Abstract
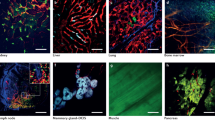
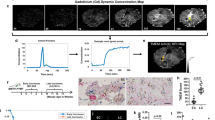
Brain metastasis frequently occurs in individuals with cancer and is often fatal. We used multiphoton laser scanning microscopy to image the single steps of metastasis formation in real time. Thus, it was possible to track the fate of individual metastasizing cancer cells in vivo in relation to blood vessels deep in the mouse brain over minutes to months. The essential steps in this model were arrest at vascular branch points, early extravasation, persistent close contacts to microvessels and perivascular growth by vessel cooption (melanoma) or early angiogenesis (lung cancer). Inefficient steps differed between the tumor types. Long-term dormancy was only observed for single perivascular cancer cells, some of which moved continuously. Vascular endothelial growth factor-A (VEGF-A) inhibition induced long-term dormancy of lung cancer micrometastases by preventing angiogenic growth to macrometastases. The ability to image the establishment of brain metastases in vivo provides new insights into their evolution and response to therapies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Steeg, P.S. Tumor metastasis: mechanistic insights and clinical challenges. Nat. Med. 12, 895–904 (2006).
Palmieri, D., Chambers, A.F., Felding-Habermann, B., Huang, S. & Steeg, P.S. The biology of metastasis to a sanctuary site. Clin. Cancer Res. 13, 1656–1662 (2007).
Wyckoff, J.B., Jones, J.G., Condeelis, J.S. & Segall, J.E. A critical step in metastasis: in vivo analysis of intravasation at the primary tumor. Cancer Res. 60, 2504–2511 (2000).
Chambers, A.F., Groom, A.C. & MacDonald, I.C. Dissemination and growth of cancer cells in metastatic sites. Nat. Rev. Cancer 2, 563–572 (2002).
Al-Mehdi, A.B. et al. Intravascular origin of metastasis from the proliferation of endothelium-attached tumor cells: a new model for metastasis. Nat. Med. 6, 100–102 (2000).
Yamauchi, K. et al. Development of real-time subcellular dynamic multicolor imaging of cancer-cell trafficking in live mice with a variable-magnification whole-mouse imaging system. Cancer Res. 66, 4208–4214 (2006).
Ito, S. et al. Real-time observation of micrometastasis formation in the living mouse liver using a green fluorescent protein gene-tagged rat tongue carcinoma cell line. Int. J. Cancer 93, 212–217 (2001).
Kedrin, D. et al. Intravital imaging of metastatic behavior through a mammary imaging window. Nat. Methods 5, 1019–1021 (2008).
Fidler, I.J., Yano, S., Zhang, R.D., Fujimaki, T. & Bucana, C.D. The seed and soil hypothesis: vascularisation and brain metastases. Lancet Oncol. 3, 53–57 (2002).
Seitz, G. et al. Imaging of cell trafficking and metastases of paediatric rhabdomyosarcoma. Cell Prolif. 41, 365–374 (2008).
Leenders, W.P. et al. Antiangiogenic therapy of cerebral melanoma metastases results in sustained tumor progression via vessel co-option. Clin. Cancer Res. 10, 6222–6230 (2004).
Luzzi, K.J. et al. Multistep nature of metastatic inefficiency: dormancy of solitary cells after successful extravasation and limited survival of early micrometastases. Am. J. Pathol. 153, 865–873 (1998).
Brown, E.B. et al. In vivo measurement of gene expression, angiogenesis and physiological function in tumors using multiphoton laser scanning microscopy. Nat. Med. 7, 864–868 (2001).
Winkler, F. et al. Kinetics of vascular normalization by VEGFR2 blockade governs brain tumor response to radiation: role of oxygenation, angiopoietin-1 and matrix metalloproteinases. Cancer Cell 6, 553–563 (2004).
Helmchen, F. & Denk, W. Deep tissue two-photon microscopy. Nat. Methods 2, 932–940 (2005).
Hoffman, R.M. Advantages of multi-color fluorescent proteins for whole-body and in vivo cellular imaging. J. Biomed. Opt. 10, 41202 (2005).
