Abstract
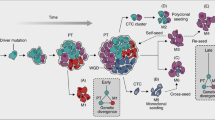
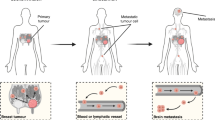
Accumulating data suggest that metastatic dissemination often occurs early during tumour formation, but the mechanisms of early metastatic spread have not yet been addressed. Here, by studying metastasis in a HER2-driven mouse breast cancer model, we show that progesterone-induced signalling triggers migration of cancer cells from early lesions shortly after HER2 activation, but promotes proliferation in advanced primary tumour cells. The switch from migration to proliferation was regulated by increased HER2 expression and tumour-cell density involving microRNA-mediated progesterone receptor downregulation, and was reversible. Cells from early, low-density lesions displayed more stemness features, migrated more and founded more metastases than cells from dense, advanced tumours. Notably, we found that at least 80% of metastases were derived from early disseminated cancer cells. Karyotypic and phenotypic analysis of human disseminated cancer cells and primary tumours corroborated the relevance of these findings for human metastatic dissemination.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Aguirre-Ghiso, J. A., Bragado, P. & Sosa, M. S. Metastasis awakening: targeting dormant cancer. Nat. Med. 19, 276–277 (2013)
Polzer, B. & Klein, C. A. Metastasis awakening: the challenges of targeting minimal residual cancer. Nat. Med. 19, 274–275 (2013)
Cole, B. F., Gelber, R. D., Gelber, S., Coates, A. S. & Goldhirsch, A. Polychemotherapy for early breast cancer: an overview of the randomised clinical trials with quality-adjusted survival analysis. Lancet 358, 277–286 (2001)
Gianni, L. et al. Treatment with trastuzumab for 1 year after adjuvant chemotherapy in patients with HER2-positive early breast cancer: a 4-year follow-up of a randomised controlled trial. Lancet Oncol. 12, 236–244 (2011)
Klein, C. A. et al. Genetic heterogeneity of single disseminated tumour cells in minimal residual cancer. Lancet 360, 683–689 (2002)
Schmidt-Kittler, O. et al. From latent disseminated cells to overt metastasis: genetic analysis of systemic breast cancer progression. Proc. Natl Acad. Sci. USA 100, 7737–7742 (2003)
Klein, C. A. Parallel progression of primary tumours and metastases. Nat. Rev. Cancer 9, 302–312 (2009)
Hüsemann, Y. et al. Systemic spread is an early step in breast cancer. Cancer Cell 13, 58–68 (2008)
Rhim, A. D. et al. EMT and dissemination precede pancreatic tumor formation. Cell 148, 349–361 (2012)
Eyles, J. et al. Tumor cells disseminate early, but immunosurveillance limits metastatic outgrowth, in a mouse model of melanoma. J. Clin. Invest. 120, 2030–2039 (2010)
Banys, M. et al. Hematogenous and lymphatic tumor cell dissemination may be detected in patients diagnosed with ductal carcinoma in situ of the breast. Breast Cancer Res. Treat. 131, 801–808 (2012)
Sänger, N. et al. Disseminated tumor cells in the bone marrow of patients with ductal carcinoma in situ. Int. J. Cancer 129, 2522–2526 (2011)
Valastyan, S. & Weinberg, R. A. Tumor metastasis: molecular insights and evolving paradigms. Cell 147, 275–292 (2011)
Fernandez-Valdivia, R. et al. Revealing progesterone’s role in uterine and mammary gland biology: insights from the mouse. Semin. Reprod. Med. 23, 22–37 (2005)
Mulac-Jericevic, B., Lydon, J. P., DeMayo, F. J. & Conneely, O. M. Defective mammary gland morphogenesis in mice lacking the progesterone receptor B isoform. Proc. Natl Acad. Sci. USA 100, 9744–9749 (2003)
Aupperlee, M. D., Smith, K. T., Kariagina, A. & Haslam, S. Z. Progesterone receptor isoforms A and B: temporal and spatial differences in expression during murine mammary gland development. Endocrinology 146, 3577–3588 (2005)
