Abstract
T cells compete in the response to antigen in vivo and this competition may drive the affinity maturation of a secondary T cell response. Here we show that high-affinity T cells out-competed lower affinity T cells during a response to antigenic challenge in vivo. Although competition between T cells specific for different peptide–major histocompatibility complexes (MHC) occurred, it was less efficient than competition between T cells of the same peptide-MHC specificity. In addition, high-affinity T cells efficiently induced antigen loss from the surface of antigen-presenting cells. Thus T cells that responded to the same peptide-MHC competed with each other by lowering the amount of ligand with which the cells could react. As a result, the activation of high-affinity cells was favored. This provides a mechanism for the affinity maturation of a secondary T cell response.
Similar content being viewed by others
Main
Although affinity maturation is a well documented and understood characteristic of B cell responses, it has only recently become clear that T cells also undergo affinity maturation. Early work showed the T cells stimulated during primary immune responses are usually polyclonal1,2,3,4. However, repeated exposure of the host to antigen gives rise to T cells with increasingly restricted T cell receptor (TCR) repertoires that have increasingly higher antigen affinities5,6,7,8,9,10,11,12. These data suggested that higher affinity T cells have a competitive advantage over lower affinity T cells, but the mechanism of this phenomenon is unknown.
Previous in vitro and in vivo experiments have suggested that competition between T cells in response to antigen can occur13,14,15. T cells bearing TCRs with a high-affinity for antigen inhibit the response of other T cells interacting with the same antigen-presenting cells (APCs)8. This inhibition occurred among T cells responding to the same and different antigens and was reduced by injection of increased numbers of antigen-bearing dendritic cells (DCs)8. Therefore inhibition of one responding population of T cells by another involved competition for some aspect of APCs8,14,15,16,17.
In thinking about how this competition could occur, we considered in vitro observations that show T cells can remove peptide–major histocompatibility complexes (MHC) from the surface of the APCs with which they are interacting18. A number of groups have reported that antigen, as well as other surface molecules, can be removed from the surface of APCs and that both TCR and CD28 on the T cell can mediate this phenomenon18,19,20. No physiologically relevant purpose for this antigen-stripping function of T cells has been shown. However, it has been suggested that it could prevent overstimulation of the antigen-specific population of T cells and thus reduce the likelihood of immunopathological phenomena such as activation-induced cell death and clonal exhaustion.
We show here that high-affinity T cells compete more effectively than low-affinity T cells in the response to antigen. In addition, in vivo, high-affinity T cells induce the loss of specific peptide-MHC from the surface of DCs without killing them or removing other proteins, such as B7. This process may account for the great efficiency with which high-affinity T cells inhibit the response of T cells with lower affinity to the same antigen. This suggests a mechanism for affinity maturation during T cell secondary responses.
Results
Competition between high- and lower affinity T cells
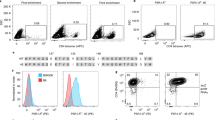
T cells compete with each other in the response to antigen8. We showed this phenomenon with adoptive transfer experiments in which T cells bearing the OT1 TCR—which is specific for the ovalbumin (OVA)-derived peptide SIINFEKL bound to H-2Kb (designated Kb-OVA)—from (B6.PL×B6)F1 (Thy1.1+/−) mice were transferred into B6 (Thy1.2+) mice. These transferred and other nontransferred controls were then challenged intravenously with bone marrow–derived DCs that were pulsed with OVA. Five days later, spleen cells from the mice were screened, by staining with Kb-OVA tetramers, to detect Thy1.1+ and Thy1.2+ CD8+ T cells that were specific for Kb-OVA (Fig. 1). In agreement with published data8, the transferred OT1 T cells almost completely blocked the response of host T cells to Kb-OVA.
Thy1.2+ B6 mice, which either had or hadn't received 2×105 Thy1.1+/− (B6×B6.PL)F1 OT1-Tg T cells, were immunized intravenously with 5×105 OVA peptide–pulsed DCs. Five days later, spleen cells from these mice were stained with Kb-OVA tetramers and antibodies to I-Ab, Thy1.1 and CD8. The dot plots were gated on all CD8+I-Ab− events. The histograms were further gated on the region marker R3 and therefore represent the tetramer staining of only the endogenous cells. Filled histograms, tetramer staining in mice challenged with pulsed DCs. Open (control) histograms, tetramer staining in mice challenged with unpulsed DCs. The numbers denote the percentage tetramer staining of total endogenous CD8+ T cells gated as in R3.
