Abstract
Lymphocyte recruitment maintains intestinal immune homeostasis but also contributes to inflammation. The orphan chemoattractant receptor GPR15 mediates regulatory T cell homing and immunosuppression in the mouse colon. We show that GPR15 is also expressed by mouse TH17 and TH1 effector cells and is required for colitis in a model that depends on the trafficking of these cells to the colon. In humans GPR15 is expressed by effector cells, including pathogenic TH2 cells in ulcerative colitis, but is expressed poorly or not at all by colon regulatory T (Treg) cells. The TH2 transcriptional activator GATA-3 and the Treg-associated transcriptional repressor FOXP3 robustly bind human, but not mouse, GPR15 enhancer sequences, correlating with receptor expression. Our results highlight species differences in GPR15 regulation and suggest it as a potential therapeutic target for colitis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Islam, S.A. & Luster, A.D. T cell homing to epithelial barriers in allergic disease. Nat. Med. 18, 705–715 (2012).
Mora, J.R. & Von Andrian, U.H. Specificity and plasticity of memory lymphocyte migration. Curr. Top. Microbiol. Immunol. 308, 83–116 (2006).
Zabel, B.A., Rott, A. & Butcher, E.C. Leukocyte chemoattractant receptors in human disease pathogenesis. Annu. Rev. Pathol. doi:10.1146/annurev-pathol-012513-104640 (2014).
Olson, T.S. & Ley, K. Chemokines and chemokine receptors in leukocyte trafficking. Am. J. Physiol. Regul. Integr. Comp. Physiol. 283, R7–R28 (2002).
Kunkel, E.J. & Butcher, E.C. Chemokines and the tissue-specific migration of lymphocytes. Immunity 16, 1–4 (2002).
Berlin, C. et al. Alpha 4 beta 7 integrin mediates lymphocyte binding to the mucosal vascular addressin MAdCAM-1. Cell 74, 185–195 (1993).
Miura, S., Hokari, R. & Tsuzuki, Y. Mucosal immunity in gut and lymphoid cell trafficking. Ann. Vascular Dis. 5, 275–281 (2012).
Wang, C., Kang, S.G., Lee, J., Sun, Z. & Kim, C.H. The roles of CCR6 in migration of Th17 cells and regulation of effector T-cell balance in the gut. Mucosal Immunol. 2, 173–183 (2009).
Joost, P. & Methner, A. Phylogenetic analysis of 277 human G-protein-coupled receptors as a tool for the prediction of orphan receptor ligands. Genome Biol. 3, 0063 (2002).
Deng, H.K., Unutmaz, D., KewalRamani, V.N. & Littman, D.R. Expression cloning of new receptors used by simian and human immunodeficiency viruses. Nature 388, 296–300 (1997).
Kim, S.V. et al. GPR15-mediated homing controls immune homeostasis in the large intestine mucosa. Science 340, 1456–1459 (2013).
Lee, A.Y. et al. Dendritic cells in colonic patches and iliac lymph nodes are essential in mucosal IgA induction following intrarectal administration via CCR7 interaction. Eur. J. Immunol. 38, 1127–1137 (2008).
Kunkel, E.J., Campbell, D.J. & Butcher, E.C. Chemokines in lymphocyte trafficking and intestinal immunity. Microcirculation 10, 313–323 (2003).
Mackay, C.R. Moving targets: cell migration inhibitors as new anti-inflammatory therapies. Nat. Immunol. 9, 988–998 (2008).
Powrie, F., Leach, M.W., Mauze, S., Caddle, L.B. & Coffman, R.L. Phenotypically distinct subsets of CD4+ T cells induce or protect from chronic intestinal inflammation in C. B-17 scid mice. Int. Immunol. 5, 1461–1471 (1993).
Shigematsu, T., Specian, R.D., Wolf, R.E., Grisham, M.B. & Granger, D.N. MAdCAM mediates lymphocyte-endothelial cell adhesion in a murine model of chronic colitis. Am. J. Physiol. Gastrointest. Liver Physiol. 281, G1309–G1315 (2001).
Picarella, D. et al. Monoclonal antibodies specific for beta 7 integrin and mucosal addressin cell adhesion molecule-1 (MAdCAM-1) reduce inflammation in the colon of scid mice reconstituted with CD45RBhigh CD4+ T cells. J. Immunol. 158, 2099–2106 (1997).
