Abstract
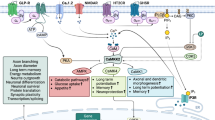
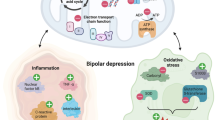
After decades of research, the mechanism of action of lithium in preventing recurrences of bipolar disorder remains only partially understood. Lithium research is complicated by the absence of suitable animal models of bipolar disorder and by having to rely on in vitro studies of peripheral tissues. A number of distinct hypotheses emerged over the years, but none has been conclusively supported or rejected. The common theme emerging from pharmacological and genetic studies is that lithium affects multiple steps in cellular signaling, usually enhancing basal and inhibiting stimulated activities. Some of the key nodes of these regulatory networks include GSK3 (glycogen synthase kinase 3), CREB (cAMP response element-binding protein) and Na+-K+ ATPase. Genetic and pharmacogenetic studies are starting to generate promising findings, but remain limited by small sample sizes. As full responders to lithium seem to represent a unique clinical population, there is inherent value and need for studies of lithium responders. Such studies will be an opportunity to uncover specific effects of lithium in those individuals who clearly benefit from the treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Schioldann J . History of the Introduction of Lithium into Medicine and Psychiatry. Adelaide, SA, Australia: Adelaide Academic Press, 2009.
Cade JFJ . Lithium salts in the treatment of psychotic excitement. Med J Aust 1949; 2: 349–351.
Blanco C, Laje G, Olfson M, Marcus SC, Pincus HA . Trends in the treatment of bipolar disorder by outpatient psychiatrists. Am J Psychiatry 2002; 159: 1005–1010.
Bramness JG, Weitoft GR, Hallas J . Use of lithium in the adult populations of Denmark, Norway and Sweden. J Affect Disord 2009; 118: 224–228.
Wyatt RJ, Henter ID, Jamison JC . Lithium revisited: savings brought about by the use of lithium, 1970–1991. Psychiatric Q 2001; 72: 149–166.
Geddes JR, Burgess S, Hawton K, Jamison K, Goodwin GM . Long-term lithium therapy for bipolar disorder: systematic review and meta-analysis of randomized controlled trials. Am J Psychiatry 2004; 161: 217–222.
Severus E, Taylor MJ, Sauer C, Pfennig A, Ritter P, Bauer M, et al. Lithium for prevention of mood episodes in bipolar disorders: systematic review and meta-analysis. Int J Bipolar Disord 2014; 2: 15 (in press).
Cipriani A, Hawton K, Stockton S, Geddes JR . Lithium in the prevention of suicide in mood disorders: updated systematic review and meta-analysis. BMJ 2013; 346: f3646.
Crossley NA, Bauer M . Acceleration and augmentation of antidepressants with lithium for depressive disorders: two meta-analyses of randomized, placebo-controlled trials. J Clin Psychiatry 2007; 68: 935–940.
Sheard MH, Marini JL, Bridges CI, Wagner E . The effect of lithium on impulsive aggressive behavior in man. Am J Psychiatry 1976; 133: 1409–1413.
Muller-Oerlinghausen B, Lewitzka U . Lithium reduces pathological aggression and suicidality: a mini-review. Neuropsychobiology 2010; 62: 43–49.
Ahrens B, Muller-Oerlinghausen B . Does lithium exert an independent antisuicidal effect? Pharmacopsychiatry 2001; 34: 132–136.
Grof P, Grof E . Varieties of lithium benefit. Prog Neuropsychopharmacol Biol Psychiatry 1990; 14: 689–696.
Yatham LN, Kennedy SH, Parikh SV, Schaffer A, Beaulieu S, Alda M, et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) collaborative update of CANMAT guidelines for the management of patients with bipolar disorder: update 2013. Bipolar Disord 2013 15: 1–44.
Judd LL, Akiskal HS, Schettler PJ, Endicott J, Maser J, Solomon DA, et al. The long-term natural history of the weekly symptomatic status of bipolar I disorder. Arch Gen Psychiatry 2002; 59: 530–537.
Bauer M, Ritter P, Grunze H, Pfennig A . Treatment options for acute depression in bipolar disorder. Bipolar Disord 2012; 14: 37–50.
Taylor DM, Cornelius V, Smith L, Young AH . Comparative efficacy and acceptability of drug treatments for bipolar depression: a multiple-treatments meta-analysis. Acta Psychiatr Scand 2014; 130: 452–469.
McKnight RF, Adida M, Budge K, Stockton S, Goodwin GM, Geddes JR . Lithium toxicity profile: a systematic review and meta-analysis. Lancet 2012; 379: 721–728.
Malhi GS, Tanious M, Das P, Coulston CM, Berk M . Potential mechanisms of action of lithium in bipolar disorder. Current understanding. CNS Drugs 2013; 27: 135–153.
