Abstract
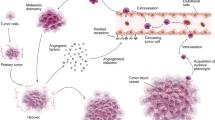
The efficacy of angiogenesis inhibitors in cancer is limited by resistance mechanisms that are poorly understood. Notably, instead of through the induction of angiogenesis, tumor vascularization can occur through the nonangiogenic mechanism of vessel co-option. Here we show that vessel co-option is associated with a poor response to the anti-angiogenic agent bevacizumab in patients with colorectal cancer liver metastases. Moreover, we find that vessel co-option is also prevalent in human breast cancer liver metastases, a setting in which results with anti-angiogenic therapy have been disappointing. In preclinical mechanistic studies, we found that cancer cell motility mediated by the actin-related protein 2/3 complex (Arp2/3) is required for vessel co-option in liver metastases in vivo and that, in this setting, combined inhibition of angiogenesis and vessel co-option is more effective than the inhibition of angiogenesis alone. Vessel co-option is therefore a clinically relevant mechanism of resistance to anti-angiogenic therapy and combined inhibition of angiogenesis and vessel co-option might be a warranted therapeutic strategy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Ferrara, N., Hillan, K.J., Gerber, H.P. & Novotny, W. Discovery and development of bevacizumab, an anti-VEGF antibody for treating cancer. Nat. Rev. Drug Discov. 3, 391–400 (2004).
Kerbel, R.S. Tumor angiogenesis. N. Engl. J. Med. 358, 2039–2049 (2008).
Hurwitz, H. et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N. Engl. J. Med. 350, 2335–2342 (2004).
Cunningham, D. et al. Bevacizumab plus capecitabine versus capecitabine alone in elderly patients with previously untreated metastatic colorectal cancer (AVEX): an open-label, randomised phase 3 trial. Lancet Oncol. 14, 1077–1085 (2013).
Ebos, J.M. & Kerbel, R.S. Antiangiogenic therapy: impact on invasion, disease progression, and metastasis. Nat. Rev. Clin. Oncol. 8, 210–221 (2011).
Vasudev, N.S. & Reynolds, A.R. Anti-angiogenic therapy for cancer: current progress, unresolved questions and future directions. Angiogenesis 17, 471–494 (2014).
Pezzella, F. et al. Angiogenesis in primary lung cancer and lung secondaries. Eur. J. Cancer 32A, 2494–2500 (1996).
Vermeulen, P.B. et al. Liver metastases from colorectal adenocarcinomas grow in three patterns with different angiogenesis and desmoplasia. J. Pathol. 195, 336–342 (2001).
Döme, B., Hendrix, M.J., Paku, S., Tóvári, J. & Tímár, J. Alternative vascularization mechanisms in cancer: Pathology and therapeutic implications. Am. J. Pathol. 170, 1–15 (2007).
Donnem, T. et al. Vessel co-option in primary human tumors and metastases: an obstacle to effective anti-angiogenic treatment? Cancer Med. 2, 427–436 (2013).
Jayson, G.C., Kerbel, R., Ellis, L.M. & Harris, A.L. Antiangiogenic therapy in oncology: current status and future directions. Lancet 388, 518–529 (2016).
Adams, R.B. et al. Selection for hepatic resection of colorectal liver metastases: expert consensus statement. HPB (Oxford) 15, 91–103 (2013).
Van den Eynden, G.G. et al. The multifaceted role of the microenvironment in liver metastasis: biology and clinical implications. Cancer Res. 73, 2031–2043 (2013).
Stessels, F. et al. Breast adenocarcinoma liver metastases, in contrast to colorectal cancer liver metastases, display a non-angiogenic growth pattern that preserves the stroma and lacks hypoxia. Br. J. Cancer 90, 1429–1436 (2004).
Gruenberger, B. et al. Bevacizumab, capecitabine, and oxaliplatin as neoadjuvant therapy for patients with potentially curable metastatic colorectal cancer. J. Clin. Oncol. 26, 1830–1835 (2008).