Rae, J.M., Creighton, C.J., Meck, J.M., Haddad, B.R. & Johnson, M.D. MDA-MB-435 cells are derived from M14 melanoma cells—a loss for breast cancer, but a boon for melanoma research. Breast Cancer Res. Treat. 104, 13–19 (2007).
Döme, B., Timar, J. & Paku, S. A novel concept of glomeruloid body formation in experimental cerebral metastases. J. Neuropathol. Exp. Neurol. 62, 655–661 (2003).
Townson, J.L. & Chambers, A.F. Dormancy of solitary metastatic cells. Cell Cycle 5, 1744–1750 (2006).
Scherbarth, S. & Orr, F.W. Intravital videomicroscopic evidence for regulation of metastasis by the hepatic microvasculature: effects of interleukin-1α on metastasis and the location of B16F1 melanoma cell arrest. Cancer Res. 57, 4105–4110 (1997).
Wood, S. Pathogenesis of metastasis formation observed in vivo in the rabbit ear chamber. AMA Arch. Pathol. 66, 550–568 (1958).
Kawaguchi, T., Tobai, S. & Nakamura, K. Extravascular migration of tumor cells in the brain: an electron microscopic study. Invasion Metastasis 2, 40–50 (1982).
Chambers, A.F., MacDonald, I.C., Schmidt, E.E., Morris, V.L. & Groom, A.C. Clinical targets for anti-metastasis therapy. Adv. Cancer Res. 79, 91–121 (2000).
Koop, S. et al. Fate of melanoma cells entering the microcirculation: over 80% survive and extravasate. Cancer Res. 55, 2520–2523 (1995).
Holash, J. et al. Vessel cooption, regression, and growth in tumors mediated by angiopoietins and VEGF. Science 284, 1994–1998 (1999).
Calabrese, C. et al. A perivascular niche for brain tumor stem cells. Cancer Cell 11, 69–82 (2007).
Yano, S. et al. Expression of vascular endothelial growth factor is necessary but not sufficient for production and growth of brain metastasis. Cancer Res. 60, 4959–4967 (2000).
Küsters, B. et al. Vascular endothelial growth factor-A(165) induces progression of melanoma brain metastases without induction of sprouting angiogenesis. Cancer Res. 62, 341–345 (2002).
Küsters, B. et al. Micronodular transformation as a novel mechanism of VEGF-A–induced metastasis. Oncogene 26, 5808–5815 (2007).
Weis, S., Cui, J., Barnes, L. & Cheresh, D. Endothelial barrier disruption by VEGF-mediated Src activity potentiates tumor cell extravasation and metastasis. J. Cell Biol. 167, 223–229 (2004).
Holmgren, L., O'Reilly, M.S. & Folkman, J. Dormancy of micrometastases: balanced proliferation and apoptosis in the presence of angiogenesis suppression. Nat. Med. 1, 149–153 (1995).
Bouvet, M. et al. In vivo color-coded imaging of the interaction of colon cancer cells and splenocytes in the formation of liver metastases. Cancer Res. 66, 11293–11297 (2006).
Ramaswamy, S., Ross, K.N., Lander, E.S. & Golub, T.R. A molecular signature of metastasis in primary solid tumors. Nat. Genet. 33, 49–54 (2003).
Kaye, A.H. & Laws, E.R. Brain Tumors: An Encyclopedic Approach. Ch. 49, 999–1026 (Churchill Livingstone, London, 2001).
Fidler, I.J. & Talmadge, J.E. Evidence that intravenously derived murine pulmonary melanoma metastases can originate from the expansion of a single tumor cell. Cancer Res. 46, 5167–5171 (1986).
Sellappan, S et al. Lineage infidelity of MDA-MB-435 cells: expression of melanocyte proteins in a breast cancer cell line. Cancer Res. 64, 3479–3485 (2004).
Schackert, G., Price, J.E., Bucana, C.D. & Fidler, I.J. Unique patterns of brain metastasis produced by different human carcinomas in athymic nude mice. Int. J. Cancer 44, 892–897 (1989).
