Abstract
Tissue repair is fundamental to our survival as tissues are challenged by recurrent damage. During mammalian skin repair, cells respond by migrating and proliferating to close the wound. However, the coordination of cellular repair behaviours and their effects on homeostatic functions in a live mammal remains unclear. Here we capture the spatiotemporal dynamics of individual epithelial behaviours by imaging wound re-epithelialization in live mice. Differentiated cells migrate while the rate of differentiation changes depending on local rate of migration and tissue architecture. Cells depart from a highly proliferative zone by directionally dividing towards the wound while collectively migrating. This regional coexistence of proliferation and migration leads to local expansion and elongation of the repairing epithelium. Finally, proliferation functions to pattern and restrict the recruitment of undamaged cells. This study elucidates the interplay of cellular repair behaviours and consequent changes in homeostatic behaviours that support tissue-scale organization of wound re-epithelialization.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Change history
07 March 2017
Owing to technical problems, this Article was published online later than the date given in the print version. The published date should read '1 March 2017', and is correct in the online versions.
References
Eming, S., Martin, P. & Tomic-Canic, M. Wound repair and regeneration: mechanisms, signaling, and translation. Sci. Trans. Med. 6, 265sr6 (2014).
Gurtner, G., Werner, S., Barrandon, Y. & Longaker, M. Wound repair and regeneration. Nature 453, 314–321 (2008).
Clark, R. A., Ghosh, K. & Tonnesen, M. G. Tissue engineering for cutaneous wounds. J. Invest. Dermatol. 127, 1018–1029 (2007).
Simpson, C. L., Patel, D. M. & Green, K. J. Deconstructing the skin: cytoarchitectural determinants of epidermal morphogenesis. Nat. Rev. Mol. Cell Biol. 12, 565–580 (2011).
Fuchs, E. & Raghavan, S. Getting under the skin of epidermal morphogenesis. Nat. Rev. Genet. 3, 199–209 (2002).
Xin, T., Greco, V. & Myung, P. Hardwiring stem cell communication through tissue structure. Cell 164, 1212–1225 (2016).
Mesa, K. R., Rompolas, P. & Greco, V. The dynamic duo: niche/stem cell interdependency. Stem Cell Rep. 4, 961–966 (2015).
Kandyba, E. E., Hodgins, M. B. & Martin, P. E. A murine living skin equivalent amenable to live-cell imaging: analysis of the roles of connexins in the epidermis. J. Invest. Dermatol. 128, 1039–1049 (2008).
Liang, C.-C. C., Park, A. Y. & Guan, J.-L. L. In vitro scratch assay: a convenient and inexpensive method for analysis of cell migration in vitro. Nat. Protoc. 2, 329–333 (2007).
Hertle, M. D., Kubler, M. D., Leigh, I. M. & Watt, F. M. Aberrant integrin expression during epidermal wound healing and in psoriatic epidermis. J. Clin. Invest. 89, 1892–1901 (1992).
Nunan, R. et al. Ephrin-Bs drive junctional downregulation and actin stress fiber disassembly to enable wound re-epithelialization. Cell Rep. 13, 1380–1395 (2015).
Safferling, K. et al. Wound healing revised: a novel reepithelialization mechanism revealed by in vitro and in silico models. J. Cell Biol. 203, 691–709 (2013).
Bereiter-Hahn, J. in Biology of the Integument 2 Vertebrates Ch. 23, 443–471 (Springer-Verlag, 1986).
Christophers, E. Some observations on stratum corneum. Curr. Med. Res. Opin. 7, 26–28 (1982).
Coulombe, P. A. & Takahashi, K. The cellular mechanisms of keratinocyte migration into a skin wound site: an open question with important implications. Cell Vision 3, 217–223 (1996).
Danjo, Y. & Gipson, I. K. Specific transduction of the leading edge cells of migrating epithelia demonstrates that they are replaced during healing. Exp. Eye Res. 74, 199–204 (2002).
Zhao, M., Song, B., Pu, J., Forrester, J. V. & McCaig, C. D. Direct visualization of a stratified epithelium reveals that wounds heal by unified sliding of cell sheets. FASEB J. 17, 397–406 (2003).