Denning, T.L., Kim, G. & Kronenberg, M. Cutting edge: CD4+CD25+ regulatory T cells impaired for intestinal homing can prevent colitis. J. Immunol. 174, 7487–7491 (2005).
Wang, C. et al. Effect of alpha4beta7 blockade on intestinal lymphocyte subsets and lymphoid tissue development. Inflamm. Bowel Dis. 16, 1751–1762 (2010).
Soriano, A. et al. VCAM-1, but not ICAM-1 or MAdCAM-1, immunoblockade ameliorates DSS-induced colitis in mice. Lab. Invest. 80, 1541–1551 (2000).
Powrie, F. et al. Inhibition of Th1 responses prevents inflammatory bowel disease in scid mice reconstituted with CD45RBhi CD4+ T cells. Immunity 1, 553–562 (1994).
Yen, D. et al. IL-23 is essential for T cell-mediated colitis and promotes inflammation via IL-17 and IL-6. J. Clin. Invest. 116, 1310–1316 (2006).
Elson, C.O. et al. Monoclonal anti-interleukin 23 reverses active colitis in a T cell-mediated model in mice. Gastroenterology 132, 2359–2370 (2007).
Fuss, I.J. et al. Disparate CD4+ lamina propria (LP) lymphokine secretion profiles in inflammatory bowel disease. Crohn's disease LP cells manifest increased secretion of IFN-gamma, whereas ulcerative colitis LP cells manifest increased secretion of IL-5. J. Immunol. 157, 1261–1270 (1996).
Brand, S. Crohn's disease: Th1, Th17 or both? The change of a paradigm: new immunological and genetic insights implicate Th17 cells in the pathogenesis of Crohn's disease. Gut 58, 1152–1167 (2009).
Ho, I.C., Tai, T.S. & Pai, S.Y. GATA3 and the T-cell lineage: essential functions before and after T-helper-2-cell differentiation. Nat. Rev. Immunol. 9, 125–135 (2009).
Wang, Y., Su, M.A. & Wan, Y.Y. An essential role of the transcription factor GATA-3 for the function of regulatory T cells. Immunity 35, 337–348 (2011).
Wohlfert, E.A. et al. GATA3 controls Foxp3+ regulatory T cell fate during inflammation in mice. J. Clin. Invest. 121, 4503–4515 (2011).
Rudra, D. et al. Transcription factor Foxp3 and its protein partners form a complex regulatory network. Nat. Immunol. 13, 1010–1019 (2012).
Kanhere, A. et al. T-bet and GATA3 orchestrate Th1 and Th2 differentiation through lineage-specific targeting of distal regulatory elements. Nat. Commun. 3, 1268 (2012).
Wei, G. et al. Genome-wide analyses of transcription factor GATA3-mediated gene regulation in distinct T cell types. Immunity 35, 299–311 (2011).
Zhang, Y. et al. Model-based analysis of ChIP-Seq (MACS). Genome Biol. 9, R137 (2008).
Marine, J. & Winoto, A. The human enhancer-binding protein Gata3 binds to several T-cell receptor regulatory elements. Proc. Natl. Acad. Sci. USA 88, 7284–7288 (1991).
Arvey, A. et al. Inflammation-induced repression of chromatin bound by the transcription factor Foxp3 in regulatory T cells. Nat. Immunol. 15, 580–587 (2014).
Lahl, K., Sweere, J., Pan, J. & Butcher, E. Orphan chemoattractant receptor GPR15 mediates dendritic epidermal T-cell recruitment to the skin. Eur. J. Immunol. 44, 2577–2581 (2014).
Schneider, M.A., Meingassner, J.G., Lipp, M., Moore, H.D. & Rot, A. CCR7 is required for the in vivo function of CD4+ CD25+ regulatory T cells. J. Exp. Med. 204, 735–745 (2007).
Sydora, B.C. et al. beta7 Integrin expression is not required for the localization of T cells to the intestine and colitis pathogenesis. Clin. Exp. Immunol. 129, 35–42 (2002).
Strober, W., Fuss, I.J. & Blumberg, R.S. The immunology of mucosal models of inflammation. Annu. Rev. Immunol. 20, 495–549 (2002).
Strober, W. & Fuss, I.J. Experimental models of mucosal inflammation. Adv. Exp. Med. Biol. 579, 55–97 (2006).
Heller, F. et al. Interleukin-13 is the key effector Th2 cytokine in ulcerative colitis that affects epithelial tight junctions, apoptosis, and cell restitution. Gastroenterology 129, 550–564 (2005).