This phenomenon is due to competition for some aspect of antigen-bearing APCs8. We hypothesized that this competition among T cells was the driving force behind affinity maturation of the secondary T cell response. If this was the case then high-affinity T cells should have a competitive advantage over lower affinity T cells. We tested this hypothesis by transferring T cells with high- or low-to-moderate–affinity for antigen-MHC into mice and examined their ability to interfere with the response of the endogenous T cells. We had earlier assessed the ability of T cells to compete in primary responses (Fig. 1); because affinity maturation of T cells occurs during secondary responses, we adapted our protocol to study the competitive ability of memory T cells.
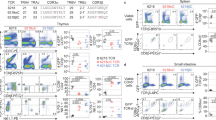
Two populations of competitor T cells were generated in vivo: high-affinity OT1-transgenic (Tg) memory T cells and “lower” affinity non-Tg B6.PL memory T cells. The lower affinity Kb-OVA–specific T cells were isolated from B6.PL (Thy1.1+) mice that had been challenged three times with an OVA-expressing vaccinia virus (VV.OVA). This generated a pool, which was 3–5% of total CD8+ T cells, of Kb-OVA–specific T cells. High-affinity T cells were isolated from B6 mice that had been given Thy1.1+ OT1 T cells and challenged once with VV.OVA. It should be noted that due to affinity maturation, challenging a host three times with VV.OVA produces T cells of higher affinity than challenging once with VV.OVA8. However these cells were not as high affinity as the OT1 T cells (Fig. 2a) and thus, for the purposes of these experiments, were considered as having lower affinity. The cells were characterized as high- or low-affinity by the intensity with which they were stained with Kb-OVA tetramers. The primed OT1 cells were stained more intensely with the tetramer than primed T cells from the B6.PL mice (Fig 2a).
(a) Characterization of high and lower affinity T cells. T cells with high affinity for Kb-OVA were prepared by immunizing B6 mice that had been given 2×106 (B6×B6.PL)F1 OT1 T cells with VV.OVA. Lower affinity Kb-OVA–specific T cells were from B6.PL mice intravenously immunized three times with VV.OVA. Splenic CD8+ T cells were purified by negative selection (see Methods) and stained with Kb-OVA tetramer. Filled histograms, tetramer staining of CD8+CD44+ cells. The background was assessed by tetramer staining of CD8+ T cells isolated from B6.PL mice immunized with control VV. MFI, mean fluorescence intensity. (b,c) Lower affinity T cells compete less efficiently than high-affinity cells. Normal B6 mice were immunized with VV.OVA to generate endogenous memory Kb-OVA–specific T cells. Between 1×105–5×105 of the Kb-OVA tetramer–staining CD8+ T cells isolated in a were transferred into these B6 mice. These transferred mice, together with nontransferred controls, were then challenged intravenously with 5×105 OVA-pulsed DCs. Five days later, spleen cells from the mice were stained with Kb-OVA tetramers and antibodies to I-Ab, Thy1.1 and CD8. Data were gated as in Fig. 15; the experiments were done three times. (b) Tetramer-staining profiles of host (Thy1.1−) CD8+ cells in animals that had received no transferred cells or in representative animals in which the lower or high-affinity transferred cells expanded to different extents. (c) Low-affinity cells can compete but are quantitatively less efficient than high-affinity cells. The yield of host Kb-OVA–specific T cells in mice that had received transferred cells is expressed as a percentage of the nontransferred controls, which was calculated as: (% of CD8+ host T cells in these mice that stained with tetramer) × 100/(% of CD8+ T cells in nontransferred mice that stained with tetramer). This calculation was plotted for each animal versus the yield of Kb-OVA–specific transferred cells, as measured by their percentage of total CD8+ T cells.
The amount of MHC class I6,8,22,23,24 and MHC class II9,21 tetramer binding, normalized to surface TCR expression, is proportional to the affinity of a given TCR for its antigen and is independent of coreceptor function. We found that CD3 expression was actually 20–40% lower on the OT1 cells compared to the lower affinity cells (data not shown), suggesting that the difference in affinity between these two populations of cells is actually greater than that observed (Fig. 2a). Although one report has suggested that the activation state of a T cell alters the way in which it binds MHC dimers24, the comparisons of tetramer staining in all our experiments were between cells with similar activation profiles (CD44hiLFA-1hiL-selectinloCD25lo 8 and data not shown). These phenotypic similarities, and the similar methods used to immunize the mice from which the cells were derived, further suggested that the only major difference between the OT1 memory and the lower affinity memory cells was their affinity for antigen. We were therefore confident in our characterization of T cells as relatively high- or low-affinity based on their staining with Kb-OVA tetramers.
