Abstract
Myeloid-derived suppressor cells (MDSCs) play critical roles in primary and metastatic cancer progression. MDSC regulation is widely variable even among patients harbouring the same type of malignancy, and the mechanisms governing such heterogeneity are largely unknown. Here, integrating human tumour genomics and syngeneic mammary tumour models, we demonstrate that mTOR signalling in cancer cells dictates a mammary tumour’s ability to stimulate MDSC accumulation through regulating G-CSF. Inhibiting this pathway or its activators (for example, FGFR) impairs tumour progression, which is partially rescued by restoring MDSCs or G-CSF. Tumour-initiating cells (TICs) exhibit elevated G-CSF. MDSCs reciprocally increase TIC frequency through activating Notch in tumour cells, forming a feedforward loop. Analyses of primary breast cancers and patient-derived xenografts corroborate these mechanisms in patients. These findings establish a non-canonical oncogenic role of mTOR signalling in recruiting pro-tumorigenic MDSCs and show how defined cancer subsets may evolve to promote and depend on a distinct immune microenvironment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Change history
20 May 2016
In the version of this Article originally published, in the fourth affiliation, 'Los Angeles' should have read 'Louisiana'. This has been corrected in all online versions of the Article.
References
Gabrilovich, D. I. & Nagaraj, S. Myeloid-derived suppressor cells as regulators of the immune system. Nat. Rev. Immunol. 9, 162–174 (2009).
Bunt, S. K., Clements, V. K., Hanson, E. M., Sinha, P. & Ostrand-Rosenberg, S. Inflammation enhances myeloid-derived suppressor cell cross-talk by signaling through Toll-like receptor 4. J. Leukoc. Biol. 85, 996–1004 (2009).
Gabrilovich, D. I., Ostrand-Rosenberg, S. & Bronte, V. Coordinated regulation of myeloid cells by tumours. Nat. Rev. Immunol. 12, 253–268 (2012).
Marvel, D. & Gabrilovich, D. I. Myeloid-derived suppressor cells in the tumor microenvironment: expect the unexpected. J. Clin. Invest. 125, 3356–3364 (2015).
Granot, Z. et al. Tumor entrained neutrophils inhibit seeding in the premetastatic lung. Cancer Cell 20, 300–314 (2011).
Strober, S. Natural suppressor (NS) cells, neonatal tolerance, and total lymphoid irradiation: exploring obscure relationships. Annu. Rev. Immunol. 2, 219–237 (1984).
Almand, B. et al. Increased production of immature myeloid cells in cancer patients: a mechanism of immunosuppression in cancer. J. Immunol. 166, 678–689 (2001).
Diaz-Montero, C. M. et al. Increased circulating myeloid-derived suppressor cells correlate with clinical cancer stage, metastatic tumor burden, and doxorubicin-cyclophosphamide chemotherapy. Cancer Immunol. Immunother. 58, 49–59 (2009).
Solito, S. et al. Myeloid-derived suppressor cell heterogeneity in human cancers. Ann. NY Acad. Sci. 1319, 47–65 (2014).
Cao, Y. et al. BMP4 inhibits breast cancer metastasis by blocking myeloid-derived suppressor cell activity. Cancer Res. 74, 5091–5102 (2014).
Donkor, M. K. et al. Mammary tumor heterogeneity in the expansion of myeloid-derived suppressor cells. Int. Immunopharmacol. 9, 937–948 (2009).
Kowanetz, M. et al. Granulocyte-colony stimulating factor promotes lung metastasis through mobilization of Ly6G + Ly6C + granulocytes. Proc. Natl Acad. Sci. USA 107, 21248–21255 (2010).
Shojaei, F. et al. G-CSF-initiated myeloid cell mobilization and angiogenesis mediate tumor refractoriness to anti-VEGF therapy in mouse models. Proc. Natl Acad. Sci. USA 106, 6742–6747 (2009).
Waight, J. D., Hu, Q., Miller, A., Liu, S. & Abrams, S. I. Tumor-derived G-CSF facilitates neoplastic growth through a granulocytic myeloid-derived suppressor cell-dependent mechanism. PLoS ONE 6, e27690 (2011).
Serafini, P. et al. High-dose granulocyte-macrophage colony-stimulating factor-producing vaccines impair the immune response through the recruitment of myeloid suppressor cells. Cancer Res. 64, 6337–6343 (2004).