Chaudhury, P. et al. Perioperative chemotherapy with bevacizumab and liver resection for colorectal cancer liver metastasis. HPB 12, 37–42 (2010).
Wong, R. et al. A multicentre study of capecitabine, oxaliplatin plus bevacizumab as perioperative treatment of patients with poor-risk colorectal liver-only metastases not selected for upfront resection. Ann. Oncol. 22, 2042–2048 (2011).
Chun, Y.S. et al. Association of computed tomography morphologic criteria with pathologic response and survival in patients treated with bevacizumab for colorectal liver metastases. J. Am. Med. Assoc. 302, 2338–2344 (2009).
Shindoh, J. et al. Optimal morphologic response to preoperative chemotherapy: an alternate outcome end point before resection of hepatic colorectal metastases. J. Clin. Oncol. 30, 4566–4572 (2012).
Boonsirikamchai, P. et al. CT findings of response and recurrence, independent of change in tumor size, in colorectal liver metastasis treated with bevacizumab. AJR Am. J. Roentgenol. 197, W1060–W1066 (2011).
Van den Eynden, G.G. et al. The histological growth pattern of colorectal cancer liver metastases has prognostic value. Clin. Exp. Metastasis 29, 541–549 (2012).
Nürnberg, A., Kitzing, T. & Grosse, R. Nucleating actin for invasion. Nat. Rev. Cancer 11, 177–187 (2011).
Otsubo, T. et al. Involvement of Arp2/3 complex in the process of colorectal carcinogenesis. Mod. Pathol. 17, 461–467 (2004).
Iwaya, K. et al. Correlation between liver metastasis of the colocalization of actin-related protein 2 and 3 complex and WAVE2 in colorectal carcinoma. Cancer Sci. 98, 992–999 (2007).
Kopetz, S. et al. Synergistic activity of the SRC family kinase inhibitor dasatinib and oxaliplatin in colon carcinoma cells is mediated by oxidative stress. Cancer Res. 69, 3842–3849 (2009).
Nyati, M.K. et al. The potential of 5-fluorocytosine/cytosine deaminase enzyme prodrug gene therapy in an intrahepatic colon cancer model. Gene Ther. 9, 844–849 (2002).
Gray, M.J. et al. Therapeutic targeting of Id2 reduces growth of human colorectal carcinoma in the murine liver. Oncogene 27, 7192–7200 (2008).
Liang, W.C. et al. Cross-species vascular endothelial growth factor (VEGF)-blocking antibodies completely inhibit the growth of human tumor xenografts and measure the contribution of stromal VEGF. J. Biol. Chem. 281, 951–961 (2006).
Miller, K.D. et al. Randomized phase III trial of capecitabine compared with bevacizumab plus capecitabine in patients with previously treated metastatic breast cancer. J. Clin. Oncol. 23, 792–799 (2005).
Miller, K. et al. Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N. Engl. J. Med. 357, 2666–2676 (2007).
Miles, D.W. et al. Phase III study of bevacizumab plus docetaxel compared with placebo plus docetaxel for the first-line treatment of human epidermal growth factor receptor 2-negative metastatic breast cancer. J. Clin. Oncol. 28, 3239–3247 (2010).
Robert, N.J. et al. RIBBON-1: randomized, double-blind, placebo-controlled, phase III trial of chemotherapy with or without bevacizumab for first-line treatment of human epidermal growth factor receptor 2-negative, locally recurrent or metastatic breast cancer. J. Clin. Oncol. 29, 1252–1260 (2011).
Brufsky, A.M. et al. RIBBON-2: a randomized, double-blind, placebo-controlled, phase III trial evaluating the efficacy and safety of bevacizumab in combination with chemotherapy for second-line treatment of human epidermal growth factor receptor 2-negative metastatic breast cancer. J. Clin. Oncol. 29, 4286–4293 (2011).
Naresh, K.N., Nerurkar, A.Y. & Borges, A.M. Angiogenesis is redundant for tumour growth in lymph node metastases. Histopathology 38, 466–470 (2001).