B6 mice were challenged with VV.OVA and left for 25 days to recover and generate a small but detectable pool of endogenous, resting memory T cells that were Kb-OVA–specific. The high- or lower affinity Thy1.1+ cells described above (Fig. 2a) were then transferred into the previously challenged B6 hosts. The hosts were then challenged with DCs pulsed with the OVA peptide. Five days later, spleen cells from these animals were stained with anti-Thy1.1, anti-CD8 and Kb-OVA tetramers to evaluate the responses of the host and donor T cells to Kb-OVA.
Host T cells from animals that received no donor Kb-OVA–specific T cells responded well (Fig. 2b). The response of host T cells was almost completely inhibited by the presence of transferred high-affinity OT1 T cells. In contrast, the endogenous responses in mice that received lower affinity T cells were inhibited only in those animals in which the transferred cells expanded to become at least 2–3% of the total CD8+ T cell population (Fig 2b,c). Thus during a secondary response, T cells with high affinity for antigen-MHC competed more efficiently in response to antigen than T cells with lower affinity. This result supported the idea of competition-driven affinity maturation of T cell responses.
Nonantigen versus antigen-specific competition
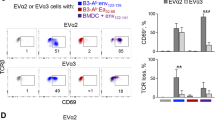
Competition between T cells responding to different peptides occurs only if the T cells are responding to peptides presented on the same APC8. Our first experiments on this subject involved competition between T cells that responded to peptides that were both bound to the same MHC protein, H-2Kb. We next wished to determine whether competition between T cells responding to peptides bound to different MHC proteins could occur. To this end, CD8+ T cells from OT1- and the P14-Tg mice25,26 were used as competitors in a cross-competition experiment. The P14-Tg TCR is specific for the lymphocytic choriomeningitis virus glycoprotein (GP)-derived peptide KAVYNFATM (referred to as GP33) in the context of MHC class I H-2Db. Both TCR-Tg mice were bred onto the B6.PL background and transferred as competitors into normal B6 mice. The mice were then challenged with DCs pulsed with the OVA and GP33 peptides individually or in combination. Five days after DC challenge, both the endogenous and transferred-cell primary responses were measured by staining the cells with anti-CD8, anti-Thy1.1 and either Kb-OVA or Db-GP33 tetramers (Fig. 3a).
(a) Responding T cells inhibit responses to other antigens provided both antigens are on the same APC. B6 mice were given 2×106 T cells from either OT1- or P14-Tg Thy1.1+/− mice. They were then challenged with 5×105 DCs pulsed with the OVA and GP33 peptides alone or in combination. Five days after DC challenge, spleen cells were stained with Kb-OVA or Db-GP33 tetramers and the percentages of host CD8+ T cells specific for the tetramers analyzed by gating on CD8+Thy1.1− events. Background staining (open histograms) was determined by staining cells from mice immunized with unpulsed DCs. One representative of three experiments is shown. Data gated as in Fig. 1. (b) Competition with T cells of the same specificity is more efficient than competition with T cells of different specificity. Various numbers of Thy1.1+ OT1 T cells were transferred to B6 mice. Transferred and nontransferred mice were challenged with DCs pulsed with OVA and SIY (which is presented by H-2Kb, but nonstimulatory to OT1 T cells). Data are mean±s.e.m of percentages of host CD8+ T cells, stained with the respective tetramer, calculated as a percentage of the same cells from nontransferred control animals. N=8 mice per group. The experiment was done three times.
Mice that had not received any transferred T cells produced a strong T cell response to both peptides, whether or not the peptides were on the same DC (Fig. 3a, rows 1 and 2). Providing the OVA and the GP33 peptides were on the same antigen-presenting DCs, OT1 T cells inhibited the endogenous T cell response to the GP33 peptide (Fig. 3a, rows 3 and 4). Likewise, P14 cells inhibited the endogenous response to OVA when OVA and GP33 were presented on the same DCs (Fig. 3a, rows 3 and 4). Therefore, providing the antigens were presented on a common APC, T cell competition occurred even when the competing populations were specific for completely different peptide-MHC complexes. However, each type of Tg T cell inhibited the endogenous response to its respective antigen better than the response to the other antigen (Fig. 3a, compare row 4 with rows 5 and 6). These data suggested that T cells compete in more than one way: first for a specific peptide-MHC complex and second for some more general feature of the APC.
This was confirmed in a titration experiment in which different numbers of Thy1.1+ OT1 T cells were transferred into B6 mice, which were then primed with DCs bearing OVA and the Kb-binding peptide SIYRRYGL (SIY)8,27. As few as 2.5×105 transferred OT1 cells could completely inhibit the endogenous T cell response to Kb-OVA (Fig. 3b). In contrast, although the OT1 cells inhibited the response to Kb-SIY to some extent, they were at least an order of magnitude less efficient. These results confirmed that T cells must compete with each other in at least two ways: specifically with respect to the peptide-MHC combination and nonspecifically with respect to interaction with the APC.
