Abstract
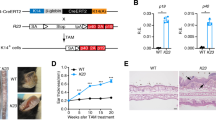
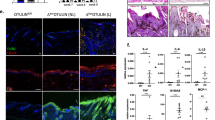
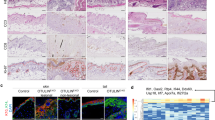
Psoriasis is a frequent, inflammatory disease of skin and joints with considerable morbidity. Here we report that in psoriatic lesions, epidermal keratinocytes have decreased expression of JunB, a gene localized in the psoriasis susceptibility region PSORS6. Likewise, inducible epidermal deletion of JunB and its functional companion c-Jun in adult mice leads (within two weeks) to a phenotype resembling the histological and molecular hallmarks of psoriasis, including arthritic lesions. In contrast to the skin phenotype, the development of arthritic lesions requires T and B cells and signalling through tumour necrosis factor receptor 1 (TNFR1). Prior to the disease onset, two chemotactic proteins (S100A8 and S100A9) previously mapped to the psoriasis susceptibility region PSORS4, are strongly induced in mutant keratinocytes in vivo and in vitro. We propose that the abrogation of JunB/activator protein 1 (AP-1) in keratinocytes triggers chemokine/cytokine expression, which recruits neutrophils and macrophages to the epidermis thereby contributing to the phenotypic changes observed in psoriasis. Thus, these data support the hypothesis that epidermal alterations are sufficient to initiate both skin lesions and arthritis in psoriasis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Schon, M. P. Animal models of psoriasis—what can we learn from them? J. Invest. Dermatol. 112, 405–410 (1999)
Nickoloff, B. J. & Nestle, F. O. Recent insights into the immunopathogenesis of psoriasis provide new therapeutic opportunities. J. Clin. Invest. 113, 1664–1675 (2004)
Shaulian, E. & Karin, M. AP-1 as a regulator of cell life and death. Nature Cell Biol. 4, E131–E136 (2002)
Eferl, R. & Wagner, E. F. AP-1: a double-edged sword in tumorigenesis. Nature Rev. Cancer 3, 859–868 (2003)
Mehic, D., Bakiri, L., Ghannadan, M., Wagner, E. F. & Tschachler, E. Fos and jun proteins are specifically expressed during differentiation of human keratinocytes. J. Invest. Dermatol. 124, 212–220 (2005)
Brocard, J. et al. Spatio-temporally controlled site-specific somatic mutagenesis in the mouse. Proc. Natl Acad. Sci. USA 94, 14559–14563 (1997)
Bonifati, C. & Ameglio, F. Cytokines in psoriasis. Int. J. Dermatol. 38, 241–251 (1999)
Uyemura, K., Yamamura, M., Fivenson, D. F., Modlin, R. L. & Nickoloff, B. J. The cytokine network in lesional and lesion-free psoriatic skin is characterized by a T-helper type 1 cell-mediated response. J. Invest. Dermatol. 101, 701–705 (1993)
Kong, J. & Li, Y. C. Upregulation of interleukin-18 expression in mouse primary keratinocytes induced to differentiate by calcium. Arch. Dermatol. Res. 294, 370–376 (2002)
Lee, E. et al. Increased expression of interleukin 23 p19 and p40 in lesional skin of patients with psoriasis vulgaris. J. Exp. Med. 199, 125–130 (2004)
Hashimoto, K. Regulation of keratinocyte function by growth factors. J. Dermatol. Sci. 24, S46–S50 (2000)
Schlingemann, J. et al. Profile of gene expression induced by the tumour promotor TPA in murine epithelial cells. Int. J. Cancer 104, 699–708 (2003)
Tanaka, T. S. et al. Genome-wide expression profiling of mid-gestation placenta and embryo using a 15,000 mouse developmental cDNA microarray. Proc. Natl Acad. Sci. USA 97, 9127–9132 (2000)
Florin, L. et al. Identification of novel AP-1 target genes in fibroblasts regulated during cutaneous wound healing. Oncogene 23, 7005–7017 (2004)
VanBuren, V. et al. Assembly, verification and initial annotation of the NIA mouse 7.4K cDNA clone set. Genome Res. 12, 1999–2003 (2002)
Broome, A. M., Ryan, D. & Eckert, R. L. S100 protein subcellular localization during epidermal differentiation and psoriasis. J. Histochem. Cytochem. 51, 675–685 (2003)
Waseem, A. et al. Keratin 15 expression in stratified epithelia: downregulation in activated keratinocytes. J. Invest. Dermatol. 112, 362–369 (1999)
