Abstract
The cellular dynamics of the egress of lymphocytes from lymph nodes are poorly defined. Here we visualized the branched organization of lymph node cortical sinuses and found that after entry, some T cells were retained, whereas others returned to the parenchyma. T cells deficient in sphingosine 1-phosphate receptor type 1 probed the sinus surface but failed to enter the sinuses. In some sinuses, T cells became rounded and moved unidirectionally. T cells traveled from cortical sinuses into macrophage-rich sinus areas. Many T cells flowed from medullary sinuses into the subcapsular space. We propose a multistep model of lymph node egress in which cortical sinus probing is followed by entry dependent on sphingosine 1-phosphate receptor type 1, capture of cells in a sinus region with flow, and transport to medullary sinuses and the efferent lymph.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Change history
16 January 2009
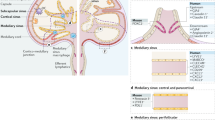
NOTE: In the version of this article initially published, the vessel label ‘Afferent’ beneath the lymph node in Fig. 1c is incorrect. The correct label is ‘Efferent’. The error has been corrected in the HTML and PDF versions of the article.
References
Schwab, S.R. & Cyster, J.G. Finding a way out: lymphocyte egress from lymphoid organs. Nat. Immunol. 8, 1295–1301 (2007).
von Andrian, U.H. & Mempel, T.R. Homing and cellular traffic in lymph nodes. Nat. Rev. Immunol. 3, 867–878 (2003).
Pappu, R. et al. Promotion of lymphocyte egress into blood and lymph by distinct sources of sphingosine-1-phosphate. Science 316, 295–298 (2007).
Rosen, H. & Goetzl, E.J. Sphingosine 1-phosphate and its receptors: an autocrine and paracrine network. Nat. Rev. Immunol. 5, 560–570 (2005).
Picker, L.J. & Siegelman, M.H. in Fundamental Immunology Vol. 4. (ed. Paul, W.E.) 479–531 (Lippincott-Raven, Philadelphia, 1999).
Wei, S.H. et al. Sphingosine 1-phosphate type 1 receptor agonism inhibits transendothelial migration of medullary T cells to lymphatic sinuses. Nat. Immunol. 6, 1228–1235 (2005).
Prevo, R., Banerji, S., Ni, J. & Jackson, D.G. Rapid plasma membrane-endosomal trafficking of the lymph node sinus and high endothelial venule scavenger receptor/homing receptor stabilin-1 (FEEL-1/CLEVER-1). J. Biol. Chem. 279, 52580–52592 (2004).
Hirakawa, S. et al. VEGF-A induces tumor and sentinel lymph node lymphangiogenesis and promotes lymphatic metastasis. J. Exp. Med. 201, 1089–1099 (2005).
Pham, T.H., Okada, T., Matloubian, M., Lo, C.G. & Cyster, J.G. S1P1 receptor signaling overrides retention mediated by Gαi–coupled receptors to promote T cell egress. Immunity 28, 122–133 (2008).
Belisle, C. & Sainte-Marie, G. Tridimensional study of the deep cortex of the rat lymph node. III. Morphology of the deep cortex units. Anat. Rec. 199, 213–226 (1981).
Kelly, R.H. Functional anatomy of lymph nodes. I. The paracortical cords. Int. Arch. Allergy Appl. Immunol. 48, 836–849 (1975).
He, Y. Scanning electron microscope studies of the rat mesenteric lymph node with special reference to high-endothelial venules and hitherto unknown lymphatic labyrinth. Arch. Histol. Jpn. 48, 1–15 (1985).
Sanna, M.G. et al. Enhancement of capillary leakage and restoration of lymphocyte egress by a chiral S1P1 antagonist in vivo. Nat. Chem. Biol. 2, 434–441 (2006).
Martens, J.H. et al. Differential expression of a gene signature for scavenger/lectin receptors by endothelial cells and macrophages in human lymph node sinuses, the primary sites of regional metastasis. J. Pathol. 208, 574–589 (2006).
Phan, T.G., Grigorova, I., Okada, T. & Cyster, J.G. Subcapsular encounter and complement-dependent transport of immune complexes by lymph node B cells. Nat. Immunol. 8, 992–1000 (2007).
