Abstract
Stem cell fate is influenced by specialized microenvironments that remain poorly defined in mammals1,2,3. To explore the possibility that haematopoietic stem cells derive regulatory information from bone, accounting for the localization of haematopoiesis in bone marrow, we assessed mice that were genetically altered to produce osteoblast-specific, activated PTH/PTHrP receptors (PPRs)4. Here we show that PPR-stimulated osteoblastic cells that are increased in number produce high levels of the Notch ligand jagged 1 and support an increase in the number of haematopoietic stem cells with evidence of Notch1 activation in vivo. Furthermore, ligand-dependent activation of PPR with parathyroid hormone (PTH) increased the number of osteoblasts in stromal cultures, and augmented ex vivo primitive haematopoietic cell growth that was abrogated by γ-secretase inhibition of Notch activation. An increase in the number of stem cells was observed in wild-type animals after PTH injection, and survival after bone marrow transplantation was markedly improved. Therefore, osteoblastic cells are a regulatory component of the haematopoietic stem cell niche in vivo that influences stem cell function through Notch activation. Niche constituent cells or signalling pathways provide pharmacological targets with therapeutic potential for stem-cell-based therapies.
Similar content being viewed by others
Main
Mammalian bone marrow architecture involves haematopoietic stem cells (HSCs) in close proximity to the endosteal surfaces5,6, with more differentiated cells arranged in a loosely graduated fashion as the central longitudinal axis of the bone is approached5,7,8. This nonrandom organization of the marrow suggests a possible relationship between HSCs and osteoblasts—osteogenic cells lining the endosteal surface. Osteoblasts produce haematopoietic growth factors9,10,11 and are activated by parathyroid hormone (PTH) or the locally produced PTH-related protein (PTHrP), through the PTH/PTHrP receptor (PPR). We tested whether osteoblasts contribute to the unique microenvironment of the bone marrow in vivo using a constitutively active PPR (col1-caPPR) under the control of the α1(I) collagen promoter active in osteoblastic cells in a transgenic mouse4 (Fig. 1a).
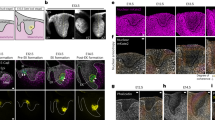
a, Representation of transgene construct. b, c, Haematoxylin and eosin staining of sections of decalcified proximal tibia from 12-week-old wild-type (WT) and transgenic (Tg) littermates. Magnifications, ×100. d, Increased frequency of Lin-Sca-1+c-Kit+ cells in transgenic bone marrow. The same symbol designates sex-matched sibling pairs (n = 6 in each group; solid bar, mean). e, Increased LTC-ICs in transgenic bone marrow Lin- haematopoietic cells grown on wild-type stroma. f, g, Bone marrow cells from col1-caPPR male mice had an increased ability to reconstitute female recipients by PCR for the Y chromosome (n = 4 in each group). h, No difference in HSCs residing in G0 and G1 (representative analysis from three separate experiments). i, Unchanged CFU-Cs.
The long bones of col1-caPPR mice had increased numbers of trabeculae (Fig. 1b, c) and trabecular osteoblastic cells, as defined by expression of osteocalcin, alkaline phosphatase, collagen type I, osteopontin and matrix metalloproteinase 13 (ref. 4). Haematopoietic cells were found in small regions between trabeculae. The bony change was restricted to the metaphyseal area and there was no substantial alteration in the overall haematopoietic cell content of the bone marrow (Supplementary Fig. 1).