Loss of antigen-MHC from APCs in vivo
It has been suggested that the mechanism for competition between T cells for sites on the APC may act through the “sequestering” of peptide-MHC ligands from the APC surface by the T cell15. In addition, T cells can strip specific peptide-MHC from the APC surface in vitro18,19,20. This can also lead to stripping of other APC surface proteins, such as B7 and intercellular adhesion molecule (ICAM)19,20. These phenomena could explain both the antigen-specific and -nonspecific competition between T cells that we observed. To determine whether removal of proteins from APCs was indeed involved in T cell competition, we designed an experiment in which we could follow the fate and amounts of peptide-MHC complexes on DCs in vivo.
DCs were cultured from the bone marrow of green fluorescent protein (GFP)-Tg mice8,28; high amounts of GFP were expressed by all bone marrow–derived cells, which allowed easy identification of cells derived from these animals after they had been transferred to other mice. Cultured DCs were pulsed with OVA peptide, then the Kb-OVA–specific monoclonal antibody (mAb) 25D1.1629 was used to measure the amount of OVA peptide presented. OVA-pulsed and -unpulsed GFP+ DCs were injected intradermally into B6 mice with or without the transfer of small numbers of OT1 T cells. The draining lymph nodes were removed at various timepoints after injection and treated with collagenase to release the DCs. More than 95% of all GFP+ cells recovered from the challenged mice were I-Ab+ CD11c+CD11b+B220− (data not shown), which indicated that the recovered population of cells were predominantly DCs. The 25D1.16 staining of I-Ab+GFP+ DCs was then assessed. Immediately after OVA pulsing, the DCs expressed high amounts of Kb-OVA complexes (Fig. 4a). After transfer into animals that did not contain OT1 T cells, the expression of Kb-OVA complexes on the DCs decreased only minimally over time (Fig. 4a,b). However, in the presence of OT1 T cells, expression of Kb-OVA complexes fell rapidly and was barely detectable 36–48 h after transfer (Fig. 4a,b).
(a) Antibody staining of Kb-OVA complexes on GFP+I-Abhi cells. 2×106–4×106 unpulsed (control DC) or OVA-pulsed (OVA DC) DCs from the GFP mouse were injected intradermally into B6 mice with or without i.v. transfer of 1×106–2×106 Thy1.1+ OT1 cells (OVA DC + OT1). At various timepoints after DC challenge, the draining lymph nodes were isolated and collagenase digested to release the DCs and the DCs were stained with the anti–Kb-OVA (25D1.16) and anti–I-Ab. For each histogram 400–1000 GFP+I-Ab+ events were collected from three or four mice per timepoint and treatment. (b) MFI of 25D1.16 on GFP+I-Abhi cells. Data are mean±s.d.; one representative of six experiments is shown. (c) Loss of Kb-OVA is not accompanied by loss of all MHC class I. Cells from a and b were stained with anti–H-2Kb and anti–H-2Db. Data are expressed as mean MFI for each MHC class I on OVA-pulsed DCs, with or without OT1 transfer, as a percentage of the MFI of each MHC class I on nonpulsed DC isolated from control mice. An average of three mice were used per timepoint.
This reduction in Kb-OVA staining occurred in the absence of changes in the overall expression of H-2Kb or H-2Db on the DCs, as the amounts of these proteins on DCs remained relatively constant throughout the experiment, whether or not the animals contained OT1 cells (Fig. 4c). Therefore, interaction of antigen-specific T cells with the APC in vivo resulted in the specific loss of only the specific peptide-MHC from the APC surface. Our data do not indicate whether this was due to the T cell stripping antigen from the APC surface or specific down-modulation of peptide-MHC by the APC during the time it formed a synapse with antigen-specific T cells.
Targeted reduction in peptide-MHC on APCs
The fact that OT1 T cells did not reduce overall surface expression of H-2Kb or H-2Db on DCs suggested that the OT1 cells only affected the surface expression of peptide-MHC complexes with which they could react. To assess this directly, GFP+ DCs were again transferred into normal mice, as described above. In this experiment, however, the DCs were prepulsed with both OVA and GP33 peptides and were injected into B6 mice, with or without transfer of OT1 or P14 Thy1.1+ T cells. At various timepoints after DC challenge, the GFP+ DCs were isolated as before and expression of Kb-OVA complexes was assessed by staining with 25D1.16. The presence of the P14 cells did not induce the loss of 25D1.16 staining (Fig. 5a) but did inhibit the endogenous Kb-OVA–specific T cell response (Figs. 3 and 5b). However, mice transferred with OT1 cells again showed loss of 25D1.16 staining (Fig. 5a). Therefore the nonantigen-specific inhibition that occurred when T cells reacted with different peptide-MHC complexes on the surface of APCs was not caused by bystander T cell–mediated reduction of other complexes on the DCs.