Brisken, C. Progesterone signalling in breast cancer: a neglected hormone coming into the limelight. Nat. Rev. Cancer 13, 385–396 (2013)
Liao, M. J. et al. Enrichment of a population of mammary gland cells that form mammospheres and have in vivo repopulating activity. Cancer Res. 67, 8131–8138 (2007)
Korkaya, H., Paulson, A., Iovino, F. & Wicha, M. S. HER2 regulates the mammary stem/progenitor cell population driving tumorigenesis and invasion. Oncogene 27, 6120–6130 (2008)
Ginestier, C. et al. ALDH1 is a marker of normal and malignant human mammary stem cells and a predictor of poor clinical outcome. Cell Stem Cell 1, 555–567 (2007)
Lee, Y. J. & Gorski, J. Estrogen-induced transcription of the progesterone receptor gene does not parallel estrogen receptor occupancy. Proc. Natl Acad. Sci. USA 93, 15180–15184 (1996)
Stephens, P. J. et al. The landscape of cancer genes and mutational processes in breast cancer. Nature 486, 400–404 (2012)
Fehm, T. et al. A concept for the standardized detection of disseminated tumor cells in bone marrow from patients with primary breast cancer and its clinical implementation. Cancer 107, 885–892 (2006)
Gužvić, M. et al. Combined genome and transcriptome analysis of single disseminated cancer cells from bone marrow of prostate cancer patients reveals unexpected transcriptomes. Cancer Res. 74, 7383–7394 (2014)
Klein, C. A. Framework models of tumor dormancy from patient-derived observations. Curr. Opin. Genet. Dev. 21, 42–49 (2011)
Brastianos, P. K. et al. Genomic characterization of brain metastases reveals branched evolution and potential therapeutic targets. Cancer Discov. 5, 1164–1177 (2015)
Brisken, C. et al. Essential function of Wnt-4 in mammary gland development downstream of progesterone signaling. Genes Dev. 14, 650–654 (2000)
Fernandez-Valdivia, R. et al. The RANKL signaling axis is sufficient to elicit ductal side-branching and alveologenesis in the mammary gland of the virgin mouse. Dev. Biol. 328, 127–139 (2009)
Asselin-Labat, M. L. et al. Steroid hormone receptor status of mouse mammary stem cells. J. Natl. Cancer Inst. 98, 1011–1014 (2006)
Joshi, P. A. et al. Progesterone induces adult mammary stem cell expansion. Nature 465, 803–807 (2010)
Mukherjee, A. et al. Targeting RANKL to a specific subset of murine mammary epithelial cells induces ordered branching morphogenesis and alveologenesis in the absence of progesterone receptor expression. FASEB J. 24, 4408–4419 (2010)
Narod, S. A., Iqbal, J., Giannakeas, V., Sopik, V. & Sun, P. Breast cancer mortality after a diagnosis of ductal carcinoma in situ. JAMA Oncol. 1, 888–896 (2015)
Astolfi, A. et al. Gene expression analysis of immune-mediated arrest of tumorigenesis in a transgenic mouse model of HER-2/neu-positive basal-like mammary arcinoma. Am. J. Pathol. 166, 1205–1216 (2005)
Ignatiadis, M. et al. HER2-positive circulating tumor cells in breast cancer. PLoS One 6, e15624 (2011)
Hafner, C. et al. Oncogenic PIK3CA mutations occur in epidermal nevi and seborrheic keratoses with a characteristic mutation pattern. Proc. Natl Acad. Sci. USA 104, 13450–13454 (2007)
Hafner, C. et al. Multiple oncogenic mutations and clonal relationship in spatially distinct benign human epidermal tumors. Proc. Natl Acad. Sci. USA 107, 20780–20785 (2010)
Pollock, P. M. et al. High frequency of BRAF mutations in nevi. Nat. Genet. 33, 19–20 (2003)
Hutchinson, J. N., Jin, J., Cardiff, R. D., Woodgett, J. R. & Muller, W. J. Activation of Akt-1 (PKB-α) can accelerate ErbB-2-mediated mammary tumorigenesis but suppresses tumor invasion. Cancer Res. 64, 3171–3178 (2004)
Liu, H. et al. MYC suppresses cancer metastasis by direct transcriptional silencing of αV and β3 integrin subunits. Nat. Cell Biol. 14, 567–574 (2012)