Chiu CT, Chuang DM . Molecular actions and therapeutic potential of lithium in preclinical and clinical studies of CNS disorders. Pharmacol Ther 2010; 128: 281–304.
Gray JD, McEwen BS . Lithium's role in neural plasticity and its implications for mood disorders. Acta Psychiatr Scand 2013; 128: 347–361.
Lenox RH, Wang L . Molecular basis of lithium action: integration of lithium-responsive signaling and gene expression networks. Mol Psychiatry 2003; 8: 135–144.
Shorter E . The 25th anniversary of the launch of Prozac gives pause for thought: where did we go wrong? Br J Psychiatry 2014; 204: 331–332.
Baldessarini RJ, Tondo L . Does lithium treatment still work? Evidence of stable responses over three decades. Arch Gen Psychiatry 2000; 57: 187–190.
Grof P, Alda M . Discrepancies in the efficacy of lithium. Arch Gen Psychiatry 2000; 57: 191.
Kleindienst N, Greil W . Lithium in the long-term treatment of bipolar disorders. Eur Arch Psychiatr Clin Neurosci 2003; 253: 120–125.
Rybakowski JK, Chlopocka-Wozniak M, Suwalska A . The prophylactic effect of long-term lithium administration in bipolar patients entering treatment in the 1970s and 1980s. Bipolar Disord 2001; 3: 63–70.
Manchia M, Adli M, Akula N, Ardau R, Aubry JM, Backlund L, et al. Assessment of response to lithium maintenance treatment in bipolar disorder: a Consortium on Lithium Genetics (ConLiGen) report. PLoS One 2013; 8: e65636.
Kessing LV, Hansen HV, Hvenegaard A, Christensen EM, Dam H, Gluud C, et al. Treatment in a specialised out-patient mood disorder clinic v. standard out-patient treatment in the early course of bipolar disorder: randomised clinical trial. Br J Psychiatry 2013; 202: 212–219.
Kallner G, Lindelius R, Petterson U, Stockman O, Tham A . Mortality in 497 patients with affective disorders attending a lithium clinic or after having left it. Pharmacopsychiatry 2000; 33: 8–13.
Ahrens B, Muller-Oerlinghausen B, Grof P . Length of lithium treatment needed to eliminate the high mortality of affective disorders. Br J Psychiatry 1993; 163: 27–29.
Dixon JF, Hokin LE . Lithium acutely inhibits and chronically up-regulates and stabilizes glutamate uptake by presynaptic nerve endings in mouse cerebral cortex. Proc Natl Acad Sci USA 1998; 95: 8363–8368.
Manji HK, Lenox RH . Signaling: cellular insights into the pathophysiology of bipolar disorder. Biol Psychiatry 2000; 48: 518–530.
Scott J, Leboyer M, Hickie I, Berk M, Kapczinski F, Frank E, et al. Clinical staging in psychiatry: a cross-cutting model of diagnosis with heuristic and practical value. Br J Psychiatry 2013; 202: 243–245.
Hajek T, Cullis J, Novak T, Kopecek M, Blagdon R, Propper L, et al. Brain structural signature of familial predisposition for bipolar disorder: replicable evidence for involvement of the right inferior frontal gyrus. Biol Psychiatry 2013; 73: 144–152.
Coppen A . The biochemistry of affective disorders. Br J Psychiatry 1967; 113: 1237–1264.
El-Mallakh RS . Ion homeostasis and the mechanism of action of lithium. Clin Neurosci Res 2004; 4: 227–231.
Schou M . Biology and pharmacology of the lithium ion. Pharmacol Rev 1957; 9: 17–58.
Mendels J, Frazer A . Intracellular lithium concentration and clinical response: towards a membrane theory of depression. J Psychiatr Res 1973; 10: 9–18.
Dorus E, Pandey GN, Frazer A, Mendels J . Genetic determinant of lithium ion distribution. I. An in vitro monozygotic-dizygotic twin study. Arch Gen Psychiatry 1974; 31: 463–465.
Rihmer Z, Arato M, Szentistvanyi I, Banki CM . The red blood cell/plasma lithium ratio: marker of biological heterogeneity within bipolar affective illness? Psychiatr Res 1982; 6: 197–201.
Spirtes MA . Lithium levels in monkey and human brain after chronic, therapeutic, oral dosage. Pharmacol Biochem Behav 1976; 5: 143–147.
Ehrlich BE, Diamond JM . Lithium, membranes, and manic-depressive illness. J Membr Biol 1980; 52: 187–200.
Ehrlich BE, Diamond JM . Lithium fluxes in human erythrocytes. Am J Physiol 1979; 237: C102–C110.