Usui, M. L. et al. Morphological evidence for the role of suprabasal keratinocytes in wound reepithelialization. Wound Repair Regen. 13, 468–479 (2005).
Radice, G. P. The spreading of epithelial cells during wound closure in Xenopus larvae. Dev. Biol. 76, 26–46 (1980).
Brown, S. & Greco, V. Stem cells in the wild: understanding the world of stem cells through intravital imaging. Cell Stem Cell 15, 683–686 (2014).
Tumbar, T. et al. Defining the epithelial stem cell niche in skin. Science 303, 359–363 (2004).
Yang, H., Ganguly, A. & Cabral, F. Inhibition of cell migration and cell division correlates with distinct effects of microtubule inhibiting drugs. J. Biol. Chem. 285, 32242–32250 (2010).
Ganguly, A., Yang, H., Sharma, R., Patel, K. D. & Cabral, F. The role of microtubules and their dynamics in cell migration. J. Biol. Chem. 287, 43359–43369 (2012).
Hsu, Y.-C. C., Li, L. & Fuchs, E. Emerging interactions between skin stem cells and their niches. Nat. Med. 20, 847–856 (2014).
Odland, G. & Ross, R. Human wound repair I. Epidermal regeneration. J. Cell Biol. 39, 135–151 (1968).
Matoltsy, A. G. & Viziam, C. B. Further observations on epithelialization of small wounds: an autoradiographic study of incorporation and distribution of 3H-thymidine in the epithelium covering skin wounds. J. Invest. Dermatol. 55, 20–25 (1970).
Subach, F. V. et al. Photoactivatable mCherry for high-resolution two-color fluorescence microscopy. Nat. Methods 6, 153–159 (2009).
Rompolas, P. et al. Spatiotemporal coordination of stem cell commitment during epidermal homeostasis. Science 352, 1471–1474 (2016).
Tscharntke, M. et al. Impaired epidermal wound healing in vivo upon inhibition or deletion of Rac1. J. Cell. Sci. 120, 1480–1490 (2007).
Werner, S. et al. The function of KGF in morphogenesis of epithelium and reepithelialization of wounds. Science 266, 819–822 (1994).
Repertinger, S. K. et al. EGFR enhances early healing after cutaneous incisional wounding. J. Invest. Dermatol. 123, 982–989 (2004).
Patel, G. K., Wilson, C. H., Harding, K. G., Finlay, A. Y. & Bowden, P. E. Numerous keratinocyte subtypes involved in wound re-epithelialization. J. Invest. Dermatol. 126, 497–502 (2006).
Das, T. et al. A molecular mechanotransduction pathway regulates collective migration of epithelial cells. Nat. Cell Biol. 17, 276–287 (2015).
Guirao, B. et al. Unified quantitative characterization of epithelial tissue development. eLife 4, e08519 (2015).
Shaw, T. J. & Martin, P. Wound repair at a glance. J. Cell. Sci. 122, 3209–3213 (2009).
Shaw, T. J. & Martin, P. Wound repair: a showcase for cell plasticity and migration. Curr. Opin. Cell Biol. 42, 29–37 (2016).
Margadant, C. et al. Integrin α3β1 inhibits directional migration and wound re-epithelialization in the skin. J. Cell. Sci. 122, 278–288 (2009).
Razzell, W., Wood, W. & Martin, P. Recapitulation of morphogenetic cell shape changes enables wound re-epithelialisation. Development 141, 1814–1820 (2014).
Michalik, L. et al. Impaired skin wound healing in peroxisome proliferator-activated receptor (PPAR)α and PPARβ mutant mice. J. Cell Biol. 154, 799–814 (2001).
Jameson, J. et al. A role for skin gammadelta T cells in wound repair. Science 296, 747–749 (2002).
Keyes, B. E. et al. Impaired epidermal to dendritic T cell signaling slows wound repair in aged skin. Cell 167, 1323–1338.e14 (2016).