Jeong, H.S. et al. Investigation of the lack of angiogenesis in the formation of lymph node metastases. J. Natl. Cancer Inst. 107, djv155 (2015).
Colpaert, C.G. et al. Cutaneous breast cancer deposits show distinct growth patterns with different degrees of angiogenesis, hypoxia and fibrin deposition. Histopathology 42, 530–540 (2003).
Breast Cancer Progression Working Party. Evidence for novel nonangiogenic pathway in breast-cancer metastasis. Lancet 355, 1787–1788 (2000).
Szabo, V. et al. Mechanism of tumour vascularization in experimental lung metastases. J. Pathol. 235, 384–396 (2015).
Carbonell, W.S., Ansorge, O., Sibson, N. & Muschel, R. The vascular basement membrane as “soil” in brain metastasis. PLoS One 4, e5857 (2009).
Bugyik, E. et al. Lack of angiogenesis in experimental brain metastases. J. Neuropathol. Exp. Neurol. 70, 979–991 (2011).
Valiente, M. et al. Serpins promote cancer cell survival and vascular co-option in brain metastasis. Cell 156, 1002–1016 (2014).
Jain, R.K. et al. Biomarkers of response and resistance to antiangiogenic therapy. Nat. Rev. Clin. Oncol. 6, 327–338 (2009).
Semelka, R.C., Hussain, S.M., Marcos, H.B. & Woosley, J.T. Perilesional enhancement of hepatic metastases: correlation between MR imaging and histopathologic findings-initial observations. Radiology 215, 89–94 (2000).
Kuczynski, E.A. et al. Co-option of liver vessels and not sprouting angiogenesis drives acquired sorafenib resistance in hepatocellular carcinoma. J. Natl. Cancer Inst. 108, djw030 (2016).
Rubenstein, J.L. et al. Anti-VEGF antibody treatment of glioblastoma prolongs survival but results in increased vascular cooption. Neoplasia 2, 306–314 (2000).
Küsters, B. et al. Vascular endothelial growth factor-A(165) induces progression of melanoma brain metastases without induction of sprouting angiogenesis. Cancer Res. 62, 341–345 (2002).
Leenders, W.P. et al. Antiangiogenic therapy of cerebral melanoma metastases results in sustained tumor progression via vessel co-option. Clin. Cancer Res. 10, 6222–6230 (2004).
Pàez-Ribes, M. et al. Antiangiogenic therapy elicits malignant progression of tumors to increased local invasion and distant metastasis. Cancer Cell 15, 220–231 (2009).
de Groot, J.F. et al. Tumor invasion after treatment of glioblastoma with bevacizumab: radiographic and pathologic correlation in humans and mice. Neuro-oncol. 12, 233–242 (2010).
Lu, K.V. et al. VEGF inhibits tumor cell invasion and mesenchymal transition through a MET/VEGFR2 complex. Cancer Cell 22, 21–35 (2012).
Sennino, B. et al. Suppression of tumor invasion and metastasis by concurrent inhibition of c-Met and VEGF signaling in pancreatic neuroendocrine tumors. Cancer Discov. 2, 270–287 (2012).
Depner, C. et al. EphrinB2 repression through ZEB2 mediates tumour invasion and anti-angiogenic resistance. Nat. Commun. 7, 12329 (2016).
Bland, J.M. & Altman, D.G. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1, 307–310 (1986).
Ribero, D. et al. Bevacizumab improves pathologic response and protects against hepatic injury in patients treated with oxaliplatin-based chemotherapy for colorectal liver metastases. Cancer 110, 2761–2767 (2007).
Chang, H.H., Leeper, W.R., Chan, G., Quan, D. & Driman, D.K. Infarct-like necrosis: a distinct form of necrosis seen in colorectal carcinoma liver metastases treated with perioperative chemotherapy. Am. J. Surg. Pathol. 36, 570–576 (2012).