Fernandez-Moncada I, Barros LF . Non-preferential fuelling of the Na+/K+-ATPase pump. Biochem J 2014; 460: 353–361.
Konradi C, Eaton M, MacDonald ML, Walsh J, Benes FM, Heckers S . Molecular evidence for mitochondrial dysfunction in bipolar disorder. Arch Gen Psychiatry 2004; 61: 300–308.
Naydenov AV, MacDonald ML, Ongur D, Konradi C . Differences in lymphocyte electron transport gene expression levels between subjects with bipolar disorder and normal controls in response to glucose deprivation stress. Arch Gen Psychiatry 2007; 64: 555–564.
Andreazza AC, Shao L, Wang JF, Young LT . Mitochondrial complex I activity and oxidative damage to mitochondrial proteins in the prefrontal cortex of patients with bipolar disorder. Arch Gen Psychiatry 2010; 67: 360–368.
Aperia A . New roles for an old enzyme: Na,K-ATPase emerges as an interesting drug target. J Intern Med 2007; 261: 44–52.
Zhang L, Zhang Z, Guo H, Wang Y . Na+/K+-ATPase-mediated signal transduction and Na+/K+-ATPase regulation. Fund Clin Pharmacol 2008; 22: 615–621.
Kirshenbaum GS, Clapcote SJ, Duffy S, Burgess CR, Petersen J, Jarowek KJ, et al. Mania-like behavior induced by genetic dysfunction of the neuron-specific Na+,K+-ATPase alpha3 sodium pump. Proc Natl Acad Sci USA 2011; 108: 18144–18149.
Antia IJ, Smith CE, Wood AJ, Aronson JK . The upregulation of Na+,K+-ATPase pump numbers in lymphocytes from the first-degree unaffected relatives of patients with manic depressive psychosis in response to in vitro lithium and sodium ethacrynate. J Affect Disord 1995; 34: 33–39.
Looney SW, El-Mallakh RS . Meta-analysis of erythrocyte Na,K-ATPase activity in bipolar illness. Depress Anxiety 1997; 5: 53–65.
Reddy PL, Khanna S, Subhash MN, Channabasavanna SM, Rao BS . Erythrocyte membrane sodium-potassium adenosine triphosphatase activity in affective disorders. J Neural Transm Gen Sect 1992; 89: 209–218.
Linnoila M, MacDonald E, Reinila M, Leroy A, Rubinow DR, Goodwin FK . RBC membrane adenosine triphosphatase activities in patients with major affective disorders. Arch Gen Psychiatry 1983; 40: 1021–1026.
Huang X, Lei Z, El-Mallakh RS . Lithium normalizes elevated intracellular sodium. Bipolar Disord 2007; 9: 298–300.
Banerjee U, Dasgupta A, Rout JK, Singh OP . Effects of lithium therapy on Na+-K+-ATPase activity and lipid peroxidation in bipolar disorder. Progr Neuropsychopharmacol Biol Psychiatry 2012; 37: 56–61.
Jope RS, Jenden DJ, Ehrlich BE, Diamond JM . Choline accumulates in erythrocytes during lithium therapy. N Engl J Med 1978; 299: 833–834.
Jope R . Effects of lithium treatment in vitro and in vivo on acetylcholine metabolism in rat brain. J Neurochem 1979; 33: 487–495.
Price LH, Heninger GR . Lithium in the treatment of mood disorders. N Engl J Med 1994; 331: 591–598.
Manji HK, Hsiao JK, Risby ED, Oliver J, Rudorfer MV, Potter WJ . The mechanisms of action of lithium: I: effects on serotoninergic and noradrenergic systems in normal subjects. Arch Gen Psychiatry 1991; 48: 505–512.
Beaulieu JM, Sotnikova TD, Yao WD, Kockeritz L, Woodgett JR, Gainetdinov RR et al. Lithium antagonizes dopamine-dependent behaviors mediated by an AKT/glycogen synthase kinase 3 signaling cascade. Proc Natl Acad Sci U S A 2004; 101: 5099–5104.
Nonaka S, Hough CJ, Chuang DM . Chronic lithium treatment robustly protects neurons in the central nervous system against excitotoxicity by inhibiting N-methyl-d-aspartate receptor-mediated calcium influx. Proc Natl Acad Sci USA 1998; 95: 2642–2647.
Young LT, Li PP, Kish SJ, Siu LP, Kamble A, Hornykiewcz O, et al. Cerebral cortex Gsa protein levels and forskolin-stimulated cyclic AMP formation are increased in bipolar affective disorder. J Neurochem 1993; 61: 890–898.
Jope RS . Anti-bipolar therapy: mechanism of action of lithium. Mol Psychiatry 1999; 4: 117–128.