Assessing the composition of the bone marrow mononuclear cell fraction (BMMC), we found that the stem-cell-enriched lineage-negative (Lin-) Sca-1+c-Kit+ subpopulation of cells was significantly greater in the bone marrow of the transgenic animals (P = 0.008; Fig. 1d). There was a corresponding increase in the absolute number per hind limb: wild-type, 32,500 ± 8,000; transgenic, 65,700 ± 7,500. Testing whether functionally defined cell types were also increased, we used the quantitative limiting-dilution ‘long-term culture-initiating cell’ (LTC-IC) assay, which linearly correlates with in vivo HSC function12. Using the Lin- fraction of BMMC as the input population, we confirmed an increase in the frequency of primitive HSC-like cells in the transgenic animals (P = 0.00009; Fig. 1e). An increase in HSCs was further corroborated by competitive transplantation of irradiated recipients that showed superior engraftment of transgenic cells (P = 0.001; Fig. 1f, g). The magnitude of the increase was comparable in the three independent stem cell assays used. As functional assays may be influenced by the cell cycle, we analysed the proportions of Sca-1+Lin- cells that were in the G0 versus G1 phase, and detected no differences between the transgenic and wild-type mice (P = 0.768; Fig. 1h). These data confirm an increase in the stem cell population in the transgenic animals. However, when the more mature progenitor population was quantified using the CFU-C (colony forming unit-culture) assay, no difference between the transgenic and wild-type animals was observed (P = 0.573; Fig. 1i). Therefore, cell expansion was not global across differentiated subsets, but was notably restricted to stem cells.
To assess whether the impact on primitive cells was dependent on stroma or haematopoietic cells, we evaluated the ability of stromal cells from wild-type or transgenic animals to support wild-type BMMC in LTC-IC assays. Stromal cells expressing the transgene demonstrated augmented support of LTC-IC (P = 0.004; Fig. 2a). So, the increased number of primitive cells in the col1-caPPR mice was stroma-determined and was independent of the haematopoietic cell genotype.
a, Stromal cells from transgenic mice (n = 6 versus n = 6 wild-type littermates) improve support of wild-type HSCs. b, Increased anti-Jag1 antibody staining (red) in sections of the proximal tibia from transgenic versus wild-type littermates. Magnifications, ×200. c, Positive anti-osteopontin antibody staining in transgenic cells expressing Jag1 in sequential representative sections of the proximal tibia from a transgenic mouse. d, Increased anti-NICD antibody staining of haematopoietic Lin-Sca-1+c-Kit+ cells from transgenic compared with wild-type littermates. Isotype controls are also shown (representative histogram from three independent experiments). e, HSC expansion mediated by col1-caPPR stromal cells was blocked by the addition of γ-secretase inhibitor to LTC-IC assays.
To assess possible mechanisms, we examined levels of the cytokines interleukin 6 (IL-6), kit ligand or stem cell factor (SCF), and the chemokine stroma-derived factor 1 (SDF-1 or CXCL12), by immunohistochemistry in cells of osteoblast origin determined by osteopontin expression (Supplementary Fig. 2). Each protein was produced at increased levels in the transgenic stroma compared with wild-type controls. To address whether these diffusible cytokines could account for the effect on primitive cells, we performed LTC-ICs across a semi-permeable membrane and noted abolition of benefit from the activated PPR (Supplementary Fig. 3). Therefore, membrane- or matrix-bound cytokines were necessary for the stromal effect on HSCs.
