek, T. et al. The distinct metabolic profile of hematopoietic stem cells reflects their location in a hypoxic niche. Cell Stem Cell 7, 380–390 (2010).
Zheng, J. et al. Inhibitory receptors bind ANGPTLs and support blood stem cells and leukaemia development. Nature 485, 656–660 (2012).
Kang, X. et al. The ITIM-containing receptor LAIR1 is essential for acute myeloid leukaemia development. Nat. Cell Biol. 17, 665–677 (2015).
Park, J., Euhus, D.M. & Scherer, P.E. Paracrine and endocrine effects of adipose tissue on cancer development and progression. Endocr. Rev. 32, 550–570 (2011).
Park, J., Kusminski, C.M., Chua, S.C. & Scherer, P.E. Leptin receptor signaling supports cancer cell metabolism through suppression of mitochondrial respiration in vivo. Am. J. Pathol. 177, 3133–3144 (2010).
Zheng, J. et al. Ex vivo expanded hematopoietic stem cells overcome the MHC barrier in allogeneic transplantation. Cell Stem Cell 9, 119–130 (2011).
Zheng, J. et al. Profilin 1 is essential for retention and metabolism of mouse hematopoietic stem cells in bone marrow. Blood 123, 992–1001 (2014).
Deng, M. et al. A motif in LILRB2 critical for Angptl2 binding and activation. Blood 124, 924–935 (2014).
Sugihara, E. et al. Ink4a and Arf are crucial factors in the determination of the cell of origin and the therapeutic sensitivity of Myc-induced mouse lymphoid tumor. Oncogene 31, 2849–2861 (2012).
Weng, A.P. et al. Activating mutations of NOTCH1 in human T cell acute lymphoblastic leukemia. Science 306, 269–271 (2004).
Krivtsov, A.V. et al. Transformation from committed progenitor to leukaemia stem cell initiated by MLL-AF9. Nature 442, 818–822 (2006).
Somervaille, T.C. & Cleary, M.L. Identification and characterization of leukemia stem cells in murine MLL-AF9 acute myeloid leukemia. Cancer Cell 10, 257–268 (2006).
Yan, M. et al. A previously unidentified alternatively spliced isoform of t(8;21) transcript promotes leukemogenesis. Nat. Med. 12, 945–949 (2006).
Shapiro-Shelef, M. & Calame, K. Regulation of plasma-cell development. Nat. Rev. Immunol. 5, 230–242 (2005).
Shi, W. et al. Transcriptional profiling of mouse B cell terminal differentiation defines a signature for antibody-secreting plasma cells. Nat. Immunol. 16, 663–673 (2015).
Vaisse, C. et al. Leptin activation of Stat3 in the hypothalamus of wild-type and ob/ob mice but not db/db mice. Nat. Genet. 14, 95–97 (1996).
Morris, D.L. & Rui, L. Recent advances in understanding leptin signaling and leptin resistance. Am. J. Physiol. Endocrinol. Metab. 297, E1247–E1259 (2009).
Weigle, D.S. et al. Effect of fasting, refeeding, and dietary fat restriction on plasma leptin levels. J. Clin. Endocrinol. Metab. 82, 561–565 (1997).
Andò, S. & Catalano, S. The multifactorial role of leptin in driving the breast cancer microenvironment. Nat. Rev. Endocrinol. 8, 263–275 (2011).
Khandekar, M.J., Cohen, P. & Spiegelman, B.M. Molecular mechanisms of cancer development in obesity. Nat. Rev. Cancer 11, 886–895 (2011).
Chua, S.C. Jr. et al. Phenotypes of mouse diabetes and rat fatty due to mutations in the OB (leptin) receptor. Science 271, 994–996 (1996).
Chen, H. et al. Evidence that the diabetes gene encodes the leptin receptor: identification of a mutation in the leptin receptor gene in db/db mice. Cell 84, 491–495 (1996).
Coleman, D.L. & Hummel, K.P. The influence of genetic background on the expression of the obese (Ob) gene in the mouse. Diabetologia 9, 287–293 (1973).
Zhang, Y. et al. Positional cloning of the mouse obese gene and its human homologue. Nature 372, 425–432 (1994).
Fantuzzi, G. & Faggioni, R. Leptin in the regulation of immunity, inflammation, and hematopoiesis. J. Leukoc. Biol. 68, 437–446 (2000).
Boi, M., Zucca, E., Inghirami, G. & Bertoni, F. PRDM1/BLIMP1: a tumor suppressor gene in B and T cell lymphomas. Leuk. Lymphoma 56, 1223–1228 (2015).
Hangaishi, A. & Kurokawa, M. Blimp-1 is a tumor suppressor gene in lymphoid malignancies. Int. J. Hematol. 91, 46–53 (2010).
Ross, J.A. et al. Genetic variation in the leptin receptor gene and obesity in survivors of childhood acute lymphoblastic leukemia: a report from the Childhood Cancer Survivor Study. J. Clin. Oncol. 22, 3558–3562 (2004).
Wheeler, E. et al. Genome-wide SNP and CNV analysis identifies common and low-frequency variants associated with severe early-onset obesity. Nat. Genet. 45, 513–517 (2013).
Vishalakshi, N. et al. A comprehensive curated reaction map of leptin Signaling Pathway. J. Proteomics Bioinform. 4, 184–189 (2011).
Teras, L.R. et al. in Energy Balance and Hematologic Malignancies Vol. 5 1st edn. (eds. Mittelman, S.D. & Berger, N.A.) 1–69 (Springer, New York, 2012).
Sheng, X. & Mittelman, S.D. The role of adipose tissue and obesity in causing treatment resistance of acute lymphoblastic leukemia. Front Pediatr. 2, 53 (2014).
