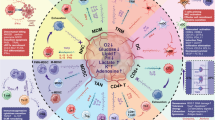
Abstract
Tumor recurrence represents a major clinical challenge. Our data show that emergent recurrent tumors acquire a phenotype radically different from that of their originating primary tumors. This phenotype allows them to evade a host-derived innate immune response elicited by the progression from minimal residual disease (MRD) to actively growing recurrence. Screening for this innate response predicted accurately in which mice recurrence would occur. Premature induction of recurrence resensitized MRD to the primary therapy, suggesting a possible paradigm shift for clinical treatment of dormant disease in which the current expectant approach is replaced with active attempts to uncover MRD before evolution of the escape phenotype is complete. By combining screening with second-line treatments targeting innate insensitivity, up to 100% of mice that would have otherwise relapsed were cured. These data may open new avenues for early detection and appropriately timed, highly targeted treatment of tumor recurrence irrespective of tumor type or frontline treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Aguirre-Ghiso, J.A. Models, mechanisms and clinical evidence for cancer dormancy. Nat. Rev. Cancer 7, 834–846 (2007).
Goss, P.E. & Chambers, A.F. Does tumour dormancy offer a therapeutic target? Nat. Rev. Cancer 10, 871–877 (2010).
Hensel, J.A., Flaig, T.W. & Theodorescu, D. Clinical opportunities and challenges in targeting tumour dormancy. Nat. Rev. Clin. Oncol. 10, 41–51 (2013).
McGowan, P.M., Kirstein, J.M. & Chambers, A.F. Micrometastatic disease and metastatic outgrowth: clinical issues and experimental approaches. Future Oncol. 5, 1083–1098 (2009).
Pantel, K., Alix-Panabieres, C. & Riethdorf, S. Cancer micrometastases. Nat. Rev. Clin. Oncol. 6, 339–351 (2009).
Weinhold, K.J., Goldstein, L.T. & Wheelock, E.F. Tumour-dormant states established with L5178Y lymphoma cells in immunised syngeneic murine hosts. Nature 270, 59–61 (1977).
Weinhold, K.J., Goldstein, L.T. & Wheelock, E.F. The tumor dormant state. Quantitation of L5178Y cells and host immune responses during the establishment and course of dormancy in syngeneic DBA/2 mice. J. Exp. Med. 149, 732–744 (1979).
Weinhold, K.J., Miller, D.A. & Wheelock, E.F. The tumor dormant state. Comparison of L5178Y cells used to establish dormancy with those that emerge after its termination. J. Exp. Med. 149, 745–757 (1979).
Wikman, H., Vessella, R. & Pantel, K. Cancer micrometastasis and tumour dormancy. APMIS 116, 754–770 (2008).
Aguirre-Ghiso, J.A., Bragado, P. & Sosa, M.S. Metastasis awakening: targeting dormant cancer. Nat. Med. 19, 276–277 (2013).
Polzer, B. & Klein, C.A. Metastasis awakening: the challenges of targeting minimal residual cancer. Nat. Med. 19, 274–275 (2013).
Albini, A., Tosetti, F., Li, V.W., Noonan, D.M. & Li, W.W. Cancer prevention by targeting angiogenesis. Nat. Rev. Clin. Oncol. 9, 498–509 (2012).
Almog, N. et al. Transcriptional switch of dormant tumors to fast-growing angiogenic phenotype. Cancer Res. 69, 836–844 (2009).
Indraccolo, S. et al. Interruption of tumor dormancy by a transient angiogenic burst within the tumor microenvironment. Proc. Natl. Acad. Sci. USA 103, 4216–4221 (2006).
Murdoch, C., Muthana, M., Coffelt, S.B. & Lewis, C.E. The role of myeloid cells in the promotion of tumour angiogenesis. Nat. Rev. Cancer 8, 618–631 (2008).
Ossowski, L. & Aguirre-Ghiso, J.A. Dormancy of metastatic melanoma. Pigment Cell Melanoma Res. 23, 41–56 (2010).
Karrison, T.G., Ferguson, D.J. & Meier, P. Dormancy of mammary carcinoma after mastectomy. J. Natl. Cancer Inst. 91, 80–85 (1999).
Kovács, A.F., Ghahremani, M.T., Stefenelli, U. & Bitter, K. Postoperative chemotherapy with cisplatin and 5-fluorouracil in cancer of the oral cavity and the oropharynx–long-term results. J. Chemother. 15, 495–502 (2003).