Neurath, M.F. Cytokines in inflammatory bowel disease. Nat. Rev. Immunol. 14, 329–342 (2014).
Birzele, F. et al. Next-generation insights into regulatory T cells: expression profiling and FoxP3 occupancy in Human. Nucleic Acids Res. 39, 7946–7960 (2011).
Samstein, R.M. et al. Foxp3 exploits a pre-existent enhancer landscape for regulatory T cell lineage specification. Cell 151, 153–166 (2012).
Villar, D., Flicek, P. & Odom, D.T. Evolution of transcription factor binding in metazoans—mechanisms and functional implications. Nat. Rev. Genet. 15, 221–233 (2014).
Lefrancois, L. & Lycke, N. Isolation of mouse small intestinal intraepithelial lymphocytes, Peyer's patch, and lamina propria cells. Curr. Protoc. Immunol. Unit 3.19 (2001).
Zúñiga, L.A. et al. IL-17 regulates adipogenesis, glucose homeostasis, and obesity. J. Immunol. 185, 6947–6959 (2010).
Habtezion, A., Toivola, D.M., Butcher, E.C. & Omary, M.B. Keratin-8-deficient mice develop chronic spontaneous Th2 colitis amenable to antibiotic treatment. J. Cell Sci. 118, 1971–1980 (2005).
Chinen, T. et al. Prostaglandin E2 and SOCS1 have a role in intestinal immune tolerance. Nat. Commun. 2, 190 (2011).
Fiocchi, C. & Youngman, K.R. Isolation of human intestinal mucosal mononuclear cells. Curr. Protoc. Immunol. Unit 7.30 (2001).
Rani, A. et al. IL-2 regulates expression of C-MAF in human CD4 T cells. J. Immunol. 187, 3721–3729 (2011).
Wei, G. et al. Global mapping of H3K4me3 and H3K27me3 reveals specificity and plasticity in lineage fate determination of differentiating CD4+ T cells. Immunity 30, 155–167 (2009).
Gökmen, M.R. et al. Genome-wide regulatory analysis reveals that T-bet controls Th17 lineage differentiation through direct suppression of IRF4. J. Immunol. 191, 5925–5932 (2013).
Baekkevold, E.S. et al. A role for CCR4 in development of mature circulating cutaneous T helper memory cell populations. J. Exp. Med. 201, 1045–1051 (2005).
Wirtz, S., Neufert, C., Weigmann, B. & Neurath, M.F. Chemically induced mouse models of intestinal inflammation. Nat. Protoc. 2, 541–546 (2007).
Fitch, F.W., Gajewski, T.F. & Hu-Li, J. Production of TH1 and TH2 cell lines and clones. Curr. Protoc. Immunol. Chapter 3, Unit 3.13. doi:10.1002/0471142735 (2006).
Pandiyan, P. et al. CD4+CD25+Foxp3+ regulatory T cells promote Th17 cells in vitro and enhance host resistance in mouse Candida albicans Th17 cell infection model. Immunity 34, 422–434 (2011).
Fantini, M.C., Dominitzki, S., Rizzo, A., Neurath, M.F. & Becker, C. In vitro generation of CD4+ CD25+ regulatory cells from murine naive T cells. Nat. Protoc. 2, 1789–1794 (2007).
Acknowledgements
This work was supported by US National Institute of Health (NIH) grant R37 AI047822 to E.C.B., NIH grants K08 DK069385 and R03 DK085426 to A. Habtezion, the FACS Core facility of the Stanford Digestive Disease Center (NIH Digestive Disease Center grants DK56339) and the VA Palo Alto Health Care System. Research was also supported by the Wellcome Trust (R.G.J. and G.M.L., grant number 091009), the Medical Research Council (G.M.L., grant number G0802068), the National Institute for Health Research (NIHR) University College London Hospitals Biomedical Research Centre and the NIHR Biomedical Research Centre based at Guy's and St Thomas' National Health Service (NHS) Foundation Trust and King's College London. The views expressed are those of the authors and not necessarily those of the NIH, NHS, the NIHR or the Department of Health. L.P.N., H.H. and T.T.D. were recipients of fellowships under NIH Training grant T32 AI07290. L.P.N. was also a recipient of NIH postdoctoral fellowship grant 1F32 AI082924. T.T.D. is supported by a Cardiovascular Institute Fellowship under NIH T32 HL098049. H.H. is funded by NIH grant AI109452A, was a recipient of an Investigator Career Award from the Arthritis Foundation and was supported in part by a CIRM grant. We thank J. Xue (Stanford University) for assistance with the RT-PCR experiments, J. Chen (Stanford University) for technical assistance with the animal work and the Stanford Tissue Bank for providing the human colon specimens. We thank D. Littman (NYU) for recovering his cryopreserved Gpr15gfp mouse embryos for us in response to our request for collaboration to test our hypothesis that GPR15 mediates colon lymphocyte homing.
