Abstract
During the blood stages of malaria, several hundred parasite-encoded proteins are exported beyond the double-membrane barrier that separates the parasite from the host cell cytosol1,2,3,4,5,6. These proteins have a variety of roles that are essential to virulence or parasite growth7. There is keen interest in understanding how proteins are exported and whether common machineries are involved in trafficking the different classes of exported proteins8,9. One potential trafficking machine is a protein complex known as the Plasmodium translocon of exported proteins (PTEX)10. Although PTEX has been linked to the export of one class of exported proteins10,11, there has been no direct evidence for its role and scope in protein translocation. Here we show, through the generation of two parasite lines defective for essential PTEX components (HSP101 or PTEX150), and analysis of a line lacking the non-essential component TRX2 (ref. 12), greatly reduced trafficking of all classes of exported proteins beyond the double membrane barrier enveloping the parasite. This includes proteins containing the PEXEL motif (RxLxE/Q/D)1,2 and PEXEL-negative exported proteins (PNEPs)6. Moreover, the export of proteins destined for expression on the infected erythrocyte surface, including the major virulence factor PfEMP1 in Plasmodium falciparum, was significantly reduced in PTEX knockdown parasites. PTEX function was also essential for blood-stage growth, because even a modest knockdown of PTEX components had a strong effect on the parasite’s capacity to complete the erythrocytic cycle both in vitro and in vivo. Hence, as the only known nexus for protein export in Plasmodium parasites, and an essential enzymic machine, PTEX is a prime drug target.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Marti, M., Good, R. T., Rug, M., Knuepfer, E. & Cowman, A. F. Targeting malaria virulence and remodeling proteins to the host erythrocyte. Science 306, 1930–1933 (2004)
Hiller, N. L. et al. A host-targeting signal in virulence proteins reveals a secretome in malarial infection. Science 306, 1934–1937 (2004)
Sargeant, T. J. et al. Lineage-specific expansion of proteins exported to erythrocytes in malaria parasites. Genome Biol. 7, R12 (2006)
van Ooij, C. et al. The malaria secretome: from algorithms to essential function in blood stage infection. PLoS Pathog. 4, e1000084 (2008)
Boddey, J. A. et al. Role of plasmepsin V in export of diverse protein families from the Plasmodium falciparum exportome. Traffic 14, 532–550 (2013)
Heiber, A. et al. Identification of new PNEPs indicates a substantial non-PEXEL exportome and underpins common features in Plasmodium falciparum protein export. PLoS Pathog. 9, e1003546 (2013)
Maier, A. G. et al. Exported proteins required for virulence and rigidity of Plasmodium falciparum-infected human erythrocytes. Cell 134, 48–61 (2008)
Boddey, J. A. & Cowman, A. F. Plasmodium nesting: remaking the erythrocyte from the inside out. Annu. Rev. Microbiol. 67, 243–269 (2013)
Elsworth, B., Crabb, B. S. & Gilson, P. R. Protein export in malaria parasites: an update. Cell. Microbiol. 16, 355–363 (2014)
de Koning-Ward, T. F. et al. A newly discovered protein export machine in malaria parasites. Nature 459, 945–949 (2009)
Riglar, D. T. et al. Spatial association with PTEX complexes defines regions for effector export into Plasmodium falciparum-infected erythrocytes. Nature Commun. 4, 1415 (2013)
Matthews, K. et al. The Plasmodium translocon of exported proteins (PTEX) component thioredoxin-2 is important for maintaining normal blood-stage growth. Mol. Microbiol. 89, 1167–1186 (2013)
Matz, J. M., Matuschewski, K. & Kooij, T. W. Two putative protein export regulators promote Plasmodium blood stage development in vivo. Mol. Biochem. Parasitol. 191, 44–52 (2013)
Bullen, H. E. et al. Biosynthesis, localisation and macromolecular arrangement of the Plasmodium falciparum translocon of exported proteins; PTEX. J. Biol. Chem. 287, 7871–7884 (2012)
Pino, P. et al. A tetracycline-repressible transactivator system to study essential genes in malaria parasites. Cell Host Microbe 12, 824–834 (2012)