(a) P14 cells do not cause the loss of Kb-OVA from DCs pulsed with OVA and GP33. Unpulsed (control DC) or OVA + GP33–pulsed (OVA and GP33 DC) GFP+ DCs (4×106) were injected intradermally into mice with or without transfer of Thy1.1+ P14- or OT1-Tg T cells (+ P14 transfer and + OT1 transfer, respectively). Five days after DC challenge, cells were isolated and stained for the presence of Kb-OVA complexes as in Fig. 4. Numbers on the histograms indicate the MFI of 25D1.16 (Kb-OVA complex) staining on GFP+I-Abhi cells. (b) Transferred P14 T cells responding to Db-GP33 on DCs compete specifically and nonspecifically with host T cells responding to Kb-OVA on the same DCs. Cells from a were stained with the respective tetramer as in Figs. 1–3. The histograms were gated on all Thy1.1−MHC class II−CD8+ events. Background staining was determined by tetramer staining of cells from mice immunized with unpulsed DCs. Data were analyzed as in Fig. 3. Numbers on the histograms indicate the percentages of host CD8+ T cells that were stained with tetramer. One representative of three experiments is shown. Data gated as in Fig. 1.
Loss of APCs or costimulatory proteins in vivo
In vitro, T cells can absorb various molecules from the surface of an APC19,20. To determine whether competition between T cells responding to different antigens affected the presence of other surface molecules, mice were challenged intradermally with OVA- and GP33-pulsed GFP+ DCs in the presence or absence of transferred OT1 or P14 T cells. We isolated DCs from draining lymph nodes 24 and 48 h after challenge and stained them for expression the accessory proteins B7-1, B7-2, ICAM-1, CD40 and CD48. The results showed that the numbers of DCs were essentially unaffected by the presence or absence of either P14 or OT1 T cells over the time-course of the experiment (Fig. 6a). In addition, there was no indication that the presence of OT1 cells negatively affected the expression of any of the major costimulatory proteins on the DC surface (Fig. 6b). Therefore, competition between T cells in response to the same or different peptide-MHC complexes on the same APCs is not due to death of the APCs or to loss of accessory proteins on these cells.
B6 mice, with or without the transfer of either 1×106 Thy1.1+ P14- or Thy1.1+ OT1-Tg T cells, were challenged intradermally with 3×106–4×106 GFP+ DCs pulsed with OVA + GP33. At 24 and 48 h after DC challenge, the draining lymph nodes were removed, collagenase-digested and stained as in Fig. 4. (a) The percentage of GFP+I-Ab+ cells was determined by flow cytometry as in Fig. 4. The absolute number of GFP+ DCs was then determined by multiplying this percentage by the total cell number. (b) The cells isolated in a were also separately stained with the antibodies shown as well as I-Ab. All I-Ab+GFP+ events were assessed for their expression of the respective surface marker. The MFI of the respective marker was then compared to the MFI of the same marker on unpulsed I-AbGFP+ DCs from control mice. Data are the mean±s.d. percentage of the control MFI (experimental MFI/control MFI×100); three mice analyzed per group. No differences in marker expression were observed between transferred and nontransferred mice. One representative of two experiments is shown.
Discussion
We have shown here that the T cell reaction with specific peptide-MHC on the surface of APCs leads to the loss of that peptide-MHC combination, but not other combinations, from the surface of DCs. However, our data do not indicate how this occurs. The T cells may strip the antigen from the DC surface or the DCs may specifically down-modulate peptide-MHC complexes after forming a synapse with antigen-specific T cells. Published in vivo15 and in vitro18,19,20 data suggests that the former idea is correct. In either case, peptide presentation by DCs is decreased in a way that would inhibit further productive interactions with other T cells specific for the same antigen. Such a phenomenon should make T cells of lower affinity less likely to detect the decreasing amount of antigen on the APC, which would result in the preferential expansion of higher affinity cells. Therefore this process could account for the affinity maturation that occurs during secondary T cell responses6,7,8,9,10,11,12.