VerMilyea, M. D. et al. Transcriptome asymmetry within mouse zygotes but not between early embryonic sister blastomeres. EMBO J. 30, 1841–1851 (2011)
Dull, T. et al. A third-generation lentivirus vector with a conditional packaging system. J. Virol. 72, 8463–8471 (1998)
Petti, L. M. & Ray, F. A. Transformation of mortal human fibroblasts and activation of a growth inhibitory pathway by the bovine papillomavirus E5 oncoprotein. Cell Growth Differ. 11, 395–408 (2000)
Stewart, S. A. et al. Lentivirus-delivered stable gene silencing by RNAi in primary cells. RNA 9, 493–501 (2003)
Thery, C., Amigorena, S., Raposo, G. & Clayton, A. Isolation and characterization of exosomes from cell culture supernatants and biological fluids. Current Protoc. Cell Biology Chapter 3, Unit 3.22 (2006)
Dueck, A., Eichner, A., Sixt, M. & Meister, G. A miR-155-dependent microRNA hierarchy in dendritic cell maturation and macrophage activation. FEBS Lett. 588, 632–640 (2014)
Meyer, L. R. et al. The UCSC genome browser database: extensions and updates 2013. Nucleic Acids Res. 41, D64–D69 (2013)
Yang, Y. H., Buckley, M. J. & Speed, T. P. Analysis of cDNA microarray images. Brief. Bioinform. 2, 341–349 (2001)
Yang, Y. H. et al. Normalization for cDNA microarray data: a robust composite method addressing single and multiple slide systematic variation. Nucleic Acids Res. 30, e15 (2002)
Khojasteh, M., Lam, W. L., Ward, R. K. & MacAulay, C. A stepwise framework for the normalization of array CGH data. BMC Bioinformatics 6, 274 (2005)
Smyth, G. K. & Speed, T. Normalization of cDNA microarray data. Methods 31, 265–273 (2003)
Ritchie, M. E. et al. limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res. 43, e47 (2015)
Marioni, J. C. et al. Breaking the waves: improved detection of copy number variation from microarray-based comparative genomic hybridization. Genome Biol. 8, R228 (2007)
Venkatraman, E. S. & Olshen, A. B. A faster circular binary segmentation algorithm for the analysis of array CGH data. Bioinformatics 23, 657–663 (2007)
Mermel, C. H. et al. GISTIC2.0 facilitates sensitive and confident localization of the targets of focal somatic copy-number alteration in human cancers. Genome Biol. 12, R41 (2011)
Klein, C. A. et al. Comparative genomic hybridization, loss of heterozygosity, and DNA sequence analysis of single cells. Proc. Natl Acad. Sci. USA 96, 4494–4499 (1999)
Acknowledgements
We thank T. Perry for his critical reading of the manuscript. This work was supported by grants from the DFG (Kl 1233/2-1, KL 1233/3-1, KL 1233/10-1 (C.A.K.); Me2064/4-1, (G.M.); SP 938/2-1 (R.S.); INST 89/341-1 FUGG (TissueFAX)); the Dr Josef Steiner Foundation and ERC (322602) to C.A.K.; the SWCRF, CA109182, CA196521, CA163131, BC132674 (J.A.A.-G.) F31 CA183185 (K.L.H.) BC112380 (M.S.S.), NIH 1S10RR024745 Microscopy CoRE at ISMMS and by a donation from A. Jungmayer.
Author information
Authors and Affiliations
Contributions
C.A.K. and H.H. designed and evaluated core experiments. H.H. performed core experiments. M.M.S.O., C.W., L.K.N., C.E., C.R. and M.Gu. helped with in vivo, in vitro and primary culture experiments. M.H., M.M., M.Gr., R.S. and H.H. performed bioinformatic and statistical analyses. M.W.-K., K.L.H., M.S.S. and F.W. performed staining and pathological analysis. N.E. and G.M. performed miRNA sequencing and analysis. G.H., N.P., A.K.H., F.-A.T., S.Y.B., B.R., S.B. and T.F. performed DCC analysis or collected patient data. C.A.K. and H.H. wrote the manuscript with input from J.A.A.-G.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Extended data figures and tables
Extended Data Figure 1 Early lesion signature induction and expression of HER2 and PGR.