Acknowledgements
F.W. and J.H. received funding for this work from the German Cancer Foundation (Deutsche Kebshilfe), and F.W. received a grant from the German Research Foundation (Deutsche Forschungsgemeinschaft; WI1930/4-1). J.H. received additional funding from the German Federal Ministry of Education and Research (Bundesministerium für Bildung und Forschung) and German Federal Ministry of Economics and Technology (Bundesministerium für Wirtschaft und Technologie) (16IN0675; 13N10171; 13N9268). Y.K. received a research grant from the Hypatia Foundation. We wish to thank C. Eggert for her excellent technical assistance, A. Ullrich, W. Hiddemann, R. Jain and U. Koedel for helpful discussions, K. Ogston for editing the manuscript and G. Mitteregger for her supervision of the animal facility. The PC14-PE6 human lung cancer cell line was kindly provided by I.J. Fidler, MD Anderson Cancer Center.
Author information
Authors and Affiliations
Contributions
Y.K. designed and performed experiments, carried out data analysis, prepared figures and wrote the manuscript. L.v.B. contributed to experimental work, especially to the generation of extravasation videos. M.F. provided technical support and methodological input regarding MPLSM. W.E.F.K. performed FACS sorting experiments. R.G. provided technical support and helpful discussions. J.H. contributed to the design of experiments and coordinated and supervised MPLSM. F.W. had the idea to establish the new animal model, designed and coordinated research, wrote the manuscript and supervised the project.
Corresponding author
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–4 and Supplementary Methods (PDF 1223 kb)
Supplementary Video 1
Initial arrest of cancer cells in the brain microvasculature. Passive movement of PC14-PE6 lung carcinoma cells (red) in relation to perfused brain microvessels (green, FITC dextran) imaged immediately after internal carotid artery injection for 3 min. Single images were acquired every 0.5 s, 50 μm deep in the brain parenchyma. Cells are arrested in capillaries of the same diameter, primarily at vascular bifurcations; n = 4 mice. (AVI 5714 kb)
Supplementary Video 2
Cancer cell arrest stays dynamic for hours. When followed over 1 h after internal carotid injection, it becomes evident that cells continuously give up and reenter a resting position; permanent arrest is rare. This could explain why neither areas with permanent absence of blood flow in vivo, nor brain infarcts in histological examinations have been detected. Bifurcations of capillaries of the same diameter are still the preferred sites for arrest. Images were acquired every 30 s for 60 minafter injection of PC14-PE6 lung carcinoma cells (n = 4 animals; here: 20–50 μm depth). (AVI 5287 kb)
Supplementary Video 3
Transmigration of the vascular wall. A melanoma cell (red, arrows) has partly extravasated through a hole in the wall (detected by additional GFP-positivity of endothelial cells in this animal, not shown) of blood vessel number 1. Note the extensive movement of the extravasated part, extending and retracting lamellipodia-like protrusions (arrowheads). The extravasated part is located in close proximity to a deeper larger vessel, which has no disruption of the endothelial lining (number 2). This video demonstrates the activity of the extravasation process, which always took longer than 30 min (n = 5 extravasating A2058 melanoma cells in n = 4 animals observed). Images were acquired every 45 s for 60 min, 24 h after injection (20–100 μm depth). (AVI 5711 kb)
Rights and permissions
About this article
Cite this article
Kienast, Y., von Baumgarten, L., Fuhrmann, M. et al. Real-time imaging reveals the single steps of brain metastasis formation. Nat Med 16, 116–122 (2010). https://doi.org/10.1038/nm.2072
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.2072
This article is cited by
-
PTEN-restoration abrogates brain colonisation and perivascular niche invasion by melanoma cells
British Journal of Cancer (2024)
-
Pericyte signaling via soluble guanylate cyclase shapes the vascular niche and microenvironment of tumors
The EMBO Journal (2024)
-
Intravital imaging to study cancer progression and metastasis
Nature Reviews Cancer (2023)
-
Dissecting metastasis using preclinical models and methods
Nature Reviews Cancer (2023)
-
L1CAM deployed perivascular tumor niche promotes vessel wall invasion of tumor thrombus and metastasis of renal cell carcinoma
Cell Death Discovery (2023)