Our data do indicate, however, that high-affinity T cells that react with specific antigen-MHC on APCs in vivo do not cause the loss of other peptide-MHC combinations on the same cells. Therefore some other process must account for the ability of T cells specific for different antigens to compete with each other. Although, in vitro, the loss of some accessory molecules from DCs after T cell interaction occurs18,19,20, we observed no loss of the accessory proteins B7-1, B7-2, ICAM-1, CD40, CD48, CD11b, CD11c and I-Ab from the DC surface (data not shown). Thus, the mechanism of nonantigen-specific competition may be due to competition for surface molecules other than those analyzed, soluble factors produced by the DC, limited space within lymphoid tissue in the DC compartment or a combination of all the above.
Given these data, it is easy to envision the scenario by which multiple challenges of a host with antigen favors the outgrowth of increasingly higher affinity T cells, leading the entire antigen-specific population toward oligo- or mono-clonality. High-affinity T cells are able to respond to lower amounts of antigen and may therefore be the first to detect its presence on the surface of APCs. This interaction leads to the stimulation and proliferation of the T cell, as well as the loss of antigen from the surface of the APC. The resulting reduced presentation of antigen favors the stimulation of even higher affinity T cells. In addition to inducing the specific loss of peptide-MHC complexes, the higher affinity T cells will proliferate to the point where they can compete as a population for all other stimulatory aspects of the APC and effectively inhibit other T cells of both the same and of different antigen specificities. The combination of these two competitive mechanisms therefore effectively drives the affinity maturation of a secondary T cell response. These studies show another dynamic aspect of the interaction between T cells and APCs and suggest that the responding T cells may play as much a role in shaping antigen presentation as the APCs do in shaping the T cell response.
Methods
Mice.
C57BL/6 (B6) and B6.PL-Thy1a/Cy (B6.PL) mice aged 6–8 weeks old were from the Jackson Laboratory (Bar Harbor, ME) and were used for all experiments. OT1-Tg mice30,31, specific for H-2Kb bound to the SIINFEKL peptide, and P14-Tg mice25,26, specific for H-2Db bound to the KAVYNFATM peptide (from P. Ohashi), were crossed with B6.PL mice to generate Thy1.1+/− TCR-Tg mice. UBI-GFP mice (referred to as GFP mice), which expressed GFP under the control of the human ubiquitin promotor, were generated at the National Jewish Microinjection Facility28.
Antibodies and tetramers.
Allophycocyanin-conjugated anti-CD8; fluorescein isothyocyanate (FITC)-conjugated CD44 and Thy1.2; cychrome-conjugated B220, H-2Db and streptavidin; biotin-conjugated I-Ab; and phycoerytherin (PE)-conjugated H-2Kb, B7-1, B7-2, ICAM-1,CD40, CD11c and CD11b were all from Pharmingen (San Diego CA). H-2Kb and H-2Db tetrameric molecules were produced as described8. The 25D1.16 hybridoma used to make the antibody was from R. Germain. Kb tetramers bearing an irrelevant peptide were used to establish the background staining of experimental samples. Each batch of Kb-OVA tetramer was tested and normalized for binding to naïve OT1 T cells before use in experiments.
Virus infection of animals.
VV.OVA was propagated in, and titrated by, plaque assay on cultured 143B osteosarcoma cells as described32. Priming with VV.OVA was done as described8. Multiple VV.OVA challenges were done at least 2 weeks apart. For the experiments in Fig. 2, CD8+ T cells were prepared from spleens with CD8+ StemCep columns (StemCell Technologies, Vancouver, Canada), according to the manufacturer's protocol.
Cell preparation and analysis.
DCs were cultured from bone marrow as described8,9. Briefly, bone marrow cells from normal B6 or GFP-Tg mice were cultured in 10 ng/ml of granulocyte-macrophage colony-stimulating factor (GM-CSF) for 2 days, nonadherant cells were then removed and further cultured in GM-CSF from the B78Hi/GMCSF.1 cell line33 (from H. Levitsky) for another 4–5 days. Cells were pulsed with peptides at 10–100 μg/ml for 8–12 h. DCs were collected and incubated for 30 min with 1 μg/ml of lipopolysaccharide to induce maturation. For intradermal transfer, DCs were injected into both the flank and scruff of the neck. At various times after intradermal DC injection, axillary, brachial and inguinal lymph nodes were isolated and subjected to collagenase treatment as described1. After collagenase treatment, the cells were resuspended in incomplete Click's medium (Irvine Scientific, Irvine, CA) with 5 mM EDTA to prevent clumping of the DCs. The cells were stained with trinitrophenol (TNP)-25D1.1629 (from R. Germain) and anti–I-Ab on ice for at least 30 min. After washing in 5 mM EDTA Click's medium, cychrome–anti-TNP was added for 30 min on ice. Cells were then washed, fixed in 3% PFA and analyzed by flow cytometry on a FACScaliber (Becton Dickinson, Mountain View, CA). Histograms showing the intensity of 25D1.16 staining (that is, amount of Kb-OVA complexes) on the injected DCs were obtained by gating on GFP+I-Ab+ events. Parallel wells were stained with combinations of antibodies to H-2Kb, H-2Db, B7-1, B7-2, ICAM-1, CD40, CD11c, CD11b and/or CD48 to assess amounts of these markers on the transferred DCs.