Yamada, S., Kubo, M. & Hayashida, Y. Lymph flow dynamics into the thoracic duct of the rat. Jpn. J. Physiol. 38, 729–733 (1988).
Dahan, A., Mendelman, A., Amsili, S., Ezov, N. & Hoffman, A. The effect of general anesthesia on the intestinal lymphatic transport of lipophilic drugs: comparison between anesthetized and freely moving conscious rat models. Eur. J. Pharm. Sci. 32, 367–374 (2007).
Nombela-Arrieta, C. et al. A central role for DOCK2 during interstitial lymphocyte motility and sphingosine-1-phosphate-mediated egress. J. Exp. Med. 204, 497–510 (2007).
Kunkel, E.J. & Butcher, E.C. Chemokines and the tissue-specific migration of lymphocytes. Immunity 16, 1–4 (2002).
Ley, K., Laudanna, C., Cybulsky, M.I. & Nourshargh, S. Getting to the site of inflammation: the leukocyte adhesion cascade updated. Nat. Rev. Immunol. 7, 678–689 (2007).
Nicander, L., Nafstad, P., Landsverk, T. & Engebretsen, R.H. A study of modified lymphatics in the deep cortex of ruminant lymph nodes. J. Anat. 178, 203–212 (1991).
Compton, C.C. & Raviola, E. Structure of the sinus-lining cells in the popliteal lymph node of the rabbit. Anat. Rec. 212, 408–423 (1985).
Dickstein, J.B., Hay, J.B., Lue, F.A. & Moldofsky, H. The relationship of lymphocytes in blood and in lymph to sleep/wake states in sheep. Sleep 23, 185–190 (2000).
Engeset, A., Sokolowski, J. & Olszewski, W.L. Variation in output of leukocytes and erythrocytes in human peripheral lymph during rest and activity. Lymphology 10, 198–203 (1977).
Schwab, S.R. et al. Lymphocyte sequestration through S1P lyase inhibition and disruption of S1P gradients. Science 309, 1735–1739 (2005).
Stachowiak, A.N., Wang, Y., Huang, Y.C. & Irvine, D.J. Homeostatic lymphoid chemokines synergize with adhesion ligands to trigger T and B lymphocyte chemokinesis. J. Immunol. 177, 2340–2348 (2006).
Mueller, S.N. et al. Regulation of homeostatic chemokine expression and cell trafficking during immune responses. Science 317, 670–674 (2007).
Davis, M.D., Clemens, J.J., Macdonald, T.L. & Lynch, K.R. Sphingosine 1-phosphate analogs as receptor antagonists. J. Biol. Chem. 280, 9833–9841 (2005).
Frost, P. Further evidence for the role of macrophages in the initiation of lymphocyte trapping. Immunology 27, 609–616 (1974).
Egen, J.G. et al. Macrophage and T cell dynamics during the development and disintegration of mycobacterial granulomas. Immunity 28, 271–284 (2008).
van den Berg, T.K. et al. Sialoadhesin on macrophages: its identification as a lymphocyte adhesion molecule. J. Exp. Med. 176, 647–655 (1992).
Suzuki, K., Kumanogoh, A. & Kikutani, H. Semaphorins and their receptors in immune cell interactions. Nat. Immunol. 9, 17–23 (2008).
Crivellato, E. & Mallardi, F. The sinus endothelial cell architecture in the mouse lymph node. Structural peculiarities and close correlation with the fibroblastic reticular cells. J. Submicrosc. Cytol. Pathol. 30, 495–502 (1998).
Heath, T.J. & Spalding, H.J. Pathways of lymph flow to and from the medulla of lymph nodes in sheep. J. Anat. 155, 177–188 (1987).
Baluk, P. et al. Functionally specialized junctions between endothelial cells of lymphatic vessels. J. Exp. Med. 204, 2349–2362 (2007).
Matloubian, M. et al. Lymphocyte egress from thymus and peripheral lymphoid organs is dependent on S1P receptor 1. Nature 427, 355–360 (2004).
Allen, C.D., Okada, T., Tang, H.L. & Cyster, J.G. Imaging of germinal center selection events during affinity maturation. Science 315, 528–531 (2007).
Lo, C.G., Xu, Y., Proia, R.L. & Cyster, J.G. Cyclical modulation of sphingosine-1-phosphate receptor 1 surface expression during lymphocyte recirculation and relationship to lymphoid organ transit. J. Exp. Med. 201, 291–301 (2005).