Haase, S., Hanssen, E., Matthews, K., Kalanon, M. & de Koning-Ward, T. F. The exported protein PbCP1 localises to cleft-like structures in the rodent malaria parasite Plasmodium berghei. PLoS ONE 8, e61482 (2013)
Pasini, E. M. et al. Proteomic and genetic analysis demonstrate that Plasmodium berghei blood stages export a large and diverse repertoire of proteins. Mol. Cell. Proteomics 12, 426–448 (2012)
Drew, D. R., Sanders, P. & Crabb, B. S. Plasmodium falciparum merozoite surface protein 8 is a ring-stage membrane protein that localizes to the parasitophorous vacuole of infected erythrocytes. Infect. Immun. 73, 3912–3922 (2005)
de Koning-Ward, T. F., Drew, D. R., Chesson, J. M., Beeson, J. & Crabb, B. S. Truncation of Plasmodium berghei merozoite surface protein 8 does not affect in vivo blood-stage development. Mol. Biochem. Parasitol. 159, 69–72 (2008)
Prommana, P. et al. Inducible knockdown of Plasmodium gene expression using the glmS ribozyme. PLoS ONE 8, e73783 (2013)
Salanti, A. et al. Evidence for the involvement of VAR2CSA in pregnancy-associated malaria. J. Exp. Med. 200, 1197–1203 (2004)
Culvenor, J. G., Day, K. P. & Anders, R. F. Plasmodium falciparum ring-infected erythrocyte surface antigen is released from merozoite dense granules after erythrocyte invasion. Infect. Immun. 59, 1183–1187 (1991)
Pologe, L. G. & Ravetch, J. V. A chromosomal rearrangement in a P. falciparum histidine-rich protein gene is associated with the knobless phenotype. Nature 322, 474–477 (1986)
Sleebs, B. E. et al. Inhibition of Plasmepsin V activity demonstrates its essential role in protein export, PfEMP1 display and survival of malaria parasites. PLoS Biol. 12, e1001897 (2014)
Blisnick, T. et al. Pfsbp1, a Maurer’s cleft Plasmodium falciparum protein, is associated with the erythrocyte skeleton. Mol. Biochem. Parasitol. 111, 107–121 (2000)
Riglar, D. T. et al. Super-resolution dissection of coordinated events during malaria parasite invasion of the human erythrocyte. Cell Host Microbe 9, 9–20 (2011)
Cooke, B. M. et al. A Maurer’s cleft-associated protein is essential for expression of the major malaria virulence antigen on the surface of infected red blood cells. J. Cell Biol. 172, 899–908 (2006)
Cooke, B. M., Rogerson, S. J., Brown, G. V. & Coppel, R. L. Adhesion of malaria-infected red blood cells to chondroitin sulfate A under flow conditions. Blood 88, 4040–4044 (1996)
Crabb, B. S. et al. Targeted gene disruption shows that knobs enable malaria-infected red cells to cytoadhere under physiological shear stress. Cell 89, 287–296 (1997)
Janse, C. J., Ramesar, J. & Waters, A. P. High-efficiency transfection and drug selection of genetically transformed blood stages of the rodent malaria parasite Plasmodium berghei. Nature Protocols 1, 346–356 (2006)
Rogerson, S. J., Chaiyaroj, S. C., Ng, K., Reeder, J. C. & Brown, G. V. Chondroitin sulfate A is a cell surface receptor for Plasmodium falciparum-infected erythrocytes. J. Exp. Med. 182, 15–20 (1995)
Boyle, M. J. et al. Isolation of viable Plasmodium falciparum merozoites to define erythrocyte invasion events and advance vaccine and drug development. Proc. Natl Acad. Sci. USA 107, 14378–14383 (2010)
de Koning-Ward, T. F. et al. A new rodent model to assess blood stage immunity to the Plasmodium falciparum antigen merozoite surface protein 119 reveals a protective role for invasion inhibitory antibodies. J. Exp. Med. 198, 869–875 (2003)
Boyle, M. J., Richards, J. S., Gilson, P. R., Chai, W. & Beeson, J. G. Interactions with heparin-like molecules during erythrocyte invasion by Plasmodium falciparum merozoites. Blood 115, 4559–4568 (2010)
Umbers, A. J. et al. Placental malaria-associated inflammation disturbs the insulin-like growth factor axis of fetal growth regulation. J. Infect. Dis. 203, 561–569 (2011)
Beeson, J. G. et al. Antigenic differences and conservation among placental Plasmodium falciparum-infected erythrocytes and acquisition of variant-specific and cross-reactive antibodies. J. Infect. Dis. 193, 721–730 (2006)
