Abstract
Changes in the gut microbiota may underpin many human diseases, but the mechanisms that are responsible for altering microbial communities remain poorly understood. Antibiotic usage elevates the risk of contracting gastroenteritis caused by Salmonella enterica serovars1, increases the duration for which patients shed the pathogen in their faeces, and may on occasion produce a bacteriologic and symptomatic relapse2,3. These antibiotic-induced changes in the gut microbiota can be studied in mice, in which the disruption of a balanced microbial community by treatment with the antibiotic streptomycin leads to an expansion of S. enterica serovars in the large bowel4. However, the mechanisms by which streptomycin treatment drives an expansion of S. enterica serovars are not fully resolved. Here we show that host-mediated oxidation of galactose and glucose promotes post-antibiotic expansion of S. enterica serovar Typhimurium (S. Typhimurium). By elevating expression of the gene encoding inducible nitric oxide synthase (iNOS) in the caecal mucosa, streptomycin treatment increased post-antibiotic availability of the oxidation products galactarate and glucarate in the murine caecum. S. Typhimurium used galactarate and glucarate within the gut lumen of streptomycin pre-treated mice, and genetic ablation of the respective catabolic pathways reduced S. Typhimurium competitiveness. Our results identify host-mediated oxidation of carbohydrates in the gut as a mechanism for post-antibiotic pathogen expansion.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Pavia, A. T. et al. Epidemiologic evidence that prior antimicrobial exposure decreases resistance to infection by antimicrobial-sensitive Salmonella. J. Infect. Dis. 161, 255–260 (1990)
Nelson, J. D., Kusmiesz, H., Jackson, L. H. & Woodman, E. Treatment of Salmonella gastroenteritis with ampicillin, amoxicillin, or placebo. Pediatrics 65, 1125–1130 (1980)
Aserkoff, B. & Bennett, J. V. Effect of antibiotic therapy in acute salmonellosis on the fecal excretion of salmonellae. N. Engl. J. Med. 281, 636–640 (1969)
Bohnhoff, M., Drake, B. L. & Miller, C. P. Effect of streptomycin on susceptibility of intestinal tract to experimental Salmonella infection. Proc. Soc. Exp. Biol. Med. 86, 132–137 (1954)
Nuccio, S. P. & Bäumler, A. J. Comparative analysis of Salmonella genomes identifies a metabolic network for escalating growth in the inflamed gut. MBio 5, e00929–14 (2014)
Kelterborn, E. Kauffmann–White–Schema (1989) 1–171 (Bundesgesundheitsamt, 1992)
Lamichhane-Khadka, R., Frye, J. G., Porwollik, S., McClelland, M. & Maier, R. J. Hydrogen-stimulated carbon acquisition and conservation in Salmonella enterica serovar Typhimurium. J. Bacteriol. 193, 5824–5832 (2011)
Lamichhane-Khadka, R., Benoit, S. L., Maier, S. E. & Maier, R. J. A link between gut community metabolism and pathogenesis: molecular hydrogen-stimulated glucarate catabolism aids Salmonella virulence. Open Biol. 3, 130146 (2013)
Barthel, M. et al. Pretreatment of mice with streptomycin provides a Salmonella enterica serovar Typhimurium colitis model that allows analysis of both pathogen and host. Infect. Immun. 71, 2839–2858 (2003)
Tsolis, R. M., Adams, L. G., Ficht, T. A. & Bäumler, A. J. Contribution of Salmonella typhimurium virulence factors to diarrheal disease in calves. Infect. Immun. 67, 4879–4885 (1999)
Ng, K. M. et al. Microbiota-liberated host sugars facilitate post-antibiotic expansion of enteric pathogens. Nature 502, 96–99 (2013)
Spees, A. M. et al. Streptomycin-induced inflammation enhances Escherichia coli gut colonization through nitrate respiration. MBio 4, e00430–13 (2013)
Stefanovic-Racic, M. et al. Comparison of the nitric oxide synthase inhibitors methylarginine and aminoguanidine as prophylactic and therapeutic agents in rat adjuvant arthritis. J. Rheumatol. 22, 1922–1928 (1995)