Spleen and lymph node cells were isolated and stained with tetramer as described8,21. Briefly, cells were stained at 37 °C for 2 h in the presence of 1–5 μg/ml of tetramer. Allophycocyanate–anti-CD8, TNP-anti–I-Ab and FITC–anti-Thy1.1 were added for another 30 min. The cells were washed and cychrome–anti-TNP was added at 4 °C for 30 min. The cells were washed, fixed and analyzed by four-color flow cytometry on a FACScaliber instrument and analyzed with CellQuest software (Becton Dickinson).
References
Casanova, J. L., Romero, P., Widmann, C., Kourilsky, P. & Maryanski, J. L. T cell receptor genes in a series of class I major histocompatibility complex-restricted cytotoxic T lymphocyte clones specific for a Plasmodium berghei nonapeptide: implications for T cell allelic exclusion and antigen-specific repertoire. J. Exp. Med. 174, 1371–1383 (1991).
Cole, G. A., Hogg, T. L. & Woodland, D. L. The MHC class I-restricted T cell response to Sendai virus infection in C57BL/6 mice: a single immunodominant epitope elicits an extremely diverse repertoire of T cells. Int. Immunol. 6, 1767–1775 (1994).
Horwitz, M. S., Yanagi, Y. & Oldstone, M. B. T-cell receptors from virus-specific cytotoxic T lymphocytes recognizing a single immunodominant nine-amino-acid viral epitope show marked diversity. J. Virol. 68, 352–357 (1994).
McHeyzer-Williams, M. G. & Davis, M. M. Antigen-specific development of primary and memory T cells in vivo. Science 268, 106–111 (1995).
McMichael, A. J., Saaszuki, T., McDevitt, H. O. & Payne, R. O. Increased frequency of HLA-Cw3 and HLA-Dw4 in rheumatoid arthritis. Arth. Rheum. 20, 1037–1042 (1977).
Busch, D. H. & Pamer, E. G. T cell affinity maturation by selective expansion during infection. J. Exp. Med. 189, 701–710 (1999).
Fasso, M. et al. T cell receptor (TCR)-mediated repertoire selection and loss of TCR Vβ diversity during the initiation of a CD4(+) T cell response in vivo. J. Exp. Med. 192, 1719–1730 (2000).
Kedl, R. M. et al. T Cells Compete for access to antigen-bearing antigen-presenting cells. J. Exp. Med. 192, 1105–1114 (2000).
Rees, W. et al. An inverse relationship between T cell receptor affinity and antigen dose during CD4(+) T cell responses in vivo and in vitro. Proc. Natl Acad. Sci. USA 96, 9781–9786 (1999).
Savage, P. A., Boniface, J. J. & Davis, M. M. A kinetic basis for T cell receptor repertoire selection during an immune response. Immunity 10, 485–492 (1999).
Slifka, M. K. & Whitton, J. L. Functional avidity maturation of CD8+ T cells without selection of higher affinity TCR. Nature Immunol. 2, 711–717 (2001).
van Bergen, J., Kooy, Y. & Koning, F. CD4-independent T cells impair TCR triggering of CD4-dependent T cells: a putative mechanism for T cell affinity maturation. Eur. J. Immunol. 31, 646–652 (2001).
Wolpert, E. Z., Grufman, P., Sandberg, J. K., Tegnesjo, A. & Karre, K. Immunodominance in the CTL response against minor histocompatibility antigens: interference between responding T cells, rather than with presentation of epitopes. J. Immunol. 161, 4499–4505 (1998).
Grufman, P., Wolpert, E. Z., Sandberg, J. K. & Karre, K. T cell competition for the antigen-presenting cell as a model for immunodominance in the cytotoxic T lymphocyte response against minor histocompatibility antigens. Eur. J. Immunol. 29, 2197–2204 (1999).
Butz, E. A. & Bevan, M. J. Massive expansion of antigen-specific CD8+ T cells during an acute virus infection. Immunity 8, 167–175 (1998).
Pion, S. et al. On the mechanisms of immunodominance in cytotoxic T lymphocyte responses to minor histocompatibility antigens. Eur. J. Immunol. 27, 421–430 (1997).