a, The proportion of cancer cells disseminating to the bone marrow in BALB-NeuT mice decreases with increasing primary tumour area. DCCs were identified using anti-cytokeratin antibodies in bone marrow samples. The y axis displays the number of detected DCCs per 106 bone marrow cells divided by the total tumour area in mm2. The number of mice used per data point is written below the graph. b, Laser microdissection of epithelial structures: two examples of 7–9-week-old BALB-NeuT mammary glands showing microdissection of regions with incipient epithelial hyperplasia. For all samples similar amounts of tissue (up to 100,000 μm2) were isolated. c, qPCR validation of microarray profiles. qPCR was performed for 10 genes, upregulated or downregulated in microarray samples of early lesions and all changes, except one (Zfp408), were confirmed. d, qPCR for the mRNA level of all steroid hormone receptors (EL, early lesions; PT, advanced primary tumour; Met, lung metastasis). e, Primary cultures from mammary tissue of 7–9-week-old BALB-NeuT mice, were treated with different concentrations (1, 10, and 100 nM) of progesterone (P), oestrogen (E), aldosterone (A), cortisol (C), testosterone (T) or vehicle (ethanol; untreated) for 75 h. Only progesterone induces upregulation of the complete early lesion signature. f, Increased expression of PGR-B in young mammary glands (9-week old BALB/c and BALB-NeuT mice with early lesions compared to 25-week-old BALB/c mice), but not primary tumours correlates with increased HER2 expression. g, Progesterone induces the early lesion signature in 4T1 cells (highly aggressive and metastatic cell line derived from a spontaneous BALB/c mammary tumour), but not in 67NR (tumorigenic and non-metastatic cell line derived from a spontaneous BALB/c mammary tumour) and MM3MG cells (normal mammary epithelial cell line derived from a BALB/c mouse). h, Progesterone treatment induces upregulation of HER2 expression in 4T1 cells. i, Overexpression of PGR-B in MM3MG cells induces upregulation of HER2 expression. ****P ≤ 0.0001 (Student’s t-test and Stouffer’s combined probability test); data are mean ± s.d. For gel source data, see Supplementary Fig. 1.
Extended Data Figure 2 Progesterone regulates migration and is linked to branching morphogenesis.
a, qPCR analysis of Pgr, Rank (also known as Tnfrsf11a), Rankl and Wnt4 in normal and transgenic mouse mammary tissue or tumours. Note the increased expression of Pgr, Wnt4 and Rankl in early lesions compared to primary tumours. Only Rank (the Rankl receptor) is strongly expressed in primary tumours. b, Primary cultures of early lesions treated with progesterone, WNT4, and RANKL. WNT4 and RANKL treatment induce the early lesion signature and act synergistically. c, d, PGR (green) staining at 5 and 12 weeks of age (FVB wild-type mice). Scale bars, 100 μm. The percentage of PGR+ cells per duct was quantified (n = 2 mice per age group) in the distal and proximal portions of the gland (relative to the origin). PGR-expressing cells were more abundant in distal ducts (number of analysed ducts per group is displayed above each column). LN, lymph node.e, f, Photomicrograph of migration assay (e) and quantification of migrating cells (f) derived from fresh tissue (e, left) or dissociated spheres derived from primary tumours or early lesions (e, right; f, quantification). Progesterone, WNT4 and RANKL induce migration of early-lesion-derived but not primary-tumour-derived cells (see also Fig. 2a). g, Scheme of combined migration and sphere assay. The lower chamber is filled with serum-free sphere medium and the bottom is covered with poly-HEMA to prevent adhesion and enable sphere formation. After 72 h migration, the insert is removed and the lower chamber is analysed (after 11 days) for mammosphere formation (see Methods). h, Effect of oestrogen and progesterone on migration and sphere formation of mammary cells derived from early lesions. Cells were exposed to 10 nM oestrogen or progesterone or 10 nM oestrogen + 10 nM progesterone inhibitor (RU486). *P ≤ 0.05; **P ≤ 0.01; ***P ≤ 0.001; ****P ≤ 0.0001 (Student’s t-test); Data are mean ± s.e.m. (d) or mean ± s.d. (other panels).
