Abstract
Reactive oxygen species (ROS) produced by the phagocyte NADPH oxidase (NOX2) are required for microbial clearance; however, when produced in excess they exacerbate inflammatory response and injure surrounding tissues. NOX2 is a multicomponent enzyme composed of membrane-associated cytochrome b588 and cytosolic components p47phox, p67phox, p40phox, and rac1/2. We investigated whether vasoactive intestinal peptide (VIP), an endogenous immune-modulatory peptide, could affect ROS production by NOX2 in primary human phagocytes. VIP did not modulate basal ROS production by phagocytes, but it inhibited monocyte and not neutrophil ROS production in response to the bacterial peptide N-formyl-methionyl-leucyl-phenylalanine (fMLF). The action of VIP was essentially mediated by high-affinity G-protein coupled receptors VPAC1 as its specific agonist, [ALA11,22,28]VIP, mimicked VIP-inhibitory effect, whereas the specific VPAC1 antagonist, PG97-269, blunted VIP action. Further, we showed that VIP inhibited fMLF-induced phosphorylation of ERK1/2 (extracellular signal–regulated kinase 1/2), p38MAPK (p38 mitogen-activated protein kinase) pathways, and phosphorylation of p47phox on Ser345 residue. Also, VIP exerted an anti-inflammatory effect in a model of carrageenan-induced inflammation in rats. We thus found that VIP exerts anti-inflammatory effects by inhibiting the “MAPK–p47phox phosphorylation–NOX2 activation” axis. These data suggest that VIP acts as a natural anti-inflammatory agent of the mucosal system and its analogs could be novel anti-inflammatory molecules.
Similar content being viewed by others
Introduction
Vasoactive intestinal peptide (VIP), a 28 amino-acid peptide, is part of the secretin/glucagon family that includes several peptides such as pituitary adenylate cyclase–activating polypeptide (PACAP).1 VIP is widely distributed in nervous, endocrine, and immune systems, and it has been shown to modulate innate as well as adaptative immunity.2 VIP, in innate immunity, inhibits the production of pro-inflammatory cytokines and chemokines from activated macrophage and stimulates the production of anti-inflammatory cytokine interleukin (IL)-10. In tailoring adaptive immunity, VIP enhances T helper type 2 (Th2) responses, reduces the pro-inflammatory Th1 responses, and promote T regulatory functions.3 Further, VIP can also have a role in homing and distribution of unstimulated T lymphocytes.4 The physiological action of VIP is essentially mediated by high-affinity G-protein coupled receptors VPAC1 and VPAC2. The structurally related peptide, PACAP, which also modulate inflammation, exerts its action through PAC1 as well as VPAC receptors.5 VIP has been shown to decrease the severity of trinitobenzene sulfonic acid or trinitobenzene sulfonic acid–induced colitis in mice that represents a hapten-induced model of colonic inflammation with increased Th1 and Th17 cytokines, further extending VIP immunomodulatory action.6 VIP can act on the pathophysiological process, which precedes the local respiratory burst by phagocytes (neutrophils and monocytes) such as edema,7 the chemotaxis of phagocytes,8 and opsonized zymosan-induced activation.9 Excessive phagocyte activation results in excessive reactive oxygen species (ROS) release, which can damage host tissue and exacerbate inflammation underscoring the need for a tight regulation by different mediators such as pro- or anti-inflammatory cytokines and endogenous peptides, such as VIP.
In phagocytes, ROS are generated by the multicomponent enzyme NADPH oxidase (NOX2), which is composed of membrane-associated cytochrome b588 and cytosolic components p47phox, p67phox, p40phox, and rac1/2.9 The phosphorylation of cytosolic p47phox is important for the assembly and activation of NADPH oxidase, which can be modulated by a variety of mediators, including pro- and anti-inflammatory cytokines.10 ROS production induced by the bacterial peptide N-formyl-methionyl-leucyl-phenylalanine (fMLF) in neutrophils or monocytes involves activation of extracellular signal–regulated kinase (ERK), p38 mitogen-activated protein kinase (p38MAPK) pathways, and phosphorylation of several serine residues of p47phox. Among the different serine residues, the phosphorylation of Ser 345 residue of p47phox is inhibited by either IL-10 or adiponectin, resulting in a diminished ROS production by phagocytes in response to fMLF.11, 12 Regulation of Ser345 phosphorylation status is crucial in inhibiting or even potentiating subsequent fMLF effect on phagocyte ROS production and this pathway could have a role in VIP anti-inflammatory effects.
The mucosal lining of the lungs and colon are exposed to a large amount of exogenous and endogenous bacteria, which produce and release enormous amounts of inflammatory mediators, such as lipopolysaccharide (LPS) and formylated peptides, such as fMLF. Despite the presence of these pro-inflammatory agents and inflammatory immune cells in the mucosa, inflammation stays under control in the majority of individuals. We thus hypothesized that peptides present in the mucosa might have inhibitory effects on phagocyte ROS production. In this study, we found that VIP was a strong inhibitor of fMLF-induced ROS production in human whole blood by altering the “MAPK–p47phox phosphorylation–NOX2 activation” axis. This inhibition was more effective in primary human monocytes vs. neutrophils and VIP has an anti-inflammatory effect in carrageenan-induced inflammation in rats. These data, altogether, highlight the novel anti-inflammatory mechanism driven by VIP, which may be beneficial in mucosal immunity.