Palmer, R. M., Ashton, D. S. & Moncada, S. Vascular endothelial cells synthesize nitric oxide from l-arginine. Nature 333, 664–666 (1988)
de Souza, M. The use of TEMPO (2,2,6,6-tetramethylpiperidine-N-oxyl) for the oxidation of primary and secondary alcohols. Quim. Nova 27, 287–292 (2004)
Sheldon, R. A. & Arends, I. W. C. E. Organocatalytic oxidations mediated by nitroxyl radicals. Adv. Synth. Catal. 346, 1051–1071 (2004)
Ozawa, A. & Freter, R. Ecological mechanism controlling growth of Escherichia coli in continuous flow cultures and in the mouse intestine. J. Infect. Dis. 114, 235–242 (1964)
Theriot, C. M. et al. Antibiotic-induced shifts in the mouse gut microbiome and metabolome increase susceptibility to Clostridium difficile infection. Nature Commun . 5, 3114 (2014)
Hwang, I. et al. Alteration of gut microbiota by vancomycin and bacitracin improves insulin resistance via glucagon-like peptide 1 in diet-induced obesity. FASEB J. 29, 2397–2411 (2015)
Tängdén, T. & Giske, C. G. Global dissemination of extensively drug-resistant carbapenemase-producing Enterobacteriaceae: clinical perspectives on detection, treatment and infection control. J. Intern. Med. 277, 501–512 (2015)
Lawes, M. & Maloy, S. MudSacI, a transposon with strong selectable and counterselectable markers: use for rapid mapping of chromosomal mutations in Salmonella typhimurium. J. Bacteriol. 177, 1383–1387 (1995)
Winter, S. E. et al. Contribution of flagellin pattern recognition to intestinal inflammation during Salmonella enterica serotype Typhimurium infection. Infect. Immun. 77, 1904–1916 (2009)
Fiehn, O. et al. Quality control for plant metabolomics: reporting MSI-compliant studies. Plant J. 53, 691–704 (2008)
Grozdanov, L. et al. Analysis of the genome structure of the nonpathogenic probiotic Escherichia coli strain Nissle 1917. J. Bacteriol. 186, 5432–5441 (2004)
Stojiljkovic, I., Bäumler, A. J. & Heffron, F. Ethanolamine utilization in Salmonella typhimurium: nucleotide sequence, protein expression, and mutational analysis of the cchA cchB eutE eutJ eutG eutH gene cluster. J. Bacteriol. 177, 1357–1366 (1995)
Miller, S. I., Kukral, A. M. & Mekalanos, J. J. A two-component regulatory system (phoP phoQ) controls Salmonella typhimurium virulence. Proc. Natl Acad. Sci. USA 86, 5054–5058 (1989)
Rivera-Chávez, F. et al. Salmonella uses energy taxis to benefit from intestinal inflammation. PLoS Pathog. 9, e1003267 (2013)
Kingsley, R. A. et al. Molecular and phenotypic analysis of the CS54 island of Salmonella enterica serotype Typhimurium: identification of intestinal colonization and persistence determinants. Infect. Immun. 71, 629–640 (2003)
Raffatellu, M. et al. Lipocalin-2 resistance confers an advantage to Salmonella enterica serotype Typhimurium for growth and survival in the inflamed intestine. Cell Host Microbe 5, 476–486 (2009)
Winter, S. E. et al. Host-derived nitrate boosts growth of E. coli in the inflamed gut. Science 339, 708–711 (2013)
Acknowledgements
This work was supported by Public Health Service grants OD010931 (E.M.V.), AI060555 (S.-P.N.), AI096528 (A.J.B.), AI109799 (R.M.T), AI112241 (C.A.L.), AI112258 (R.M.T), AI112445 (A.J.B.), U24 DK097154 (O.F.), AI112949 (A.J.B.) and AI114922 (A.J.B.).
Author information
Authors and Affiliations
Contributions
F.F. performed bacterial growth assays, most animal experiments and analysed the results. O.F. performed GC/MS measurements. M.X.B. scored histological sections. A.J.B., L.T., C.A.L., E.M.V., T.K. and T.W. assisted with animal experiments. F.F., S.-P.N., R.M.T. and A.J.B. were responsible for the overall study design. F.F. and A.J.B. wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Additional information
Reviewer Information Nature thanks D. Bolam, D. Bumann, M. Fischbach & D. M. Monack for their contribution to the peer review of this work.
Extended data figures and tables
Extended Data Figure 1 Galactarate/glucarate fermentation by S. enterica.