Mork A, Geisler A . Effects of lithium ex vivo on the GTP-mediated inhibition of calcium-stimulated adenylate cyclase activity in rat brain. Eur J Pharmacol 1989; 168: 347–354.
Mork A, Geisler A . Effects of GTP on hormone-stimulated adenylate cyclase activity in cerebral cortex, striatum, and hippocampus from rats treated chronically with lithium. Biol Psychiatry 1989; 26: 279–288.
Mork A, Geisler A . Mode of action of lithium on the catalytic unit of adenylate cyclase from rat brain. Pharmacol Toxicol 1987; 60: 241–248.
Berridge MJ . Inositol trisphosphate and diacylglycerol as second messengers. Biochem J 1984; 220: 345–360.
Berridge MJ . The biology and medicine of calcium signalling. Mol Cell Endocrinol 1994; 98: 119–124.
Jope RS, Song L, Li PP, Young LT, Kish SJ, Pacheco MA, et al. The phosphoinositide signal transduction system is impaired in bipolar affective disorder brain. J Neurochem 1996; 66: 2402–2409.
van Calker D, Belmaker RH . The high affinity inositol transport system—implications for the pathophysiology and treatment of bipolar disorder. Bipolar Disord 2000; 2: 102–107.
Belmaker RH, Agam G, van CD, Richards MH, Kofman O . Behavioral reversal of lithium effects by four inositol isomers correlates perfectly with biochemical effects on the PI cycle: depletion by chronic lithium of brain inositol is specific to hypothalamus, and inositol levels may be abnormal in postmortem brain from bipolar patients. Neuropsychopharmacology 1998; 19: 220–232.
Lubrich B, van-Calker D . Inhibition of the high affinity myo-inositol transport system: a common mechanism of action of antibipolar drugs? Neuropsychopharmacology 1999; 21: 519–529.
Moore GJ, Bebchuk JM, Parrish JK, Faulk MW, Arfken CL, Strahl BJ, et al. Temporal dissociation between lithium-induced changes in frontal lobe myo-inositol and clinical response in manic-depressive illness. Am J Psychiatry 1999; 156: 1902–1908.
O'Brien WT, Klein PS . Validating GSK3 as an in vivo target of lithium action. Biochem Soc Trans 2009; 37: 1133–1138.
Schubert T, Stoll L, Muller WE . Therapeutic concentrations of lithium and carbamazepine inhibit cGMP accumulation in human lymphocytes. A clinical model for a possible common mechanism of action? Psychopharmacology (Berl) 1991; 104: 45–50.
Schubert T, Muller WE . Lithium but not cholinergic ligands influence guanylate cyclase activity in intact human lymphocytes. Biochem Pharmacol 1990; 39: 439–444.
Ghasemi M, Dehpour AR . The NMDA receptor/nitric oxide pathway: a target for the therapeutic and toxic effects of lithium. Trends Pharmacol Sci 2011; 32: 420–434.
Prast H, Philippu A . Nitric oxide as modulator of neuronal function. Prog Neurobiol 2001; 64: 51–68.
Harvey BH, Carstens ME, Taljaard JJ . Evidence that lithium induces a glutamatergic: nitric oxide-mediated response in rat brain. Neurochem Res 1994; 19: 469–474.
Boer U, Cierny I, Krause D, Heinrich A, Lin H, Mayr G, et al. Chronic lithium salt treatment reduces CRE/CREB-directed gene transcription and reverses its upregulation by chronic psychosocial stress in transgenic reporter gene mice. Neuropsychopharmacology 2008; 33: 2407–2415.
Warsh JJ, Andreopoulos S, Li PP . Role of intracellular calcium signaling in the pathophysiology and pharmacotherapy of bipolar disorder: current status. Clin Neurosci Res 2004; 4: 201–213.
Emamghoreishi M, Schlichter L, Li PP, Parikh S, Sen J, Kamble A, et al. High intracellular calcium concentrations in transformed lymphoblasts from subjects with bipolar I disorder. Am J Psychiatry 1997; 154: 976–982.
Perova T, Kwan M, Li PP, Warsh JJ . Differential modulation of intracellular Ca2+ responses in B lymphoblasts by mood stabilizers. Int J Neuropsychopharmacol 2010; 13: 693–702.
Jope RS . Lithium and GSK-3: one inhibitor, two inhibitory actions, multiple outcomes. Trends Pharmacol Sci 2003; 24: 441–443.
Meffre D, Grenier J, Bernard S, Courtin F, Dudev T, Shackleford G, et al. Wnt and lithium: a common destiny in the therapy of nervous system pathologies? Cell Mol Life Sci 2014; 71: 1123–1148.
Lang F, Strutz-Seebohm N, Seebohm G, Lang UE . Significance of SGK1 in the regulation of neuronal function. J Physiol 2010; 588: 3349–3354.