Extended Data Figure 3 HER2 expression levels regulate migration and proliferation.
a, Parental MM3MG cells, a cell line derived from mammary epithelial cells of wild-type BALB/c mice, do not express ERα but express low levels of HER2 and PGR-B compared to 4T1 and TUBO cells (TUBO cells were grown at low density; see Fig. 3 and Extended Data Figs 4, 5). b, Immunoblot confirming successful transduction of the MM3MG cell line with Her2 and Pgr-B. Note that transduction of PGR-B increases HER2 levels. c, d, Overexpression of Pgr-B in MM3MG cells (MM3MG-Pgr-B) reduces migration, whereas Her2 overexpression (MM3MG–Her2) increases migration of cells. Addition of progesterone does not alter migration of Pgr-B-overexpressing cells (MM3MG–Pgr-B). e, Overexpression of Pgr-B in MM3MG cells reduces sphere formation, whereas Her2 overexpression increases sphere formation. c–e, Migrating/sphere forming cells are not from the PGR+, but the PGR− population, which are responsive to PIPS. f–j, To investigate which PGR− cells were the target population of progesterone signalling, we exposed parental MM3MG cells and Her2-transduced cells to progesterone, PIPS or mixed the cells with PGR+ cells (only for migration experiments). Progesterone, WNT4 and RANKL, and co-culture with MM3MG–Pgr-B induced sphere formation and migration of MM3MG cells, but decreased these responses in MM3MG–Her2 cells. k, Overexpression of Her2 increases proliferation of MM3MG cells (MM3MG–Her2). WNT4 and RANKL (WR) further increase proliferation of MM3MG–Her2 cells, but decreases proliferation of the parental (MM3MG) cells. Therefore based on expression of HER2, cells either migrate (HER2low/−) or proliferate (HER2high). l, WNT4 and RANKL treatment induces proliferation of primary cultured cells derived from primary tumours, but reduces it in cells derived from early lesions. m, Reduction of HER2 signalling by lapatinib overrides the inhibitory effect of WNT4 and RANKL, and increases migration in MM3MG–Her2 cells. However, strong inhibition of HER2 signalling reduces migration. n, Lapatinib inhibits HER2 signalling by preventing phosphorylation. o, Cells that migrated through the pores of the migration chamber insert were stained for HER2 (FITC, green) and PGR or ERα (Cy3, red). In 1:1 co-culture of MM3MG–Pgr-B and MM3MG–Her2 (top) only HER2-expressing cells migrate. Migrated primary cells derived from early lesions (middle) do not express PGR and display faint HER2 staining (brightness of HER2 and PGR staining increased by 50% for better visibility). HER2 and PGR double-positive T47D cells fixed onto the filters of migration chambers served as positive control of staining. m–o, Cells with low/intermediate signalling of HER2 show the highest response in migration and sphere formation induction by PIPS. *P ≤ 0.05; **P ≤ 0.01; ***P ≤ 0.001; ****P ≤ 0.0001; NS, not significant; (F-test of the slope (k, l) or Student’s t-test (other panels)); data are mean ± s.d. For gel source data, see Supplementary Fig. 1.
Extended Data Figure 4 Cell density and regulation of PGR and HER2 signalling.
a, PGR expression silenced in tumours can be re-activated in culture and re-silenced in vivo. b, PGR re-expression only occurs in TUBO cells grown at low density and high density after frequent medium change. c, Downregulation of PGR in early lesion cells cultured in a transwell assay next to primary tumour cells suggests the existence of a secreted factor passing through the membrane of the transwell insert and downregulating Pgr mRNA (left) and protein (right). d, T47D cells exposed to conditioned medium from TUBO cells display reduced PGR mRNA (left) and protein (right). e, Exosomes derived from the cell culture medium of TUBO cells grown at high density (exosome fraction) induce downregulation of PGR in T47D cells. f, miRNA sequencing to identify PGR regulating miRNAs. Left, top 10 upregulated miRNAs in Her2-overexpressing cells (MM3MG–Her2) compared to control (MM3MG). Middle, top 10 expressed miRNAs in TUBO cells and TUBO-cell-derived exosomes. Right, miRNAs predicted by the miRANDA web software to regulate Pgr g, Among all candidate miRNAs only miR-30a-5p and miR-9-5p induce downregulation of Pgr mRNA in T47D cells. h, Downregulation of PGR in T47D cells treated with miR-30a-5p and miR-9-5p. i, Expression of miR-30-5p in early lesions and primary tumour samples compared to mammary glands from 8-week-old BALB/c mice. j, Density induced upregulation of HER2 in TUBO cells grown at low or high density and early lesions compared to primary tumour samples (left) and progesterone-responsiveness of low-density TUBO cells (right). Note that levels of HER2, PGR, the glucocorticoid (GR), mineralocorticoid (MR) and androgen receptors (AR) are regulated by progesterone in a dose-dependent manner except ER-α (see related result in Extended Data Fig 1d). k–m, TUBO cells grown at low density and exposed to progesterone or PIPS migrated more (k, l) and produced more spheres (m), similar to cells derived from early lesions (see Fig. 2). **P ≤ 0.01; ***P ≤ 0.001; ****P ≤ 0.0001(Student’s t-test); data are mean ± s.d. For gel source data, see Supplementary Fig. 1.
