Abstract
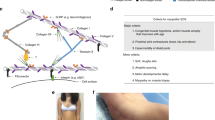
Among the diverse family of collagens, the widely expressed microfibrillar type VI collagen is believed to play a role in bridging cells with the extracellular matrix. Several observations imply substrate properties for cell attachment1 as well as association with major collagen fibers2. Previously, we have established genetic linkage between the genes encoding the three constituent α-chains of type VI collagen and Bethlem myopathy3–5. A distinctive feature of this autosomal dominant disorder consists of contractures of multiple joints in addition to generalized muscular weakness and wasting6–10. Nine kindreds show genetic linkage to the COL6A1–COL6A2 cluster on chromosome 21q22.3 (refs 3,4; manuscript submitted) whereas one family shows linkage to markers on chromosome 2q37 close to COL6A3 (ref. 5). Sequence analysis in four families reveals a mutation in COL6A1 in one and a COL6A2 mutation in two other kindreds. Both mutations disrupt the Gly-X-Y motif of the triple helical domain by substitution of Gly for either Val or Ser. Analogous to the putative perturbation of the anchoring function of the dystrophin-associated complex in congenital muscular dystrophy with mutations in the α2-subunit of laminin, our observations suggest a similar mechanism in Bethlem myopathy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Stallcup, W.B., Dahlin, K. & Healy, P. Interaction of the NG2 chondroitin sulfate proteoglycan with collagen type VI. J. Cell Biol. 111, 3177–3188 (1990).
Bonaldo, P., Russo, V., Bucciotti, F., Doliana, R. & Colombatti, A. Structural and functional features of the alpha 3 chain indicate a bridging role for chicken collagen VI in connective tissues. Biochemistry 29, 1245–1254 (1990).
Jöbsis, G.J., Barth, P.G., Boers, J.M., Baas, F., Bolhuis, P.A. & de Visser, M. Bethlem myopathy: clinical and genetic aspects. Neurology 45, 881S (1995).
Jöbsis, G.J. et al. Genetic localization of Bethlem myopathy. Neurology 46, 779–782 (1996).
Speer, M.C. et al. Evidence for locus heterogeneity in the Bethlem myopathy and linkage to 2q37. Hum. Mol. Genet. 5, 1043–1046 (1996).
Bethlem, J. & van Wijngaarden, G.K. Benign myopathy, with autosomal dominant inheritance: a report on three pedigrees. Brain 99, 91–100 (1976).
Mohire, M.D. et al. Early-onset benign autosomal dominant limb-girdle myopathy with contractures (Bethlem myopathy). Neurology 38, 573–580 (1988).
Boers, J.M. Een congenitale myopathie met contracturen. Thesis, University of Amsterdam, 1984).
Arts, W.F., Bethlem, J. & Volkers, W.S. Further investigations on benign myopathy with autosomal dominant inheritance. J. Neurol. 217, 201–206 (1978).
Merlini, L. et al. Bethlem myopathy: early-onset benign autosomal dominant myopathy with contractures. Description of two new families. Neuromusc. Disord. 4, 503–511 (1994).
Renieri, A. et al. Mutation scanning of the entire COL4A5 coding sequence in Alport syndrome and genotype-phenotype correlation. Am. J. Hum. Genet. 57, A9 (1995).
Vogel, B.E. et al. A substitution of cysteine for glycine 748 of the a1 chain produces a kink at this site in the procollagen I molecule and an altered N-proteinase cleavage site over 225 nm away. J. Biol. Chem. 263, 19249–19255 (1988).
Steinmann, B. & Raghunath, M. Delayed helix formation of mutant collagen. Science 267, 258 (1995).
Romanic, A.M. et al. Self-assembly of collagen I from a proband homozygous for a mutation that substituted serine for glycine at position 661 in the alpha 2 (I) chain; possible relationship between the effects of mutations on critical concentration and the severity of the phenotype. J. Biol. Chem. 269, 11614–11619 (1994).
Swasdison, S. & Mayne, R. Location of the integrin complex and extracellular matrix molecules at the chicken myotendinous junction. Cell Tissue Res. 257, 537–543 (1989).
Hessle, H. & Engvall, E. Type VI collagen; studies on its localization, structure, and biosynthetic form with monoclonal antibodies. J. Biol. Chem. 259, 3955–3961 (1984).
von der Mark, H., Aumailley, M., Wick, G., Fleischmajer, R. & Timpl, R. Immunochemistry, genuine size and tissue localization of collagen VI. Eur. J. Biochem. 142, 493–502 (1984).
Mochizuki, T. et al. Identification of mutations in the α3 (IV) and α4 (IV) collagen genes in autosomal recessive Alport syndrome. Nature Genet. 8, 77–81 (1994).
Ibrahimi, A. et al. Cloning of α2 chain of type VI collagen and expression during mouse development. Biochem. J. 289, 141–147 (1993).
Ozawa, E. et al. Dystrophin-associated proteins in muscular dystrophy. Hum. Mol. Genet. 4, 1171–1716 (1995).
Lim, L.E. et al. β-sarcoglycan: characterization and role in limb-girdle muscular dystrophy linked to 4q12. Nature Genet. 11, 257–265 (1995).
Bönnemann, C.G. et al. β-sarcoglycan (A3b) mutations cause autosomal recessive muscular dystrophy with loss of the sarcoglycan complex. Nature Genet. 11, 266–273 (1995).
Helbling-Leclerc, A. et al. Mutations in the laminin alpha 2-chain gene (LAMA2) cause merosin-deficient congenital muscular dystrophy. Nature Genet. 11, 216–218 (1995).
Xu, H., Wu, X.R., Wewer, U.M. & Engvall, E. Murine muscular dystrophy caused by a mutation in the laminin β2 (Lama2) gene. Nature Genet. 8, 297–302 (1994).
Schäffer, A.A., Grupta, S.K., Shriram, K. & Cottingham, R.W. Avoiding recomputation in linkage analysis. Hum. Hered. 44, 225–237 (1994).
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Jöbsis, G., Keizers, H., Vreijling, J. et al. Type VI collagen mutations in Bethlem myopathy, an autosomal dominant myopathy with contractures. Nat Genet 14, 113–115 (1996). https://doi.org/10.1038/ng0996-113
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ng0996-113
This article is cited by
-
Single-nucleus transcriptomics reveals functional compartmentalization in syncytial skeletal muscle cells
Nature Communications (2020)
-
Quantitative proteomics and single-nucleus transcriptomics of the sinus node elucidates the foundation of cardiac pacemaking
Nature Communications (2019)
-
siRNA-mediated Allele-specific Silencing of a COL6A3 Mutation in a Cellular Model of Dominant Ullrich Muscular Dystrophy
Molecular Therapy - Nucleic Acids (2014)
-
ColVI myopathies: where do we stand, where do we go?
Skeletal Muscle (2011)