Abstract
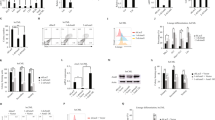
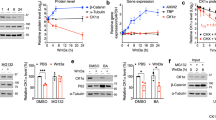
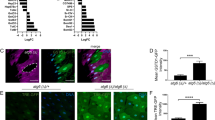
AIRAPL (arsenite-inducible RNA-associated protein-like) is an evolutionarily conserved regulator of cellular proteostasis linked to longevity in nematodes, but its biological function in mammals is unknown1,2,3. We show herein that AIRAPL-deficient mice develop a fully-penetrant myeloproliferative neoplastic process. Proteomic analysis of AIRAPL-deficient mice revealed that this protein exerts its antineoplastic function through the regulation of the insulin/insulin-like growth factor 1 (IGF-1) signaling pathway. We demonstrate that AIRAPL interacts with newly synthesized insulin-related growth factor-1 receptor (IGF1R) polypeptides, promoting their ubiquitination and proteasome-mediated degradation. Accordingly, genetic and pharmacological IGF1R inhibitory strategies prevent the hematological disease found in AIRAPL-deficient mice as well as that in mice carrying the Jak2V617F mutation, thereby demonstrating the causal involvement of this pathway in the pathogenesis of myeloproliferative neoplasms4,5,6. Consistent with its proposed role as a tumor suppressor of myeloid transformation, AIRAPL expression is widely abrogated in human myeloproliferative disorders. Collectively, these findings support the oncogenic relevance of proteostasis deregulation in hematopoietic cells, and they unveil novel therapeutic targets for these frequent hematological neoplasias.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Yun, C. et al. Proteasomal adaptation to environmental stress links resistance to proteotoxicity with longevity in Caenorhabditis elegans. Proc. Natl. Acad. Sci. USA 105, 7094–7099 (2008).
Hassan, W.M., Merin, D.A., Fonte, V. & Link, C.D. AIP-1 ameliorates β-amyloid peptide toxicity in a Caenorhabditis elegans Alzheimer's disease model. Hum. Mol. Genet. 18, 2739–2747 (2009).
Ferguson, A.A., Springer, M.G. & Fisher, A.L. skn-1–dependent and –independent regulation of aip-1 expression following metabolic stress in Caenorhabditis elegans. Mol. Cell. Biol. 30, 2651–2667 (2010).
Levine, R.L. & Gilliland, D.G. Myeloproliferative disorders. Blood 112, 2190–2198 (2008).
Campbell, P.J. & Green, A.R. The myeloproliferative disorders. N. Engl. J. Med. 355, 2452–2466 (2006).
Tefferi, A. & Vainchenker, W. Myeloproliferative neoplasms: molecular pathophysiology, essential clinical understanding and treatment strategies. J. Clin. Oncol. 29, 573–582 (2011).
Balch, W.E., Morimoto, R.I., Dillin, A. & Kelly, J.W. Adapting proteostasis for disease intervention. Science 319, 916–919 (2008).
Hartl, F.U., Bracher, A. & Hayer-Hartl, M. Molecular chaperones in protein folding and proteostasis. Nature 475, 324–332 (2011).
Vembar, S.S. & Brodsky, J.L. One step at a time: endoplasmic reticulum–associated degradation. Nat. Rev. Mol. Cell Biol. 9, 944–957 (2008).
Walter, P. & Ron, D. The unfolded protein response: from stress pathway to homeostatic regulation. Science 334, 1081–1086 (2011).
López-Otín, C., Blasco, M.A., Partridge, L., Serrano, M. & Kroemer, G. The hallmarks of aging. Cell 153, 1194–1217 (2013).
Hanahan, D. & Weinberg, R.A. Hallmarks of cancer: the next generation. Cell 144, 646–674 (2011).
Skarnes, W.C. et al. A conditional knockout resource for the genome-wide study of mouse gene function. Nature 474, 337–342 (2011).
Zhou, T., Kinney, M.C., Scott, L.M., Zinkel, S.S. & Rebel, V.I. Revisiting the case for genetically engineered mouse models in human myelodysplastic syndrome research. Blood 126, 1057–1068 (2015).
Kiel, M.J. et al. SLAM family receptors distinguish hematopoietic stem and progenitor cells and reveal endothelial niches for stem cells. Cell 121, 1109–1121 (2005).
Yildirim, E. et al. Xist RNA is a potent suppressor of hematologic cancer in mice. Cell 152, 727–742 (2013).
Nangalia, J. et al. Somatic CALR mutations in myeloproliferative neoplasms with nonmutated JAK2. N. Engl. J. Med. 369, 2391–2405 (2013).
Klampfl, T. et al. Somatic mutations of calreticulin in myeloproliferative neoplasms. N. Engl. J. Med. 369, 2379–2390 (2013).