Anacker C, Cattaneo A, Musaelyan K, Zunszain PA, Horowitz M, Molteni R, et al. Role for the kinase SGK1 in stress, depression, and glucocorticoid effects on hippocampal neurogenesis. Proc Natl Acad Sci USA 2013; 110: 8708–8713.
Beaulieu JM, Caron MG . Looking at lithium: molecular moods and complex behaviour. Mol Interv 2008; 8: 230–241.
Grimes CA, Jope RS . CREB DNA binding activity is inhibited by glycogen synthase kinase-3 beta and facilitated by lithium. J Neurochem 2001; 78: 1219–1232.
Beaulieu JM . A role for Akt and glycogen synthase kinase-3 as integrators of dopamine and serotonin neurotransmission in mental health. J Psychiatry Neurosci 2012; 37: 7–16.
Mota de Freitas D, Castro MM, Geraldes CF . Is competition between Li and Mg2 the underlying theme in the proposed mechanisms for the pharmacological action of lithium salts in bipolar disorder? Acc Chem Res 2006; 39: 283–291.
Layden B, Diven C, Minadeo N, Bryant FB, Mota-de-Freitas D . Li+/Mg2+ competition at therapeutic intracellular Li+ levels in human neuroblastoma SH-SY5Y cells. Bipolar Disord 2000; 2: 200–204.
Dermitzakis ET . Cellular genomics for complex traits. Nat Rev Genet 2012; 13: 215–220.
Moore GJ, Bebchuk JM, Wilds IB, Chen G, Manji HK . Lithium-induced increase in human brain grey matter. Lancet 2000; 356: 1241–1242.
Hajek T, Cullis J, Novak T, Kopecek M, Hoschl C, Blagdon R, et al. Hippocampal volumes in bipolar disorders: opposing effects of illness burden and lithium treatment. Bipolar Disord 2012; 14: 261–270.
Moore GJ, Bebchuk JM, Hasanat K, Chen G, Seraji-Bozorgzad N, Wilds IB, et al. Lithium increases N-acetyl-aspartate in the human brain: in vivo evidence in support of bcl-2's neurotrophic effects? Biol Psychiatry 2000; 48: 1–8.
Hajek T, Bauer M, Pfennig A, Cullis J, Ploch J, O'Donovan C, et al. Large positive effect of lithium on prefrontal cortex N-acetylaspartate in patients with bipolar disorder: 2-centre study. J Psychiatr Neurosci 2012; 37: 185–192.
Chen RW, Chuang DM . Long term lithium treatment suppresses p53 and Bax expression but increases Bcl-2 expression. A prominent role in neuroprotection against excitotoxicity. J Biol Chem 1999; 274: 6039–6042.
Martinsson L, Wei Y, Xu D, Melas PA, Mathe AA, Schalling M, et al. Long-term lithium treatment in bipolar disorder is associated with longer leukocyte telomeres. Transl Psychiatry 2013; 3: e261.
Maurer IC, Schippel P, Volz HP . Lithium-induced enhancement of mitochondrial oxidative phosphorylation in human brain tissue. Bipolar Disord 2009; 11: 515–522.
Wood GE, Young LT, Reagan LP, Chen B, McEwen BS . Stress-induced structural remodeling in hippocampus: prevention by lithium treatment. Proc Natl Acad Sci USA 2004; 101: 3973–3978.
Deshauer D, Grof E, Alda M, Grof P . Patterns of DST positivity in remitted affective disorders. Biol Psychiatry 1999; 45: 1023–1029.
Bauer M, Alda M, Priller J, Young LT . Implications of the neuroprotective effects of lithium for the treatment of bipolar and neurodegenerative disorders. Pharmacopsychiatry 2003; 36: S250–S254.
Hajek T, Bauer M, Simhandl C, Rybakowski J, O'Donovan C, Pfennig A, et al. Neuroprotective effect of lithium on hippocampal volumes in bipolar disorder independent of long-term treatment response. Psychol Med 2014; 44: 507–517.
Frank E, Swartz HA, Kupfer DJ . Interpersonal and social rhythm therapy: managing the chaos of bipolar disorder. Biol Psychiatry 2000; 48: 593–604.
McCarthy MJ, Welsh DK . Cellular circadian clocks in mood disorders. J Biol Rhythm 2012; 27: 339–352.
Seggie J, Werstiuk E, Grota L, Brown GM . Chronic lithium treatment and twenty-four hour rhythm of serum prolactin, growth hormone and melatonin in rats. Prog Neuropsychopharmacol Biol Psychiatry 1983; 7: 827–830.
Kasahara T, Kubota M, Miyauchi T, Noda Y, Mouri A, Nabeshima T, et al. Mice with neuron-specific accumulation of mitochondrial DNA mutations show mood disorder-like phenotypes. Mol Psychiatry 2006; 11: 577–593.
