Abstract
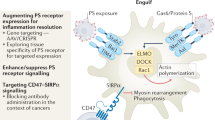
Atherosclerosis is the disease process that underlies heart attack and stroke1. Advanced lesions at risk of rupture are characterized by the pathological accumulation of diseased vascular cells and apoptotic cellular debris2. Why these cells are not cleared remains unknown3. Here we show that atherogenesis is associated with upregulation of CD47, a key anti-phagocytic molecule that is known to render malignant cells resistant to programmed cell removal, or ‘efferocytosis’4,5,6,7. We find that administration of CD47-blocking antibodies reverses this defect in efferocytosis, normalizes the clearance of diseased vascular tissue, and ameliorates atherosclerosis in multiple mouse models. Mechanistic studies implicate the pro-atherosclerotic factor TNF-α as a fundamental driver of impaired programmed cell removal, explaining why this process is compromised in vascular disease. Similar to recent observations in cancer5, impaired efferocytosis appears to play a pathogenic role in cardiovascular disease, but is not a fixed defect and may represent a novel therapeutic target.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Libby, P., Ridker, P. M. & Hansson, G. K. Progress and challenges in translating the biology of atherosclerosis. Nature 473, 317–325 (2011)
Schrijvers, D. M., De Meyer, G. R., Kockx, M. M., Herman, A. G. & Martinet, W. Phagocytosis of apoptotic cells by macrophages is impaired in atherosclerosis. Arterioscler. Thromb. Vasc. Biol. 25, 1256–1261 (2005)
Thorp, E. & Tabas, I. Mechanisms and consequences of efferocytosis in advanced atherosclerosis. J. Leukoc. Biol. 86, 1089–1095 (2009)
Oldenborg, P. A. et al. Role of CD47 as a marker of self on red blood cells. Science 288, 2051–2054 (2000)
Chao, M. P., Majeti, R. & Weissman, I. L. Programmed cell removal: a new obstacle in the road to developing cancer. Nat. Rev. Cancer 12, 58–67 (2011)
Gardai, S. J. et al. Cell-surface calreticulin initiates clearance of viable or apoptotic cells through trans-activation of LRP on the phagocyte. Cell 123, 321–334 (2005)
Majeti, R. et al. CD47 is an adverse prognostic factor and therapeutic antibody target on human acute myeloid leukemia stem cells. Cell 138, 286–299 (2009)
Kinchen, J. M. & Ravichandran, K. S. Phagocytic signaling: you can touch, but you can’t eat. Curr. Biol. 18, R521–R524 (2008)
Fadok, V. A. et al. Macrophages that have ingested apoptotic cells in vitro inhibit proinflammatory cytokine production through autocrine/paracrine mechanisms involving TGF-β, PGE2, and PAF. J. Clin. Invest. 101, 890–898 (1998)
Henson, P. M., Bratton, D. L. & Fadok, V. A. Apoptotic cell removal. Curr. Biol. 11, R795–R805 (2001)
World Health Organization. The top ten causes of death. http://www.who.int/mediacentre/factsheets/fs310/en/ (2014)
Shankman, L. S. et al. KLF4-dependent phenotypic modulation of smooth muscle cells has a key role in atherosclerotic plaque pathogenesis. Nat. Med. 21, 628–637 (2015)
Tabas, I. Macrophage death and defective inflammation resolution in atherosclerosis. Nat. Rev. Immunol. 10, 36–46 (2010)
Thorp, E., Cui, D., Schrijvers, D. M., Kuriakose, G. & Tabas, I. Mertk receptor mutation reduces efferocytosis efficiency and promotes apoptotic cell accumulation and plaque necrosis in atherosclerotic lesions of apoe−/− mice. Arterioscler. Thromb. Vasc. Biol. 28, 1421–1428 (2008)
Willingham, S. B. et al. The CD47-signal regulatory protein alpha (SIRPα) interaction is a therapeutic target for human solid tumors. Proc. Natl Acad. Sci. USA 109, 6662–6667 (2012)
Perisic, L. et al. Profiling of atherosclerotic lesions by gene and tissue microarrays reveals PCSK6 as a novel protease in unstable carotid atherosclerosis. Arterioscler. Thromb. Vasc. Biol. 33, 2432–2443 (2013)
Kojima, Y. et al. Cyclin-dependent kinase inhibitor 2B regulates efferocytosis and atherosclerosis. J. Clin. Invest. 124, 1083–1097 (2014)