Author information
Authors and Affiliations
Contributions
J.P., E.O'H., A. Habetzion, E.C.B. and L.P.N. performed exploratory gene profiling that identified GPR15 as a candidate colon-homing receptor. L.P.N. performed experiments and wrote the manuscript. H.H. and A.E. performed mouse T cell polarization and short-term homing experiments. J.P. identified the Gpr15 enhancer and the Gata3 mutation and J.P. and T.T.D. characterized it. A. Hertweck and M.R.G. performed ChIP-Seq and ChIP-qPCR. G.M.L. and R.G.J. initiated and supervised the ChIP work. R.G.J. performed ChIP, analyzed ChIP-Seq data and wrote parts of the manuscript. E.C.B. initiated the project, analyzed data, provided overall supervision and wrote the manuscript. A. Habetzion supervised the project and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 GPR15 is preferentially expressed on colon CD4+ T cells with a memory/effector (CD45RBlo, CD44hi) and activated phenotype.
GPR15 is preferentially expressed on colon CD4+ T cells with a memory/effector (CD45RBlo, CD44hi) and activated phenotype. (a) GPR15 (GFP) expression by memory/effector (CD44hi, CD45RBlo) CD4+ T cells of colon in Gpr15gfp/+ mice. Peripheral lymph nodes (PLN), mesenteric lymph node (MLN), Peyer’s patches (PP), intraepithelial lymphocytes (IEL), lamina propria (LP), small intestine (SI). n = 9, except for colon and SI IELs, where n = 5; mean ± s.e.m. (b) Expression of activation and gut-trafficking molecules on GFP+ CD4+ cells of colon LP (black); CCR9 on GFP+ CD4+ T cells of SI (dashed); (c) cytokines and Treg cell-associated proteins on sorted colon LP GFP+ CD4+ T cells; isotype (gray shade). Representative of 3 experiments.
Supplementary Figure 2 GPR15 mediates accumulation of TEM and Treg cells in the mouse colon.
GPR15 mediates accumulation of TEM and Treg cells in the mouse colon. (a) Gpr15-KO (CD45.2) or het (CD45.2) bone marrow cells were combined with Gpr15-het (CD45.1) cells and transferred into irradiated hosts (CD45.1 × CD45.2 F1) to generate experimental (Exp) or control (Ctrl) chimeras, respectively. (b) Frequency of Gpr15-het and Gpr15-KO cells among CD4+ T subsets in experimental chimeras. (c) Splenocytes from DO11.10 Gpr15-het or DO11.10 Gpr15-KO were i.v. injected into Balb/c (Thy-1.1) mice. After 24 h, recipients were treated intra-rectally with OVA and CT. Accumulation of OVA-specific CD4+ T cells in tissues was assessed 5 days later. (d) Cells are gated on Gpr15-het or KO derived antigen-specific (DO11+) memory CD4+ T cells. (e) CFSE-labeled splenocytes from Gpr15-het (Thy-1.1, Thy-1.2) and KO (Thy-1.2) DO11 mice were co-injected i.v. in equal proportion into congenic non-DO11 hosts (Thy-1.1) on day 0. Recipients were treated with OVA and CT per rectum on day 1, FTY720 or PBS i.p. on day 3, and tissues were collected on day 5.
Supplementary Figure 3 Preferential colon-homing of GPR15-expressing effector CD4+ T cells.
Preferential colon-homing of GPR15-expressing effector CD4+ T cells. Allotype-marked Gpr15-het and KO CD4+ were cultured under TH17-polarizing conditions for 3 d, then injected into normal hosts. After 8-10 h, lymphocytes were isolated and the ratios of Gpr15-het to KO CD4+ T cells localized to the indicated organs were determined and normalized to that of the spleen. n = 4 recipients per group; mean ± s.e.m. (ANOVA with Tukey’s post test), *P < 0.05, **P < 0.001. In an independent experiment with 2 recipient mice, Gpr15-het cells displayed an even greater preference for localization to the colon; in that experiment the ratio of Gpr15-het to KO CD4+ cells was 10-11 fold higher in colon than in spleen in the recipients, whereas similar to the results presented here, there was no significant difference in het versus KO T cell localization to lymph nodes. NA: not available due to poor cell recovery from this SI.