Bunt, S. K., Sinha, P., Clements, V. K., Leips, J. & Ostrand-Rosenberg, S. Inflammation induces myeloid-derived suppressor cells that facilitate tumor progression. J. Immunol. 176, 284–290 (2006).
Song, X. et al. CD11b + /Gr-1 + immature myeloid cells mediate suppression of T cells in mice bearing tumors of IL-1β-secreting cells. J. Immunol. 175, 8200–8208 (2005).
Bunt, S. K. et al. Reduced inflammation in the tumor microenvironment delays the accumulation of myeloid-derived suppressor cells and limits tumor progression. Cancer Res. 67, 10019–10026 (2007).
Sinha, P., Clements, V. K., Fulton, A. M. & Ostrand-Rosenberg, S. Prostaglandin E2 promotes tumor progression by inducing myeloid-derived suppressor cells. Cancer Res. 67, 4507–4513 (2007).
Gallina, G. et al. Tumors induce a subset of inflammatory monocytes with immunosuppressive activity on CD8 + T cells. J. Clin. Invest. 116, 2777–2790 (2006).
Bronte, V. et al. IL-4-induced arginase 1 suppresses alloreactive T cells in tumor-bearing mice. J. Immunol. 170, 270–278 (2003).
Gabrilovich, D. et al. Vascular endothelial growth factor inhibits the development of dendritic cells and dramatically affects the differentiation of multiple hematopoietic lineages in vivo. Blood 92, 4150–4166 (1998).
Psaila, B. & Lyden, D. The metastatic niche: adapting the foreign soil. Nat. Rev. Cancer 9, 285–293 (2009).
Yang, L. et al. Abrogation of TGF beta signaling in mammary carcinomas recruits Gr-1 + CD11b + myeloid cells that promote metastasis. Cancer Cell 13, 23–35 (2008).
Du, R. et al. HIF1α induces the recruitment of bone marrow-derived vascular modulatory cells to regulate tumor angiogenesis and invasion. Cancer Cell 13, 206–220 (2008).
Welm, B. E. et al. Inducible dimerization of FGFR1: development of a mouse model to analyze progressive transformation of the mammary gland. J. Cell. Biol. 157, 703–714 (2002).
Pond, A. C. et al. Fibroblast growth factor receptor signaling dramatically accelerates tumorigenesis and enhances oncoprotein translation in the mouse mammary tumor virus-Wnt-1 mouse model of breast cancer. Cancer Res. 70, 4868–4879 (2010).
Herschkowitz, J. I. et al. Comparative oncogenomics identifies breast tumors enriched in functional tumor-initiating cells. Proc. Natl Acad. Sci. USA 109, 2778–2783 (2012).
Li, H., Ji, M., Klarmann, K. D. & Keller, J. R. Repression of Id2 expression by Gfi-1 is required for B-cell and myeloid development. Blood 116, 1060–1069 (2010).
Sato, T., Nakashima, A., Guo, L., Coffman, K. & Tamanoi, F. Single amino-acid changes that confer constitutive activation of mTOR are discovered in human cancer. Oncogene 29, 2746–2752 (2010).
Coffelt, S. B. et al. IL-17-producing gammadelta T cells and neutrophils conspire to promote breast cancer metastasis. Nature 522, 345–348 (2015).
Dey, J. H. et al. Targeting fibroblast growth factor receptors blocks PI3K/AKT signaling, induces apoptosis, and impairs mammary tumor outgrowth and metastasis. Cancer Res. 70, 4151–4162 (2010).
Cancer Genome Atlas Network Comprehensive molecular portraits of human breast tumours. Nature 490, 61–70 (2012).
Buzzeo, M. P., Yang, J., Casella, G. & Reddy, V. Hematopoietic stem cell mobilization with G-CSF induces innate inflammation yet suppresses adaptive immune gene expression as revealed by microarray analysis. Exp. Hematol. 35, 1456–1465 (2007).
Zhang, X. H. et al. Latent bone metastasis in breast cancer tied to Src-dependent survival signals. Cancer Cell 16, 67–78 (2009).
Wei, G. et al. Gene expression-based chemical genomics identifies rapamycin as a modulator of MCL1 and glucocorticoid resistance. Cancer Cell 10, 331–342 (2006).
Wang, B. T. et al. The mammalian target of rapamycin regulates cholesterol biosynthetic gene expression and exhibits a rapamycin-resistant transcriptional profile. Proc. Natl Acad. Sci. USA 108, 15201–15206 (2011).