Results
VIP inhibits fMLF-induced ROS production by human monocytes
VIP has a therapeutic effect on chronic inflammatory diseases such as rheumatoid arthritis,13 which is associated with a high amount of ROS in the patient synovial fluid.11, 14 In this context, we investigated the effect of VIP on an important human phagocyte innate function, the production of ROS. The kinetic of ROS production in human whole blood in response to the bacterial peptide fMLF alone or in the presence of VIP and its related peptides was measured by a chemiluminescence method (Figure 1a). The rapid ROS production induced by fMLF was inhibited by VIP and the histogram of the corresponding area under the curve from several experiments is indicated in (Figure 1b). Among the closely related peptide, PACAP-38 inhibited fMLF-induced ROS production while secretin was inactive, suggesting a specificity of VIP/PACAP action. We then explored whether the observed VIPinhibitory action was due to either or both major circulating phagocytes (monocytes or neutrophils) known to produce ROS in response to fMLF. Results show that VIP dose dependently inhibited fMLF-induced ROS production by isolated human monocytes (1–100 nM) (Figure 1c,d) while being ineffective on neutrophil response even at 100 nM (Figure 1e,f).
Effect of vasoactive intestinal peptide (VIP) and related peptides on N-formyl-methionyl-leucyl-phenylalanine (fMLF)-induced reactive oxygen species (ROS) production of human blood. A representative kinetics of (a) chemiluminescence detected in the whole blood of a healthy donor in response to peptides is shown. Blood was incubated at 37 °C in the absence (control (CTL) ●) or the presence of 1 μM VIP (Δ) or 1 μM PACAP-38 (▾) or 1 μM secretin (○) during 10 min prior to the addition of 1 μM fMLF. (b) Histograms represent ROS as calculated by the mean of the total area under chemiluminescence curves, corresponding to four healthy donors. The response to fMLF only (CTL) is taken as 100%. Isolated (c, d) monocytes or (e, f) neutrophils were similarly challenged with (1, 10, 100 nM) of VIP prior to the addition of 0.1 μM fMLF, ROS production was measured by the chemiluminescence method. Data are means±s.e.m. of four separate experiments (*P<0.05).
VIP acts on VPAC1 in human monocytes
The effective VIP concentration, which is in the nanomolar range, and the above peptide specificity suggest that VIP action may be mediated by either VPAC1 or VPAC2 receptors. Thus we searched for the expression of these receptors in isolated phagocytes from five healthy donors. Quantitative PCR data (Figure 2a) show that VPAC1 is more expressed than VPAC2 in both circulating human monocytes and neutrophils; however, the expression of VPAC1 was higher in monocytes than in neutrophils. To ascertain whether VIP inhibits the fMLF-induced response through the interaction with VPAC1 on monocytes, we used a specific VPAC1 agonist, [ALA11,22,28]VIP (ALA), and a VPAC1-specific antagonist, PG97-269 (PG).15 A representative kinetic of ROS production by monocytes with fMLF alone as control (CTL) and in the presence of VIP, ALA, and PG is shown (Figure 2b). The cumulative data are represented by histograms (Figure 2c) and are compared with fMLF-induced ROS production (CTL). It can be noted that VIP or the VPAC1 agonist ALA effectively inhibited the fMLF-induced ROS response and that the antagonist PG alone had no effect. When PG was incubated in the presence of VIP, it abolished the initial inhibitory effect of VIP on fMLF-induced ROS response. Interestingly, the specific VPAC2 agonist, BAY 55-9837, was ineffective in modulating fMLF-induced ROS response (Supplementary Figure S1 online). These data suggest the involvement of VIP/VPAC1 interaction in monocytes that may inhibit fMLF-induced intracellular signaling leading to ROS production.
Vasoactive intestinal peptide (VIP) inhibits N-formyl-methionyl-leucyl-phenylalanine (fMLF)-induced reactive oxygen species (ROS) production in human monocytes expressing VPAC1 receptor. (a) The relative mRNA expression of VIP receptors (VPAC1 or VPACP2) vs. glyceraldehyde 3-phosphate dehydrogenase (GAPDH) was estimated in five individual samples of isolated human monocytes or neutrophils. For functional studies, prior to fMLF (0.1 μM) stimulation, isolated monocytes were incubated in the absence (control (CTL)) or in the presence of 0.1 μM VIP, 0.1 μM ALA (VPAC1 receptor agonist [ALA11,22,28]VIP), or 1 μM PG (antagonist PG97-269) alone or with the combination of 1 μM PG and 0.1 μM VIP. (b) ROS production measured by chemiluminescence; (c) histograms represent mean area under the curve in respect to fMLF-induced ROS response (CTL) Data are means±s.e.m. of three separate experiments (*P<0.05).
VIP has no effect on phorbol myristate acetate (PMA)-induced ROS production and on fMLF-induced calcium increase in monocytes
Protein kinase C (PKC) are involved in NOX2 activation in phagocytes and thus we wanted to know whether VIP could affect this pathway. To this end, we induced ROS production with PMA, a direct activator of PKC, and analyzed the effect of VIP. Results show (Figure 3a) that, in contrast to its effect on fMLF-induced ROS production, VIP was not able to inhibit PMA-induced ROS production even at high concentrations. Stimulation of cells by fMLF via its high-affinity receptor formyl peptide receptor 1 or FPR1 trigger free calcium increase in cells that is involved in the activation of several enzymes, such as PKC. Thus we wanted to know whether VIP can affect this pathway. Results show that VIP did not change fMLF-induced cytosolic calcium response of monocytes (Figure 3b). These data suggest that VIP does not affect the “FPR-G-protein calcium and PKC” axis.