Supplementary Figure 4 Similar susceptibility of Gpr15-KO and WT mice to DSS- and TNBS-induced colitis.
Similar susceptibility of Gpr15-KO and WT mice to DSS- and TNBS-induced colitis. (a) Similar weight loss of Gpr15-KO and wildtype Balb/c mice given drinking water containing 4.5% DSS (w/v) beginning day 0. (b) Representative H&E analysis of distal colon section and corresponding blinded histopathology score. Scale bar represents 20 μm. n = 3, mean + s.e.m. (c) Similar weight loss of Gpr15-KO and WT mice that were rectally instilled with TNBS (2 mg) on day 0. Combined results of 2 independent experiments. n = 7 Gpr15-KO, n = 6 WT, mean ± s.e.m. (d) Representative H&E analysis of distal colon section on day 4 and blinded histopathology score; n = 4 Gpr15-KO and n = 3 WT mice, mean + s.e.m. Scale bar represents 20 μm. Data representative of 2 independent experiments are shown.
Supplementary Figure 5 Similar TEM cell differentiation by Gpr15-het and KO cells.
Similar TEM cell differentiation by Gpr15-het and KO cells. (a) Naive CD45RBhi CD4+ T cells from Gpr15-KO (CD45.2) or het (CD45.1, CD45.2) mice were co-injected into Rag2-/- recipients in equal proportion. After two weeks, Gpr15-het- and KO-derived CD4+ T cells display similar frequencies of IFN-γ and IL-17 expression. Representative flow cytometry plots (b), non-normalized (c) and normalized data (d) are shown. (e) Naive CD4+ T cells from Gpr15-het or KO mice were injected into Rag2-/- recipients, and GPR15 (GFP+) CD4+ T cells were sorted from recipient colon or MLN after two weeks. (f) Expression of IFN-γ, IL-17, Foxp3 and Ki-67 by sorted GFP+ CD4+ T cells from pooled colon or MLN. Results of a single experiment performed are shown for comparison with the cytokine expression of total het- and KO-derived effector cells in (3b).
Supplementary Figure 6 Minimal Foxp3 mRNA expression by human colon GPR15+ memory CD4+ T cells, and comparison of GPR15 expression by resting and activated human Treg cells.
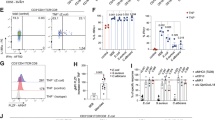
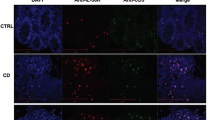
Minimal Foxp3 mRNA expression by human colon GPR15+ memory CD4+ T cells, and comparison of GPR15 expression by resting and activated human Treg cells. (a) Expression of GPR15, Foxp3 and II2ra in sorted human colon cells (as indicated) from 1 UC and 2 non-UC samples was determined by Realtime RT-PCR and normalized to GAPDH. n = 3, mean + s.e.m., *P < 0.05, unpaired Student’s t-test. (b) GPR15 staining of rested and activated human colon Treg cells. Human colonic lymphocytes were stained with polyclonal anti-GPR15 antibody pre or post activation with PMA and ionomycin at 37 °C. Cells are gated on CD45RO+ CD4+ T cells. (c,d) Colon T cell GPR15 expression in Crohn’s disease. Lymphocytes isolated from resectioned colon of 2 Crohn’s patients were activated and incubated with antibodies to GPR15 (or rabbit IgG isotype), Foxp3 and cytokines. Cells are gated on memory CD4+ T cells (CD4+, CD45RO+).
Supplementary Figure 7 Mouse-specific mutation in GATA-3 binding motif of Gpr15 enhancer region.