Avril, M. et al. Immunization with VAR2CSA-DBL5 recombinant protein elicits broadly cross-reactive antibodies to placental Plasmodium falciparum-infected erythrocytes. Infect. Immun. 78, 2248–2256 (2010)
Hommel, M. et al. Evaluation of the antigenic diversity of placenta-binding Plasmodium falciparum variants and the antibody repertoire among pregnant women. Infect. Immun. 78, 1963–1978 (2010)
Beeson, J. et al. Antibodies to variant surface antigens of Plasmodium falciparum-infected erythrocytes and adhesion inhibitory antibodies are associated with placental malaria and have overlapping and distinct targets. J. Infect. Dis. 189, 540–551 (2004)
Chan, J. A. et al. Targets of antibodies against Plasmodium falciparum-infected erythrocytes in malaria immunity. J. Clin. Invest. 122, 3227–3238 (2012)
Maier, A. G. et al. Skeleton-binding protein 1 functions at the parasitophorous vacuole membrane to traffic PfEMP1 to the Plasmodium falciparum-infected erythrocyte surface. Blood 109, 1289–1297 (2007)
Beeson, J. G. et al. Plasmodium falciparum isolates from infected pregnant women and children are associated with distinct adhesive and antigenic properties. J. Infect. Dis. 180, 464–472 (1999)
Acknowledgements
We thank T. Templeton, B. Franke-Fayard, C. Janse, A. Cowman, J. Boddey, B. Cooke, M. Duffy, L. Tilley, R. Anders, F. Fowkes, A. McLean and D. Bursac for reagents and/or other assistance with aspects of this study; D. Stanisic, F. Baiwog and I. Mueller for contributions to clinical studies of pregnant women; and P. Siba. We also thank the Australian Red Cross Blood Bank for the provision of human blood and serum. This work was supported by grants from the National Health and Medical Research Council (NHMRC) of Australia (1021560, 1025665 and 637406) and the Victorian State Government Operational Infrastructure Support Scheme. T.F.d.K.-W. is an NHMRC Career Development Fellow, and J.G.B. is a NHMRC Senior Research Fellow. B.E. and K.M. are the recipients of Australian Postgraduate Awards.
Author information
Authors and Affiliations
Contributions
B.E., K.M,. P.R.G. and T.F.d.K.-W. designed, performed and interpreted much of the experimental work. B.S.C. designed and interpreted the work and, along with P.R.G. and T.F.d.K.-W., wrote the manuscript. C.Q.N., M.K., S.C.C., P.R.S., S.A.C. and N.A.C. performed experiments and provided intellectual insight into aspects of this study. P.J.S., P.P., J.C., M.F.A., J.G.B. and S.J.R. provided reagents and intellectual input into study design. All authors commented on the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Extended data figures and tables
Extended Data Figure 1 Disruption of P. berghei TRX2 leads to reduced protein export.
a, IFA of fixed infected erythrocytes using P. berghei semi-immune sera reveals TRX2 knockout parasites (TRX2 KO) show reduced surface labelling compared with wild-type P. berghei ANKA parasites (WT), indicative of a reduction in expression of parasite antigens on the surface of erythrocytes infected with the TRX2 KO. Pre-bleed sera were used as a negative control. b, Quantitative FACS analysis of erythrocytes harvested from asynchronously infected mice (n = 6) show that two independent clonal populations of TRX2 KO parasites exhibit significantly reduced levels of surface labelling with P. berghei semi-immune sera compared with wild-type parasites (*P < 0.05; **P < 0.01; ***P < 0.001, unpaired t-test). c, As b, except that synchronous mouse infections were initiated by injecting purified merozoites into the tail veins of mice, and surface labelling of infected erythrocytes with semi-immune sera was performed at time points relative to when the wild-type line reinvaded erythrocytes for the second cycle (left); p.i., post invasion. Even taking into consideration that disruption of TRX2 leads to slower growth by about 6 h, the surface labelling of TRX2 KO parasites at a stage of growth comparable to that of wild-type parasites is also significantly reduced (right) (n = 3 independent experiments). d, Giemsa smears showing the stages of parasite development at time points relative to when wild-type parasites had invaded erythrocytes.
