Abstract
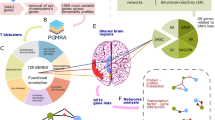
The role of non-diagnostic features in the pathophysiology of autism spectrum disorders (ASDs) is unclear. Increasing evidence suggests immune system alterations in ASD may be implicated in the severity of behavioral impairment and other developmental outcomes. The primary objective of this meta-analysis was to investigate if there is a characteristic abnormal cytokine profile in ASD compared with healthy controls (HCs). We identified relevant studies following a search of MEDLINE, EMBASE, PsycINFO, Web of Knowledge and Scopus. A meta-analysis was performed on studies comparing plasma and serum concentrations of cytokines in unmedicated participants with ASD and HCs. Results were reported according to PRISMA statement. Seventeen studies with a total sample size of 743 participants with ASD and 592 HC were included in the analysis. Nineteen cytokines were assessed. Concentrations of interleukin (IL)-1beta (P<0.001), IL-6 (P=0.03), IL-8 (P=0.04), interferon-gamma (P=0.02), eotaxin (P=0.01) and monocyte chemotactic protein-1 (P<0.05) were significantly higher in the participants with ASD compared with the HC group, while concentrations of transforming growth factor-β1 were significantly lower (P<0.001). There were no significant differences between ASD participants and controls for the other 12 cytokines analyzed. The findings of our meta-analysis identified significantly altered concentrations of cytokines in ASD compared to HCs, strengthening evidence of an abnormal cytokine profile in ASD where inflammatory signals dominate.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Goldman SE, Surdyka K, Cuevas R, Adkins K, Wang L, Malow BA . Defining the sleep phenotype in children with autism. Dev Neuropsychol 2009; 34: 560–573.
Careaga M, Ashwood P . Autism spectrum disorders: from immunity to behavior. Methods Mol Biol 2012; 934: 219–240.
Valicenti-Mcdermott M, McVICAR K, Rapin I, Wershil BK, Cohen H, Shinnar S . Frequency of gastrointestinal symptoms in children with autistic spectrum disorders and association with family history of autoimmune disease. J Dev Behav Pediatr 2006; 27: S128–S136.
Rossignol DA, Frye RE . Mitochondrial dysfunction in autism spectrum disorders: a systematic review and meta-analysis. Mol Psychiatry 2011; 17: 290–314.
Ashwood P, Wills S, Van de Water J . The immune response in autism: a new frontier for autism research. J Leukoc Biol 2006; 80: 1–15.
Goines PE, Ashwood P . Cytokine dysregulation in autism spectrum disorders (ASD): possible role of the environment. Neurotoxicol Teratol 2012; 36: 67–81.
Crespi BJ, Thiselton DL . Comparative immunogenetics of autism and schizophrenia. Genes Brain Behav 2011; 10: 689–701.
Garay PA, Hsiao EY, Patterson PH, Kimberley McAllister A . Maternal immune activation causes age-and region-specific changes in brain cytokines in offspring throughout development. Brain Behavior Immunity 2012; 31: 54–68.
Smith SEP, Li J, Garbett K, Mirnics K, Patterson PH . Maternal immune activation alters fetal brain development through interleukin-6. J Neurosci 2007; 27: 10695–10702.
Atladóttir HÓ, Pedersen MG, Thorsen P, Mortensen PB, Deleuran B, Eaton WW et al. Association of family history of autoimmune diseases and autism spectrum disorders. Pediatrics 2009; 124: 687–694.
Vargas DL, Nascimbene C, Krishnan C, Zimmerman AW, Pardo CA . Neuroglial activation and neuroinflammation in the brain of patients with autism. Ann Neurol 2005; 57: 67–81.
Wei H, Zou H, Sheikh AM, Malik M, Dobkin C, Brown WT et al. IL-6 is increased in the cerebellum of autistic brain and alters neural cell adhesion, migration and synaptic formation. J Neuroinflam 2011; 8: 52.
Croonenberghs J, Bosmans E, Deboutte D, Kenis G, Maes M . Activation of the inflammatory response system in autism. Neuropsychobiology 2002; 45: 1–6.