Specificity of vasoactive intestinal peptide (VIP) actions on human monocyte reactive oxygen species (ROS) production. Further studies were performed to explore the mode of VIP action. (a) Isolated monocytes were incubated with different concentrations (1, 10, 100 nM) of VIP at 37 °C for 10 min prior to phorbol myristate acetate (PMA)-induced ROS production. The data are expressed as a percentage to ROS response induced by PMA. (b) Further, cytosolic calcium was measured in monocytes by means of Fura-2/AM fluorescence and 0.1 μM N-formyl-methionyl-leucyl-phenylalanine (fMLF) was added (arrow) alone (top panel) or after 10 min of incubation with 0.1 μM VIP (bottom panel). The fluorescence ratio represents the cytosolic calcium and the graph is representative of four different experiments in the presence of VIP. We did not observe any significant difference in fMLF-induced calcium response in either the presence or absence of VIP.
VIP inhibits MAPK phosphorylation induced by fMLF in monocytes
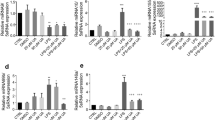
We investigated whether VIP could affect fMLF-induced MAPK signaling pathways, namely, ERK1/2 and p38MAPK, involved in fMLF-induced ROS response. Results show (Figure 4a,b) that incubation of monocytes with VIP alone did not induce ERK1/2 phosphorylation, whereas fMLF induced a dramatic increase of ERK1/2 phosphorylation and preincubation of monocytes with VIP clearly reduced this fMLF-induced effect. Interestingly, the same effect was obtained for p38 MAPK phosphorylation (Figure 4c,d) as VIP alone did not induce p38 phosphorylation, whereas fMLF induced a dramatic increase of this phosphorylation and preincubation of monocytes with VIP clearly reduced the fMLF-induced effect. These results suggest that VIP inhibits a common pathway upstream of MAPK activation in human monocytes.
Vasoactive intestinal peptide (VIP) inhibits N-formyl-methionyl-leucyl-phenylalanine (fMLF)-induced monocyte mitogen-activated protein kinase/extracellular signal–regulated kinase 1/2 (MAPK/ERK1/2) and MAPK/P-38 phosphorylation. Isolated monocytes were incubated at 37 °C for 10 min in the absence or presence of VIP before stimulation with 0.1 μM fMLF. The reaction was stopped and the lysed monocytes were analyzed by sodium dodecyl sulfate–polyacrylamide gel electrophoresis and immunoblotting as described in the Methods section. Shown in panel (a) is a representative western blot of phosphorylated-MAP/ERKP1/2 and total MAP/ERK and (b) represents the mean densitometric quantification of different western blots. Similarly, shown in panels (c and d) are representative western blots of phosphorylated-MAP/p38 and total MAP/p38 and the corresponding mean densitometric quantification. The data are expressed as a ratio of phosphorylated kinase/total kinase and represent means±s.e.m. of three separate experiments. VIP induces a significant (*P<0.05) decrease of fMLF response.
VIP action involves the inhibition of p47phox phosphorylation on Ser345
Phosphorylation of p47phox is crucial for the activation of NOX2 and ROS production in phagocytes. P47phox is phosphorylated on several serines localized in the C-terminal portion of the protein between Ser303 and Ser379. However, only Ser345 is a MAPK phosphorylation site known to be phosphorylated by p38 and ERK1/2 MAPKs.11, 16 Western blotting with a specific antibody raised against phosphorylated Ser345 of p47phox shows that fMLF significantly increased Ser345 phosphorylation as compared with VIP (Figure 5a,b). Interestingly, preincubation of monocytes with VIP clearly reduced the fMLF-induced Ser345 phosphorylation.
Effect of vasoactive intestinal peptide (VIP) on N-formyl-methionyl-leucyl-phenylalanine (fMLF)-induced Ser 345 phosphorylation of p47phox. Isolated monocytes were incubated at 37 °C for 10 min in the absence or presence of VIP before stimulation with 0.1 μM fMLF. The reaction was stopped and the lysed monocytes were analyzed by sodium dodecyl sulfate–polyacrylamide gel electrophoresis and immunoblotting as described in the Methods section. Western blottings were performed with a specific antibody directed against phosphorylated Ser345 of p47phox and anti-total p47phox. Shown in top panel (a) is a representative western blot of phosphorylated and total p47phox. (b) Quantification of different western blots are expressed as a ratio of phosphorylated Ser345 over total p47phox and represent means±s.e.m. of three separate experiments. VIP induces a significant (*P<0.05) decrease of fMLF response.