Garbin, U. et al. Expansion of necrotic core and shedding of Mertk receptor in human carotid plaques: a role for oxidized polyunsaturated fatty acids? Cardiovasc. Res. 97, 125–133 (2013)
Daugherty, A., Manning, M. W. & Cassis, L. A. Angiotensin II promotes atherosclerotic lesions and aneurysms in apolipoprotein E-deficient mice. J. Clin. Invest. 105, 1605–1612 (2000)
Isenberg, J. S. et al. CD47 is necessary for inhibition of nitric oxide-stimulated vascular cell responses by thrombospondin-1. J. Biol. Chem. 281, 26069–26080 (2006)
Bäck, M. & Hansson, G. K. Anti-inflammatory therapies for atherosclerosis. Nat. Rev. Cardiol. 12, 199–211 (2015)
Hopkins, P. N. Molecular biology of atherosclerosis. Physiol. Rev. 93, 1317–1542 (2013)
Greenberg, J. D., Furer, V. & Farkouh, M. E. Cardiovascular safety of biologic therapies for the treatment of RA. Nat. Rev. Rheumatol. 8, 13–21 (2011)
Pang, W. W. et al. Hematopoietic stem cell and progenitor cell mechanisms in myelodysplastic syndromes. Proc. Natl Acad. Sci. USA 110, 3011–3016 (2013)
Feil, S. et al. Transdifferentiation of vascular smooth muscle cells to macrophage-like cells during atherogenesis. Circ. Res. 115, 662–667 (2014)
Chung, I. M., Schwartz, S. M. & Murry, C. E. Clonal architecture of normal and atherosclerotic aorta: implications for atherogenesis and vascular development. Am. J. Pathol. 152, 913–923 (1998)
McPherson, R. et al. A common allele on chromosome 9 associated with coronary heart disease. Science 316, 1488–1491 (2007)
Liu, J. et al. Pre-clinical development of a humanized anti-CD47 antibody with anti-cancer therapeutic potential. PLoS One 10, e0137345 (2015)
ClinicalTrials.gov: NCT02216409
Libby, P. Inflammation in atherosclerosis. Nature 420, 868–874 (2002)
Saksi, J. et al. Gene expression differences between stroke-associated and asymptomatic carotid plaques. J. Mol. Med. (Berl.) 89, 1015–1026 (2011)
King, J. Y. et al. Pathway analysis of coronary atherosclerosis. Physiol. Genomics 23, 103–118 (2005)
Ashley, E. A. et al. Network analysis of human in-stent restenosis. Circulation 114, 2644–2654 (2006)
Perisic, L. et al. Gene expression signatures, pathways and networks in carotid atherosclerosis. J. Intern. Med. 279, 293–308 (2016)
Chen, Y. C. et al. A novel mouse model of atherosclerotic plaque instability for drug testing and mechanistic/therapeutic discoveries using gene and microRNA expression profiling. Circ. Res. 113, 252–265 (2013)
Jun, J. et al. Effect of intermittent hypoxia on atherosclerosis in apolipoprotein E-deficient mice. Atherosclerosis 209, 381–386 (2010)
Alexander, M. R. et al. Genetic inactivation of IL-1 signaling enhances atherosclerotic plaque instability and reduces outward vessel remodeling in advanced atherosclerosis in mice. J. Clin. Invest. 122, 70–79 (2012)
Yang, H. et al. A customized and versatile high-density genotyping array for the mouse. Nat. Methods 6, 663–666 (2009)
Ghazalpour, A. et al. Comparative analysis of proteome and transcriptome variation in mouse. PLoS Genet. 7, e1001393 (2011)
Rong, J. X., Shapiro, M., Trogan, E. & Fisher, E. A. Transdifferentiation of mouse aortic smooth muscle cells to a macrophage-like state after cholesterol loading. Proc. Natl Acad. Sci. USA 100, 13531–13536 (2003)
Weiskopf, K. et al. Engineered SIRPα variants as immunotherapeutic adjuvants to anticancer antibodies. Science 341, 88–91 (2013)
Leeper, N. J. et al. Loss of CDKN2B promotes p53-dependent smooth muscle cell apoptosis and aneurysm formation. Arterioscler. Thromb. Vasc. Biol. 33, e1–e10 (2013)
Acknowledgements
This study was supported by the National Institutes of Health (R01HL12522401 and R01HL12337001 to NJL and U01HL099999 to ILW) and the Ludwig Center at Stanford. The authors wish to acknowledge J. Knowles for his critical review of the manuscript.