Ricci S, Businaro R, Ippoliti F, Vasco Lo VR, Massoni F, Onofri E et al. Altered cytokine and BDNF levels in autism spectrum disorder. Neurotox Res 2013; 24: 491–501.
Suzuki K, Matsuzaki H, Iwata K, Kameno Y, Shimmura C, Kawai S et al. Plasma cytokine profiles in subjects with high-functioning autism spectrum disorders. PLoS ONE 2011; 6: e20470.
Ashwood P, Krakowiak P, Hertz-Picciotto I, Hansen R, Pessah IN, Van de Water J . Associations of impaired behaviors with elevated plasma chemokines in autism spectrum disorders. J Neuroimmunol 2011a; 232: 196–199.
Hashim H, Abdelrahman H, Mohammed D, Karam R . Association between plasma levels of transforming growth factor-b1, IL-23 and IL-17 and the severity of autism in Egyptian children. Res Autism Spect Dis 2013; 7: 199–204.
Banks WA . Blood-brain barrier transport of cytokines: a mechanism for neuropathology. Curr Pharm Design 2005; 11: 973–984.
Fung A, Vizcaychipi M, Lloyd D, Wan Y, Ma D . Central nervous system inflammation in disease related conditions: mechanistic prospects. Brain Res 2012; 1446: 144–155.
Erickson MA, Dohi K, Banks WA . Neuroinflammation: a common pathway in CNS diseases as mMediated at the blood-brain barrier. Neuroimmunomodulation 2012; 19: 121–130.
Chez MG, Dowling T, Patel PB, Khanna P, Kominsky M . Elevation of tumor necrosis factor-alpha in cerebrospinal fluid of autistic children. Pediatr Neurol 2007; 36: 361–365.
Okada K, Hashimoto K, Iwata Y, Nakamura K, Tsujii M, Tsuchiya KJ et al. Decreased serum levels of transforming growth factor-(beta)1 in patients with autism. Prog Neuro-Psychopharmacol Biol Psychiatry 2007; 31: 187–190.
Molloy CA, Morrow AL, Meinzen-Derr J, Schleifer K, Dienger K, Manning-Courtney P et al. Elevated cytokine levels in children with autism spectrum disorder. J Neuroimmunol 2006; 172: 198–205.
Enstrom A, Onore C, Hertz-Picciotto I, Hansen R, Croen L, Van de Water J et al. Detection of IL-17 and IL-23 in plasma samples of children with autism. Am J Biochem Biotechnol 2008; 4: 114–120.
Singh VK . Plasma increase of interleukin- 12 and interferon-gamma pathological significance in autism. J Neuroimmunol 1996; 66: 143–145.
Ashwood P, Enstrom A, Krakowiak P, Hertz-Picciotto I, Hansen R, Croen LA et al. Decreased transforming growth factor beta1 in autism: a potential link between immune dysregulation and impairment in clinical behavioral outcomes. J Neuroimmunol 2008; 204: 149–153.
Al-Ayadhi LY, Mostafa GA . Elevated serum levels of interleukin-17 A in children with autism. J Neuroinflamm 2012; 9: 158.
Jyonouchi H, Geng L, Ruby A, Reddy C, Zimmerman-Bier B . Evaluation of an association between gastrointestinal symptoms and cytokine production against common dietary proteins in children with autism spectrum disorders. J Pediatr 2005; 146: 605–610.
Ashwood P, Krakowiak P, Hertz-Picciotto I, Hansen R, Pessah IN, Van de Water J . Altered T cell responses in children with autism. Brain Behav Immun 2011; 25: 840–849.
Malik M, Sheikh AM, Wen G, Spivack W, Brown WT, Li X . Expression of inflammatory cytokines, Bc12 and cathepsin D are altered in lymphoblasts of autistic subjects. Immunobiology 2010; 216: 80–85.
Saresella M, Marventano I, Guerini FR, Mancuso R, Ceresa L, Zanzottera M et al. An autistic endophenotype results in complex immune dysfunction in healthy siblings of autistic children. Biol Psychiatry 2009; 66: 978–984.