Jope RS . A bimodal model of the mechanism of action of lithium. Mol Psychiatry 1999; 4: 21–25.
Muller-Oerlinghausen B, Berghofer A, Bauer M . Bipolar disorder. Lancet 2002; 359: 241–247.
Grof P, Duffy A, Cavazzoni P, Grof E, Garnham J, MacDougall M, et al. Is response to prophylactic lithium a familial trait? J Clin Psychiatry 2002; 63: 942–947.
Garnham J, Munro A, Slaney C, MacDougall M, Passmore M, Duffy A, et al. Prophylactic treatment response in bipolar disorder: results of a naturalistic observation study. J Affect Disord 2007; 104: 185–190.
Tondo L, Baldessarini RJ, Floris G . Long-term clinical effectiveness of lithium maintenance treatment in types I and II bipolar disorders. Br J Psychiatry 2001; 41 (Suppl.): s184–s190.
Licht RW, Vestergaard P, Brodersen A . Long-term outcome of patients with bipolar disorder commenced on lithium prophylaxis during hospitalization: a complete 15-year register-based follow-up. Bipolar Disord 2008; 10: 79–86.
Kulhara P, Basu D, Mattoo SK, Sharan P, Chopra R . Lithium prophylaxis of recurrent bipolar affective disorder: long-term outcome and its psychosocial correlates. J Affect Disord 1999; 54: 87–96.
Maj M, Pirozzi R, Magliano L, Bartoli L . Long-term outcome of lithium prophylaxis in bipolar disorder: a 5 year prospective study of 402 patients at a lithium clinic. Am J Psychiatry 1998; 155: 30–35.
Grof P, Alda M, Grof E, Fox D, Cameron P . The challenge of predicting response to stabilising lithium treatment. The importance of patient selection. Br J Psychiatry 1993; 163 (Suppl.): 16–19.
Calabrese JR, Fatemi SH, Kujawa M, Woyshville MJ . Predictors of response to mood stabilizers. J Clin Psychopharmacol 1996; 16: 24S–31S.
Maj M . Clinical prediction of response to lithium prophylaxis in bipolar patients: a critical update. Lithium 1992; 3: 15–21.
McCarthy MJ, Leckband SG, Kelsoe JR . Pharmacogenetics of lithium response in bipolar disorder. Pharmacogenomics 2010; 11: 1439–1465.
Kleindienst N, Engel R, Greil W . Which clinical factors predict response to prophylactic lithium? A systematic review for bipolar disorders. Bipolar Disord 2005; 7: 404–417.
Passmore M, Garnham J, Duffy A, MacDougall M, Munro A, Slaney C, et al. Phenotypic spectra of bipolar disorder in responders to lithium versus lamotrigine. Bipolar Disord 2003; 5: 110–114.
Alda M, Grof P, Grof E . MN blood groups and bipolar disorder: evidence of genotypic association and Hardy–Weinberg disequilibrium. Biol Psychiatry 1998; 44: 361–363.
Rohayem J, Bayle JF, Richa S . Predictors of prophylactic response to lithium. Encephale 2008; 34: 394–399.
Kleindienst N, Engel RR, Greil W . Psychosocial and demographic factors associated with response to prophylactic lithium: a systematic review for bipolar disorders. Psychol Med 2005; 35: 1685–1694.
Robins E, Guze SB . Establishment of diagnostic validity in psychiatric illness: its application to schizophrenia. Am J Psychiatry 1970; 126: 983–987.
Berghofer A, Alda M, Adli M, Baethge C, Bauer M, Bschor T, et al. Long-term effectiveness of lithium in bipolar disorder: a multicenter investigation of patients with typical and atypical features. J Clin Psychiatry 2008; 69: 1860–1868.
Grof P, Alda M, Grof E, Zvolsky P, Walsh M . Lithium response and genetics of affective disorders. J Affect Disord 1994; 32: 85–95.
Alda M, Grof P, Rouleau GA, Turecki G, Young LT . Investigating responders to lithium prophylaxis as a strategy for mapping susceptibility genes for bipolar disorder. Prog Neuropsychopharmacol Biol Psychiatry 2005; 29: 1038–1045.
McKnew DH, Cytryn L, Buchsbaum MS, Hamovit J, Lamour M, Rapoport JL, et al. Lithium in children of lithium-reponding parents. Psychiatr Res 1981; 4: 171–180.
Duffy A, Alda M, Milin R, Grof P . A consecutive series of treated affected offspring of parents with bipolar disorder: is response associated with the clinical profile? Can J Psychiatry 2007; 52: 369–376.
Kruger S, Alda M, Young LT, Goldapple K, Parikh S, Mayberg HS . Risk and resilience markers in bipolar disorder: brain responses to emotional challenge in bipolar patients and their healthy siblings. Am J Psychiatry 2006; 163: 257–264.