VIP attenuates carrageenan-induced edema in rat hind paws
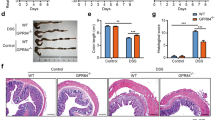
As VIP was able to inhibit monocyte ROS production, a process involved in inflammation, we wanted to test its effect on a pro-resolving pathway in vivo. Edema is transiently induced during inflammation and it can be mimicked in rat paws by local carrageenan injection.17 Carrageenan is a highly sulfated polysaccharide isolated from Chondrus crispus, a marine algae, and is used to induced inflammation in several experimental animals.18 Further, carrageenan-evoked inflammatory action is associated with increased NOX2/ROS production in phagocytes.19, 20 Thus we tested VIP effect on carrageenan-induced acute paw edema in rats. The 5-week-old rats that received carrageenan in their right paws had a progressive increase in the thickness of edema as compared with their saline-injected left paws (Figure 6a). The maximal increased was observed after 3 h postinjection of carrageenan and thereafter the edema began to resolve. When animals were treated with VIP (Figure 6a, dotted line), the edema-response curve with carrageenan followed a similar pattern as above while being less affected. The paw-edema thickness of VIP-treated animal was significantly decreased after 2 and 3 h as compared with those treated with carrageenan only. This is further illustrated by the overall state of corresponding paws (Figures 6b–d, bottom panels). At the 3-h time point, histological analysis was performed and the corresponding stained paw tissues indicate that carrageenan alone induced a large area of edema, which occupied most of the lamina propria (Figure 6c) as shown by arrow and dotted line as compared with saline CTL tissue (Figure 6b). When VIP was associated with carrageenan, the area of edema was reduced and located in the depth of lamina propria as indicated by the arrow and dotted line (Figure 6d). The marked histological and macroscopic changes induced by carrageenan were curtailed when the animals were pretreated with VIP. Also, when rats were administered by intraperitoneal injection (IP) a bolus of VIP 30 min after carrageenan-induced edema, a sharp decrease was observed in edema size as compared with saline CTL (Supplementary Figure S2). Taken together, the results show a VIP-protective effect against carrageenan-induced paw edema in rats.
Vasoactive intestinal peptide (VIP) reduces carrageenan-induced edema in rat hind paws. Carrageenan was injected into the footpad of the right hind paw of rats that had previously received either VIP or saline alone as described in the Methods section. The measured thickness (mm) of carrageenan-induced edema alone (●) or with VIP-treated animals (▪) relative to saline-treated left paw (▴) is indicated at different time points in panel (a). The rat paws of corresponding animals after 3 h of receiving (b) saline alone or (c) carrageenan alone or (d) carrageenan with VIP are shown. The bottom panels show the corresponding rat paw. Their processed sections were stained with hematoxylin and eosin as described in the Methods section and representative histological sections ( × 10) are shown and dotted lines and arrow indicate the area affected by edema. The graph data are representative of means±s.e.m. of three separate experiments and difference between carrageenan- vs. VIP and carrageenan-treated rats are indicated (*P<0.05, n=10 rats).
Discussion
VIP is a neurotransmitter that is present in almost all organs and tissues, including lymphoid organs, and its immunomodulatory properties may represent a regulatory link between inflammation and diseases.21 VIP receptor agonists are thought to have a therapeutic potential in Crohn’s disease6 and rheumatoid arthritis13 as VIP-cytoprotective effect is mediated by downregulating several key cytokines IL-6, tumor necrosis factor (TNF)-α, IL-12, and chemokine. VIP downregulation of TNF-α is mediated by cAMP-protein kinase A (PKA) pathway, which is maintained in the presence of phosphodiesterase inhibitors and represents a potential antiarthritic treatment.22 VIP could also act on the TNF-α-induced production of an excessive amount of ROS by NOX2, in synovial fluid of rheumatoid arthritis patient, which is thought to participate in the associated tissue damage and amplified inflammation.14 In line with this concept, VIP and the receptor VPAC1 agonist display antioxidant and anti-inflammatory effect in diabetic mice.23 There are very few reported studies that have investigated the effect of VIP and related peptides on ROS production by phagocytes, which are the main producers of ROS and require a tight regulation.
In the current study, we first show that VIP could inhibit fMLF-induced ROS response in whole human blood, suggesting that VIP may act on either neutrophils or monocytes that represent the major source of ROS. To discriminate between the two, we then isolated primary human monocytes and neutrophils and found that VIP in the nanomolar range was an efficient inhibitor of fMLF-induced respiratory burst of monocytes only. This VIP action on monocytes is likely to be mediated by VPAC1 or VPAC2 receptors, which are members of class B receptors belonging to the superfamily of G-protein coupled receptor.5 The observed difference in the response to VIP between monocytes and neutrophils may be attributed to a much lower protein expression of both VPAC1 and VPAC2 receptors in human neutrophils as compared with monocytes or to different cellular localization. Also, VPAC1, which was found abundantly expressed in monocytes as compared with VPAC2, would represent the main receptor involved in the action of VIP. This is sustained by several lines of evidence: the specific VPAC2 agonist, BAY 55-9837, was ineffective in modulating fMLF-induced ROS response (Supplementary Figure S1); and VIP action was fully inhibited by the highly selective antagonist of VPAC1, PG97-269, and mimicked by the agonist [ALA11,22,28]VIP.