The Notch signalling pathway involves membrane-bound ligands and regulates cell-fate specification in a wide variety of systems, including HSC self-renewal13,14,15,16,17. By changing the balance of daughter cell self-renewal versus differentiation, Notch signalling has been shown to increase stem cell numbers without expanding mature cells in a manner reminiscent of the phenotype observed here13,16. Furthermore, the Notch ligand jagged 1 (Jag1) has been shown to be expressed by marrow stromal cells16,18 and by murine osteoblasts19. Notch activation plus cytokine receptor signalling has a combinatorial effect on haematopoietic cells14. We therefore investigated by immunohistochemistry Jag1 protein levels in the marrow of transgenic mice, and observed that overall levels of Jag1 were markedly increased (Fig. 2b). The cells expressing Jag1 were osteoblastic, as indicated by morphology and by osteopontin expression (Fig. 2c). To examine whether the haematopoietic stem cells responded to the increased expression of Jag1 in the transgenic animals, we assessed the level of the Notch1 intracellular domain (NICD) in the Lin-Sca-1+c-Kit+ HSCs from wild-type and transgenic mice. This anti-NICD antibody has previously been shown to preferentially detect the activated intracellular form of Notch1 (ref. 20). Whereas wild-type mice had minimal staining for NICD compared with isotype controls, Lin-Sca-1+c-Kit+ cells from transgenic mice had a notable increase in the level of NICD (Fig. 2d). Moreover, long-term co-cultures performed in the presence or absence of a γ-secretase inhibitor capable of blocking Notch cleavage21 showed that addition of the inhibitor reduced the supportive capacity of transgenic stroma to baseline levels (Fig. 2e). These data support a model in which PPR activation in the osteoblastic population increases cell number and the overall production of Jag1. This, in turn, may activate Notch on primitive haematopoietic cells, resulting in expansion of the stem cell compartment.
Since the col1-caPPR mice represented a genetic means of activating a receptor that could also be activated by endogenous ligand, we tested whether the effects of col1-caPPR stroma could be recapitulated through exposure of wild-type stroma to PTH. LTC-IC assays were performed using C57Bl/6 stroma expanded in vitro in the presence or absence of PTH, after which BMMC was introduced to the stroma in the presence or absence of PTH. When stroma was grown in medium containing PTH, it closely resembled the LTC-IC results using the col1-caPPR stroma, increasing LTC-IC (P = 0.004; Fig. 3a). Of note, the effect was not seen using stromal cells that were expanded in the absence of PTH, or when PTH was added at the same time as the haematopoietic cells, suggesting an effect on the composition or activity of the stroma as it matures in vitro. To assess whether there was an increase in the number of osteoblastic cells in the stromal cell cultures, we performed alkaline phosphatase staining. After 14 days, the cultures were confluent and heterogeneous, and there was an increase in the number of alkaline-phosphatase-positive cells in the PTH-treated cultures (Fig. 3b). These data confirm that activation of PPR induces an increase in the number of osteoblastic cells. To further assess whether the effects of PPR activation on primitive haematopoietic cells were due to activation of the Notch pathway, we performed LTC-IC in the presence or absence of the γ-secretase inhibitor. Addition of the inhibitor abrogated the impact of PTH on the stromal support of primitive haematopoietic cells (Fig. 3c). Therefore, Notch activation is necessary for osteoblastic-cell-induced increases in primitive haematopoietic cells. Taken together, these results support the concept that PPR activation can increase the number of osteoblastic cells, resulting in Notch1-mediated expansion of HSCs.
a, PTH-treated wild-type BM-SCs reproduce the col1-caPPR effect (SP, stromal preparation; CM, culture maintenance). b, Increased numbers of alkaline-phosphatase-positive BM-SCs (red) in PTH-treated cultures (n = 4 in both groups). c, PTH-mediated HSC expansion was blocked by the addition of γ-secretase inhibitor to LTC-IC assays. d, PTH-treated mice (n = 8) had increased Lin-Sca-1+c-Kit+ cells (mock-injected mice, n = 7) (mean absolute number per hind limb: PTH-treated, 211,000 ± 12,000; mock-treated, 139,000 ± 29,000). e, PTH-treated mice had increased LTC-IC frequency. f, Bone marrow cells from PTH-treated mice had increased ability to reconstitute secondary recipients as shown by flow cytometry for CD45.2 (n = 5 in each group). g, Unchanged CFU-C frequency (n = 5 in each group).