Vojdani A, Mumper E, Granpeesheh D, Mielke L, Traver D, Bock K et al. Low natural killer cell cytotoxic activity in autism: the role of glutathione, IL-2 and IL-15. J Neuroimmunol 2008; 205: 148–154.
Abdallah MW, Larsen N, Mortensen EL, Atladottir HO, Norgaard-Pedersen B, Bonefeld-Jorgensen EC et al. Neonatal levels of cytokines and risk of autism spectrum disorders: An exploratory register-based historic birth cohort study utilizing the Danish Newborn Screening Biobank. J Neuroimmunol 2012; 252: 75–82.
Deverman BE, Patterson PH . Cytokines and CNS development. Neuron 2009; 64: 61–78.
Hsiao EY, McBride SW, Chow J, Mazmanian SK, Patterson PH . Modeling an autism risk factor in mice leads to permanent immune dysregulation. Proc Natl Acad Sci 2012; 109: 12776–12781.
Miller BJ, Buckley P, Seabolt W, Mellor A, Kirkpatrick B . Meta-analysis of cytokine alterations in schizophrenia: clinical status and antipsychotic effects. Bioi Psychiatry 2011; 70: 663–671.
Potvin S, Stip E, Sepehry AA, Gendron A, Bah R, Kouassi E . Inflammatorycytokine alterations in schizophrenia: a systematic quantitative review. Biol Psychiatry 2008; 63: 801–808.
Modabbernia A, Taslimi S, Brietzke E, Ashrafi M . Cytokine alterations in bipolar disorder: a meta-analysis of 30 studies. Biol Psychiatry 2013; 74: 15–25.
Dowlati Y, Herrmann N, Swardfager W, Liu H, Sham L, Reim EK et al. A meta-analysis of cytokines in major depression. Biol Psychiatry 2010; 67: 446–457.
Onore C, Enstrom A, Krakowiak P, Hertz-Picciotto I, Hansen R, Van de Water J et al. Decreased cellular IL-23 but not IL-17 production in children with autism spectrum disorders. J Neuroimmunol 2009; 216: 126–129.
Napolioni V, Ober-Reynolds B, Szelinger S, Corneveaux JJ, Pawlowski T, Ober-Reynolds S et al. Plasma cytokine profiling in sibling pairs discordant for autism spectrum disorder. J Neuroinflam 2013; 10: 38.
Tostes MHFS, Teixeira HC, Gattaz WF, Brandao MAF, Raposo NRB . Altered neurotrophin, neuropeptide, cytokines and nitric oxide levels in autism. Pharmacopsychiatry 2012; 45: 241–243.
Moher D, Liberati A, Tetzlaff J, Altman DG . Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 2009; 151: 264–269.
Borenstein M, Hedges L, Higgins J, Rothstein H . Comprehensive meta-analysis version 2. Biostat: Englewood, NJ, 2005.
Cohen J . Statistical Power Analysis for the Behavioral Sciences. Lawrence Erlbaum Associates: Hillsdale, NJ, 1988.
Hedges L, Olkin I . Statistical Methods for Meta-Analysis. Academic Press: Orlando, 1985.
Egger M, Smith GD, Schneider M, Minder C . Bias in meta-analysis detected by a simple, graphical test. Br Med J 1997; 315: 629–634.
Higgins JPT, Thompson SG . Quantifying heterogeneity in a meta-analysis. Statist Med 2002; 21: 1539–1558.
Higgins JPT, Thompson SG, Deeks JJ, Altman DG . Measuring inconsistency in meta-analyses. Br Med J 2003; 327: 557–560.
Al-Ayadhi LY . Pro-inflammatory cytokines in autistic children in central Saudi Arabia. Neurosciences 2005; 10: 155–158.
Wakkad ASEDE, Saleh MT . The proinflammatory cytokines in children with autism. Pak J Biol Sci 2006; 9: 2593–2599.
Ashwood P, Krakowiak P, Hertz-Picciotto I, Hansen R, PESSAH I, Van de Water J . Elevated plasma cytokines in autism spectrum disorders provide evidence of immune dysfunction and are associated with impaired behavioral outcome. Brain Behav Immun 2011b; 25: 40–45.