These results are in agreement with earlier observation that VIP was able to inhibit the production of ROS in human monocytes activated by serum opsonized zymosan24 and by fMLF25 while the mechanism remained obscure. It is likely that cAMP-PKA pathway produced by VIP activation of VPAC1 could inhibit fMLF-induced ROS response. Further, it has been shown that fMLF activates the high-affinity FPR1 receptor present in phagocytes, which mediates ERK and p38MAPK activation and cytosolic Ca2+ mobilization leading to NOX2 production of ROS. Our results showed that VIP greatly diminished fMLF-induced phosphorylation of ERK and P38MAPK in human monocytes, whereas having no observable effect on cytosolic Ca2+ mobilization. These inhibitory actions of VIP/VPAC1 are in consonance with its anti-inflammatory functions. This could be extended to the closely related peptide, PACAP-38, which can act on VPAC1, as its own specific receptor PAC1 is absent on human monocytes. However, PACAP-27, unlike the predominant extended peptide PACAP-38, stimulates cytoplasmic calcium mobilization and phosphorylation ERK in both human monocytes and neutrophils and promote ROS production by itself.26, 27 The proposed explanation is that PACAP-27 is a functional ligand of the high-affinity receptor FPR1 of fMLF present in phagocytes. The PACAP-27/FPR1 activation is responsible for the associated induced ROS production, as well as chemotactic migration CD11b surface upregulation, and cytokine production.27 In our study, we found that either PACAP-38 or VIP inhibited fMLF-induced ROS response in whole blood in favor of a predominant VPAC1 interaction in line with VIP/VPAC1 major control of immunological answer in animal studies.28.
It has been previously shown that monocyte activation by bacteria or bacterial compounds such as fMLF leads to phosphorylation of cytosolic components, including p47phox subunit, a protein with an important role in the assembly and activation of NADPH oxidase.10 Thus the molecular mechanism underlying the VIP/VPAC1 inhibition of ROS response via the phagocytic NADPH oxidase was characterized by evaluating its effect on phosphorylation of the crucial Ser345 residue of p47phox subunit. We found that VIP inhibited the phosphorylation of Ser345 residue of p47phox subunit in response to fMLF and this is likely to be due to the identified downstream inhibition of kinase activation (ERK/p38MAPK) in agreement with the anti-inflammatory mechanism exerted by IL-10 and adiponectin.11, 12 Further, the availability of VIP to act on the VPAC1 receptors is likely as neurons, immune cells, and multiple tissues are able to increase VIP levels in response to inflammation after LPS challenge.13, 29 Also, VPAC1 receptor upregulation in macrophages and monocytes is a common response to acute and chronic pro-inflammatory stimuli.30, 31
The complexity of VIP actions has been highlighted using VIP-deficient mice, which exhibited resistance to LPS-induced endotoxemia.32 The absence of VIP engenders an intrinsic defect in pro-inflammatory cellular response to endotoxin with a decreased level of cytokines that could increase survival. However, in primary human monocytes, recent studies have shown that VIP is able to decrease the expression of TNFα and IL-6 receptors in LPS-stimulated monocytes but not in Salmonella typhimurium 4/74–infected monocytes.33 Thus the authors suggested that VIP should be administered as an adjunctive therapy to antibiotic treatment. This can be extended to other opportunistic bacteria associated with Crohn’s disease such as adherent-invasive Escherichia coli LF82, which crosses the intestinal mucosa and invades phagocytes by circumventing the respiratory burst.34, 35 Effective destruction of such invasive bacteria by antibiotics in conjunction with VIP to downregulate associated inflammation and excessive ROS in fistulizing Crohn’s disease broaden its therapeutic interest for inflammatory diseases. Further, we showed that VIP can also reduce carrageenan-induced paw edema in rats corresponding to an initial response of acute inflammation. This and data showing VIP-induced reduction of swelling in murine experimental arthritis model13 sustain the in vivo VIP anti-inflammatory action.
In conclusion, our results show a selective VIP/VPAC1 signaling axis in human monocytes, which decreases ROS production by NADPH oxidase and can contribute to the cytoprotective and anti-inflammatory actions of VIP in humans.
Methods
Reagents and antibodies. Human recombinant VIP, secretin, the specific VPAC1 agonist [ALA11,22,28]VIP and antagonist PG97-269 as described in the pharmacological function of receptors for VIP15 were from GL Biochem (Shanghai) Ltd, Shanghai, China. PACAP-38 and Bay 55-9837 were purchased from R&D systems (Lille, France). The peptides were certified as endotoxin-free. fMLF and protease inhibitors were from Sigma-Aldrich (Saint Quentin Fallavier, France). Antibodies against total p38 MAPK, phospho-p38 MAPK, and phospho-ERK1/2 were purchased from R&D systems. Antibodies against total ERK1/2, as well as secondary horseradish peroxidase (HRP)-labeled goat anti-rabbit antibodies, were from Santa Cruz Biotechnology (Heidelberg, Germany). The use of our rabbit polyclonal antibodies against p47phox and anti-phospho-Ser345p47phox has been described previously.16
Animals. Male Sprague-Dawley rats weighing 100–120 g were obtained from Centre Elevage Janvier, Le genest-St-Isle, France. They were housed at room temperature (21–23 °C) with a 12/12 h light/dark cycle. The animals had free access to tap water and standard food and were treated in accordance with European Community guidelines concerning care and use of laboratory animals. Experiments were performed during the light phase of the cycle. Prior to their use, they were allowed 1 week for acclimatization within the work area environment. All of the experimental protocols used in this study were approved by the local animal ethics committee and the authorized number is 02133.01.