As the addition of exogenous PTH could influence in vitro stem cell support, we evaluated the pharmacological use of PTH in vivo. Wild-type C57Bl/6 mice were injected daily with PTH using a dosing schedule known to increase osteoblasts. After four weeks, PTH-treated mice had a significant increase in the absolute number of Lin-Sca-1+c-Kit+ cells (P = 0.0049; Fig. 3d) and LTC-IC (P = 0.0012; Fig. 3e) compared with vehicle-injected controls. To further clarify that functional HSCs were increased by PTH, competitive transplantation into secondary irradiated recipients was used and an increase in engraftment was documented (P = 0.022; Fig. 3f). These data provide evidence for an increase in the number of HSCs induced by PTH. Consistent with observations in the transgenic animals, PTH treatment did not affect the concentration of haematopoietic progenitors as assessed by CFU-C (P = 0.780; Fig. 3g). Therefore, pharmacological activation of PPR increased HSC, but appeared to do so without a broad haematopoietic cell expansion. These data are consistent with HSC expansion by enhanced self-renewal, a phenomenon known to result from Notch activation13,14,15,16,17.
To assess whether PPR stimulation could have a meaningful physiological effect, we chose a model relevant to the clinical use of stem cells in humans. PTH was administered to animals undergoing myeloablative bone marrow transplantation using limiting numbers of donor cells to mimic a setting of therapeutic need. Survival at 28 days in control mice that received mock injections after transplant was 27%. In sharp contrast, animals receiving pulse dosing of PTH had improved outcomes with 100% survival (Fig. 4a). The bone marrow histology of the two groups was also substantially different, with an increase in cellularity and a decrease in fat cells in the PTH-treated group (Fig. 4b–e). Therefore, PTH alteration of the bone marrow microenvironment can result in improved engraftment and thereby markedly affect the results of this physiological challenge. Manipulating the microenvironment is a means to influence haematopoietic outcomes that is relevant for human medicine.
a, Kaplan–Meier survival analysis of C57Bl/6 mice transplanted with limiting numbers of BMMC cells and treated with either PTH or mock injection for four weeks (n = 18 in each group from three independent experiments). Histology at four weeks of long bones from either PTH-treated animals (b, c) or mock-injected controls (d, e).
The studies reported here and in anatomical detail in the accompanying paper by Zhang et al.22 indicate that osteoblastic cells represent a regulatory component of the bone marrow microenvironment. Zhang and colleagues show that the number of these cells is influenced by bone morphogenetic protein (BMP) signalling and directly correlates with HSC number. We show that PPR signalling affects osteoblastic cells, leading to an increase in the number of HSCs through Notch activation. The concept that a stable, custom microenvironment or niche might control stem cells was initially hypothesized by Schofield23. In a niche, neighbouring subsets of cells and extracellular substrates house stem cells, and provide specialized functions to modulate stem cell self-renewal and progeny production in vivo1. Apart from gonadal tissue of the Drosophila2,3, physiological niches have not been well defined, largely owing to limited definition of functional microenvironment constituents. That the osteoblast may have a role in the haematopoietic system was first proposed by Taichman and Emerson9,24, a hypothesis for which our data and those of Zhang et al.22 now provide direct in vivo support. By identifying cellular participants that affect stem cells in trans, it might be possible to define the complexity of the niche and to tease apart the systems that direct stem cell behaviour. In so doing, strategies for altering stem cells to achieve therapeutic outcomes become feasible. We show here the potential for such an approach—the definition of the osteoblast as a participant has allowed the identification of a pharmacological manipulation for expanding primitive haematopoietic cells. PTH may be useful in stem cell expansion ex vivo or in vivo, and has potential implications for stem cell harvesting and recovery after transplantation. Understanding the interactions between bone and bone marrow may, therefore, yield practical methods for manipulating stem cells and define a model for the impact of microenvironment on cell physiology.
Methods
Sample preparation and histological analysis
Col1-caPPR mice were generated and genotyped previously, as described4. For all studies, mice were killed by CO2 asphyxiation. The institutional animal care committee approved all studies described.