Manzardo AM, Henkhaus R, Dhillon S, Butler MG . Plasma cytokine levels in children with autistic disorder and unrelated siblings. Int J Dev Neurosci 2012; 30: 121–127.
Sweeten TL, Posey DJ, Shankar S, McDougle CJ . High nitric oxide production in autistic disorder: a possible role for interferon-γ. Biol Psychiatry 2004; 55: 434–437.
El-Ansary A, Al-Ayadhi L . Neuroinflammation in autism spectrum disorders. J Neuroinflam 2012; 9: 1–9.
Schroder K, Hertzog PJ, Ravasi T, Hume DA . Interferon-γ: an overview of signals, mechanisms and functions. J Leukoc Biol 2004; 75: 163–189.
Berger A . Science commentary: Th1 and Th2 responses: what are they? Br Med J 2000; 321: 424–424.
Gomes FCA, Sousa V de O, Romão L . Emerging roles for TGF-β1 in nervous system development. Int J Dev Neurosci 2005; 23: 413–424.
Maes M, Bosmans E, Meltzer HY, Scharpé S, Suy E . Interleukin-1 beta: a putative mediator of HPA axis hyperactivity in major depression? Am J Psychiatry 1993; 150: 1189–1193.
Nishimoto N, Kishimoto T . Interleukin 6: from bench to bedside. Nat Clin Pract Rheumatol 2006; 2: 619–626.
Papanicolaou DA . The Pathophysiologic roles of interleukin-6 in human disease. Ann Intern Med 1998; 128: 127.
Rohleder N, Aringer M, Boentert M . Role of interleukin‐6 in stress, sleep, and fatigue. Ann New York Acad Sci 2012; 1261: 88–96.
Vgontzas AN, Papanicolaou DA, Bixler EO, Lotsikas A, Zachman K, Kales A et al. Circadian interleukin-6 secretion and quantity and depth of sleep. J Clin Endo 84: 203–2607.
Skogstrand K, Thorsen P, Norgaard-Pedersen B, Schendel DE, Sorensen LC, Hougaard DM . Simultaneous measurement of 25 inflammatory markers and neurotrophins in neonatal dried blood spots by immunoassay with xMAP technology. Clin Chem 2005; 51: 1854–1866.
Skogstrand K, Ekelund CK, Thorsen P, Vogel I, Jacobsson B, Nørgaard-Pedersen B et al. Effects of blood sample handling procedures on measurable inflammatory markers in plasma, serum and dried blood spot samples. J Immunol Methods 2008; 336: 78–84.
Keustermans GCE, Hoeks SBE, Meerding JM, Prakken BJ, de Jager W . Cytokine assays: An assessment of the preparation and treatment of blood and tissue samples. Methods 2013; 61: 10–17.
de Jager W, Prakken BJ, Bijlsma JWJ, Kuis W, Rijkers GT . Improved multiplex immunoassay performance in human plasma and synovial fluid following removal of interfering heterophilic antibodies. J Immunol Methods 2005; 300: 124–135.
Breen EC, Reynolds SM, Cox C, Jacobson LP, Magpantay L, Mulder CB et al. Multisite comparison of high-sensitvity multiplex cytokine assays. Clin vaccine immunol 2011; 18: 1229–1242.
McFaul SJ, Bowman PD, Villa VM . Hemoglobin stimulates the release of proinflammatory cytokines from leukocytes in whole blood. J Lab Clin Med 2000; 135: 263–269.
Niwa Y, Akamatsu H, Sumi H, Ozaki Y, Abe A . Evidence for degradation of cytokines in the serum of patients with atopic dermatitis by calcium-dependent protease. Arch Dermatol Res 2000; 292: 391–396.
de Jager W, Bourcier K, Rijkers GT, Prakken BJ, Seyfert-Margolis V . Prerequisites for cytokine measurements in clinical trials with multiplex immunoassays. BMC immunol 2009; 10: 52.
Frey DJ, Fleshner M, Wright KP . The effects of 40 h of total sleep deprivation on inflammatory markers in healthy young adults. Brain Behav Immun 2007; 21: 1050–1057.