Severino G, Squassina A, Costa M, Pisanu C, Calza S, Alda M, et al. Pharmacogenomics of bipolar disorder. Pharmacogenomics 2013; 14: 655–674.
Geoffroy PA, Bellivier F, Leboyer M, Etain B . Can the response to mood stabilizers be predicted in bipolar disorder? Front Biosci (Elite Ed) 2014; 6: 120–138.
Manchia M, Squassina A, Congiu D, Chillotti C, Ardau R, Severino G, et al. Interacting genes in lithium prophylaxis: preliminary results of an exploratory analysis on the role of DGKH and NR1D1 gene polymorphisms in 199 Sardinian bipolar patients. Neurosci Lett 2009; 467: 67–71.
Campos-de-Sousa S, Guindalini C, Tondo L, Munro J, Osborne S, Floris G, et al. Nuclear receptor rev-erb-{alpha} circadian gene variants and lithium carbonate prophylaxis in bipolar affective disorder. J Biol Rhythm 2010; 25: 132–137.
McCarthy MJ, Nievergelt CM, Shekhtman T, Kripke DF, Welsh DK, Kelsoe JR . Functional genetic variation in the Rev-Erbalpha pathway and lithium response in the treatment of bipolar disorder. Genes Brain Behav 2011; 10: 852–861.
Benedetti F, Serretti A, Pontiggia A, Bernasconi A, Lorenzi C, Colombo C, et al. Long-term response to lithium salts in bipolar illness is influenced by the glycogen synthase kinase 3-beta -50T/C SNP. Neurosci Lett 2005; 376: 51–55.
Serretti A, Lilli R, Mandelli L, Lorenzi C, Smeraldi E . Serotonin transporter gene associated with lithium prophylaxis in mood disorders. Pharmacogenom J 2001; 1: 71–77.
Rybakowski JK, Suwalska A, Czerski PM, Dmitrzak-Weglarz M, Leszczynska-Rodziewicz A, Hauser J . Prophylactic effect of lithium in bipolar affective illness may be related to serotonin transporter genotype. Pharmacol Rep 2005; 57: 124–127.
Michelon L, Meira-Lima I, Cordeiro Q, Miguita K, Breen G, Collier D, et al. Association study of the INPP1, 5HTT, BDNF, AP-2beta and GSK-3beta GENE variants and restrospectively scored response to lithium prophylaxis in bipolar disorder. Neurosci Lett 2006; 403: 288–293.
Rybakowski JK, Suwalska A, Skibinska M, Szczepankiewicz A, Leszczynska-Rodziewicz A, Permoda A, et al. Prophylactic lithium response and polymorphism of the brain-derived neurotrophic factor gene. Pharmacopsychiatry 2005; 38: 166–170.
Mamdani F, Alda M, Grof P, Young LT, Rouleau G, Turecki G . Lithium response and genetic variation in the CREB family of genes. Am J Med Genet B 2008; 147B: 500–504.
Li M, Luo XJ, Rietschel M, Lewis CM, Mattheisen M, Muller-Myhsok B, et al. Allelic differences between Europeans and Chinese for CREB1 SNPs and their implications in gene expression regulation, hippocampal structure and function, and bipolar disorder susceptibility. Mol Psychiatry 2014; 19: 452–461.
Kakiuchi C, Kato T . Lithium response and −116C/G polymorphism of XBP1 in Japanese patients with bipolar disorder. Int J Neuropsychopharmacol 2005; 8: 631–632.
Masui T, Hashimoto R, Kusumi I, Suzuki K, Tanaka T, Nakagawa S, et al. A possible association between the −116C/G single nucleotide polymorphism of the XBP1 gene and lithium prophylaxis in bipolar disorder. Int J Neuropsychopharmacol 2006; 9: 83–88.
Ewald H, Wang AG, Vang M, Mors O, Nyegaard M, Kruse TA . A haplotype-based study of lithium responding patients with bipolar affective disorder on the Faroe Islands. Psychiatr Genet 1999; 9: 23–34.
Morissette J, Villeneuve A, Bordeleau L, Rochette D, Laberge C, Gagne B, et al. Genome-wide search for linkage of bipolar affective disorders in a very large pedigree derived from a homogeneous population in Quebec points to a locus of major effect on chromosome 12q23-q24. Am J Med Genet B 1999; 88: 567–587.
Lopez de Lara C, Jaitovich-Groisman I, Cruceanu C, Mamdani F, Lebel V, Yerko V, et al. Implication of synapse-related genes in bipolar disorder by linkage and gene expression analyses. Int J Neuropsychopharmacol 2010; 13: 1397–1410.