Bifulco, M. & Malfitano, A.M. Comment on “the negative impact of being underweight and weight loss on survival of children with acute lymphoblastic leukemia.”. Haematologica 100, e118–e119 (2015).
Butturini, A.M. et al. Obesity and outcome in pediatric acute lymphoblastic leukemia. J. Clin. Oncol. 25, 2063–2069 (2007).
Oeffinger, K.C. et al. Obesity in adult survivors of childhood acute lymphoblastic leukemia: a report from the Childhood Cancer Survivor Study. J. Clin. Oncol. 21, 1359–1365 (2003).
Yun, J.P. et al. Diet-induced obesity accelerates acute lymphoblastic leukemia progression in two murine models. Cancer Prev. Res. (Phila.) 3, 1259–1264 (2010).
Myers, M.G. Jr., Leibel, R.L., Seeley, R.J. & Schwartz, M.W. Obesity and leptin resistance: distinguishing cause from effect. Trends Endocrinol. Metab. 21, 643–651 (2010).
Pramanik, R., Sheng, X., Ichihara, B., Heisterkamp, N. & Mittelman, S.D. Adipose tissue attracts and protects acute lymphoblastic leukemia cells from chemotherapy. Leuk. Res. 37, 503–509 (2013).
Baskin, D.G. et al. Increased expression of mRNA for the long form of the leptin receptor in the hypothalamus is associated with leptin hypersensitivity and fasting. Diabetes 47, 538–543 (1998).
Weng, A.P. et al. c-Myc is an important direct target of Notch1 in T-cell acute lymphoblastic leukemia/lymphoma. Genes Dev. 20, 2096–2109 (2006).
Nowak, D., Stewart, D. & Koeffler, H.P. Differentiation therapy of leukemia: 3 decades of development. Blood 113, 3655–3665 (2009).
Efficace, F. et al. Randomized phase III trial of retinoic acid and arsenic trioxide versus retinoic acid and chemotherapy in patients with acute promyelocytic leukemia: health-related quality-of-life outcomes. J. Clin. Oncol. 32, 3406–3412 (2014).
Lo-Coco, F. et al. Retinoic acid and arsenic trioxide for acute promyelocytic leukemia. N. Engl. J. Med. 369, 111–121 (2013).
Hurwitz, R. et al. Characterization of a leukemic cell line of the pre-B phenotype. Intl. J. Cancer. Journal international du cancer 23, 174–180 (1979).
Filshie, R., Gottlieb, D. & Bradstock, K. VLA-4 is involved in the engraftment of the human pre-B acute lymphoblastic leukaemia cell line NALM-6 in SCID mice. Br. J. Haematol. 102, 1292–1300 (1998).
Zhang, C.C., Kaba, M., Iizuka, S., Huynh, H. & Lodish, H.F. Angiopoietin-like 5 and IGFBP2 stimulate ex vivo expansion of human cord blood hematopoietic stem cells as assayed by NOD/SCID transplantation. Blood 111, 3415–3423 (2008).
Rocke, D.M. & Durbin, B. A model for measurement error for gene expression arrays. J. Comput. Biol. 8, 557–569 (2001).
Dozmorov, I. & Centola, M. An associative analysis of gene expression array data. Bioinformatics 19, 204–211 (2003).
Dozmorov, I. & Lefkovits, I. Internal standard-based analysis of microarray data. Part 1: analysis of differential gene expressions. Nucleic Acids Res. 37, 6323–6339 (2009).
Kamburov, A., Stelzl, U., Lehrach, H. & Herwig, R. The ConsensusPathDB interaction database: 2013 update. Nucleic Acids Res. 41, D793–D800 (2013).
Krämer, A., Green, J., Pollard, J. Jr. & Tugendreich, S. Causal analysis approaches in Ingenuity Pathway Analysis. Bioinformatics 30, 523–530 (2014).
Acknowledgements
We would like to acknowledge the support by grants from the US National Institutes of Health 1R01CA172268 (C.C.Z.), Leukemia & Lymphoma Society Awards 1024-14 (C.C.Z.) and TRP-6024-14 (C.C.Z.), CPRIT RP140402 (C.C.Z.), 1R01HL089966 (L.J.H.), R01-DK55758 (P.E.S.) and RP140412 (P.E.S.).
Author information
Authors and Affiliations
Contributions
C.C.Z. and Z.L. designed experiments. C.C.Z. conceived the study. Z.L., J.X., G.W., J.S. and P.E.S. performed experiments and interpreted data. L.J.-S.H., X.K., Y.Z. and M.L. performed experiments. Z.L. and J.X. performed statistical analysis. R.C., W.C., J.F.A., T.S. and N.W. provided patient samples. The manuscript was written by C.C.Z. and Z.L. and contributed to by all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–19 and Supplementary Tables 1–6 (PDF 23156 kb)
Rights and permissions
About this article
Cite this article
Lu, Z., Xie, J., Wu, G. et al. Fasting selectively blocks development of acute lymphoblastic leukemia via leptin-receptor upregulation. Nat Med 23, 79–90 (2017). https://doi.org/10.1038/nm.4252
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4252
This article is cited by
-
Caloric restriction leads to druggable LSD1-dependent cancer stem cells expansion
Nature Communications (2024)
-
Disruption to the FOXO-PRDM1 axis resulting from deletions of chromosome 6 in acute lymphoblastic leukaemia
Leukemia (2023)
-
Gut microbiome immaturity and childhood acute lymphoblastic leukaemia
Nature Reviews Cancer (2023)
-
Bone Marrow Adipose Tissue: Regulation of Osteoblastic Niche, Hematopoiesis and Hematological Malignancies
Stem Cell Reviews and Reports (2023)
-
Obesity and Leukemia: Biological Mechanisms, Perspectives, and Challenges
Current Obesity Reports (2023)