Curtis, C. et al. The genomic and transcriptomic architecture of 2,000 breast tumours reveals novel subgroups. Nature 486, 346–352 (2012).
Zhang, X. et al. A renewable tissue resource of phenotypically stable, biologically and ethnically diverse, patient-derived human breast cancer xenograft models. Cancer Res. 73, 4885–4897 (2013).
DeRose, Y. S. et al. Tumor grafts derived from women with breast cancer authentically reflect tumor pathology, growth, metastasis and disease outcomes. Nat. Med. 17, 1514–1520 (2011).
Movahedi, K. et al. Identification of discrete tumor-induced myeloid-derived suppressor cell subpopulations with distinct T cell-suppressive activity. Blood 111, 4233–4244 (2008).
Dontu, G. et al. In vitro propagation and transcriptional profiling of human mammary stem/progenitor cells. Genes Dev. 17, 1253–1270 (2003).
Shipitsin, M. et al. Molecular definition of breast tumor heterogeneity. Cancer Cell 11, 259–273 (2007).
Dumitru, C. A., Moses, K., Trellakis, S., Lang, S. & Brandau, S. Neutrophils and granulocytic myeloid-derived suppressor cells: immunophenotyping, cell biology and clinical relevance in human oncology. Cancer Immunol. Immunother. 61, 1155–1167 (2012).
Yang, L. et al. Expansion of myeloid immune suppressor Gr + CD11b + cells in tumor-bearing host directly promotes tumor angiogenesis. Cancer Cell 6, 409–421 (2004).
Lu, H. et al. A breast cancer stem cell niche supported by juxtacrine signalling from monocytes and macrophages. Nat. Cell Biol. 16, 1105–1117 (2014).
Oskarsson, T. et al. Breast cancer cells produce tenascin C as a metastatic niche component to colonize the lungs. Nat. Med. 17, 867–874 (2011).
Bray, S. J. Notch signalling: a simple pathway becomes complex. Nat. Rev. Mol. Cell Biol. 7, 678–689 (2006).
Yu, X. et al. Notch signaling activation in human embryonic stem cells is required for embryonic, but not trophoblastic, lineage commitment. Cell Stem Cell 2, 461–471 (2008).
Blokzijl, A. et al. Cross-talk between the Notch and TGF-beta signaling pathways mediated by interaction of the Notch intracellular domain with Smad3. J. Cell. Biol. 163, 723–728 (2003).
Valdez, J. M. et al. Notch and TGFβ form a reciprocal positive regulatory loop that suppresses murine prostate basal stem/progenitor cell activity. Cell Stem Cell 11, 676–688 (2012).
Hu, Y. & Smyth, G. K. ELDA: extreme limiting dilution analysis for comparing depleted and enriched populations in stem cell and other assays. J. Immunol. Methods 347, 70–78 (2009).
Nagalla, S. et al. Interactions between immunity, proliferation and molecular subtype in breast cancer prognosis. Genome Biol. 14, R34 (2013).
Gentles, A. J. et al. The prognostic landscape of genes and infiltrating immune cells across human cancers. Nat. Med. 21, 938–945 (2015).
Iglesia, M. D. et al. Prognostic B-cell signatures using mRNA-seq in patients with subtype-specific breast and ovarian cancer. Clin. Cancer Res. 20, 3818–3829 (2014).
Baselga, J. et al. Everolimus in postmenopausal hormone-receptor-positive advanced breast cancer. N. Engl. J. Med. 366, 520–529 (2012).
Kim, K. et al. Eradication of metastatic mouse cancers resistant to immune checkpoint blockade by suppression of myeloid-derived cells. Proc. Natl Acad. Sci. USA 111, 11774–11779 (2014).
Chi, H. Regulation and function of mTOR signalling in T cell fate decisions. Nat. Rev. Immunol. 12, 325–338 (2012).
Cui, T. X. et al. Myeloid-derived suppressor cells enhance stemness of cancer cells by inducing microRNA101 and suppressing the corepressor CtBP2. Immunity 39, 611–621 (2013).
Acharyya, S. et al. A CXCL1 paracrine network links cancer chemoresistance and metastasis. Cell 150, 165–178 (2012).
Chang, C. H. et al. Mammary stem cells and tumor-initiating cells are more resistant to apoptosis and exhibit increased DNA repair activity in response to DNA damage. Stem Cell Rep. 5, 378–391 (2015).