Mouse-specific mutation in GATA-3 binding motif of Gpr15 enhancer region. An ~3000 bp, evolutionarily conserved region downstream of the GPR15 gene contains a cluster of TFBSs that are capable of integrating known GPR15-inducing signals. The conserved sequence is embedded in a region that is transcriptionally active (positions indicated in the figure) in GPR15-expressing cells (GM12878) but not in non GPR15-expressing cells. Two MA0037.2 GATA-3 consensus sites (JASPAR transcription factor database) are conserved in primates but not rodents (see Figure 6; one of the two similar sites is shown). A destructive mouse-specific A-to-G mutation in a GATA-3 binding site (MA0037.1 motif) adjacent to the highly conserved STAT-6 binding site is highlighted in blue. GPR15 expression is also from the ENCODE consortium (NCBI GEO accession number GSE19090, Affymetrix exon expression array): GM12878 cells had a strong GPR15 signal (+++, raw expression value 2733.13 ± 232.82, n = 3), correlating with strong active promoter activity, whereas the other cells lines with repressive or only weak enhancer marks at the GPR15 enhancer locus lacked GPR15 expression (NS; expression value < 53 in each case).
Supplementary Figure 8 GATA-3 and Foxp3 binding in Treg cells.
GATA-3 and Foxp3 binding in Treg cells. (a) ChIP-Seq data showing binding of GATA3 (blue) in TH2 cells and FOXP3 (green) in nTreg cells at the human GPR15 locus (hg18 build). US, upstream site; DS, downstream site. Details as for Fig. 6. One ChIP experiment from each of the two donors from the study of Birzele and colleagues (ref. 42) is shown (donor 1 replicate 2 and donor 2 replicate 1). The accession numbers for the data are listed in the Supplementary Table 1. (b) As (a), except for Gata-3 and Foxp3 at the Gpr15 locus in the indicated mouse cells (mm9 build). (c) Position of the GPR15 enhancer in lists of FOXP3 binding sites ranked by P value, generated from replicate ChIP-seq experiments in human and mouse Treg cells. The binding sites are arranged with the most significant at the left down to the least significant (P =10-3) on the right. Binding sites with significance below the default MACS threshold of 10-5 are shown in green. The position of the GPR15 enhancer in each ranked list of binding sites is indicated by a black line, with its significance given above. In mouse iTreg cells, there are 2 binding sites within the enhancer (see (b)); the significance of the 5’ most binding site is shown, but the 3’ binding site has a similar P value. The human datasets are from Birzele and colleagues (ref. 42) and the mouse nTreg dataset is from Samstein et al. (ref 43).
Supplementary Figure 9 Assessment of specificity of polyclonal antibody to human GPR15 and comparison of staining to that of an anti-GPR15 monoclonal Ab.
Assessment of specificity of polyclonal antibody to human GPR15 and comparison of staining to that of an anti-GPR15 monoclonal Ab. (a) L1.2 cells stably transfected with the human GPR15 ORF and C-terminal GFP tag were incubated with 1 μg (black line) or 0.5 μg antibody (dashed), or were unstained (gray shade; left panel). Polyclonal antibody binds GFP+ cells in human GPR15 transfectant cells (middle panels). L1.2 cells stably expressing human GPR15 (black line), mouse GPR15 (dashed) or control vector (grey shade) were stained with 1 μg antibody, and there is greater binding of antibody to human transfectants (right panel). (b,c) Similar staining of colon CD4+ T cells by polyclonal (b) and monoclonal (c) antibody to human GPR15. Lymphocytes isolated from human colon were activated and incubated with GPR15-specific polyclonal (or rabbit IgG isotype) or monoclonal GPR15 antibody (or mouse IgG2B), Foxp3 and cytokines. Cells are gated on CD4+ CD45RO+ memory cells.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–9 and Supplementary Tables 1 and 2 (PDF 4462 kb)
Rights and permissions
About this article
Cite this article
Nguyen, L., Pan, J., Dinh, T. et al. Role and species-specific expression of colon T cell homing receptor GPR15 in colitis. Nat Immunol 16, 207–213 (2015). https://doi.org/10.1038/ni.3079
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.3079
This article is cited by
-
Timely T cell recruitment protects against viral myocarditis
Nature Cardiovascular Research (2023)
-
Regulation of psoriasis, colitis, and the intestinal microbiota by clusterin
Scientific Reports (2023)
-
Dietary L-Tryptophan consumption determines the number of colonic regulatory T cells and susceptibility to colitis via GPR15
Nature Communications (2023)
-
Protective Effect of Saffron in Mouse Colitis Models Through Immune Modulation
Digestive Diseases and Sciences (2022)
-
Coordinated co-migration of CCR10+ antibody-producing B cells with helper T cells for colonic homeostatic regulation
Mucosal Immunology (2021)