Okada, T. et al. Antigen-engaged B cells undergo chemotaxis toward the T zone and form motile conjugates with helper T cells. PLoS Biol. 3, e150 (2005).
Acknowledgements
We thank A. Bullen and M. Krummel for help with the two-photon microscope; R. Proia (US National Cancer Institute) for S1P1-deficient mice; L. Shiow for help with movie preparation; and J. An for colony management. Supported by the Cancer Research Institute (I.L.G.), the Irvington Institute for Immunological Research (S.R.S.), the National Health and Medical Research Council and American Australian Association (T.G.P.), the Boyer Graduate Program in the Biochemical Sciences (T.H.M.P.), the Howard Hughes Medical Institute (J.G.C.) and the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
All authors contributed to the design of the research; I.L.G. did most of the experiments; S.R.S. did several explant experiments; T.G.P. and T.O. helped to establish the intravital imaging and labeling procedures and assisted in some experiments; T.H.M.P. helped with Edg1−/− fetal liver chimera preparation; I.L.G., S.R.S. and J.G.C. analyzed the data; and I.L.G. and J.G.C. prepared the manuscript.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–4 and Methods (PDF 3800 kb)
Supplementary Movie 1
LYVE-1+ cortical sinus structure. The first part of the movie shows a three-dimensional (3-D) reconstruction of a 214 μm z-stack through a LYVE-1+ structure imaged by two photon microscopy from the cortical side of an explanted inguinal lymph node. The second part of the movie shows a z stack of this same region that starts close to the capsule and extends deeper into the lymph node. LYVE-1+ sinuses were labeled with anti-LYVE-1 (green) and T cells with CMTMR (red). LYVE-1+ structures filled with LYVE-1+ signal are capsule-proximal regions packed with LYVE-1+ macrophages (MΦ). Deeper into the lymph node sinuses have well-defined borders and no meshwork of LYVE-1+ signal inside. (MOV 7721 kb)
Supplementary Movie 2
Cortical sinus entry of T cells is dependent on S1P1 (30 minutes). Time-lapse image sequence of 18 μz-projection shows a fragment of a LYVE-1+ cortical sinus labeled to detect LYVE-1 (red) and Edg1+/+ (GFP, green) and Edg1−/− (CMTMR, red) T cells. In the first image sequence, the tracks of several T cells that contacted the sinus border are highlighted by dots. The dots change from white to yellow if cell entry occurs. For clarity only some of the T cells that made contact are displayed with such tracks. The second image sequence is a replay of the first, now using white and yellow arrows to register correspondingly Edg1+/+ and Edg1−/− T cells in contact with the outer border of the LYVE-1+ sinus. The arrows appear only if the next step of the T cell is transmigration or departure from the sinus border within the time and z stack of the movie. White circles indicate the time and location where a T cell transmigrated into the sinus. The asterix highlights two cells that entered at a similar location. The score indicates the number of T cell contacts with the sinus outer border versus the number of entries into the sinus. Elapsed time is shown as mm:ss. (MOV 7721 kb)
Supplementary Movie 3
LYVE-1+ cortical sinus probing by Edg1+/+ and Edg1−/− T cells during entry decision-making (30 minutes). Two-photon microscopy of explanted inguinal lymph node. Four time-lapse image sequences of 2, 1, 2 or 2 z-planes, correspondingly, that contain fragments of LYVE-1+ cortical sinuses (green) and T cells approaching them from the parenchyma (Edg1+/+, double labeled with CFSE and CMTMR, yellow, or Edg1−/−, CMTMR, red). White arrows point to the imaged cells and their processes. Elapsed time is shown as mm:ss. (MOV 2335 kb)
Supplementary Movie 4
Drainage of PE into the medullary sinuses (30 minutes). Two-photon intravital microscopy of the medullary region of the inguinal lymph node ∼5 min after R-PE injection into the tail of the mouse. The two time-lapse image sequences represent superficial (closer to the capsule) and somewhat deeper 15 μm z-projections. The movie shows gradual drainage of R-PE (red) into the medullary sinuses of the lymph node. Medullary LYVE-1+ structures are labeled by anti-LYVE-1 (green). Edg1+/+ T cells (GFP, yellow) and Edg1−/− T cells (red) were both labeled with CMTMR. Elapsed time is shown as mm:ss. (MOV 6861 kb)