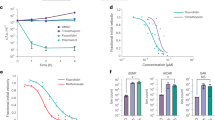
a, One of the biochemical reactions used in the Salmonella serotyping scheme by Kauffman and White is the ability to ferment galactarate6. We divided 1,367 S. enterica subspecies enterica serovars into two groups: those associated with extraintestinal disease (serovars Typhi, Paratyphi A, Paratyphi B, Paratyphi C, Sendai, Choleraesuis, Typhisuis, Dublin, Bovismorbificans, Abortusovis, Abortusequi, Gallinarum biovar Gallinarum and Galliunarum biovar Pullorum) and those associated with human gastroenteritis (the remaining 1,354 serovars). The bar graph shows the percentages of serovars in each group that are positive, negative, delayed or differing (some isolates within the serovar are positive while others are negative) for this reaction. b, Detection of galactarate in chow for conventional or germ-free mice using GC/MS (n = 4). c, Schematic drawing of the two gene clusters encoding proteins involved in the degradation of glucarate and galactarate in S. Typhimurium (ATCC14028), E. coli (Nissle 1917) and Klebsiella oxytoca (KCTC1686). Arrows indicate genes. The bracket indicates the DNA region deleted in the indicated mutants. d, Minimal medium or mucin broth supplemented with the indicated carbon sources (0.1% w/v) was inoculated with a 1:1 mixture of the wild-type S. Typhimurium and indicated mutants. Competitive index (CI) recovered after 24 h incubation in an anaerobic chamber. e, Streptomycin-treated C57BL6 mice (n = 6) were infected with a 1:1 mixture of the indicated S. Typhimurium strains and the competitive index in colon contents determined 4 days after infection. Bars represent geometric means ± standard errors (d, e). A Student’s t-test was applied to determine statistical significance.
Extended Data Figure 2 Evaluation of caecal inflammation in streptomycin-treated mice 4 days after S. Typhimurium infection.
a, Streptomycin pre-treated mice were infected with the indicated strain mixtures and caecal histopathology was scored four days later for four mice per group. The criteria used for histopathology scoring are listed in Extended Data Table 4. Each bar represents data from an individual animal. b, Representative images of haematoxylin and eosin (H&E)-stained caecal sections scored in a, along with an image from a mock-infected mouse for comparison. All images were taken at the same magnification. m, mucosa; s, submucosa; ml, muscle layer; lu, lumen.
Extended Data Figure 3 Detection of galactaric acid and glucaric acid by GC/MS.
a, Representative GC elution profile of a caecal sample containing galactaric acid and glucaric acid (arrows). b, Representative single ion monitoring scan spectrum of galactaric acid and glucaric acid.
Extended Data Figure 4 Elevated Nos2 expression leads to nitrosyl radical-mediated oxidation of galactose.
a, Expression levels of Nos2 mRNA in RNA isolated from the caecal tip three days after mock-treatment (mock) or treatment of mice with streptomycin (Strep) was determined by quantitative real-time PCR. Bars represent geometric means ± standard errors. A Student’s t-test was applied to determine statistical significance. b, Schematic of the oxidation of galactose to galactarate by TEMPO. 2,2,6,6-tetramethyl piperidine-1-oxyl (TEMPO) is a stable free nitrosyl radical that can oxidize terminal alcohol and aldehyde groups to carboxyl groups15. Consumption of TEMPO during the redox reaction is prevented by addition of a co-oxidant (NaOCl), which regenerates the nitrosyl radical.
Extended Data Figure 5 Galactarate/glucarate fermentation by E. coli.
a, Minimal medium or mucin broth supplemented with the indicated carbon sources was inoculated with a 1:1 mixture of the E. coli wild type (wt) and a garDXP garD mutant. CI, competitive index recovered after 24 h incubation in an anaerobic chamber. Growth was verified with 3 biological replicates. b, Streptomycin-treated C57BL6 mice (n = 6) were infected with a 1:1 mixture of the indicated E. coli strains and received the iNOS inhibitor aminoguanidine (AG) or vehicle control. The competitive index in colon contents was determined four days after infection. Bars represent geometric means ± standard errors (a, b). A Student’s t-test was applied to determine statistical significance.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Faber, F., Tran, L., Byndloss, M. et al. Host-mediated sugar oxidation promotes post-antibiotic pathogen expansion. Nature 534, 697–699 (2016). https://doi.org/10.1038/nature18597
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature18597
This article is cited by
-
Delayed gut microbiota maturation in the first year of life is a hallmark of pediatric allergic disease
Nature Communications (2023)
-
Gut Microbiota Resilience Mechanisms Against Pathogen Infection and its Role in Inflammatory Bowel Disease
Current Clinical Microbiology Reports (2023)
-
Oxidative ornithine metabolism supports non-inflammatory C. difficile colonization
Nature Metabolism (2022)
-
Resistance is futile? Mucosal immune mechanisms in the context of microbial ecology and evolution
Mucosal Immunology (2022)
-
Genomic signatures of host adaptation in group B Salmonella enterica ST416/ST417 from harbour porpoises
Veterinary Research (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.