Chernyavsky, A. I., Arredondo, J., Wess, J., Karlsson, E. & Grando, S. A. Novel signaling pathways mediating reciprocal control of keratinocyte migration and wound epithelialization through M3 and M4 muscarinic receptors. J. Cell Biol. 166, 261–272 (2004).
Vaezi, A., Bauer, C., Vasioukhin, V. & Fuchs, E. Actin cable dynamics and Rho/Rock orchestrate a polarized cytoskeletal architecture in the early steps of assembling a stratified epithelium. Dev. Cell 3, 367–381 (2002).
Song, X. et al. ERBB3-independent activation of the PI3K pathway in EGFR-mutant lung adenocarcinomas. Cancer Res. 75, 1035–1045 (2015).
Xie, W., Chow, L. T., Paterson, A. J., Chin, E. & Kudlow, J. E. Conditional expression of the ErbB2 oncogene elicits reversible hyperplasia in stratified epithelia and up-regulation of TGFα expression in transgenic mice. Oncogene 18, 3593–3607 (1999).
Pruitt, S. C., Freeland, A., Rusiniak, M. E., Kunnev, D. & Cady, G. K. Cdkn1b overexpression in adult mice alters the balance between genome and tissue ageing. Nat. Commun. 4, 2626 (2013).
Madisen, L. et al. A robust and high-throughput Cre reporting and characterization system for the whole mouse brain. Nat. Neurosci. 13, 133–140 (2010).
Muzumdar, M. D., Tasic, B., Miyamichi, K., Li, L. & Luo, L. A global double-fluorescent Cre reporter mouse. Genesis 45, 593–605 (2007).
Vasioukhin, V., Degenstein, L., Wise, B. & Fuchs, E. The magical touch: genome targeting in epidermal stem cells induced by tamoxifen application to mouse skin. Proc. Natl Acad. Sci. USA 96, 8551–8556 (1999).
Barker, J. H. et al. The hairless mouse ear: an in vivo model for studying wound neovascularization. Wound Repair Regen. 2, 138–143 (1994).
Auffray, C. et al. Monitoring of blood vessels and tissues by a population of monocytes with patrolling behavior. Science 317, 666–670 (2007).
Rompolas, P., Mesa, K. R. & Greco, V. Spatial organization within a niche as a determinant of stem-cell fate. Nature 502, 513–518 (2013).
Rompolas, P. et al. Live imaging of stem cell and progeny behaviour in physiological hair-follicle regeneration. Nature 487, 496–499 (2012).
Pineda, C. M. et al. Intravital imaging of hair follicle regeneration in the mouse. Nat. Protoc. 10, 1116–1130 (2015).
Tomasz, M. Mitomycin C: small, fast and deadly (but very selective). Chem. Biol. 2, 575–579 (1995).
Rieder, C. L. & Palazzo, R. E. Colcemid and the mitotic cycle. J. Cell Sci. 102, 387–392 (1992).
Dunlap, M. K. & Donaldson, D. J. Inability of colchicine to inhibit newt epidermal cell migration or prevent concanavalin A-mediated inhibition of migration. Studies in vivo. Exp. Cell Res. 116, 15–19 (1978).
Mesa, K. R. et al. Niche-induced cell death and epithelial phagocytosis regulate hair follicle stem cell pool. Nature 522, 94–97 (2015).
Zito, G. et al. Spontaneous tumour regression in keratoacanthomas is driven by Wnt/retinoic acid signalling cross-talk. Nat. Commun. 5, 3543 (2014).
Deschene, E. R. et al. β-catenin activation regulates tissue growth non-cell autonomously in the hair stem cell niche. Science 343, 1353–1356 (2014).