Chen CH, Lee CS, Lee MT, Ouyang WC, Chen CC, Chong MY, et al. Variant GADL1 and response to lithium therapy in bipolar I disorder. N Engl J Med 2014; 370: 119–128.
Ikeda M, Kondo K, Iwata N . Variant GADL1 and response to lithium in bipolar I disorder. N Engl J Med 2014; 370: 1856–1857.
Consortium on Lithium Genetics, Hou L, Heilbronner U, Rietschel M, Kato T, Kuo PH, et al. Variant GADL1 and response to lithium in bipolar I disorder. N Engl J Med 2014; 370: 1857–1859.
Ferreira MA, O'Donovan MC, Meng YA, Jones IR, Ruderfer DM, Jones L, et al. Collaborative genome-wide association analysis supports a role for ANK3 and CACNA1C in bipolar disorder. Nat Genet 2008; 40: 1056–1058.
Muhleisen TW, Leber M, Schulze TG, Strohmaier J, Degenhardt F, Treutlein J, et al. Genome-wide association study reveals two new risk loci for bipolar disorder. Nat Commun 2014; 5: 3339.
Nanavati D, Austin DR, Catapano LA, Luckenbaugh DA, Dosemeci A, Manji HK, et al. The effects of chronic treatment with mood stabilizers on the rat hippocampal post-synaptic density proteome. J Neurochem 2011; 119: 617–629.
McQuillin A, Rizig M, Gurling HMD . A microarray gene expression study of the molecular pharmacology of lithium carbonate on mouse brain mRNA to understand the neurobiology of mood stabilization and treatment of bipolar affective disorder. Pharmacogenet Genom 2007; 17: 605–617.
Leussis MP, Berry-Scott EM, Saito M, Jhuang H, de HG, Alkan O, et al. The ANK3 bipolar disorder gene regulates psychiatric-related behaviors that are modulated by lithium and stress. Biol Psychiatry 2013; 73: 683–690.
Toker L, Belmaker RH, Agam G . Gene-expression studies in understanding the mechanism of action of lithium. Expert Rev Neurother 2012; 12: 93–97.
Farah R, Khamisy-Farah R, Amit T, Youdim MB, Arraf Z . Lithium's gene expression profile, relevance to neuroprotection A cDNA microarray study. Cell Mol Neurobiol 2013; 33: 411–420.
Li PP . Transcriptional mechanisms of lithium action: therapeutic implications. Clin Neurosci Res 2004; 4: 271–280.
Einat H . New ways of modeling bipolar disorder. Harv Rev Psychiatry 2014; 22: 348–352.
Perlis RH, Smoller JW, Ferreira MA, McQuillin A, Bass N, Lawrence J, et al. A genomewide association study of response to lithium for prevention of recurrence in bipolar disorder. Am J Psychiatry 2009; 166: 718–725.
Squassina A, Manchia M, Borg J, Congiu D, Costa M, Georgitsi M, et al. Evidence for association of an ACCN1 gene variant with response to lithium treatment in Sardinian patients with bipolar disorder. Pharmacogenomics 2011; 12: 1559–1569.
Schulze T . Genomic and phenomic correlates of lithium response in bipolar disorder: a consortium on lithium genetics (ConLiGen) report. Bipolar Disord 2014; 16: 26 (abstract).
Bergen S, Song J, Lichtenstein P, Landen M . Genome-wide association study of lithium response in a Swedish population. Bipolar Disord 2014; 16: 64 (abstract).
Acknowledgements
I wish to thank Dr Claire O'Donovan, Dr Alessio Squassina, Nathan Corbett as well as anonymous reviewers for helpful comments on the earlier version of the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no conflict of interest.
Rights and permissions
About this article
Cite this article
Alda, M. Lithium in the treatment of bipolar disorder: pharmacology and pharmacogenetics. Mol Psychiatry 20, 661–670 (2015). https://doi.org/10.1038/mp.2015.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2015.4
This article is cited by
-
Does treatment with autophagy-enhancers and/or ROS-scavengers alleviate behavioral and neurochemical consequences of low-dose rotenone-induced mild mitochondrial dysfunction in mice?
Molecular Psychiatry (2023)
-
Effect of lithium administration on brain activity under an emotion regulation paradigm in healthy participants: a functional magnetic resonance imaging study
Psychopharmacology (2023)
-
Transcriptomics and miRNomics data integration in lymphoblastoid cells highlights the key role of immune-related functions in lithium treatment response in Bipolar disorder
BMC Psychiatry (2022)
-
The Purinergic System as a Target for the Development of Treatments for Bipolar Disorder
CNS Drugs (2022)
-
Regulation of sensorimotor gating via Disc1/Huntingtin-mediated Bdnf transport in the cortico-striatal circuit
Molecular Psychiatry (2022)