Author information
Authors and Affiliations
Contributions
Y.K. designed and conducted most experiments including the mouse microsurgery, morphometric analyses, in vitro cell culture, TaqMan, western blot, ChIP and luciferase reporter experiments. V.N., D.D. and L.M. assisted with the electron microscopy studies and blinded histology. J.Y., J.P.V. and K.M. conducted the in vitro efferocytosis assays and FACS studies. L.P. and U.H. performed the carotid staining and BiKE biobank analyses. A.C. provided coronary samples and assisted with the histopathological studies. M.C., A.J.L., E.S., P.B., T.Q. and C.M. conducted the microarray, co-expression and in silico bioinformatic studies. Y.K., I.L.W. and N.J.L. conceived the study, analysed the data and wrote the paper. All authors discussed the results and commented on the manuscript.
Corresponding author
Ethics declarations
Competing interests
N.J.L. and I.L.W. have filed a patent describing inhibition of CD47 as a method of preventing atherosclerosis. This patent has been licensed by Forty Seven Inc. N.J.L., J.P.V. and I.L.W. declare equity ownership in Forty Seven Inc. I.L.W. is a Director of Forty Seven, Inc.
Additional information
Reviewer Information Nature thanks I. Tabas and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Extended data figures and tables
Extended Data Figure 1 CD47 expression correlates with risk for clinical cardiovascular events and is progressively upregulated in the necrotic core of human blood vessels during atherogenesis.
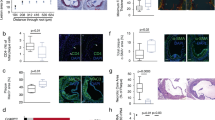
a, cDNA microarray expression profiling in the BiKE carotid endarterectomy biobank reveals that the relative expression of CD47 is increased in vascular homogenates taken from subjects with symptomatic disease (stroke or transient ischaemic attack, n = 85) compared to those with stable, asymptomatic lesions (n = 40). Similar findings were observed in the non-overlapping discovery and validation cohorts from BiKE (n = 55), and a second validation cohort from the Helsinki Carotid Endarterectomy Study (HeCES, n = 21). Data presented as Tukey box plots. b, Immunohistochemical staining reveals that CD47 co-localizes with lipidated plaque within human coronary lesions, as measured by Oil-Red-O (ORO) staining. c, Immunofluorescence staining of coronary samples confirms that CD47 is upregulated within the necrotic core. d, High magnification (40×) imaging of atherosclerotic coronary plaque confirms that CD47 expression is present on the surface of nucleated cells undergoing cell death, as indicated by HMGB1 staining. Specificity of the anti-CD47 antibody is confirmed in assays where the signal was quenched by preincubating the sections with recombinant CD47 peptide before primary antibody exposure. e, Additional representative coronary artery segments spanning the spectrum of progressive coronary artery disease (non-atherosclerotic coronary, early ‘fatty streak’, inwardly remodelled plaque, and advanced ulcerated lesion with necrotic core) confirm that CD47 is progressively upregulated during the development of coronary artery disease. The tunica media is indicated by dotted lines. f, Additional staining in human carotid artery sections confirms that CD47 expression is upregulated in atherosclerosis relative to healthy tissue, and appears most pronounced within the necrotic core. g, High magnification (100×) imaging confirms that the CD47 expression is specific to lesional cells, including SMCs (α-SMA), macrophages (CD68) and cells undergoing programmed cell death (Casp3). Comparisons made by two-tailed t-tests. **P < 0.01, *P < 0.05. Original magnification, ×40 (d), ×4 (f, g).