Extended Data Figure 5 Cell density and regulation of PGR and HER2 signalling in human cell lines.
To investigate whether human breast cancer cells display similar regulatory circuits as found in mouse cells, we selected 16 cell lines of different breast cancer subtypes. a, HER2 mRNA expression levels in 15 human cell lines compared to the hTERT-HME cell line. Different colours indicate the subtype of breast cancer of each cell line. b, The expression of miR-9-5p in human breast cancer cell lines compared to hTERT-HME cells. Note that cell lines highly expressing HER2 (see a) express more miR-9-5p similar to primary tumours of BALB-NeuT and TUBO cells (see Fig. 3b, c), whereas two HER2high/PGRhigh cell lines, BT474 and T47D, do not express miR-9-5p similar to human HER2high/PGRhigh samples (see Fig. 5d). c, High cell density leads to upregulation of HER2 mRNA (top) or protein levels (bottom) in several cell lines. Only four cell lines were analysed for protein level (HER2 level was not influenced by cell density in CAMA1; HER2 level regulated by cell density in HCC1806, MDA-MB-231 and MCF7). Numbers below the blots denote fold change of HER2 in high density compared to low density normalized over β-actin. d, Expression of miR-9-5p is upregulated by cell density in SKBR3, HCC1937, HCC1806 and MCF7 cell lines. e, Migration and sphere-forming potential of 10 out of 16 cell lines grown at low and high densities, and treated with PIPS or progesterone. The first 7 cell lines regulate HER2 transcripts by density (see c) and their response to PIPS is similar to TUBO cells and primary mammary cell cultures of BALB-NeuT mice (see Fig. 2 and Extended Data Fig. 4l, m). The remaining three cell lines do not regulate HER2 transcripts by cell density, but respond to progesterone similarly to the TUBO cell line and primary mammary cell cultures of BALB-NeuT mice (see Fig. 2 and Extended Data Fig. 4l, m). We did not perform functional assays with BT549 (triple negative subtype), T47D (luminal, MCF7-like), MDA-MB-175, ZR75-1 (luminal, CAMA1-like), hTERT-HME (transformed normal, similar to MCF10A) because of breast cancer subtype redundancy or poor growth (HCC1569). y axes show the percentage of migrating cells (left) and observed spheres (right) relative to seeded cells. Data are mean ± s.d. For gel source data, see Supplementary Fig. 1.
Extended Data Figure 6 Differentiation ability and metastasis formation.