Zhang, X. H. et al. Selection of bone metastasis seeds by mesenchymal signals in the primary tumor stroma. Cell 154, 1060–1073 (2013).
Hoeflich, K. P. et al. In vivo antitumor activity of MEK and phosphatidylinositol 3-kinase inhibitors in basal-like breast cancer models. Clin. Cancer Res. 15, 4649–4664 (2009).
Acknowledgements
We would like to thank Novartis for providing BGJ-398, and H. C. Lo and D. Weiss for helpful input. We also thank the Antibody-Based Proteomics Shared Resource of the Dan L. Duncan Cancer Center supported by Cancer Center Support grant NCI P30CA125123, and A. Welm, Huntsman Cancer Institute, USA for generously providing some of the PDX models. X.H.-F.Z. is supported by NCI CA183878, the Breast Cancer Research Foundation, US Department of Defense DAMD W81XWH-13-1-0195, Susan G. Komen CCR14298445, and McNair Medical Institute. T.Welte is supported by the Helis Foundation. H.W. is supported by US Department of Defense DAMD W81XWH-13-1-0296. Studies with the p53-null tumours were supported by NIH grant CA148761 to J.M.R. and with the WNT1–iFGFR tumours by NIH grant CA16303 to J.M.R. RRPA experiments were supported by Cancer Prevention and Research Institute of Texas (CPRIT) Core Facilities Support Award RP120092 to D.P.E. The authors acknowledge the joint participation by Diana Helis Henry Medical Research Foundation through its direct engagement in the continuous active conduct of medical research in conjunction with Baylor College of Medicine.
Author information
Authors and Affiliations
Contributions
Conception and design: X.H.-F.Z., J.M.R. and T.Welte. Development of methodology: T.Welte, I.S.K., L.T., X.G., S.H., J.X., T.Wang and Q.M. Acquisition of data: T.Welte, I.S.K., L.T., X.G., H.W., J.L., X.B.H., J.I.H., A.P., G.X., S.K., T.N., L.L., D.P.E., S.H., J.X., Y.L., M.T.L., T.Wang, T.F.W. and L.X. Analysis and interpretation of data: T.Welte, X.H.-F.Z., J.M.R., T.Wang, I.S.K. and Q.M. Writing and review of manuscript: X.H.-F.Z., T.Welte, T.Wang and J.M.R. Study supervision: X.H.-F.Z. and J.M.R.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
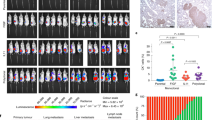
Supplementary Figure 1 Inter-tumoral heterogeneity of MDSC accumulation in mammary tumour models.
(a) Quantification of S100A8 + cells identified by immunofluorescence staining. Six fields were randomly picked from each tumour, and three tumours were included. (b) Relative expression of the S100A8 gene in the bulk of tumour and in CD11b+Gr1+ cells purified from the tumour by FACS. n = 2 and 5 tumours for the bulk tumour and purified CD11b + Gr1 + cells, respectively. (c) In vitro CD3- and IL-2 stimulated T-cell proliferation, measured by CFSE decrease assay, is inhibited by MDSCs. The percentage of proliferating T-cells in conditioned medium (bottom) under indicated conditions. CD11b+Ly6G+ cells and T cells were admixed at 3:1. Two experiments each with technical triplicates were performed with similar results; results of one representative experiment are shown.
Supplementary Figure 3 G-CSF inhibition reduces primary tumour growth and lung metastasis, an effect that is partially overcome by exogenous MDSCs.
(a) P53N tumour bearing mice were treated with G-CSF neutralizing antibody. Relative G-CSF levels in blood after treatment were measured by ELISA. n = 5 and 3 animals in IgG and anti-G-CSF groups, respectively. Two experiments were performed with consistent results, one representative experiment is shown. (b) 4T1 tumour cells were lentivirus-transduced with G-CSF shRNA (Control: GIPZ vector transduced). Efficiency in reducing G-CSF levels in vivo (left panel) and in vitro (right panel) was evaluated by G-CSF ELISA. Left: n = 10 and 17 animals for Control and shG-CSF groups, respectively. Right: cells cultured in 3 different wells were used as technical replicates. Two independent experiments were conducted with representative results shown. (c) MDSC numbers in blood of P53N-C tumour bearing mice after G-CSF-neutralizing antibody regimen compared to IgG control antibody-treated tumour-bearing mice. n = 3, 4, and 7 animals for the three groups, respectively P value is determined by non-parametric Wilcoxon test. (d) 4T1 cells transduced with vector control lentivirus (GIPZ, control) or with G-CSF shRNA expressing lentivirus (shG-CSF) were orthotopically injected to mammary gland. MDSC numbers in blood were quantified. n = 9 and 7 animals for the two groups, respectively. (e) No direct role of G-CSF in 4T1 tumour cell survival. Cell viability was assessed by WST-1 assay in presence of G-CSF neutralizing antibody or G-CSF shRNA compared to controls ‘n.s.’: no significant difference. One experiment was performed in which cells of different groups were cultured in 5 wells each. Error bars indicate s.e.m., and P values are calculated by two-tailed Student’s t tests unless otherwise noted. Statistics source data of Supplementary Fig. 3b–d are provided in Supplementary Table 4.