Levine, R.L. et al. Activating mutation in the tyrosine kinase JAK2 in polycythemia vera, essential thrombocythemia and myeloid metaplasia with myelofibrosis. Cancer Cell 7, 387–397 (2005).
James, C. et al. A unique clonal JAK2 mutation leading to constitutive signaling causes polycythaemia vera. Nature 434, 1144–1148 (2005).
Baxter, E.J. et al. Acquired mutation of the tyrosine kinase JAK2 in human myeloproliferative disorders. Lancet 365, 1054–1061 (2005).
Renehan, A.G. et al. Insulin-like growth factor (IGF)-I, IGF-binding protein 3 and cancer risk: systematic review and meta-regression analysis. Lancet 363, 1346–1353 (2004).
Pollak, M. Insulin and insulin-like growth factor signaling in neoplasia. Nat. Rev. Cancer 8, 915–928 (2008).
Gallagher, E.J. & LeRoith, D. Minireview: IGF, insulin and cancer. Endocrinology 152, 2546–2551 (2011).
Glinka, T. et al. Signal peptide–mediated translocation is regulated by a p97-AIRAPL complex. Biochem. J. 457, 253–261 (2014).
Kang, S.W. et al. Substrate-specific translocational attenuation during ER stress defines a pre-emptive quality control pathway. Cell 127, 999–1013 (2006).
Khatib, A.M. et al. Inhibition of proprotein convertases is associated with loss of growth and tumorigenicity of HT-29 human colon carcinoma cells: importance of insulin-like growth factor 1 (IGF-1) receptor processing in IGF-1–mediated functions. J. Biol. Chem. 276, 30686–30693 (2001).
Holzenberger, M. et al. IGF-1 receptor regulates lifespan and resistance to oxidative stress in mice. Nature 421, 182–187 (2003).
García-Echeverría, C. et al. In vivo antitumor activity of NVP-AEW541–a novel, potent and selective inhibitor of the IGF-IR kinase. Cancer Cell 5, 231–239 (2004).
Li, J. et al. JAK2V617F homozygosity drives a phenotypic switch in myeloproliferative neoplasms but is insufficient to sustain disease. Blood 123, 3139–3151 (2014).
Pérez, C. et al. Aberrant DNA methylation profile of chronic and transformed classic Philadelphia-negative myeloproliferative neoplasms. Haematologica 98, 1414–1420 (2013).
Guo, S. et al. Complex oncogene dependence in microRNA-125a–induced myeloproliferative neoplasms. Proc. Natl. Acad. Sci. USA 109, 16636–16641 (2012).
Inoue, D. et al. Myelodysplastic syndromes are induced by histone methylation–altering ASXL1 mutations. J. Clin. Invest. 123, 4627–4640 (2013).
Braunstein, I., Zach, L., Allan, S., Kalies, K.U. & Stanhill, A. Proteasomal degradation of preemptive quality control (pQC) substrates is mediated by an AIRAPL-p97 complex. Mol. Biol. Cell 26, 3719–3727 (2015).
Lovly, C.M. et al. Rationale for cotargeting IGF-1R and ALK in ALK fusion–positive lung cancer. Nat. Med. 20, 1027–1034 (2014).
Meyer, S.C. et al. CHZ868, a type II JAK2 inhibitor, reverses type I JAK inhibitor persistence and demonstrates efficacy in myeloproliferative neoplasms. Cancer Cell 28, 15–28 (2015).
Liu, P., Jenkins, N.A. & Copeland, N.G. A highly efficient recombineering-based method for generating conditional knockout mutations. Genome Res. 13, 476–484 (2003).
Li, J. et al. JAK2V617F impairs hematopoietic stem cell function in a conditional knock-in mouse model of JAK2V617F-positive essential thrombocythemia. Blood 116, 1528–1538 (2010).
Porta-de-la-Riva, M., Fontrodona, L., Villanueva, A. & Cerón, J. Basic Caenorhabditis elegans methods: synchronization and observation. J. Vis. Exp. 64, e4019 (2012).
Rual, J.F. et al. Toward improving Caenorhabditis elegans phenome mapping with an ORFeome-based RNAi library. Genome Res. 14 10B, 2162–2168 (2004).
Kamath, R.S. & Ahringer, J. Genome-wide RNAi screening in Caenorhabditis elegans. Methods 30, 313–321 (2003).
Wernig, G. et al. Expression of Jak2V617F causes a polycythemia vera–like disease with associated myelofibrosis in a murine bone marrow transplant model. Blood 107, 4274–4281 (2006).
Rybak, A. et al. A feedback loop comprising lin-28 and let-7 controls pre-let-7 maturation during neural stem-cell commitment. Nat. Cell Biol. 10, 987–993 (2008).