Retsky, M.W., Demicheli, R., Hrushesky, W.J., Baum, M. & Gukas, I.D. Dormancy and surgery-driven escape from dormancy help explain some clinical features of breast cancer. APMIS 116, 730–741 (2008).
Drake, C.G., Jaffee, E.M. & Pardoll, D.M. Mechanisms of immune evasion by tumors. Adv. Immunol. 90, 51–81 (2006).
Garrido, F., Cabrera, T. & Aptsiauri, N. “Hard” and “soft” lesions underlying the HLA class I alterations in cancer cells: implications for immunotherapy. Int. J. Cancer 127, 249–256 (2010).
Kaluza, K.M. et al. Adoptive T cell therapy promotes the emergence of genomically altered tumor escape variants. Int. J. Cancer 131, 844–854 (2012).
Liu, K., Caldwell, S.A., Greeneltch, K.M., Yang, D. & Abrams, S.I. CTL adoptive immunotherapy concurrently mediates tumor regression and tumor escape. J. Immunol. 176, 3374–3382 (2006).
Nagaraj, S. et al. Altered recognition of antigen is a mechanism of CD8+ T cell tolerance in cancer. Nat. Med. 13, 828–835 (2007).
Sanchez-Perez, L. et al. Potent selection of antigen loss variants of B16 melanoma following inflammatory killing of melanocytes in vivo. Cancer Res. 65, 2009–2017 (2005).
Kaluza, K.M. et al. Adoptive transfer of cytotoxic T lymphocytes targeting two different antigens limits antigen loss and tumor escape. Hum. Gene Ther. 23, 1054–1064 (2012).
Kottke, T. et al. Use of biological therapy to enhance both virotherapy and adoptive T-cell therapy for cancer. Mol. Ther. 16, 1910–1918 (2008).
Rommelfanger, D.M. et al. Systemic combination virotherapy for melanoma with tumor antigen-expressing vesicular stomatitis virus and adoptive T-cell transfer. Cancer Res. 72, 4753–4764 (2012).
Wongthida, P. et al. Activating systemic T-cell immunity against self tumor antigens to support oncolytic virotherapy with vesicular stomatitis virus. Hum. Gene Ther. 22, 1343–1353 (2011).
Kottke, T. et al. Precise scheduling of chemotherapy primes VEGF-producing tumors for successful systemic oncolytic virotherapy. Mol. Ther. 19, 1802–1812 (2011).
Kottke, T. et al. Antiangiogenic cancer therapy combined with oncolytic virotherapy leads to regression of established tumors in mice. J. Clin. Invest. 120, 1551–1560 (2010).
Kottke, T. et al. Broad antigenic coverage induced by vaccination with virus-based cDNA libraries cures established tumors. Nat. Med. 17, 854–859 (2011).
Pulido, J. et al. Using virally expressed melanoma cDNA libraries to identify tumor-associated antigens that cure melanoma. Nat. Biotechnol. 30, 337–343 (2012).
Melcher, A. et al. Tumor immunogenicity is determined by the mechanism of cell death via induction of heat shock protein expression. Nat. Med. 4, 581–587 (1998).
Sanchez-Perez, L. et al. Synergy of adoptive T-cell therapy with intratumoral suicide gene therapy is mediated by host NK cells. Gene Ther. 14, 998–1009 (2007).
Vile, R.G. et al. Generation of an anti-tumour immune response in a non-immunogenic tumour: HSVtk-killing in vivo stimulates a mononuclear cell infiltrate and a TH1-like profile of intratumoural cytokine expression. Int. J. Cancer 71, 267–274 (1997).
Vile, R.G., Nelson, J.A., Castleden, S., Chong, H. & Hart, I.R. Systemic gene therapy of murine melanoma using tissue specific expression of the HSVtk gene involves an immune component. Cancer Res. 54, 6228–6234 (1994).
Karapanagiotou, E.M. et al. Phase I/II trial of carboplatin and paclitaxel chemotherapy in combination with intravenous oncolytic reovirus in patients with advanced malignancies. Clin. Cancer Res. 18, 2080–2089 (2012).
Dranoff, G. Experimental mouse tumour models: what can be learnt about human cancer immunology? Nat. Rev. Immunol. 12, 61–66 (2011).
Cray, C. Acute phase proteins in animals. Prog. Mol. Biol. Transl. Sci. 105, 113–150 (2012).