Carrageenan-induced paw edema in rats. Rats received an IP of a saline solution containing VIP (10 μM) (0.2 mg per kg of body weight) 1 day and 1 h prior to a subplantar injection of carrageenan into the footpad of the right hind paw of rats, as described previously by Winter et al.17 The negative CTL received an equivalent volume 0.5 ml of saline vehicle by IP. Thereafter, 0.2 ml of saline solution containing 1% carrageenan was injected subcutaneously onto the plantar surface of one of the hind paws of all rats. The CTL paw was injected with saline solution. The paw thickness was measured at several time points (0 and 1, 2, 3, and 4 h after carrageenan injection) using a Dial Caliper (0–150/0.02 mm, Mitutoyo, Kawasaki, Japan). The difference in size between carrageenan-treated and CTL paws was calculated. Excised rat paws of different animals after 3 h of treatment with saline or saline and VIP or carrageenan or carrageenan and VIP were fixed in 4% formaldehyde for 72 h and then decalcified with EDTA (0.5 M) during 4 weeks. The tissue was fixed in 4% formaldehyde for 4 h prior to automatic dehydration using the Tissue Processor Leica ASP300 (Leica Microsystémes SAS, Nanterre, France) before inclusion. Tissue sections were stained with hematoxylin and eosin for histological analysis.
Monocyte and neutrophil isolation from peripheral blood. Neutrophils and monocytes were isolated from freshly drawn citrated blood of healthy subjects using dextran and Ficoll fractionation of El Benna et al.36 After centrifugation at 400 g for 30 min, neutrophil and monocyte/lymphocyte rings were collected. Erythrocytes were removed from neutrophils by hypotonic lysis. Following isolation, neutrophils were resuspended in Hank’s balanced salt solution (HBSS) and the cells were counted. Monocytes/lymphocytes were washed and resuspended in HBSS to a final density of 2 × 107 cells ml−1. Monocytes were purified by using anti-CD14-labeled microbeads from Miltenyi (Paris, France).12 Cell counting and purity were determined by Turk’s staining and flow cytometry analysis, respectively.
Measurement of ROS production. ROS production was measured at 37 °C by the luminol-enhanced chemiluminescence method: 3 × 105 human monocytes were resuspended in 500 μl of HBSS buffer containing 10 μM luminol and placed in the thermostated chamber of the luminometer (Biolumat LB937; Berthold, France SAS, Thoiry, France). Whole blood was diluted by 1/400 with HBBS buffer and assayed as above. Chemiluminescence was recorded in the presence of whole blood in the absence (CTL) or presence of recombinant VIP or related peptides PACAP-38 and secretin at a final concentration of 1 μM. After 10 min at 37 °C, 1 μM fMLF was added to CTL or pretreated samples. Isolated phagocytes (monocytes and neutrophils) are usually more responsive than whole blood to agonist (unpublished observations and Ristola and Repo37). Thus VIP and fMLF was used at 0.1 μM for ROS assays of isolated phagocytes.
Western blotting. Monocytes (5 × 106) in HBSS (160 μl) were stimulated with VIP (0.1 μM) for 10 min at 37 °C with mild shaking. The cells were then stimulated with 0.1 μM fMLF for 45 s. The reaction was stopped by adding 4 × concentrated Laemmli buffer containing 5 mmol l−1 Na3VO4, 2.5 mmol l−1 P-NPP, 10 mmol l−1 NaF, 5 mmol l−1 EDTA, 5 mmol l−1 EGTA, 20 μg l−1 leupeptin, 20 μg l−1 pepstatin, and 20 μg l−1 aprotinin. Samples were then incubated for 5 min in boiling water (100 °C) and stored at −80 °C. Samples were sonicated (10 s) before migration. Monocyte samples (106 cells) were subjected to sodium dodecyl sulfate–10% polyacrylamide gel electrophoresis using standard techniques. The separated proteins were transferred to nitrocellulose and blocked in 5% milk in TBS-T for 1 h. After blocking, the membranes were probed with anti-phospho-p38 MAPK Thr180/Tyr182 (1:1000), anti-p38 MAPK (1:1000), anti-phospho-ERK1 (T202/204)/ERK2 (T185/Y187) (1:2000), anti-ERK1 (1:1000), anti-ERK2 (1:1000), anti-phosphoSer345 (1:10,000), anti p47phox (1:5000), HRP-labeled mouse anti-goat, and HRP-labeled goat anti-rabbit antibodies (1:5000). The blots were revealed by using a chemiluminescence method.
Quantitative reverse transcriptase–PCR procedure. Total RNAs in freshly isolated human neutrophils and monocytes were extracted using the NucleoSpin RNA II Kit (Macherey-Nagel, Hoerdt, France). Quality and integrity of RNA were evaluated using an Agilent 2100 bioanalyzer (Agilent Technologies, Courtaboeuf, France). Real-time PCR amplification was carried out using a LightCycler 480 PCR system (Roche Diagnostics, Paris, France). The quantitative PCR medium included 4 μl of cDNA, 10 μl of Light Cycler 480 SYBR Green I master mix (Roche Diagnostics), and 2 μl of each forward and reverse primer in a final reaction volume of 20 μl. Primer sets (QuantiTect Primer Assays, Qiagen, Courtaboeuf, France) were designed against the complete nucleotide sequences, as deposited on GENE GLOBE, using Qiagen QT00044002 (Hs_VIPR1_1_SG) for human VPAC1, QT00073388 (Hs_VIPR2_1_SG) for human VPAC2, and QT01192646 (Hs_GAPDH_2_SG) for the calibrator glyceraldehyde-3-phosphate dehydrogenase (GAPDH). Assays were run using the following protocol: 95 °C for 5 min, 95 °C for 10 s, gene-specific annealing temperature 60 °C for 30 s, 72 °C for 30 min for 40 cycles, followed by a gradual increase in temperature from 50 °C to 97 °C during the melting stage. The VPAC1, VPAC2, and GAPDH amplicon sizes were144, 77, and 119 bp, respectively. Data were analyzed with the 2−ΔCT method described by Schmittgen and Livak,38 normalizing data to the internal control (GAPDH).