Campbell, L. et al. Downregulation and altered spatial pattern of caveolin-1 in chronic plaque psoriasis. Br. J. Dermatol. 147, 701–709 (2002)
Apte, S. S., Olsen, B. R. & Murphy, G. The gene structure of tissue inhibitor of metalloproteinases (TIMP)-3 and its inhibitory activities define the distinct TIMP gene family. J. Biol. Chem. 270, 14313–14318 (1995)
Black, R. A. TIMP3 checks inflammation. Nature Genet. 36, 934–935 (2004)
Nickoloff, B. J. et al. Is psoriasis a T-cell disease? Exp. Dermatol. 9, 359–375 (2000)
Galadari, H., Fuchs, B. & Lebwohl, M. Newly available treatments for psoriatic arthritis and their impact on skin psoriasis. Int. J. Dermatol. 42, 231–237 (2003)
Cook, P. W., Pittelkow, M. R. & Piepkorn, M. Overexpression of amphiregulin in the epidermis of transgenic mice induces a psoriasis-like cutaneous phenotype. J. Invest. Dermatol. 113, 860 (1999)
Cheng, J. et al. Cachexia and graft-vs.-host-disease-type skin changes in keratin promoter-driven TNF alpha transgenic mice. Genes Dev. 6, 1444–1456 (1992)
Groves, R. W., Mizutani, H., Kieffer, J. D. & Kupper, T. S. Inflammatory skin disease in transgenic mice that express high levels of interleukin 1 α in basal epidermis. Proc. Natl Acad. Sci. USA 92, 11874–11878 (1995)
Carroll, J. M., Crompton, T., Seery, J. P. & Watt, F. M. Transgenic mice expressing IFN-gamma in the epidermis have eczema, hair hypopigmentation, and hair loss. J. Invest. Dermatol. 108, 412–422 (1997)
Guo, L., Yu, Q. C. & Fuchs, E. Targeting expression of keratinocyte growth factor to keratinocytes elicits striking changes in epithelial differentiation in transgenic mice. EMBO J. 12, 973–986 (1993)
Xia, Y. P. et al. Transgenic delivery of VEGF to mouse skin leads to an inflammatory condition resembling human psoriasis. Blood 102, 161–168 (2003)
Li, A. G., Wang, D., Feng, X. H. & Wang, X. J. Latent TGFβ1 overexpression in keratinocytes results in a severe psoriasis-like skin disorder. EMBO J. 23, 1770–1781 (2004)
Sano, S. et al. Stat3 links activated keratinocytes and immunocytes required for development of psoriasis in a novel transgenic mouse model. Nature Med. 11, 43–49 (2005)
Semprini, S. et al. Evidence for differential S100 gene over-expression in psoriatic patients from genetically heterogeneous pedigrees. Hum. Genet. 111, 310–313 (2002)
Ryckman, C., Vandal, K., Rouleau, P., Talbot, M. & Tessier, P. A. Proinflammatory activities of S100: proteins S100A8, S100A9, and S100A8/A9 induce neutrophil chemotaxis and adhesion. J. Immunol. 170, 3233–3242 (2003)
Vandal, K. et al. Blockade of S100A8 and S100A9 suppresses neutrophil migration in response to lipopolysaccharide. J. Immunol. 171, 2602–2609 (2003)
Angel, P., Szabowski, A. & Schorpp-Kistner, M. Function and regulation of AP-1 subunits in skin physiology and pathology. Oncogene 20, 2413–2423 (2001)
Johansen, C., Kragballe, K., Rasmussen, M., Dam, T. N. & Iversen, L. Activator protein 1 DNA binding activity is decreased in lesional psoriatic skin compared with nonlesional psoriatic skin. Br. J. Dermatol. 151, 600–607 (2004)
Fang, D. et al. Dysregulation of T lymphocyte function in itchy mice: a role for Itch in TH2 differentiation. Nature Immunol. 3, 281–287 (2002)
Gao, M. et al. Jun turnover is controlled through JNK-dependent phosphorylation of the E3 ligase Itch. Science 306, 271–275 (2004)
Nickoloff, B. J. The search for pathogenic T cells and the genetic basis of psoriasis using a severe combined immunodeficient mouse model. Cutis 65, 110–114 (2000)
Boyman, O. et al. Spontaneous development of psoriasis in a new animal model shows an essential role for resident T cells and tumour necrosis factor-alpha. J Exp Med 199, 731–736 (2004)
Janco, R. L. & English, D. Cyclosporine and human neutrophil function. Transplantation 35, 501–503 (1983)