a, b, Representative images (a) and quantification (b) of PGR expression of mammary epithelial cells from wild-type BALB/c mice at 4, 8, 25 and 40 weeks of age. Scale bars, 100 μm. PGR expression was reduced by 75% in 40-week-old wild-type mammary gland compared to 4-week-old mice and disappeared in primary tumours (see also Extended Data Figs 1f, 2a). n, number of ducts or glands (in early lesions and normal tissue) or visual fields in primary tumours. c, d, Representative micrographs of lesions 8 weeks after transplantation of early lesion spheres resembling DCIS (c) or less-advanced early lesions (d) displaying PGR expression (brown nuclear staining). e, Tumour growth from primary tumourspheres in young and old recipients. f, Differentiation of cells from early lesions but not of primary tumour cells in Matrigel (left) or in sphere culture (right) into acinus-like structures. Progesterone stimulation accelerated formation of acinus-like structures by early lesion cells, under mammosphere conditions. NED, no evidence of differentiation. g, Staining for CK8/18, PGR and EpCAM (epithelial cell adhesion molecule) shows expression of PGR and CK8/18 only in differentiated structures (top) compared to undifferentiated spheres (bottom). h, i, Primary tumourspheres were transplanted alone (n = 23) or co-transplanted with MM3MG–Pgr-B (n = 5) or MM3MG spheres (n = 5). DCCs numbers in bone marrow (h) and the number of mice with tumours (i) were checked 4 weeks later. Pgr-B-transduced mammary epithelia suppressed metastatic dissemination and accelerated tumour formation from primary tumourspheres. j, Pregnancy at the early lesion stage induces dissemination. A group of young BALB-NeuT mice mated (n = 5) at the early lesion stage (7-week-old) and were killed at the end of pregnancy. These mice did not form palpable tumours, but had a higher number of DCCs compared to unmated control mice (n = 6). k, Pregnancy at the advanced tumour stage. A group of BALB-NeuT mice (n = 5) were mated at the time of in situ carcinoma (15-week-old) and killed at the end of pregnancy. All pregnant mice had faster growing tumours compared to unmated control mice. l, Schematic of transplantation protocol for mammary gland or primary tumour tissue pieces into wild-type recipients. m, Example of primary tumour and macro-metastasis assessment. n, Number of metastatic foci in transplanted mice. 18 mice from the gland model and 3 mice from the tumour model were excluded from analyses owing to the fusion of metastatic lesions, which made it difficult to count individual lesions. o, Similar growth kinetics of primary tumours from gland and tumour piece models for samples from the red box in Fig. 4e. p, q, Mice from o were compared for the duration of the follow-up period after surgery. Mice from both groups were killed at the first signs of general health deterioration, which occurred earlier in gland-model mice (p). Longer follow-up time after curative surgery did not result in more metastases in recipients transplanted with primary tumour pieces (q).*P ≤ 0.05; **P ≤ 0.01; ***P ≤ 0.001; ****P ≤ 0.0001; NS, not significant; (Student’s t-test (b, f, h, j); Fisher’s exact test (i); F-test for the slopes (c, k); Mann–Whitney U-test (n–q)). Data are shown as mean ± s.d. (b, e, f, k) or median (h, j, n–q).
Extended Data Figure 7 Array CGH analysis of primary tumour–metastasis pairs.
a, Number of aberrations detected by array comparative genomic hybridization in primary tumours and matched lung metastases. Dot plot with median; statistical analysis by Mann–Whitney U-test. b, Heatmap of copy number states for the 28 primary tumours and 44 matched metastases across chromosomes 1–19 and X. Light, medium and dark yellow or blue colours indicate weak, intermediate and strong amplification (yellow) or deletion (blue) amplitudes, respectively (thresholds at ± 0.1, ± 0.2, ± 0.3). c, Prototype aberrations (top) constructed from segmented array CGH profiles (bottom) of the primary tumour (PT) and the matched metastases (Met 1–3) of mouse 3769 (phylogenetic tree and phylogenetic paths displayed in Fig. 4h, i). Prototypes (top) are organized in stacked rows per chromosome and numbered according to chromosome and positional order of their first change point, for example, 1.2 denotes the second prototype of chromosome 1. These prototype aberrations are then used to construct the phylogenetic paths (for example, Fig. 4i) and trees. For better visibility, small focal aberrations were enlarged to have a minimal extension of 300 probes. Yellow, amplification (+1); blue, deletion (−1). Corresponding segmentation profiles of the normalized and wavy-pattern-corrected array CGH data (grey dots) are indicated by red lines (bottom). For segmentation and prototype construction, see Methods. d, Table for calculating the relative time points of dissemination (Fig. 4j). PT ab, number of aberrations in the primary tumour; Mk ab, number of aberrations in the matched metastases (k = 1, 2, 3); PT–Mk cab, number of common aberrations between primary tumours and metastases; PT–Mk pcab, proportion of common aberrations relative to the primary tumour, that is, pcab = cab/PT ab.