Taams, L. S. et al. Anergic T cells actively suppress T cell responses via the antigen-presenting cell. Eur. J. Immunol. 28, 2902–2912 (1998).
Huang, J. F. et al. TCR-Mediated internalization of peptide-MHC complexes acquired by T cells. Science 286, 952–954 (1999).
Hudrisier, D., Riond, J., Mazarguil, H., Gairin, J. E. & Joly, E. Cutting edge: CTLs rapidly capture membrane fragments from target cells in a TCR signaling-dependent manner. J. Immunol. 166, 3645–3649 (2001).
Hwang, I. et al. T cells can use either T cell receptor or CD28 receptors to absorb and internalize cell surface molecules derived from antigen-presenting cells. J. Exp. Med. 191, 1137–1148 (2000).
Crawford, F., Kozono, H., White, J., Marrack, P. & Kappler, J. Detection of antigen-specific T cells with multivalent soluble class II MHC covalent peptide complexes. Immunity 8, 675–682 (1998).
Bodinier, M. et al. Efficient detection and immunomagnetic sorting of specific T cells using multimers of MHC class I and peptide with reduced CD8 binding. Nature Med. 6, 707–710 (2000).
Yee, C., Savage, P. A., Lee, P. P., Davis, M. M. & Greenberg, P. D. Isolation of high avidity melanoma-reactive CTL from heterogeneous populations using peptide-MHC tetramers. J. Immunol. 162, 2227–2234 (1999).
Fahmy, T. M., Bieler, J. G., Edidin, M. & Schneck, J. P. Increased TCR avidity after T cell activation: a mechanism for sensing low-density antigen. Immunity 14, 135–143 (2001).
Brandle, D. et al. Involvement of both T cell receptor Vα and Vβ variable region domains and α chain junctional region in viral antigen recognition. Eur. J. Immunol. 21, 2195–2202 (1991).
Ashton-Rickardt, P. G. et al. Evidence for a differential avidity model of T cell selection in the thymus. Cell 76, 651–663 (1994).
Udaka, K., Wiesmuller, K. H., Kienle, S., Jung, G. & Walden, P. Self-MHC-restricted peptides recognized by an alloreactive T lymphocyte clone. J. Immunol. 157, 670–678 (1996).
Schaefer, B. C., Schaefer, M. L., Kappler, J. W., Marrack, P. & Kedl, R. M. Observation of antigen dependent CD8+ T cell/dendritic cell interactions in vivo. (Submitted, 2001).
Porgador, A., Yewdell, J. W., Deng, Y., Bennink, J. R. & Germain, R. N. Localization, quantitation, and in situ detection of specific peptide-MHC class I complexes using a monoclonal antibody. Immunity 6, 715–726 (1997).
Hogquist, K. A. et al. T cell receptor antagonist peptides induce positive selection. Cell 76, 17–27 (1994).
Kelly, J. M. et al. Identification of conserved T cell receptor CDR3 residues contacting known exposed peptide side chains from a major histocompatibility complex class I-bound determinant. Eur. J. Immunol. 23, 3318–3326 (1993).
Mitchell, T., Kappler, J. & Marrack, P. Bystander virus infection prolongs activated T cell survival. J. Immunol. 162, 4527–4535 (1999).
Levitsky, H. I., Lazenby, A., Hayashi, R. J. & Pardoll, D. M. In vivo priming of two distinct antitumor effector populations: the role of MHC class I expression. J. Exp. Med. 179, 1215–1224 (1994).
Acknowledgements
We thank D. Becker and T. DeBlieck for expert technical assistance. Supported by USPHS grants AI17134, AI18785 and AI22295, the Cancer Research Institute (R. M. K.) and the Leukemia and Lymphoma Society (B. C. S.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kedl, R., Schaefer, B., Kappler, J. et al. T cells down-modulate peptide-MHC complexes on APCs in vivo. Nat Immunol 3, 27–32 (2002). https://doi.org/10.1038/ni742
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni742
This article is cited by
-
T-cell receptor signal strength and epigenetic control of Bim predict memory CD8+ T-cell fate
Cell Death & Differentiation (2020)
-
Rapidly Generated Multivirus-specific Cytotoxic T Lymphocytes for the Prophylaxis and Treatment of Viral Infections
Molecular Therapy (2012)
-
Antigen‐driven T‐cell repertoire selection during adaptive immune responses
Immunology & Cell Biology (2011)
-
CD4+ T cell-released exosomes inhibit CD8+ cytotoxic T-lymphocyte responses and antitumor immunity
Cellular & Molecular Immunology (2011)
-
Intercellular Exchange of Surface Molecules and its Physiological Relevance
Archivum Immunologiae et Therapiae Experimentalis (2010)