Extended Data Figure 2 CD47 expression is increased in mouse models of atherosclerosis.
a, Mice injected with biotin-labelled anti-CD47 antibodies reveal that these antibodies accumulate in the vasculature of atherosclerotic mice (middle), relative to non-atherosclerotic control mice (left). No staining is detected in Cd47−/− mice (right), indicating specificity of the antibody. b, Western blotting of tissue homogenates obtained from wild-type and Cd47−/− mice (with and without quenching CD47 peptide) further confirms the specificity of the antibody. For gel source data, see Supplementary Fig. 1. c, High resolution immunofluorescence staining of murine atherosclerotic plaques indicate that CD47 is specifically expressed on the surface of lesional cells, rather than extracellular debris. Original magnification, ×40. d, Publically available microarray data from laser capture microdissected (LCM) vascular tissue reveals that CD47 expression is increased within the macrophage and foam-cell-rich area of human plaque, relative to macrophage and foam-cell-poor areas (GSE23303). e, Similar results were observed in LCM tissue from mouse atherosclerotic plaque tissue, relative to non-atherosclerotic medial and adventitial tissue (GSE21419). f, g, Additional results from the Gene Expression Omnibus (GEO) database reveal that aortic CD47 expression is upregulated in murine models of atherosclerosis, as observed in the current study (GSE2372 and GSE19286). **P < 0.03, *P < 0.05.
Extended Data Figure 3 Anti-CD47 antibody reduces atherosclerotic burden in several orthogonal in vivo models.
a, Study timeline detailing osmotic minipump implantation and high-fat feeding to induce atherosclerosis in the apoE−/− and ‘angiotensin infusion’ model used herein. Kaplan–Meier curves indicate no change in mortality with anti-CD47 treatment during 28 days of follow up. b, c, Additional representative examples confirm that anti-CD47 antibody reduces atherosclerosis content in the aortic sinus (b) and reduces the percentage of the en face aorta covered by atherosclerotic plaque (c). d–g, Several additional atherosclerosis models were also used in this study to confirm the beneficial effects of anti-CD47 antibody therapy, and to model additional aspects of human cardiovascular disease, including a ‘chronic atherosclerosis’ model, where antibody therapy was given for 12 weeks (with no angiotensin infusion) (d); a ‘plaque vulnerability’ model, where the impact of antibody therapy on plaque rupture and intraplaque haemorrhage was quantified (e); an ‘established disease’ model, where therapy was given for 7 weeks after mice had already developed advanced plaques of equivalent size (f); and a ‘reduced dose’ model, where the dose of anti-CD47 antibody was reduced by 75%, relative to the preceding studies (g). h, Additionally, a ‘short term’ study was performed where mice with established lesions of equivalent size and identical apoptosis rates were pulsed for only 5 days with anti-CD47 antibodies before collection, to quantify the effect of therapy on efferocytosis rates, independent of lesion size (phagocytic index indicated by the ratio of ‘free’ (white stars) to ‘associated’ (white arrows) apoptotic bodies). Additional methodological details are provided in the Methods. Comparisons made by two-tailed t-tests. **P < 0.03, *P < 0.05. Error bars represent the s.e.m. Original magnification, ×4 (b, d–f), ×2 (c), ×10 (h).
Extended Data Figure 4 Anti-CD47 antibody promotes the phagocytosis of diseased SMCs and macrophages, without altering apoptosis.
a, In vitro caspase activity assays reveal that anti-CD47 antibody does not alter rates of programmed cell death in any vascular cell type. b, Flow cytometry assays confirm that anti-CD47 antibody has no effect on apoptosis at baseline, or in vascular SMCs exposed to 24 or 72 h of oxLDL. c, Staining controls for the in vitro phagocytosis assays. d, Representative FACS plots for the in vitro efferocytosis conditions displayed in Fig. 2e. The right upper quadrant (highlighted in red) includes double-positive cells that are taken to represent a macrophage that has ingested a target cell. e, In vitro efferocytosis assays using lipid-loaded macrophages as the target cell confirm that anti-CD47 antibody also stimulates the clearance of this vascular cell type, similar to the findings observed with SMCs. f, Additional in vitro efferocytosis assays confirm that anti-CD47 antibody stimulates phagocytosis of vascular cells in a specific manner. Error bars represent the s.e.m.