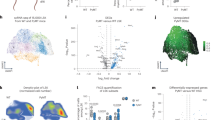
Supplementary Figure 4 A G-CSF responsive gene signature (G-CSF-sig) links the mTOR activity to MDSC infiltration in human breast cancer.
(a) Heat maps show the expression of G-CSF signature as a single score (top), and TCR pathway components (bottom) in the EMC-MSK dataset. The red sticks above the heat maps indicate tumour samples whose gene expression level exceeds the mean of all tumours by more than 2 × s.d. n = 615 patients. (b–d). Three human datasets were analysed for the relationship between expression of G-CSF signature and T-cell activation signature in tumour biopsies. n = 615, 409, and 1992 patients for (b), (c), (d), respectively. (e) As a negative control, the analysis was applied to a panel of tumour cell lines (n = 51, available from GSE12777), showing no correlation as expected. For (b–e), P values were determined based on two-side Student’s t tests for Pearson correlation coefficients. (f) Multivariate (MV) analysis of METABRIC and EMC-MSK datasets using the Cox Proportional-Hazards model to estimate the hazard ratios (HR) of G-CSF-sig. The P values were computed based on the Multivariate Cox Proportional-Hazards model. (g) MDSC quantity in P53N-C tumour-bearing hosts that are either wild type (WT) Balb/c mice or athymic nude (Nu) mice. TF (−) controls are shown for comparison. ‘n.s.’: no significant difference. n = 5 animals per group. Error bars indicate s.e.m., and P values are calculated by two-tailed Student’s t tests. (h) Representative Western blotting of pS6K(T389) and quantitative PCR assay of G-CSF in PDX tumours. Dotted lines indicate the matching between the two types of data across different PDX lines. Error bars indicate s.e.m.
Supplementary Figure 5 Correlation between high G-CSF expression and TIC features.
(a) 4T1 control cells and 4T1 cells expressing G-CSF shRNA were subjected to intracellular G-CSF FACS staining procedure. Overlay-graph demonstrates changes in G-CSF levels. The experiment was performed twice with similar results. Results of a representative experiment are shown. (b) Staining specificity control for pS6K antibody: PS6K levels were measured by intracellular FACS staining in 4T1 cells cultured in medium without serum (starved) or with 10% FBS. (c) Cells with highest G-CSF expression (top 5.3%, expression >2 times mean of total population) were compared to whole 4T1 cell population in the expression of CD24/CD29. Representative plots of gating strategy and identification of CD24highCD29high cells. (d). Same analysis as in (c), for P53N-C model. In (c) and (d): representative of three FACS staining experiments with 2–3 stained samples per experiment. (e) 4T1 cells were stained for G-CSF, CD24 and CD29. Expression of G-CSF in CD24highCD29high cells and in the total population was compared. (f) Same analysis as in (e), for P53N-C cells. (g,h). Correlation between G-CSF and Epcam+CD49f+ cells; analysis was done as described for CD24highCD29high cells in (e). In (h), EpCAMhighCD49fmed and EpCAMmedCD49fhigh denote specific cell population in P53N-C model as described in Fig. 6c. (e–h) n = 3 independent experiments each with technical replicates. Mean values of all three experiments are used to generate the plot and calculate P values. (i) Under TIC enriched conditions 4T1 tumour cells produce increased levels of soluble factors to enhance MDSC differentiation from naïve bone marrow cells. Treatment of primary mouse bone marrow cells with conditioned medium (CM) from either 4T1 cells cultured in TIC-enriching condition (as 3D suspension mammospheres) or 2D conditions favouring differentiation. To eliminate effects of media-composition, all treatment conditions contained the same percentage of 2D and 3D media by supplementing with non-conditioned media as needed. αG-CSF: Five times ED50 dose of G-CSF-neutralizing antibody. G-CSF: 40 ng ml−1 recombinant human G-CSF. (j) Treatment of primary human bone marrow cells with CM from either MC1 cells cultured in 3D TIC-enriching condition or 2D conditions favouring differentiation. Left: FACS analysis showing MDSC-like cells in treated bone marrow. Right: quantification of MDSC-like cells under indicated conditions. Data are from two independent experiments. Error bars indicate s.e.m., and P values are calculated by two-tailed Student’s t tests. Statistics source data of Supplementary Fig. 5e–h are provided in Supplementary Table 4.