Extended Data Figure 2 Generation of a HSP101 knockdown line in P. berghei.
a, Schematic representation used to construct Pbi101 KD parasites. PCR primers used to detect 5′ integration (a/b), 3′ integration (c/d) and wild-type locus (a/d) are indicated. E, EcoRI. b, Representative experiments (n = 3) showing parasitaemias in mice that were (upper panel) or were not (lower panel) pre-exposed to ATc in their drinking water before infection. At day 4 after infection, the treatment regimens in both experiments were switched. Error bars show s.e.m. for three mice per condition performed in parallel.
Extended Data Figure 3 Knockdown of HSP101 blocks protein export.
a, Representative IFA of intraerythrocytic stages showing that export of three different P. berghei proteins across the parasitophorous vacuole membrane is blocked when Pbi101 KD, but not wild-type, is exposed to ATc. Samples were harvested at the times indicated by the asterisks in Fig. 1d and e. b, IFAs show that correct localization of EXP2 and ACP is unaffected in Pbi101 KD parasites treated with ATc (right panels). In these samples, cells were permeabilized after fixation with 0.5% Triton X-100. Because the PbANKA_114540, EXP2 and ACP antibodies were all raised in rabbits, sequential labelling with anti-PbANKA_114540, anti-rabbit AlexaFluor488, anti-EXP2 or anti-ACP, and anti-rabbit AlexaFluor568 had to be performed. Control IFAs were therefore performed in which anti-EXP2 or anti-ACP were omitted (left panels).
Extended Data Figure 4 Diagnostic PCR analysis shows the ptex150 gene has been appended with a HA tag in the PTEX150-HA parasites and a HAglmS tag in the PTEX150-HAglmS parasites.
a, Diagram of the targeted genetic crossovers and binding sites of the PCR primers. b, Using the indicated primer combinations, correct 3′- recombination has occurred in the PTEX150-HA and PTEX-HAglmS parasites using primers A/C, with a band specific to the integrated locus (1.7 kb) only observed in HA-tagged parasite lines. c, Diagram showing how the glmS ribozyme after glucosamine binding is stimulated to cleave its mRNA, resulting in message destabilization and a decrease in protein levels.
Extended Data Figure 5 Growth assays of PTEX150-HA and PTEX150-HAglmS parasites show that growth of the latter declines substantially after treatment with glucosamine (GlcN).
CS2 PTEX150-HA and CS2 PTEX150-HA-glmS parasites were treated with different concentrations of glucosamine from 24–30 h after invasion (hpi) and then allowed to invade fresh erythrocytes for 4 h. At the times after invasion indicated, the cells were stained with ethidium bromide to measure DNA content as a marker for parasite growth. Representative histograms show the levels of ethidium bromide intensity (x axis) and cell number (y axis). Infected and uninfected erythrocytes (uE) are shown as black and grey, respectively. Those parasites to the right of the red line are the strongly staining trophozoites; those to the left are the younger, weakly staining ring stages. Assays were performed at least three times independently.
Extended Data Figure 6 PTEX150-HAglmS protein levels are markedly reduced on induction of the glmS ribozyme with GlcN.
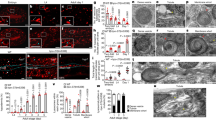
a, Western blots of PTEX150-HAglmS and control PTEX150-HA mid-ring-stage parasites (∼12 hpi) probed with the antibodies indicated on the right. GlcN was added at the concentration indicated above the blots, halfway through the previous cell cycle. b, Western blots were performed in duplicate and densitometry of the bands has been graphed showing the mean ± s.d. relative to no GlcN. Top: PTEX150 levels in the PTEX150-HAglmS (150-glmS) decrease with increasing concentrations of GlcN to a minimum ∼17% of the level without GlcN. The levels of PTEX150 in the control PTEX150-HA (150-HA) parasites does not decrease in GlcN. Middle and bottom: the levels of co-regulated HSP101 and RESA proteins and cytoplasmic constitutive HSP70-1, GAPDH and ERC proteins also decline in the PTEX150-HAglmS parasites after treatment with GlcN to about 50–60%, indicative of slowed growth due to loss of PTEX150 function. c, Western blot of infected erythrocytes treated with trypsin to cleave off surface-exposed PfEMP1. The blot has been probed with a monoclonal antibody against the intracellular C-terminal tail of PfEMP1, and the densitometry of the 350 kDa VAR2CSA band (arrow) has been compared between trypsin-treated and untreated infected erythrocytes to calculate the percentage cleaved in the presence or absence of 0.3 mM GlcN. d, IFAs of PTEX150-HAglmS probed for PfEMP1 and EXP2 after treatment with GlcN indicate a decrease in the export of PfEMP1-containing structures to the periphery of the infected erythrocyte. Scale bar, 5 μm.