Supplementary Movie 5
Flow of cells inside LYVE-1+ cortical sinuses. Two-photon intravital microscopy of inguinal lymph node. Cortical LYVE-1+ structure was volume-rendered at the mid-point of the imaging period. The structure was subdivided into MΦ–rich sinus area (red) and cortical sinuses (yellow) as described in Methods. Tracks in various colors represent trajectories of Edg1+/+ T cells inside interconnected regions of LYVE-1+ sinuses. The first part of the movie shows a rotation of the 3-D image with rendered structures and cell trajectories. The second segment is a 30 min movie that shows movement of Edg1+/+ T cells (green, center of their coordinates are indicated with gray spheres) in the regions of LYVE-1+ sinuses with flow. Note that there was a small shift in the lymph node over the course of the experiment and this causes the single volume-rendered structure that is displayed to not fully superimpose with track locations at all time points. Elapsed time is shown as mm:ss. (MOV 8155 kb)
Supplementary Movie 6
Flow of cells in medullary region (30 minutes). Two-photon intravital microscopy of inguinal lymph node from the medullary side. LYVE-1+ medullary structures were labeled with anti-LYVE-1 (green). Edg1+/+ T cells (GFP, yellow) and Edg1−/− T cells (red) were both labeled with CMTMR. Wild-type B cells (CFP, blue) are also present. The two time-lapse image sequences represent a superficial (closer to the capsule) 15 μm z-projection and a somewhat deeper 18 μm z-projection. The left segment of the deeper view shows cells moving from a sinus that is surrounded by T cells and containing little internal LYVE-1 (macrophage) signal, into a sinus region with few surrounding T cells and containing internal LYVE-1 signal. This view is suggested to correspond to a cortical to medullary sinus connection. Elapsed time is shown as mm:ss. (MOV 4498 kb)
Supplementary Movie 7
T cell motility in the medullary region (30 minutes). Two-photon intravital microscopy of inguinal lymph node from the medullary side. Labeled to detect LYVE-1+ medullary structures (green), Edg1+/+ T cells (GFP, yellow), Edg1−/− T cells (red) and B cells (CFP, blue). Time-lapse image sequences represent 18 μm z-projection. Elapsed time is shown as mm:ss. (MOV 7001 kb)
Supplementary Movie 8
Cell exit from medullary sinuses into subcapsular space (30 minutes). Two-photon intravital microscopy of Edg1+/+ (yellow) T cells in the medullary region of the lymph node. The time-lapse image sequence represents a superficial 18 μm z-projection and shows cells that are exiting through the medullary sinus into the space beneath the capsule. Medullary LYVE-1+ structures are labeled by anti-LYVE-1 (green). Arrows in both movies indicate the same cells. Elapsed time is shown as mm:ss. See also Figure 5D. (MOV 6835 kb)
Supplementary Movie 9
Flow of cells beneath the capsule at the medullary side (20 minutes). Two-photon intravital microscopy of the medullary region of the lymph node. Labeled to detect medullary LYVE-1+ structures (green), Edg1+/+ T cells (GFP, yellow), Edg1−/− T cells (red), and B cells (CFP, blue). The two time-lapse image sequences represent a superficial (closer to the capsule) 15 μm z-projection, and a deeper 15 μm z-projection. Elapsed time is shown as mm:ss. (MOV 4114 kb)
Rights and permissions
About this article
Cite this article
Grigorova, I., Schwab, S., Phan, T. et al. Cortical sinus probing, S1P1-dependent entry and flow-based capture of egressing T cells. Nat Immunol 10, 58–65 (2009). https://doi.org/10.1038/ni.1682
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.1682
This article is cited by
-
Sphingosine 1-phosphate modulation and immune cell trafficking in inflammatory bowel disease
Nature Reviews Gastroenterology & Hepatology (2022)
-
Intravital three-photon microscopy allows visualization over the entire depth of mouse lymph nodes
Nature Immunology (2022)
-
The role of bile acids in carcinogenesis
Cellular and Molecular Life Sciences (2022)
-
Lymphatic endothelial cells of the lymph node
Nature Reviews Immunology (2020)
-
A robust in vitro model for trans-lymphatic endothelial migration
Scientific Reports (2017)