Acknowledgements
We thank E. Fuchs (Rockefeller University, USA) for the K14-H2BGFP, K14-actinGFP, K14-rtTA mice; K. Politi (Yale, USA) for the TetO-Cre mice; and V. V. Verkhusha (Albert Einstein, USA) for the PAmCherry construct. We thank the Marine Biological Laboratory (MBL, USA) for their support while writing this manuscript; S. Williams (UNC, USA), M. Schober (NYU, USA) and M. Lee for critical feedback; and S. Werner (ETH, Switzerland), R. Clark (Stony Brook, USA) and P. Martin (Bristol University, UK) for their constructive criticism of this work. V.G. is supported by the National Institute of Arthritis and Musculoskeletal and Skin Disease (NIAMS), NIH, grants no. 5R01AR063663-04 and 1R01AR067755-01A1 and by a Mallinckrodt Scholar Award. V.G. is a New York Stem Cell Foundation Robertson Investigator and a HHMI Scholar. S.P. was supported by the James Hudson Brown-Alexander Brown Coxe Postdoctoral Fellowship and is currently supported by the CT Stem Cell Grant 14-SCA-YALE-05. D.G.G. and A.M.H. are supported by the Yale Rheumatic Disease Research Core Center (P30 AR053495-08). K.R.M. was and S.B. is supported by the NIH Predoctoral Program in Cellular and Molecular Biology, grant no. T32GM007223. K.R.M. is currently supported by the NSF Graduate Research Fellow. E.D.M. is supported by the National Institutes of Health, grant no. T32 GM007499. P.R. was a New York Stem Cell Foundation-Druckenmiller Fellow and was supported by the CT Stem Cell Grant 13-SCA-YALE-20. K.C. is supported by a Canadian Institutes of Health Research Postdoctoral Fellowship. Y.B. is supported by CNRS, INSERM, Institut Curie, ERC Advanced (TiMoprh, 340784), ARC (SL220130607097), ANR Labex DEEP (11-LBX-0044, ANR-10-IDEX-0001-02) and PSL grants.
Author information
Authors and Affiliations
Contributions
S.P. and V.G. designed experiments and wrote the manuscript. S.P. performed the experiments and analysed the data. D.G.G. and A.M.H. performed three-dimensional imaging analysis and quantifications. J.D.B. and E.D.M. performed immunofluorescence. B.G. and Y.B. performed characterization of tissue deformation. Y.B., K.R.M., J.D.B., A.M.H., D.G.G., K.C. and S.B. assisted with critical feedback on the research and manuscript. P.R. generated the K14-H2BPAmCherry mouse line.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 Structure and different markers of the epidermis during wound repair.
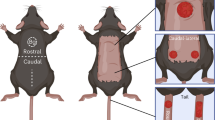
(a) Schematic of the epidermis during wound repair. (b) Thickness changes in the epidermis during wound repair (representative images from 3 mice). K14-H2BGFP, green; DAPI, blue. Scale bar, 20 μm. (c,d) Immunofluorescence staining of Keratin 5 (c; basal cell marker) and Keratin 10 (d; spinous cell marker) using K14-H2BGFP (representative images from 3 mice). Keratin 5 and Keratin10, red; K14-H2BGFP, green; DAPI, blue. Scale bar, 20 μm. (e) Keratin 10 expression in the leading edge (representative images from 3 mice). Keratin10, red; K14-actinGFP, green; DAPI, blue. Scale bar, 50 μm. (f) Full-thickness wound on the mouse ear by 1 mm punch biopsy. (g) Revisits of the same wound in the same mouse using K14-H2BGFP (representative images from 4 mice). Scale bar, 200 μm.
Supplementary Figure 2 H2BPAmCherry labeling and revisits show contribution to upper differentiated layers.
(a) Schematic of light-activation labeling and subsequent revisit. (b) Top down (x-y) view of the light activated H2BPAmCherry cells in the basal layer (100 × 100 μm2 square) using K14-H2BPAmCherry;K14-actinGFP (representative images from 5 mice). (c) Imaris 3D reconstruction of H2BPAmCherry positive cells within the skin epithelium (K14-actinGFP, green) and the dermis (fibrillar type I collagens detected as SHG, blue). (d) Daily revisits of the H2BPAmCherry positive cells shows their progression upwards in the skin epidermis and their participation to upper differentiated layers (representative images from 3 mice). (e,f) Labeling of cells within the basal layer 0 day (e) and 3 days (f) PWI and revisit 24 hours later using K14-H2BPAmCherry;K14-actinGFP (representative images from 3 mice). Arrowheads indicated strong red autofluorescence from the hair shafts. Scale bar, 50 μm. (g) H2BPAmCherry is activated in the basal layer (100 μm width) 3 days after wound. The mouse was sacrificed 1 day after labeling and immunostaining was conducted with the differentiation marker Keratin 10. H2BPAmCherry positive cells were positive for Keratin 10 staining showing functional differentiation of basal cells (representative images from 3 mice). Keratin 10, red; K14-actinGFP, green; DAPI, blue; H2BPAmCherry, gray. Scale bar, 50 μm. (h) Schematic of the differentiation of the H2BPAmCherry labeled cells.