Karashima, T., Hachisuka, H. & Sasai, Y. FK506 and cyclosporin A inhibit growth factor-stimulated human keratinocyte proliferation by blocking cells in the G0/G1 phases of the cell cycle. J. Dermatol. Sci. 12, 246–254 (1996)
Elomaa, O. et al. Transgenic mouse models support HCR as an effector gene in the PSORS1 locus. Hum. Mol. Genet. 13, 1551–1561 (2004)
Namazi, M. R. Paradoxical exacerbation of psoriasis in AIDS: proposed explanations including the potential roles of substance P and gram-negative bacteria. Autoimmunity 37, 67–71 (2004)
Passegue, E. & Wagner, E. F. JunB suppresses cell proliferation by transcriptional activation of p16(INK4a) expression. EMBO J. 19, 2969–2979 (2000)
Szabowski, A. et al. c-Jun and JunB antagonistically control cytokine-regulated mesenchymal-epidermal interaction in skin. Cell 103, 745–755 (2000)
Passegue, E., Jochum, W., Schorpp-Kistner, M., Mohle-Steinlein, U. & Wagner, E. F. Chronic myeloid leukemia with increased granulocyte progenitors in mice lacking junB expression in the myeloid lineage. Cell 104, 21–32 (2001)
Passegue, E., Wagner, E. F. & Weissman, I. L. JunB deficiency leads to a myeloproliferative disorder arising from hematopoietic stem cells. Cell 119, 431–443 (2004)
Kenner, L. et al. Mice lacking JunB are osteopenic due to cell-autonomous osteoblast and osteoclast defects. J. Cell Biol. 164, 613–623 (2004)
Behrens, A. et al. Impaired postnatal hepatocyte proliferation and liver regeneration in mice lacking c-jun in the liver. EMBO J. 21, 1782–1790 (2002)
Vasioukhin, V., Degenstein, L., Wise, B. & Fuchs, E. The magical touch: genome targeting in epidermal stem cells induced by tamoxifen application to mouse skin. Proc. Natl Acad. Sci. USA 96, 8551–8556 (1999)
Acknowledgements
We are grateful to M. Sibilia, G. Stingl, D. Maurer, J. Smolen, G. Schett and A. Rot for critical comments and suggestions to the manuscript, M. Cotton for providing adeno-Cre viruses, H. Tkadletz for help in preparing the illustrations and J. Hess for support with S100 protein expression analyses. The IMP is funded by Boehringer Ingelheim and this work was supported by grants from the Austrian Research Foundation, the Deutsche Forschungsgemeinschaft and by the Research Training Network (RTN) Program of the European Community.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Reprints and permissions information is available at npg.nature.com/reprintsandpermissions. The authors declare no competing financial interests.
Supplementary information
Supplementary Figure S1
No psoriasis following single epidermal deletion of either JunB or c-Jun. (JPG 246 kb)
Supplementary Figure S2
Cytokine expression after 4 days following three Tam injections. (JPG 364 kb)
Supplementary Figure S3
Cytokine expression after 18 days following Tam injections. (JPG 111 kb)
Supplementary Figure S4
Induction of JunB/c-Jun deletion in the presence of ciprofloxacin. (JPG 1140 kb)
Supplementary Figures Legends
Text to accompany the above Supplementary Figures. (DOC 21 kb)
Rights and permissions
About this article
Cite this article
Zenz, R., Eferl, R., Kenner, L. et al. Psoriasis-like skin disease and arthritis caused by inducible epidermal deletion of Jun proteins. Nature 437, 369–375 (2005). https://doi.org/10.1038/nature03963
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/nature03963
This article is cited by
-
Depletion of JunB increases adipocyte thermogenic capacity and ameliorates diet-induced insulin resistance
Nature Metabolism (2024)
-
Challenges and opportunities in animal models of psoriatic arthritis
Inflammation Research (2023)
-
Skin chronological aging drives age-related bone loss via secretion of cystatin-A
Nature Aging (2022)
-
Advances in the pathogenesis of psoriasis: from keratinocyte perspective
Cell Death & Disease (2022)
-
The endoribonuclease N4BP1 prevents psoriasis by controlling both keratinocytes proliferation and neutrophil infiltration
Cell Death & Disease (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.