Extended Data Figure 5 Additional examples confirm the pro-efferocytic properties of anti-CD47 antibody in vivo.
a, Additional representative images detail that mice treated with anti-CD47 antibodies have a lower overall burden of apoptotic debris (caspase in green), as well as fewer examples of ‘free’ apoptotic bodies (white stars). Those apoptotic bodies that are present in these lesions are more often found in close proximity to macrophages (Mac-3 in red) and are considered ‘associated’ with a phagocyte if physically co-localized (white arrows). b, Additional electron microscopy examples provide further qualitative evidence that phagocytes present in the lesions of mice treated with anti-CD47 antibodies are more likely to have ingested several apoptotic bodies (white arrows) compared to lesions from IgG treated mice which are more likely to have a high burden of ‘free’ apoptotic bodies (yellow arrows). c–e, Additional representative examples of the necrotic core analysis (c), the phospho-SHP1 staining (d), and the plaque haemorrhage analysis (e) are shown, as described in the Methods. Original magnification, ×10 (a, d), ×4 (c, e).
Extended Data Figure 6 Full-dose anti-CD47 antibody therapy induces anaemia, but does not appear to alter NO elaboration, TSP1-dependent signalling, or other processes relevant to vascular biology.
a, No significant change in blood pressure is observed between mice treated with IgG or anti-CD47 antibodies, arguing against a systemic difference in nitric oxide (NO) production due to antibody therapy. b, Direct measurement of pulmonary NO release via the Griess reaction indicates that anti-CD47 antibody does not increase NO elaboration in vivo. c, Western blot analysis of cultured murine vascular cells reveals that anti-CD47 antibody has no effect on the expected induction of p38 and ERK phosphorylation secondary to TSP1 treatment. d, Similarly, anti-CD47 antibody has no effect on TSP1-dependent inhibition of eNOS phosphorylation, nor acetylcholine-dependent induction of eNOS phosphorylation. e, MTT assays show that anti-CD47 antibody does not affect cellular proliferation rates in the presence of TSP1. f, In vitro efferocytosis assays show that the expected basal increase in phagocytosis observed after apoptotic cells are exposed to TSP1 (black bars) is not altered in the presence of anti-CD47 antibodies (red bars). (g). Compared to mice receiving control IgG, mice receiving anti-CD47 antibody treatment have similar body weights at baseline and at time of killing. h, No difference is observed for the weight of any organ between groups, with the exception of splenomegaly observed in the anti-CD47-treated animals. i, Histological analysis of the explanted splenic tissue reveals an increase in the red pulp of anti-CD47 treated mice without any change in fibrosis or white pulp content, suggestive of increased erythrophagocytosis in this reticuloendothelial organ. j–l, Dot plots detail the haemoglobin count (j), reticulocyte count (k) and circulating monocyte count (l) for each animal in the acute 4-week angiotensin-infusion atherosclerosis model. Note that this anaemia appears to be self-limited, and no anaemia was observed in the chronic atherosclerosis model or the reduced dose model (P = 0.54 and 0.57, respectively). m, mRNA analysis of aortic tissue reveals that anti-CD47 antibody has no significant effect on the expression of macrophage-polarization factors in vivo. n, Anti-CD47 antibody also has no effect on the aortic expression of any other candidate efferocytosis genes. o–r, Additional quantitative analyses reveals that anti-CD47 antibody has no effect on in vivo neutrophil content (as assessed by Ly6G+ area normalized to lesion size) (o); macrophage content (as assessed by Mac-3+ area normalized to lesion size) (p); T-cell content (as assessed by CD3+ area across the lesion and adventitia) (q); or smooth muscle cell content (as quantified by α-SMA+ area in the aortic sinus from the external elastic lamina to the lumen) (r). s, t, Anti-CD47 antibody also had no effect on lipid level (s) or serum insulin (t). u, MTT assays reveal that anti-CD47 antibody has no effect on the proliferation of primary aortic SMCs obtained from apoE−/− mice either at baseline (left) or in the presence of 10% serum (right). Comparisons made by two-tailed t-tests, unless otherwise specified. ***P < 0.001, **P < 0.01, *P < 0.05. Error bars represent the s.e.m. For gel source data, see Supplementary Fig. 1; for detailed serological data, see Extended Data Table 1. Original magnification, ×4.