Hind limbs from 12-week-old transgenic mice and sex-matched wild-type littermates were fixed, decalcified and processed as described4. For immunohistochemistry, sections were stained with anti-IL-6 goat polyclonal antibody M-19 (1:100 dilution), anti-SCF goat polyclonal antibody G-19 (1:100), anti-SDF-1 goat polyclonal antibody C-19 (1:50), anti-osteopontin goat polyclonal antibody P-18 (1:200), and anti-Jag1 rabbit polyclonal antibody H-114 (1:100) (all Santa Cruz Biotechnology, Inc.), a biotinylated rabbit anti-goat or goat anti-rabbit secondary antibody (Vector Labs), horseradish-peroxidase-conjugated streptavidin (Jackson Immuno Research), and AEC chromogen (Biocare Medical) or the Vector ABC alkaline phosphatase kit (Vector Labs). Slides were counterstained with Mayer's haematoxylin. Staining was completely absent in identical tissue sections in which the primary antibody was omitted (data not shown).
Preparation of bone marrow stromal layers
Femurs and tibias removed from euthanized mice were flushed with long-term culture medium (LTM), and bone marrow mononuclear cells (BM-MNCs) were cultured at an initial concentration of 5 × 106 cells ml-1 as described25.
Flow cytometric analysis
To immunophenotypically enumerate HSCs, single-cell suspensions of BMMC were stained with biotinylated lineage antibodies (anti-CD3, anti-CD4, anti-CD8, anti-Ter119, anti-Gr-1, anti-Mac-1 and anti-B220), anti-Sca-1 and anti-c-Kit (Pharmingen), then labelled with a secondary fluorescent-conjugated streptavidin and analysed on a FACScalibur cytometer (Becton Dickinson and Co.) using Cell Quest software. To assess the cell cycle in the primitive population, BMMC cells were stained with lineage antibodies, anti-Sca-1, Pyronin Y (RNA dye) and Hoechst 33342 (DNA dye) as described25. For intracellular NICD staining, Lin-Sca-1+c-Kit+ cells were permeabilized using the Fix and Perm cell-permeabilization kit (Caltag) and incubated with 1 µg of anti-NICD antibody and secondary goat anti-mouse antibody.
Colony-forming unit assay
Isolated BM-MNCs were assessed for CFU-C frequency as described previously25. In this study, we used the methylcellulose-containing medium M3434 (StemCell Technologies).
Long-term culture-initiating cell assay
LTC-IC frequency in Lin- BMMC preparations was quantified as described previously13.
In vitro treatment with PTH
LTC-IC assays were performed using wild-type stroma and haematopoietic cells. Rat PTH (1–34) (Bachem) or vehicle was added to each media change, either during stroma establishment and/or during culture maintenance (PTH final concentration, 10-7 M). For alkaline phosphatase staining, primary bone marrow stromal cells (BM-SCs) were cultured in 24-well plates. After 10 or 14 days, the adherent cells were fixed in 10% neutral formalin buffer, and alkaline phosphatase activity was determined histochemically by incubation with 0.1 mg ml-1 naphthol AS-MX phosphate (Sigma), 0.5% N,N-dimethylformamide, 0.6 mg ml-1 red violet LB salt (Sigma) in 0.1 M Tris-HCl (pH 8.5). To inhibit γ-secretase activity, 30 µM of γ-secretase inhibitor II (Calbiochem) in dimethylsulphoxide was added to the LTM and LTC-IC assays were performed. For non-contact LTC-ICs, BM-SC layers were plated into 96-well plates as described. BMMC cells were seeded into culture inserts with a membrane of 0.2 µm pore size (Nunc) placed in the wells.
In vivo PTH administration
Rat PTH (1–34) (Bachem) (80 µg per kg body weight) or vehicle was injected intraperitoneally five times a week for four weeks in 6–8-week-old wild-type C57Bl/6 male mice.