Supplementary Figure 3 The suprabasal layer does not move downwards and does not contribute to lower layers during wound repair.
(a) Schematic of possible outcomes upon spinous layer labeling. (b) Spinous layer cell labeling and revisit 1 day later using K14-H2BPAmCherry; K14-actinGFP (representative images from 3 mice). Scale bar, 50 μm. (c) Schematic of possible outcomes upon granular layer labeling. (d) Granular layer labeling and revisit 1 day later using K14-H2BPAmCherry;K14-actinGFP (representative images from 3 mice). Scale bar, 50 μm.
Supplementary Figure 4 Stratification is changed after migration is blocked.
(a) Representative quantification of the cell track displacements in Rac1+/− and Rac1−/− wounds 3 days PWI (Rac1+/−, n = 8761 cell tracks from 2 mice; Rac1−/−, n = 9659 cell tracks from 2 mice). (b) Stratification of the Rac1−/− cells during wound repair. There are a few binucleated cells in the Rac1−/− cells caused by improper cytokinesis in the basal layer. The binucleated cells are detected in spinous and granular layers indicating that stratification still occurs in the epidermis (representative images from 3 mice). Scale bar, 50 μm. (c) Representative quantification of the epidermal thickness in Rac1+/− and Rac1−/− wounds 3 days PWI (Rac1+/−, n = 1254 points from 2 mice; Rac1−/−, n = 1617 points from 2 mice). (d) x-z view of epidermis in Rac1+/− and Rac1−/− 1 wounds 3 days PWI (representative images from 3 mice for Rac1+/− and Rac1−/− respectively). Dotted lines represent the region used to quantify epidermal thickness. Scale bar, 50 μm.
Supplementary Figure 5 Different kinds of cell division occur during wound repair.
(a) x-z view of the different kinds of cell divisions (representative images from 3 mice). Scale bar, 10 μm. (b) Basal parallel divisions are in blue (n = 364), basal oblique divisions are in red (n = 29) and suprabasal parallel divisions are in green (n = 16) from Figure 3a.
Supplementary Figure 6 Quantitative characterization of tissue deformation.
(a–c) The displacement of nuclei (green dots) and the evolution of the links (blue lines) connecting them can be used to measure local tissue deformation34. A deformation is a change in tissue dimensions relative to its initial state; it is dimensionless and can be expressed as a percentage. A deformation rate is, therefore, expressed per units of time; 10−2 h−1 thus represents a 1% change in length along one direction per hour. Any deformation can be decomposed into two parts: an isotropic part (a), and an anisotropic part (b). The isotropic part (a) quantifies a local change in tissue size: an isotropic expansion corresponds to a positive value (white disk), while an isotropic contraction corresponds to a negative value (grey disk). The anisotropic part (c) quantifies the local tissue contraction-elongation (CE) (or pure shear) without change in size. We represent it with a bar in the direction of the elongation, the length and direction of which represent the magnitude and the orientation of this CE. In this figure, we illustrate the same piece of tissue (left) undergoing an isotropic expansion of about 40% (a), or a CE of same amplitude (b), or both combined (c). (d,e) The tissue deformation analysis is performed in the control (d) and Cdkn1b overexpressed using K14-rtTA;tetO-Cdkn1b;K14-H2BGFP (e) mice (representative analysis from 2 mice). Scale bar, 50 μm.
Supplementary information
Supplementary Information
Supplementary Information (PDF 52623 kb)
Supplementary Table 1
Supplementary Information (XLSX 136214 kb)
Tracking of epithelial migration over 12 hours shows a gradient migration pattern from the wound.