Extended Data Figure 7 Additional bioinformatic and experimental analyses further implicate a central role for TNF-α in vascular CD47 signalling.
a, Cytoscape network visualization of the genes which are significantly correlated with CD47 expression in both human and murine atherosclerotic plaque reveals a high number of TNF-α-related factors (indicated in blue), including ligands, receptors, and downstream signalling factors. b, PANTHER pathway analysis of those genes which were significantly associated with CD47 expression in mouse and human vascular tissue and have been previously associated with atherosclerosis through the STAGE study31, identifies ‘inflammation mediated by chemokine and cytokine signaling pathway’ as the most over-abundant pathway associated with CD47 expression in vascular tissue. c, Using the Hybrid Mouse Diversity Panel (HMDP), which correlates aortic gene expression with Luminex cytokine array data of plasma samples from over 100 inbred strains of mice, we found that vascular CD47 expression is positively correlated with three inflammatory cytokines in vivo, including TNF-α, IL-2 and CXCL1. Correlation data shown for CD47 and TNF-α. d, Co-expression studies confirm that TNF-α and CD47 expression are positively correlated in human carotid endarterectomy samples from the BiKE validation study. The Pearson correlation coefficient was determined assuming a Gaussian distribution and P values were determined using a two-tailed test. e, Experiments with primarily cultured mouse aortic SMCs indicate that TNF-α reproducibly induces Cd47 mRNA upregulation, whereas a number of other classical pro-atherosclerotic stimuli have no significant effect. Notably, CXCL1, IL4, TGF-β and IL-2 fail to induce CD47 expression in vitro, as assessed by ANOVA. f, Additional studies suggest that the effect of TNF-α on CD47 expression persists in the presence of oxLDL, as occurs in the atherosclerotic plaque. g, Western blotting confirms that TNF-α induces CD47 expression in vascular cells at the protein level. For gel source data, see Supplementary Fig. 1. h, Immunocytochemistry studies of HCASMCs confirm that CD47 expression is induced on the cell surface of TNF-α treated cells. TNF-α effect is assessed by co-staining for HMGB1, and antibody specificity is confirmed with isotype control and recombinant CD47 peptide quenching assays. i, Multiple assays (including FACS, TaqMan and immunocytochemistry studies) reveal that CD47 expression is downregulated on vascular SMCs during programmed cell death, as has previously been observed with inflammatory cells. j, Confirmatory assays in cultured human coronary artery SMCs reveal that TNF-α induces changes similar to those observed in murine cells (Fig. 3d), including an induction of CD47 under physiological conditions and a blunting of its expected downregulation during apoptosis. Original magnification, ×20. k, The capacity of TNF-α to impair CD47 downregulation during programmed cell death is also observed in mouse SMCs simultaneously exposed to pro-apoptotic stimuli and oxLDL. l, No correlation between CD47 and other candidate cytokines was observed in the BiKE biobank, further supporting a specific relationship between CD47 and TNF-α. m, Representative FACS-based apoptosis panels from cells exposed to the conditions used in Fig. 3g confirm that TNF-α suppresses efferocytosis (Fig. 3g) despite increasing programmed cell death. Comparisons made by two-tailed t-tests, unless otherwise specified. ***P < 0.001, *P < 0.05. Error bars represent the s.e.m.
Extended Data Figure 8 The CD47 promoter contains predicted binding sites for the TNF-α-related transcription factor NF-κB1.
a, UCSC genome browser screenshot showing overlay of human CD47 transcript with ENCODE transcription factor binding sites (including RELA, E2F4, and SRF), along with the active H3K27ac histone modification ChIP-seq track, and a custom track for chromatin accessibility in HCASMCs using the assay for transposase accessible chromatin followed by sequencing (ATAC-seq). These chromatin, DNase hypersensitivity sites, and published ChIP-seq data suggest that members of the NF-κB family of transcription factors could regulate CD47 expression in vascular tissue. b, Additional co-expression studies in the BiKE validation study confirm that NFKB1 and CD47 expression are positively correlated in human carotid endarterectomy samples. The Pearson correlation coefficient was determined assuming a Gaussian distribution and P values were determined using a two-tailed test. c, Additional luciferase promoter reporter assays reveal that induction of CD47 expression requires the presence of NF-κB1 and cannot be induced by other NF-κB co-factors such as RELA or c-REL. d, e, Time-course studies confirm that CD47 expression is induced by TNF-α within 24 h, suggesting a direct transcriptional relationship (TaqMan mRNA expression assays (d); luciferase reporter assays (e)). f, Additional chromatin immunoprecipitation studies confirm that NF-κB1 protein binds the CD47 promoter within 90 min of TNF-α-treatment in human coronary artery SMCs. **P < 0.01, *P < 0.05. Error bars represent the s.e.m.