Extended Data Figure 7 Export of KAHRP in PTEX150-HAglmS (glms) is decreased after treatment with GlcN.
The mean fluorescence intensity (MFI) of the erythrocyte compartment in infected erythrocytes stained with rabbit anti-KAHRP always declines after the addition of GlcN halfway through the previous cell cycle. In comparison, treatment with GlcN does not consistently decrease KAHRP export in the control PTEX150-HA (HA) parasites; the variation is possibly due to inconsistencies in sample preparation. In the graphs, the boxes and whiskers delineate the 25–75th and 10–90th centiles, respectively. Outlying data points are shown as dots. Significances: *P < 0.05; **P < 0.01; ***P < 0.001 by unpaired t-test. The number of cells (n) counted is indicated below the graph. Example immunofluorescence images of only PTEX150-HAglmS are shown. The regions occupied by the parasite are indicated by staining with DAPI and staining for EXP2. Scale bar, 5 μm.
Extended Data Figure 8 Export of SBP1 in PTEX150-HAglmS (glms) is decreased after treatment with GlcN.
The number of punctate Maurer’s clefts (MCs) present in the erythrocyte compartment in infected erythrocytes stained with rabbit anti-SBP1 nearly always declines after the addition of GlcN halfway through the previous cell cycle. In comparison, treatment with GlcN does not consistently decrease SBP1 export in the control PTEX150-HA (HA) parasites; the variation is possibly due to inconsistencies in sample preparation. In the graphs, the boxes and whiskers delineate the 25–75th and 10–90th centiles, respectively. Outlying data points are shown as dots. Significances: *P < 0.05; **P < 0.01; ***P < 0.001 by unpaired t-test. The number of cells (n) counted is indicated below the graph. Example immunofluorescence images of only PTEX150-HAglmS are shown. The regions occupied by the parasite are indicated by staining with DAPI and staining for EXP2. Scale bar, 5 μm.
Extended Data Figure 9 Export of Hyp8 in PTEX150-HAglmS (glms) is reduced following glucosamine treatment.
The number of punctate Maurer’s Clefts (MCs) present in the erythrocyte compartment in infected erythrocytes stained with rabbit anti-Hyp8 nearly always declines following addition of GlcN half way through the previous cell cycle. In comparison, GlcN treatment does not consistently reduce Hyp8 export in the control PTEX150-HA (HA) parasites and the variation is possibly due to inconsistencies in sample preparation. In the graphs, the boxes and whiskers border the 25–75th and 10–90th percentiles, respectively. Outlying data points are shown as dots. Significances: *P < 0.05; **P < 0.01; ***P < 0.001 by unpaired t-test. The number of cells (n) counted is indicated below the graph. Example immunofluorescence images of only PTEX150-HAglmS are shown. The regions occupied by the parasite are indicated by staining with DAPI and staining for EXP2. Scale bar, 5 μm.
Rights and permissions
About this article
Cite this article
Elsworth, B., Matthews, K., Nie, C. et al. PTEX is an essential nexus for protein export in malaria parasites. Nature 511, 587–591 (2014). https://doi.org/10.1038/nature13555
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature13555
This article is cited by
-
Toxoplasma protein export and effector function
Nature Microbiology (2024)
-
Histone modification analysis reveals common regulators of gene expression in liver and blood stage merozoites of Plasmodium parasites
Epigenetics & Chromatin (2023)
-
Stochastic expression of invasion genes in Plasmodium falciparum schizonts
Nature Communications (2022)
-
RhopH2 and RhopH3 export enables assembly of the RhopH complex on P. falciparum-infected erythrocyte membranes
Communications Biology (2022)
-
Cell biological analysis reveals an essential role for Pfcerli2 in erythrocyte invasion by malaria parasites
Communications Biology (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.