Bone marrow transplantation
For in vivo quantification of HSCs from wild-type and transgenic mice, 1 × 107 BM-MNCs from female FVB mice (Jackson Laboratories) were mixed with 5 × 106 cells from male wild-type or transgenic mice. Cells were injected into recipient female FVB mice lethally irradiated 24 h previously with 8.5 Gy of radiation (137Cs source). After 8 weeks, the bone marrow was removed and flushed with fully supplemented Iscove's medium. The relative contribution of engraftment from the different cell sources was assessed by semiquantitative polymerase chain reaction (PCR) for Y chromosome using primers and conditions as described previously26. Band density on the agarose gel was quantified using a ChemiImager 5500 (Alpha Innotech).
For in vivo quantification of HSCs following PTH administration, 4 × 105 BMMC cells from CD45.1 + B6.SJL mice (Jackson Laboratories) were mixed with 2 × 105 cells from vehicle-injected or PTH-injected CD45.2+ C57Bl/6 mice. Cells were injected in recipient B6.SJL mice lethally irradiated 24 h previously with 10 Gy of radiation. The relative contribution of engraftment from the different cell sources was assessed by flow cytometry of BM-MNCs using anti-CD45.1 and anti-CD45.2 antibodies (Pharmingen).
To assess post-transplantation PTH effects, lethally irradiated recipient C57Bl/6 mice were injected with 2 × 105 BM-MNCs from a donor B6.SJL mouse. Twenty-four hours later, mice were injected with PTH or vehicle for four weeks.
Statistical analysis
Results are expressed as mean ± s.e.m. Data were analysed using the unpaired two-tailed Student's t-test as appropriate for the data set. P < 0.05 was considered significant.
References
Spradling, A., Drummond-Barbosa, D. & Kai, T. Stem cells find their niche. Nature 414, 98–104 (2001)
Kiger, A. A., White-Cooper, H. & Fuller, M. T. Somatic support cells restrict germline stem cell self-renewal and promote differentiation. Nature 407, 750–754 (2000)
Tran, J., Brenner, T. J. & DiNardo, S. Somatic control over the germline stem cell lineage during Drosophila spermatogenesis. Nature 407, 754–757 (2000)
Calvi, L. M. et al. Activated parathyroid hormone/parathyroid hormone-related protein receptor in osteoblastic cells differentially affects cortical and trabecular bone. J. Clin. Invest. 107, 277–286 (2001)
Lord, B. I., Testa, N. G. & Hendry, J. H. The relative spatial distributions of CFUs and CFUc in the normal mouse femur. Blood 46, 65–72 (1975)
Gong, J. K. Endosteal marrow: a rich source of hematopoietic stem cells. Science 199, 1443–1445 (1978)
Cui, Y. F., Lord, B. I., Woolford, L. B. & Testa, N. G. The relative spatial distribution of in vitro-CFCs in the bone marrow, responding to specific growth factors. Cell Prolif. 29, 243–257 (1996)
Lord, B. I. The architecture of bone marrow cell populations. Int. J. Cell Cloning 8, 317–331 (1990)
Taichman, R. S. & Emerson, S. G. Human osteoblasts support hematopoiesis through the production of granulocyte colony-stimulating factor. J. Exp. Med. 179, 1677–1682 (1994)
Taichman, R. S., Reilly, M. J. & Emerson, S. G. Human osteoblasts support human hematopoietic progenitor cells in vitro bone marrow cultures. Blood 87, 518–524 (1996)
Taichman, R., Reilly, M., Verma, R., Ehrenman, K. & Emerson, S. Hepatocyte growth factor is secreted by osteoblasts and cooperatively permits the survival of haematopoietic progenitors. Br. J. Haematol. 112, 438–448 (2001)
Ploemacher, R. E., van der Sluijs, J. P., van Beurden, C. A., Baert, M. R. & Chan, P. L. Use of limiting-dilution type long-term marrow cultures in frequency analysis of marrow-repopulating and spleen colony-forming hematopoietic stem cells in the mouse. Blood 78, 2527–2533 (1991)