Scott, L.M. et al. JAK2 exon 12 mutations in polycythemia vera and idiopathic erythrocytosis. N. Engl. J. Med. 356, 459–468 (2007).
Villarroya-Beltri, C. et al. Sumoylated hnRNPA2B1 controls the sorting of miRNAs into exosomes through binding to specific motifs. Nat. Commun. 4, 2980 (2013).
Soria-Valles, C. et al. NF-κB activation impairs somatic cell reprogramming in aging. Nat. Cell Biol. 17, 1004–1013 (2015).
Puente, X.S. et al. Noncoding recurrent mutations in chronic lymphocytic leukemia. Nature 526, 519–524 (2015).
Mullally, A. et al. Depletion of Jak2V617F myeloproliferative neoplasm–propagating stem cells by interferon-α in a murine model of polycythemia vera. Blood 121, 3692–3702 (2013).
Norfo, R. et al. miRNA-mRNA integrative analysis in primary myelofibrosis CD34+ cells: role of miR-155–JARID2 axis in abnormal megakaryopoiesis. Blood 124, e21–e32 (2014).
Acknowledgements
We thank A.A. Ferrando, D.A. Puente, A.R. Folgueras, G.R. Ordoñez, I. Martín-Subero, A. Gutiérrez-Fernández, G. Mariño and E. Luño for advice. We also thank S. Jeay (Novartis Pharma AG, Basel Area, Switzerland; NVP-AEW541), M. Holzenberger (Faculté de médecine Pierre et Marie Curie, Paris; Igf1r-haploinsuficient mice), M.J. Muñoz Ruiz (Universidad Pablo de Olavide, Sevilla; GM6 C. elegans strain) and F.G. Wulczyn (Universitätsmedizin Berlin, Berlin; miR-125a sponge) for providing reagents. We thank A. Moyano and R. Feijoo for excellent technical assistance, and the Servicio de Histopatología (IUOPA) for histological studies. This work was supported by grants from Ministerio de Economía y Competitividad (C.L.-O.), Instituto de Salud Carlos III (RTICC) (C.L.-O.), and Principado de Asturias, Spain (J.M.P.F). We also thank the generous support by J.I. Cabrera, A.I. Campos and M. Secades. The Instituto Universitario de Oncología is supported by Fundación Bancaria Caja de Ahorros de Asturias. C.L.-O. is an Investigator of the Botin Foundation supported by Banco Santander through its Santander Universities Global Division. Work in the Green laboratory is supported by Bloodwise (grant ref. 13003), the Wellcome Trust (grant ref. 104710/Z/14/Z), the Medical Research Council, the Kay Kendall Leukaemia Fund, the Cambridge National Institute for Health Research Biomedical Research Center, the Cambridge Experimental Cancer Medicine Centre, the Leukemia and Lymphoma Society of America (grant ref. 07037), and a core support grant from the Wellcome Trust and the Medical Research Council to the Wellcome Trust-Medical Research Council Cambridge Stem Cell Institute.
Author information
Authors and Affiliations
Contributions
F.G.O. performed experimental work, data interpretation and preparation of the manuscript. C.S.-V., O.S.-F., T.B., M.M., E.C., F.R., E.B.-K., J.V., M.P.d.-l.R., J.C. and A.F. performed experimental work. J.L. and A.R.G. provided critical materials and participated in the preparation of the manuscript. J.M.P.F. and C.L.-O. supervised research and project planning, data interpretation and preparation of the manuscript. All authors discussed the results and implications and commented on the manuscript at all stages.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–13 and Supplementary Tables 1 and 2 (PDF 4843 kb)
Rights and permissions
About this article
Cite this article
Osorio, F., Soria-Valles, C., Santiago-Fernández, O. et al. Loss of the proteostasis factor AIRAPL causes myeloid transformation by deregulating IGF-1 signaling. Nat Med 22, 91–96 (2016). https://doi.org/10.1038/nm.4013
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4013
This article is cited by
-
The genome of a vestimentiferan tubeworm (Ridgeia piscesae) provides insights into its adaptation to a deep-sea environment
BMC Genomics (2023)
-
The role of RNF149 in the pre-emptive quality control substrate ubiquitination
Communications Biology (2023)
-
Hypoxic TAM-derived exosomal miR-155-5p promotes RCC progression through HuR-dependent IGF1R/AKT/PI3K pathway
Cell Death Discovery (2021)
-
AN1-type zinc finger protein 3 (ZFAND3) is a transcriptional regulator that drives Glioblastoma invasion
Nature Communications (2020)
-
NT157 has antineoplastic effects and inhibits IRS1/2 and STAT3/5 in JAK2V617F-positive myeloproliferative neoplasm cells
Signal Transduction and Targeted Therapy (2020)