Goldhirsch, A. et al. Personalizing the treatment of women with early breast cancer: highlights of the St Gallen International Expert Consensus on the Primary Therapy of Early Breast Cancer 2013. Ann. Oncol. 24, 2206–2223 (2013).
Hammond, M.E. et al. American Society of Clinical Oncology/College of American Pathologists guideline recommendations for immunohistochemical testing of estrogen and progesterone receptors in breast cancer (unabridged version). Arch. Pathol. Lab. Med. 134, e48–e72 (2010).
Wolff, A.C. et al. Recommendations for human epidermal growth factor receptor 2 testing in breast cancer: American Society of Clinical Oncology/College of American Pathologists clinical practice guideline update. J. Clin. Oncol. 31, 3997–4013 (2013).
Gourlaouen, M., Welti, J.C., Vasudev, N.S. & Reynolds, A.R. Essential role for endocytosis in the growth factor-stimulated activation of ERK1/2 in endothelial cells. J. Biol. Chem. 288, 7467–7480 (2013).
Grambsch, P.M. & Therneau, T.M. Proportional hazards tests and diagnostics based on weighted residuals. Biometrika 81, 515–526 (1994).
Acknowledgements
The study was supported by Breakthrough Breast Cancer (which recently merged with the Breast Cancer Campaign to form Breast Cancer Now), NHS funding to the NIHR Biomedical Research Centre at RM/ICR (London), the Liver Disease Biobank (Montreal) and De Stichting tegen Kanker (Antwerp). We thank I. Hart, K. Hodivala-Dilke, C. Isacke, R. Kerbel, A. Tutt and the members of the Liver Metastasis Research Network for their critical comments on the work. We thank Genentech for providing B20-4.1.1, S. Petrillo for assistance with the Liver Disease Biobank, J. Campbell for advice on statistical analysis and M. Balazsi for assistance with digital pathology. For their technical assistance, we thank the staff of the ICR Biological Services Unit and the staff of the Breast Cancer Now Histopathology Core Facility.
Author information
Authors and Affiliations
Contributions
S. Frentzas, E.S., V.L.B., P.B.V. and S. Foo performed experiments, collected data, analysed data, provided input on the study design and assisted with interpretation of the data; P.B.V., A.W., Z.G., Y.S. and G.V.D.E. performed histopathological analysis of tissue specimens; E.K., M.R.N., F.D., P.G., T.J.B. and Z.E. provided essential technical assistance with experiments; C.P. and X.T. performed statistical analysis on clinical data; A.S. and A.L. assisted with the retrieval of tissue specimens and the associated clinical data; L.R., J.V.R. and S.V.L. shared unpublished data that were crucial to the successful execution of the study and provided critical comments on the manuscript; A.K., G.B., E.L., H.N. and M.S. provided expert assistance with the analysis of clinical data and critical comments on the manuscript; L.D., D.C. and P.M. provided tissue specimens for the study and critical comments on the design of the study and the writing of the manuscript; A.R.R. conceived of and designed the study, supervised the research and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text, Figures and Tables
Supplementary Figures 1–17 and Supplementary Tables 1–13 (PDF 4133 kb)
Rights and permissions
About this article
Cite this article
Frentzas, S., Simoneau, E., Bridgeman, V. et al. Vessel co-option mediates resistance to anti-angiogenic therapy in liver metastases. Nat Med 22, 1294–1302 (2016). https://doi.org/10.1038/nm.4197
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4197
This article is cited by
-
Role of stromal PD-L1 expression in colorectal liver metastasis
BMC Cancer (2024)
-
Molecular differences of angiogenic versus vessel co-opting colorectal cancer liver metastases at single-cell resolution
Molecular Cancer (2023)
-
What’s in a name? Refining the nomenclature of liver metastases growth patterns by changing “desmoplastic” to “encapsulated”
BJC Reports (2023)
-
Angiogenic signaling pathways and anti-angiogenic therapy for cancer
Signal Transduction and Targeted Therapy (2023)
-
Targeting angiogenesis in oncology, ophthalmology and beyond
Nature Reviews Drug Discovery (2023)