Statistical analysis. All results are expressed as mean±s.e.m. One-way analysis of variance with the Tukey–Kramer post hoc test for multiple comparisons was implemented using GraphPad Prism version 4.0 for Windows (GraphPad Software, San Diego, CA). The level of significance was set at P<0.05.
References
Laburthe, M., Couvineau, A. & Marie, J.C. VPAC receptors for VIP and PACAP. Receptors Channels 8, 137–153 (2002).
Gonzalez-Rey, E., Chorny, A. & Delgado, M. Regulation of immune tolerance by anti-inflammatory neuropeptides. Nat. Rev. Immunol. 7, 52–63 (2007).
Abad, C. et al. VIP in inflammatory bowel disease: state of the art. Endocr. Metab. Immune Disord. Drug Targets 12, 316–322 (2012).
Johnston, J.A. et al. Human T lymphocyte chemotaxis and adhesion induced by vasoactive intestinal peptide. J. Immunol. 153, 1762–1768 (1994).
Couvineau, A. & Laburthe, M. VPAC receptors: structure, molecular pharmacology and interaction with accessory proteins. Br. J. Pharmacol. 166, 42–50 (2012).
Abad, C. et al. Therapeutic effects of vasoactive intestinal peptide in the trinitrobenzene sulfonic acid mice model of Crohn’s disease. Gastroenterology 124, 961–971 (2003).
Said, S.I., Berisha, H.I. & Pakbaz, H. Excitotoxicity in the lung: N-methyl-D-aspartate-induced, nitric oxide-dependent, pulmonary edema is attenuated by vasoactive intestinal peptide and by inhibitors of poly(ADP-ribose) polymerase. Proc. Natl. Acad. Sci. US. 93, 4688–4692 (1996).
Delgado, M. & Ganea, D. Vasoactive intestinal peptide inhibits IL-8 production in human monocytes by downregulating nuclear factor kappaB-dependent transcriptional activity. Biochem. Biophys. Res. Commun. 302, 275–283 (2003).
Vignais, P.V. The superoxide-generating NADPH oxidase: structural aspects and activation mechanism. Cell. Mol. Life Sci. 59, 1428–1459 (2002).
El-Benna, J., Dang, P.M., Gougerot-Pocidalo, M.A., Marie, J.C. & Braut-Boucher, F. p47phox, the phagocyte NADPH oxidase/NOX2 organizer: structure, phosphorylation and implication in diseases. Exp. Mol. Med. 41, 217–225 (2009).
Dang, P.M.-C. et al. Anti-inflammatory effect of interleukin-10 on human neutrophil respiratory burst involves inhibition of GM-CSF-induced p47PHOX phosphorylation through a decrease in ERK1/2 activity. FASEB J. 20, 1504–1506 (2006).
Chedid, P. et al. Adiponectin and its globular fragment differentially modulate the oxidative burst of primary human phagocytes. Am. J. Pathol. 180, 682–692 (2012).
Delgado, M., Abad, C., Martinez, C., Leceta, J. & Gomariz, R.P. Vasoactive intestinal peptide prevents experimental arthritis by downregulating both autoimmune and inflammatory components of the disease. Nat. Med. 7, 563–568 (2001).
El Benna, J. et al. NADPH oxidase priming and p47phox phosphorylation in neutrophils from synovial fluid of patients with rheumatoid arthritis and spondylarthropathy. Inflammation 26, 273–278 (2002).
Harmar, A.J. et al. Pharmacology and functions of receptors for vasoactive intestinal peptide and pituitary adenylate cyclase-activating polypeptide: IUPHAR review 1. Br. J. Pharmacol. 166, 4–17 (2012).
Boussetta, T. et al. The prolyl isomerase Pin1 acts as a novel molecular switch for TNF-alpha-induced priming of the NADPH oxidase in human neutrophils. Blood 116, 5795–5802 (2010).
Winter, C.A., Risley, E.A. & Nuss, G.W. Carrageenin-induced edema in hind paw of the rat as an assay for antiiflammatory drugs. Proc. Soc. Exp. Biol. Med. 111, 544–547 (1962).
Rosa, M. Biological properties of carrageenan. J. Pharm. Pharmacol. 24, 89–102 (1972).
Roussin, A. et al. Neutrophil-associated inflammatory responses in rats are inhibited by phenylarsine oxide. Eur. J. Pharmacol. 322, 91–96 (1997).
Barth, C.R. et al. Carrageenan-induced inflammation promotes ROS generation and neutrophil extracellular trap formation in a mouse model of peritonitis. Eur. J. Immunol. 46, 964–970 (2016).