O’Connor M-F, Bower JE, Cho HJ, Creswell JD, Dimitrov S, Hamby ME et al. To assess, to control, to exclude: effects of biobehavioral factors on circulating inflammatory markers. Brain Behav Immun 2009; 23: 887–897.
Casimir GJA, Mulier S, Hanssens L, Zylberberg K, Duchateau J . Gender differences in inflammatory markers in children. Shock 2010; 33: 258–262.
Goines P, Van de Water J . The immune system's role in the biology of autism. Curr Opin Neurol 2010; 23: 111–117.
Asadabadi M, Mohammadi MR, Ghanizadeh A, Modabbernia A, Ashrafi M, Hassanzadeh E et al. Celecoxib as adjunctive treatment to risperidone in children with autistic disorder: a randomized, double-blind, placebo-controlled trial. Psychopharmacology 2013; 225: 51–59.
Acknowledgements
We thank Melanie Reuss for assisting with the independent screening of titles, abstracts and full-text articles and subsequent assessment of eligibility. We acknowledge the support of National Health and Medical Research Council project grant (1043664) and Career Development Fellowship (1061922) to Associate Professor Guastella and an Australia Fellowship (494914) to Professor Hickie.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Ian B Hickie is a member of the Medical Advisory Panel for BUPA Health Insurance (Australia) and also a Board Member of Psychosis Australia Trust. From 2012, he is a Commissioner in Australia’s new National Mental Health Commission. He was until January 2012 a director of headspace: the national youth mental health foundation. Professor Hickie was previously the chief executive officer (till 2003) and clinical adviser (till 2006) of beyondblue, an Australian National Depression Initiative. He is supported principally for clinical research in depression and health services and population health initiatives related to anxiety and depression by an NHMRC Australian Medical Research Fellowship (2007–2012). He has led projects for health professionals and the community supported by governmental, community agency and pharmaceutical industry partners (Wyeth, Eli Lily, Servier, Pfizer, AstraZeneca) for the identification and management of depression and anxiety. He has received honoraria for presentations of his own work at educational seminars supported by a number of non-government organizations and the pharmaceutical industry (including Pfizer, Servier and AstraZeneca). He has served on advisory boards convened by the pharmaceutical industry in relation to specific antidepressants, including nefazodone, duloxetine and desvenlafaxine. He leads a new investigator-initiated study of the effects of agomelatine on circadian parameters (supported in part by Servier but also by other NHMRC funding) and has participated in a multicentre clinical trial of the effects of agomelatine on sleep architecture in depression and a Servier-supported study of major depression and sleep disturbance in primary care settings. In addition to national and international government-based grant bodies, investigator-initiated mental health research at the BMRI, he has been supported by various pharmaceutical manufacturers (including Servier and Pfizer) and not-for-profit entities (including the Heart Foundation, beyondblue and the BUPA Foundation).
Additional information
Supplementary Information accompanies the paper on the Molecular Psychiatry website
Supplementary information
PowerPoint slides
Rights and permissions
About this article
Cite this article
Masi, A., Quintana, D., Glozier, N. et al. Cytokine aberrations in autism spectrum disorder: a systematic review and meta-analysis. Mol Psychiatry 20, 440–446 (2015). https://doi.org/10.1038/mp.2014.59
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2014.59
This article is cited by
-
Assessment of a multisite standardized biospecimen collection protocol for immune phenotyping in neurodevelopmental disorders
Scientific Reports (2023)
-
Extracellular free water elevations are associated with brain volume and maternal cytokine response in a longitudinal nonhuman primate maternal immune activation model
Molecular Psychiatry (2023)
-
Natur und Immunmechanismen psychischer Erkrankungen
Der Nervenarzt (2023)
-
(R)-ketamine attenuates neurodevelopmental disease-related phenotypes in a mouse model of maternal immune activation
European Archives of Psychiatry and Clinical Neuroscience (2023)
-
Carbon monoxide (CO) correlates with symptom severity, autoimmunity, and responses to probiotics treatment in a cohort of children with autism spectrum disorder (ASD): a post-hoc analysis of a randomized controlled trial
BMC Psychiatry (2022)