Extended Data Figure 9 Dual inhibition of CD47 and TNF-α provides a combinatorial effect.
a, Pretreatment of mouse vascular SMCs with a chemical inhibitor (SPD 304) or a monoclonal antibody (infliximab) directed against TNF-α prevents the increase in CD47 expression normally seen after TNF-α exposure. b, Similar effects were observed with the NF-κB inhibitor, BAY 11-7085, confirming the molecular mechanism outlined in Fig. 4. c, Mice injected for four weeks with the decoy TNF-α receptor, etanercept, display a significant reduction in their in vivo expression of CD47 in splenic (left) and renal (right) tissue. d, Publically available microarray data from human clinical trials of commercially available TNF-α inhibitors reveal that subjects treated with these agents also express lower levels of CD47 in vivo (as assessed by two-tailed t-tests), confirming the mouse findings above (GSE accession numbers from left to right: 16,879 (n = 85), 12,251 (n = 22), 47,751 (n = 28) and 41,663 (n = 66)). e, f, Additional in vitro efferocytosis assays confirm a synergistic effect of anti-CD47 antibodies with a variety of TNF-α inhibitors in both the absence (e) and presence (f) of exogenous TNF-α. g, Mice with established plaques of identical size and with equivalent rates of apoptosis were treated with a short course (5 days) of IgG, anti-CD47 antibodies, etanercept, or combination therapy before collection. As shown the phagocytic index (indicated by the ratio of ‘free’ (white stars) to ‘associated’ (white arrows) apoptotic bodies) displayed a non-significant trend towards improvement for combination therapy (P > 0.05). h, When treated for a full 28 days in the angiotensin-infusion model, individual comparisons showed that etanercept alone had no effect on atherosclerosis, and combination therapy was not significantly different from anti-CD47 alone, probably due to the potent effect of anti-CD47 monotherapy. ANOVA post-hoc test analysis did identify a significant linear trend across all four groups (P for trend <0.01). i, Electron microscopy provides additional qualitative evidence that combination therapy may provide an incremental effect on efferocytosis, as suggested by an increased prevalence of macrophages within the plaque which had ingested a large number of apoptotic bodies (white arrows), a reduced prevalence of free apoptotic bodies (yellow arrows), and a reduced prevalence of uncleared cells undergoing secondary necrosis (red arrows). ***P < 0.001, **P < 0.01, *P < 0.05. Error bars represent the s.e.m.
Supplementary information
Supplementary Data
This file contains the Raw Data for Extended Data Figures 2b, 6c, 6d and 7g. (PDF 150 kb)
Rights and permissions
About this article
Cite this article
Kojima, Y., Volkmer, JP., McKenna, K. et al. CD47-blocking antibodies restore phagocytosis and prevent atherosclerosis. Nature 536, 86–90 (2016). https://doi.org/10.1038/nature18935
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature18935
This article is cited by
-
The enhanced antitumor activity of bispecific antibody targeting PD-1/PD-L1 signaling
Cell Communication and Signaling (2024)
-
Cell death by phagocytosis
Nature Reviews Immunology (2024)
-
Macrophage profiling in atherosclerosis: understanding the unstable plaque
Basic Research in Cardiology (2024)
-
Top Five Stories of the Cellular Landscape and Therapies of Atherosclerosis: Current Knowledge and Future Perspectives
Current Medical Science (2024)
-
Editorial Commentary: Top Five Stories of the Cellular Landscape and Therapies of Atherosclerosis: Current Knowledge and Future Perspectives
Current Medical Science (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.