Stier, S., Cheng, T., Dombkowski, D., Carlesso, N. & Scadden, D. T. Notch1 activation increases hematopoietic stem cell self-renewal in vivo and favors lymphoid over myeloid lineage outcome. Blood 99, 2369–2378 (2002)
Varnum-Finney, B., Brashem-Stein, C. & Bernstein, I. D. Combined effects of Notch signalling and cytokines induce a multiple log increase in precursors with lymphoid and myeloid reconstituting ability. Blood 101, 1784–1789 (2003)
Varnum-Finney, B. et al. Pluripotent, cytokine-dependent, hematopoietic stem cells are immortalized by constitutive Notch1 signalling. Nature Med. 6, 1278–1281 (2000)
Karanu, F. N. et al. The notch ligand jagged-1 represents a novel growth factor of human hematopoietic stem cells. J. Exp. Med. 192, 1365–1372 (2000)
Karanu, F. N. et al. Human homologues of Delta-1 and Delta-4 function as mitogenic regulators of primitive human hematopoietic cells. Blood 97, 1960–1967 (2001)
Li, L. et al. The human homolog of rat Jagged1 expressed by marrow stroma inhibits differentiation of 32D cells through interaction with Notch1. Immunity 8, 43–55 (1998)
Pereira, R. M., Delany, A. M., Durant, D. & Canalis, E. Cortisol regulates the expression of Notch in osteoblasts. J. Cell. Biochem. 85, 252–258 (2002)
Huppert, S. S. et al. Embryonic lethality in mice homozygous for a processing-deficient allele of Notch1. Nature 405, 966–970 (2000)
Wolfe, M. S. et al. Peptidomimetic probes and molecular modeling suggest that Alzheimer's γ-secretase is an intramembrane-cleaving aspartyl protease. Biochemistry 38, 4720–4727 (1999)
Zhang, J. et al. Identification of the haematopoietic stem cell niche and control of the niche size. Nature 425, 836–841 (2003)
Schofield, R. The relationship between the spleen colony-forming cell and the haemopoietic stem cell. Blood Cells 4, 7–25 (1978)
Taichman, R. S., Reilly, M. J. & Emerson, S. G. The hematopoietic microenvironment: osteoblasts and the hematopoietic microenvironment. Hematology 4, 421–426 (2000)
Cheng, T. et al. Hematopoietic stem cell quiescence maintained by p21cip1/waf1. Science 287, 1804–1808 (2000)
Giri, N., Kaushiva, A., Wu, T., Sellers, S. E. & Tisdale, J. F. The effects of SCF/G-CSF prestimulation on radiation sensitivity and engraftment in nonmyeloablated murine hosts. Exp. Hematol. 29, 779–785 (2001)
Acknowledgements
The authors thank J. Harvey for assistance with histological analyses. This work was supported by the National Institutes of Health (L.M.C., H.M.K., E.S. and D.T.S.), the American Society of Hematology Fellow Scholar Award (G.B.A.) and the Doris Duke Foundational Burroughs Wellcome Fund (D.T.S.)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
H. M. Kronenberg participates in research sponsored by Lilly and Chugai Pharmaceuticals.
Rights and permissions
About this article
Cite this article
Calvi, L., Adams, G., Weibrecht, K. et al. Osteoblastic cells regulate the haematopoietic stem cell niche. Nature 425, 841–846 (2003). https://doi.org/10.1038/nature02040
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/nature02040
This article is cited by
-
Extramedullary hematopoiesis in cancer
Experimental & Molecular Medicine (2024)
-
Cellular niches for hematopoietic stem cells in bone marrow under normal and malignant conditions
Inflammation and Regeneration (2023)
-
Niche formation and function in developing tissue: studies from the Drosophila ovary
Cell Communication and Signaling (2023)
-
MiR-9-1 controls osteoblastic regulation of lymphopoiesis
Leukemia (2023)
-
OVOL2 sustains postnatal thymic epithelial cell identity
Nature Communications (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.