Imaris track analysis was done using K14-H2BGFP (h:mm:ss.sss) (representative analysis from 3 mice). Bright cells located closer to the wound edge (left) are presumably dead and are not observed to move on the top of the epidermis. Each nucleus is marked by a dragon tail track, which highlights its migration path. The color of the tracks change from blue to red indicating passage of time. Also see Figure 1b. Scale bar, 100 μm. (MOV 8927 kb)
Tracking of leading edge cells shows upward movement in vivo.
Tracking analysis from Imaris of a time-lapse recording of the x-z view of the leading edge region using K14-H2BGFP (hh:mm:ss.sss) (representative analysis from 3 mice). Also see Figure 1e. Scale bar, 10 μm. (MOV 2859 kb)
Cell migration behind leading edge.
Epidermal nuclei from K14-H2BGFP are represented by dots which have different colors depending on their distance from the basement membrane. All the dots are shown in x-y, x-z, and y-z views (t = 12 hours; representative analysis from 2 mice). Also see Figure 1g. (MOV 36159 kb)
Identification of cell shape changes in the different layers of the epidermis in vivo.
Time-lapse recording of epithelial cells using membrane-fluorescent mice (K14-CreER;mTmG) shows that lamellipodia are formed during migration in basal and spinous layer cells but not in granular layer cells. The asterisk indicates a migrating spinous layer cell (h.hh) (representative analysis from 3 mice). The movie was looped 3 times to facilitate identification of the cellular behaviors. Scale bar, 10 μm. (MOV 3531 kb)
Identification of distinct regions of cellular behavior at varying distances from the wound.
Time-lapse recording of epithelial cells show 1) cells migrating but not proliferating closer to the wound edge (migration- left); 2) cells both proliferating and migrating beyond the wound edge (mixed- center); 3) cells only proliferating at the distance from the wound (proliferation- right) using K14-H2BGFP (h.hh) (representative analysis from 3 mice). The movie was looped 3 times to facilitate identification of the cellular behaviors. Also see Figure 3b. Scale bar, 10 μm. (MOV 22327 kb)
Lamellipodia formation before cell division in the mixed zone.
Time-lapse recording of an epithelial cell in the mixed zone in K14-CreER;mTmG mice shows that lamellipodia are formed during migration. However, all lamellipodia disappear just before cell division (representative analysis from 3 mice). Arrowheads indicate lamellipodia. The movie was looped 3 times to facilitate identification of the cellular behaviors. Scale bar, 10 μm. (MOV 444 kb)
Quantification of local tissue deformations.
First, nuclei positions are used as seed to generate a Voronoi tessellation defining a region for each nucleus (grey lines) and a set of neighboring nuclei. Then, a grid made of regions of about 80 × 80 μm2 is used to select nuclei that will define the regions of the tissue over which deformations will be determined (black contours). The evolution of the links connecting the centroids of neighboring Voronoi “cells” is used to calculate the deformation of each tissue patch. Between two successive images: blue links are conserved and are used in the calculation of the patch deformation; magenta links disappear (dashed lines) and appear (full lines), and are not used in the calculation (t = 12 hours; representative analysis from 2 mice). Scale bar, 50 μm. (MOV 169844 kb)
Rights and permissions
About this article
Cite this article
Park, S., Gonzalez, D., Guirao, B. et al. Tissue-scale coordination of cellular behaviour promotes epidermal wound repair in live mice. Nat Cell Biol 19, 155–163 (2017). https://doi.org/10.1038/ncb3472
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncb3472
This article is cited by
-
Mechanical state transitions in the regulation of tissue form and function
Nature Reviews Molecular Cell Biology (2024)
-
Cellular and molecular mechanisms of skin wound healing
Nature Reviews Molecular Cell Biology (2024)
-
Myc-dependent dedifferentiation of Gata6+ epidermal cells resembles reversal of terminal differentiation
Nature Cell Biology (2023)
-
Injury prevents Ras mutant cell expansion in mosaic skin
Nature (2023)
-
Tissue memory relies on stem cell priming in distal undamaged areas
Nature Cell Biology (2023)