Supplementary Figure 6 The mTOR-G-CSF-MDSC axis does not affect tumour angiogenesis.
Immunofluorescence staining of CD31 was performed to quantitate angiogenesis in 4T1 tumours with indicated treatments. The CD31 + area was assessed using ImageJ software and displayed in the right panel. n = 8, 7, 6, and 5 fields randomly picked from 4 different tumours for the four groups, respectively. n.s.: no significance. Scale bar 100 μm.
Supplementary Figure 7 MDSCs promote tumour-initiating capacity.
(a) Counts of mammosphere numbers with or without co-cultures of MDSCs. In each group, cells were cultured in four wells. Results shown are from one representative experiment among four independent experiments. Consistent trends were observed in all experiments. Scale bar, 100 μm. (b) Fold changes induced in 4T1 cells by co-culture with MDSCs are shown for total tumour cell numbers (GFP marker), and sub-populations of CD24highCD29high, CD49f+CD29high and Sca1+c-Kit+. n = 3 independent experiments per group, each experiment with technical triplicates. Combined results of all three experiments are shown. (c). Mammary gland tumours formed by 4T1 cells that had been transduced with vector control (GIPZ) or with G-CSF shRNA lentivirus, were evaluated for mammosphere formation. For each tumour, cells were cultured in four technical replicates. Results (mammosphere numbers per equal tumour cell input) of two individual GIPZ control tumours and four G-CSF shRNA tumours are shown. (d,e) Experimental design as shown in Fig. 8a. P53N-C tumour bearing mice were transiently treated with rapamycin or rapamcin plus MDSCs or left untreated. Tumor cells were extracted and tested for tumour initiation potential on injection to mammary fat pads of untreated mice. Tumor size was measured on day 17 post tumour cell transfer from indicated groups (1,000 cell-injection per mouse). n = 5 animals per group. Error bars, s.d. Kaplan Meier curve of TF survival. (200 cell injection per mouse). n = 5 animals per group. P values were determined by log-rank test. Number of mice with tumours at end of observation time and total numbers of mice are also indicated for each condition. Error bars indicate s.e.m., and P values are calculated by two-tailed Student’s t tests unless otherwise noted. Statistical source data of Supplementary Fig. 7b is provided in Supplementary Table 4.
Supplementary information
Supplementary Information
Supplementary Information (PDF 1335 kb)
Supplementary Table 1
Supplementary Information (XLSX 174 kb)
Supplementary Table 2
Supplementary Information (XLS 39 kb)
Supplementary Table 3
Supplementary Information (XLS 35 kb)
Supplementary Table 4
Supplementary Information (XLS 150 kb)
Rights and permissions
About this article
Cite this article
Welte, T., Kim, I., Tian, L. et al. Oncogenic mTOR signalling recruits myeloid-derived suppressor cells to promote tumour initiation. Nat Cell Biol 18, 632–644 (2016). https://doi.org/10.1038/ncb3355
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncb3355
This article is cited by
-
Myeloid-derived suppressor cells in cancer and cancer therapy
Nature Reviews Clinical Oncology (2024)
-
Tumor Microenvironment: A Niche for Cancer Stem Cell Immunotherapy
Stem Cell Reviews and Reports (2024)
-
Cross-talk between cancer stem cells and immune cells: potential therapeutic targets in the tumor immune microenvironment
Molecular Cancer (2023)
-
Unleashing the potential of combining FGFR inhibitor and immune checkpoint blockade for FGF/FGFR signaling in tumor microenvironment
Molecular Cancer (2023)
-
The evolution and heterogeneity of neutrophils in cancers: origins, subsets, functions, orchestrations and clinical applications
Molecular Cancer (2023)