Cray, C., Zaias, J. & Altman, N.H. Acute phase response in animals: a review. Comp. Med. 59, 517–526 (2009).
Stadnyk, A.W. & Gauldie, J. The acute phase protein response during parasitic infection. Immunol. Today 12, A7–A12 (1991).
Gonzalez-Gonzalez, E. et al. Visualization of plasmid delivery to keratinocytes in mouse and human epidermis. Sci. Rep. 1, 158 (2011).
Mukhopadhyay, D., Knebelmann, B., Cohen, H.T., Ananth, S. & Sukhatme, V.P. The von Hippel-Lindau tumor suppressor gene product interacts with Sp1 to repress vascular endothelial growth factor promoter activity. Mol. Cell Biol. 17, 5629–5639 (1997).
Overwijk, W.W. et al. Tumor regression and autoimmunity after reversal of a functionally tolerant state of self-reactive CD8+ T cells. J. Exp. Med. 198, 569–580 (2003).
Lichty, B.D., Power, A.T., Stojdl, D.F. & Bell, J.C. Vesicular stomatitis virus: re-inventing the bullet. Trends Mol. Med. 10, 210–216 (2004).
Russell, S.J., Peng, K.W. & Bell, J.C. Oncolytic virotherapy. Nat. Biotechnol. 30, 658–670 (2012).
Boisgerault, N. et al. Functional cloning of recurrence-specific antigens identifies molecular targets to treat tumor relapse. Mol. Ther. 21, 1507–1516 (2013).
Duren, M. et al. Value of stimulated serum thyroglobulin levels for detecting persistent or recurrent differentiated thyroid cancer in high- and low-risk patients. Surgery 126, 13–19 (1999).
Kloos, R.T. & Mazzaferri, E.L. A single recombinant human thyrotropin-stimulated serum thyroglobulin measurement predicts differentiated thyroid carcinoma metastases three to five years later. J. Clin. Endocrinol. Metab. 90, 5047–5057 (2005).
Cooper, D.S. et al. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19, 1167–1214 (2009).
Gogas, H. et al. Prognostic significance of autoimmunity during treatment of melanoma with interferon. N. Engl. J. Med. 354, 709–718 (2006).
Tarhini, A.A., Gogas, H. & Kirkwood, J.M. IFN-α in the treatment of melanoma. J. Immunol. 189, 3789–3793 (2012).
Hogquist, K.A. et al. T cell receptor antagonistic peptides induce positive selection. Cell 76, 17–27 (1994).
Acknowledgements
We thank T. Higgins for expert secretarial assistance and M. Behrens and K. Knutson for help with Her-2-neu mice. This work was supported by the Richard M. Schulze Family Foundation, the Mayo Foundation, Cancer Research UK, US National Institutes of Health grants R01 CA107082, R01CA130878 and R01 CA132734 and a grant from T. and J. Paul.
Author information
Authors and Affiliations
Contributions
T.K. and N.B. designed and performed experiments and wrote the manuscript. R.M.D., O.D., D.R.-K. and J.T. designed and performed experiments. J.P., D.M., R.K. and M.C. designed the experiments, analyzed the results and interpreted the data. H.P., A.M., K.H. and P.S. designed the experiments, analyzed the results, interpreted the data and wrote the manuscript. R.V. designed and performed experiments, analyzed the results, interpreted the data and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–3 (PDF 312 kb)
Rights and permissions
About this article
Cite this article
Kottke, T., Boisgerault, N., Diaz, R. et al. Detecting and targeting tumor relapse by its resistance to innate effectors at early recurrence. Nat Med 19, 1625–1631 (2013). https://doi.org/10.1038/nm.3397
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.3397
This article is cited by
-
Paracrine secretion of IL8 by breast cancer stem cells promotes therapeutic resistance and metastasis of the bulk tumor cells
Cell Communication and Signaling (2023)
-
Combination therapy with CAR T cells and oncolytic viruses: a new era in cancer immunotherapy
Cancer Gene Therapy (2022)
-
Oncolytic virotherapy induced CSDE1 neo-antigenesis restricts VSV replication but can be targeted by immunotherapy
Nature Communications (2021)
-
The limiting factors of oncolytic virus immunotherapy and the approaches to overcome them
Applied Microbiology and Biotechnology (2020)
-
Bioengineered models to study tumor dormancy
Journal of Biological Engineering (2019)