Pozo, D. VIP- and PACAP-mediated immunomodulation as prospective therapeutic tools. Trends Mol. Med. 9, 211–217 (2003).
Foey, A.D. et al. Impact of VIP and cAMP on the regulation of TNF-alpha and IL-10 production: implications for rheumatoid arthritis. Arthritis Res. Ther. 5, R317–R328 (2003).
Yu, R., Zhang, H., Huang, L., Liu, X. & Chen, J. Anti-hyperglycemic, antioxidant and anti-inflammatory effects of VIP and a VPAC1 agonist on streptozotocin-induced diabetic mice. Peptides 32, 216–222 (2011).
Wiik, P. Vasoactive intestinal peptide inhibits the respiratory burst in human monocytes by a cyclic AMP-mediated mechanism. Regul. Pept. 25, 187–197 (1989).
Kurosawa, M. & Ishizuka, T. Inhibitory effects of vasoactive intestinal peptide on superoxide anion formation by N-formyl-methionyl-leucyl-phenylalanine-activated inflammatory cells in vitro. Int. Arch. Allergy Immunol. 100, 28–34 (1993).
El Zein, N., Badran, B. & Sariban, E. The neuropeptide pituitary adenylate cyclase activating polypeptide modulates Ca2+ and pro-inflammatory functions in human monocytes through the G protein-coupled receptors VPAC-1 and formyl peptide receptor-like 1. Cell Calcium 43, 270–284 (2008).
Kim, Y. et al. Pituitary adenylate cyclase-activating polypeptide 27 is a functional ligand for formyl peptide receptor-like 1. J. Immunol. 176, 2969–2975 (2006).
Delgado, M., Gomariz, R.P., Martinez, C., Abad, C. & Leceta, J. Anti-inflammatory properties of the type 1 and type 2 vasoactive intestinal peptide receptors: role in lethal endotoxic shock. Eur. J. Immunol. 30, 3236–3246 (2000).
Brandtzaeg, P., Oktedalen, O., Kierulf, P. & Opstad, P.K. Elevated VIP and endotoxin plasma levels in human gram-negative septic shock. Regul. Pept. 24, 37–44 (1989).
Storka, A. et al. VPAC1 receptor expression in peripheral blood mononuclear cells in a human endotoxemia model. J. Transl. Med. 11, 117 (2013).
Burian, B. et al. Vasoactive intestinal peptide (VIP) receptor expression in monocyte-derived macrophages from COPD patients. Peptides 31, 603–608 (2010).
Abad, C., Tan, Y.-V., Cheung-Lau, G., Nobuta, H. & Waschek, J.A. VIP deficient mice exhibit resistance to lipopolysaccharide induced endotoxemia with an intrinsic defect in proinflammatory cellular responses. PLoS One 7, e36922 (2012).
Askar, B., Ibrahim, H., Barrow, P. & Foster, N. Vasoactive intestinal peptide (VIP) differentially affects inflammatory immune responses in human monocytes infected with viable Salmonella or stimulated with LPS. Peptides 71, 188–195 (2015).
Darfeuille-Michaud, A. et al. High prevalence of adherent-invasive Escherichia coli associated with ileal mucosa in Crohn’s disease. Gastroenterology 127, 412–421 (2004).
Elatrech, I. et al. Escherichia coli LF82 differentially regulates ROS production and mucin expression in intestinal epithelial T84 cells: implication of NOX1. Inflamm. Bowel Dis. 21, 1018–1026 (2015).
El Benna, J., Ruedi, J.M. & Babior, B.M. Cytosolic guanine nucleotide-binding protein Rac2 operates in vivo as a component of the neutrophil respiratory burst oxidase. Transfer of Rac2 and the cytosolic oxidase components p47phox and p67phox to the submembranous actin cytoskeleton during oxidase. J. Biol. Chem. 269, 6729–6734 (1994).
Ristola, M. & Repo, H. Luminol-enhanced chemiluminescence of whole blood. APMIS 97, 503–512 (1989).
Schmittgen, T.D. & Livak, K.J. Analyzing real-time PCR data by the comparative CT method. Nat. Protoc. 3, 1101–1108 (2008).
Acknowledgements
The work was supported by grants from INSERM, CNRS, Université Paris Diderot, and Inflamex. We thank Dr Veronique Albano and Mr Olivier Thibaudeau from service d’Anatomie et Cytologie Pathologique, Hôpital Xavier Bichat, Paris, France for their excellent help and advices.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Additional information
SUPPLEMENTARY MATERIAL is linked to the online version of the paper
Supplementary information
Rights and permissions
About this article
Cite this article
Chedid, P., Boussetta, T., Dang, PC. et al. Vasoactive intestinal peptide dampens formyl-peptide-induced ROS production and inflammation by targeting a MAPK-p47phox phosphorylation pathway in monocytes. Mucosal Immunol 10, 332–340 (2017). https://doi.org/10.1038/mi.2016.51
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2016.51
This article is cited by
-
VIP modulates human macrophages phenotype via FPRL1 via activation of RhoA-GTPase and PLC pathways
Inflammation Research (2021)
-
Increased IL-6 expression on THP-1 by IL-34 stimulation up-regulated rheumatoid arthritis Th17 cells
Clinical Rheumatology (2018)