Extended Data Figure 8 Phylogenetic analysis of metastasis (early divergence).
Phylogenetic trees of the top 13 out of 28 primary tumours and matched metastasis samples listed according to earliest time point of dissemination (for details see tables in Extended Data Figs 7, 9). A1–7, inferred common ancestors (intermediates); M, metastases (M1–3); N, normal cell; P, primary tumour. (see Methods). The ordinate indicates the number of aberrations per profile (on a square root scale). For the first three matched samples, the phylogenetic tree paths (middle), prototype aberrations (top right) and segmented array CGH profiles (bottom right) are also shown in addition to the phylogenetic tree (left). Aberration profiles along phylogenetic paths run from N via A1–7 to P or M1–3. Aberration prototypes are named according to chromosome and positional order of their first change point, for example, 2.2 denotes the second aberration prototype of chromosome 2 (see Methods and Extended Data Fig. 7c).
Extended Data Figure 9 Phylogenetic analysis of metastasis (late divergence).
a, Phylogenetic trees of the top 14 out of 28 primary tumour and matched metastasis samples listed according to latest time point of dissemination. For the first three mice the phylogenetic paths (mid), prototype aberrations (top right) and segmented array CGH profiles (bottom right) are also shown next to the phylogenetic tree (left). See Methods and Extended Data Figs 7, 8. b, Summary table of all phylogenetic analyses indicates the position of the corresponding mouse phylogenetic tree in Extended Data Figs 8 and 9 (EDF8 and EDF9) for each primary tumour–metastasis pair. The two bottom rows indicate the rank and the corresponding relative time point of dissemination as measured by the proportion of aberrations shared between primary tumour and metastasis (PT–M pcab; see Extended Data Fig. 7 and Fig. 4j). Note that only metastases ranked on position 36–44 diverged late. The phylogenetic tree and phylogenetic paths for mouse 3769 are displayed in Fig. 4h, i. In the pos-EDF8 and pos-EDF9 rows the darker colours are samples of which all data, including phylogenetic paths, prototype aberrations, segmented array CGH profiles and phylogenetic trees are shown. Faint colours cells in pos-EDF8 and pos-EDF9 are samples where only phylogenetic trees are shown.
Extended Data Figure 10 PGR, HER2 signalling and dissemination in breast cancer patients.
a, Double staining of a HER2high/PGRhigh human breast cancer sample (PGR, brown, nucleus; HER2, red/pink, membrane). Cells with varying expression levels of HER2 and PGR, as well as negative, single- or double-positive cells can be seen. Scale bar, 100 μm. Arrows indicate, double-positive (DP), double-negative (DN) and single-positive (SP) cells. b, Lack of PGR expression in high-density areas of HER2high/PGRhigh-classified tumour samples (see Fig. 5c) is directly linked to high miR-9-5p and miR-30a-5p expression. Data are mean ± s.d.
Supplementary information
Supplementary Information
This file contains Supplementary Figure 1, uncropped western blot gels and Supplementary Tables 1-11. (PDF 1456 kb)
Supplementary Data 1
This file contains microarray analyses. (XLS 8350 kb)
Supplementary Data 2
This file contains miRNA-Seq analyses. (XLSX 974 kb)
Source data
Rights and permissions
About this article
Cite this article
Hosseini, H., Obradović, M., Hoffmann, M. et al. Early dissemination seeds metastasis in breast cancer. Nature 540, 552–558 (2016). https://doi.org/10.1038/nature20785
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature20785
This article is cited by
-
Plasma THBS1 as a predictive biomarker for poor prognosis and brain metastasis in patients with HER2-enriched breast cancer
International Journal of Clinical Oncology (2024)
-
Breast metastatic tumors in lung can be substituted by lung-derived malignant cells transformed by alternative splicing H19 lncRNA
Breast Cancer Research (2023)
-
Circulating tumour cells for early detection of clinically relevant cancer
Nature Reviews Clinical Oncology (2023)
-
Biology, vulnerabilities and clinical applications of circulating tumour cells
Nature Reviews Cancer (2023)
-
DNA methylation at quantitative trait loci (mQTLs) varies with cell type and nonheritable factors and may improve breast cancer risk assessment
npj Precision Oncology (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.