Abstract
Inflammatory damage of mucosal surface of the eye is a hallmark of dry eye disease (DED) and, in severe cases, can lead to significant discomfort, visual impairment, and blindness. DED is a multifactorial autoimmune disorder with a largely unknown pathogenesis. Using a cross-sectional patient study and a well-characterized murine model of DED, herein we investigated the immunoregulatory function of interleukin-22 (IL-22) in the pathogenesis of DED. We found that IL-22 levels were elevated in lacrimal fluids of DED patients and inversely correlated with severity of disease. Acinar cells of the lacrimal glands (LGs), not inflammatory immune cells, are the primary source of IL-22, which suppresses inflammation in ocular surface epithelial cells upon desiccating stress. Moreover, loss of function analyses using IL-22 knockout mice demonstrated that IL-22 is essential for suppression of ocular surface infiltration of Th17 cells and inhibition of DED induction. Our novel findings elucidate immunoregulatory function of LG-derived IL-22 in inhibiting IL-17-mediated ocular surface epitheliopathy in DED thus making IL-22 a new relevant therapeutic target.
Similar content being viewed by others
Introduction
Ocular mucosal inflammation is characteristic for dry eye disease (DED),1, 2 a highly prevalent ocular surface autoimmune disorder. Uncontrolled severe DED can lead to vision loss owing to inflammation-induced corneal ulceration and scaring.3, 4 In the progression of DED, pathogenic immune cells, predominantly Th17 cells continuously migrate to the ocular mucosal surface5, 6, 7, 8, 9 and secrete pro-inflammatory mediators, including interleukin (IL)-17,10, 11 IL-1,12 and tumor necrosis factor (TNF)-α,13, 14 causing ocular surface inflammation and epitheliopathy. Despite strong evidence that T helper type 17 (Th17) cells are involved in ongoing DED inflammation, the precise pathological and regulatory mechanisms are not yet well understood.
IL-22, a member of the IL-10 superfamily, is a multifunction cytokine that is secreted by various immune cells such as Th17 and innate lymphoid cells during the course of mucosal immune response.15 Unlike other ILs, IL-22 does not directly regulate the function of immune cells. Instead, it binds to the IL-22 receptor (IL-22R) on cells of the skin, pancreas, liver, and kidney and tissues of the digestive and respiratory systems.15, 16, 17, 18 Serum levels of IL-22 have been shown to be significantly elevated in patients with Sjögren’s syndrome (SS), an autoimmune disorder causing dry eye and dry mouth conditions.19 Both protein and mRNA levels of IL-22, IL-23, and IL-17 have also been reported to be significantly high in the inflammatory salivary glands of SS patients.20 In addition, phosphorylation of signal transducer and activator of transcription 3, a specific transcriptional activator of IL-22 and IL-17 is upregulated in the exocrine glands of SS patients,21, 22 suggesting a functional association between IL-22 and IL-17 in the pathogenesis of SS. Recently, elevated levels of IL-22 have been shown in tears of patients with DED.11 Moreover, IL-22 has been shown to promote epithelial wound healing.23 Despite multiple reports on the expression of IL-22 in various eye conditions, the precise function of IL-22 in the immunopathogenesis of DED remains unknown.
In the present study, we have investigated the function and cellular source of IL-22 in the pathogenesis of DED. We found, for the first time, that the lacrimal gland (LG) secretes elevated levels of IL-22, which prevents ocular surface epitheliopathy and infiltration of pathogenic Th17 cells. Using IL-22-deficient mice, we confirmed that IL-22 contributes to the inhibition of Th17-medited inflammation and suppresses initiation and development of DED.
Results
Increased IL-22 levels in lacrimal fluids (LFs) of patients with DED
DED pathogenesis is primarily associated with the infiltration of Th17 cells, which have been demonstrated to secrete IL-17 and IL-22.11, 16 As tears are a mixed fluid composed of secretions from the LG, meibomian gland, and corneoconjunctival cells, we precisely collected the pure LG-secreted fluid (LF) and total tear fluid (TF) from conjunctival sac (see Supplementary Video online) of healthy controls and DED patients to evaluate the expression levels of IL-22 and IL-17. IL-22 levels in LFs of DED patients (median 1621 pg ml−1; interquartile range (IQR; 1154–2641) were significantly higher as compared with the healthy control (median 51 pg ml−1, IQR 25–99, P<0.001; Figure 1a). However, no significant difference in the IL-22 levels was observed in TFs of DED patients (median 566 pg ml−1, IQR 421–811) and healthy controls (median 492 pg ml−1, IQR 403–621). These increased levels of IL-22 in LFs but not in TFs suggest that LGs could be a primary source of high levels of IL-22 in DED. IL-17 levels in LFs (median 769 pg ml−1, IQR 421–1101) of DED patient were significantly higher as compared with healthy controls (median 27.5 pg ml−1, IQR 19–45, P<0.001; Figure 1b). In contrast to IL-22, IL-17 levels in TFs of DED patients (median 3289.5 pg ml−1, IQR 2514–3688) were higher than that in healthy controls (median 527 pg ml−1, IQR 216–621, P<0.001).
Interleukin (IL)-22 and IL-17 levels in tears of patients with dry eye disease (DED) and healthy controls (CTL). Lacrimal fluid (LF) from lacrimal glands and total tear fluids (TF) from conjunctival sac were collected using polyester wick from DED patients (n=31) and CTL (n=18). IL-22 and IL-17 levels in LF and TF were estimated using Nano-liquid chromatography-tandem mass spectrometry. (a) IL-22 levels in LF and TF of CTL and DED patients. (b) IL-17 levels in LF and TF of CTL and DED patients. The box plots bind the interquartile range divided by the median and dots indicate individual values (P-value by Mann–Whitney U-test). (c) Correlation analysis between ocular surface disease index (OSDI) and IL-22 levels in LF and TF of DED patients. (d) Correlation analysis between OSDI and IL-17 levels in LF and TF of DED patients. Individual points and lines represent the observed values and regression lines (r, Spearman correlation coefficient, −1⩽r⩽1; r and P-value by Spearman’s correlation test).
IL-22 levels inversely correlate with the severity of DED
Having shown the increased expression of IL-22 and IL-17 in the LFs of DED patients, we next determined the association of IL-22 and IL-17 levels with the severity of DED. Correlation and regression analyses were performed to determine correlation between cytokine levels and the severity of DED measured as ocular surface disease index (OSDI). Significant negative correlations between the levels of IL-22 both in LFs (r=−0.777, P<0.001) or TFs (r=−0.922, P<0.001) and OSDI score were observed, suggesting that IL-22 at the ocular surface could be associated with reduction of disease severity (Figure 1c). In contrast to IL-22, significant positive correlations between the IL-17 levels both in LFs (r=0.869, P<0.001) or in TFs (r=0.855, P<0.001) and OSDI scores was observed indicating that IL-17 is involved in augmenting disease severity (Figure 1d). Moreover, OSDI scores <20 were associated with undetectable levels of IL-17 in both LFs and TFs.
LGs expressed high levels of IL-22 in a murine model of DED
Increased IL-22 expression particularly in LFs and its negative correlation with disease severity prompted us to examine the cellular source of IL-22 in DED. As investigating the source of IL-22 in human LGs was not possible, we used a well-standardized murine model of DED5, 6, 7, 8 for further investigations. LGs from DED and healthy mice (control) were harvested. Real-time PCR was performed to measure IL-22 mRNA expression. Similar to our observation in DED patients, DED induction in mice resulted in a significant increase in IL-22 mRNA expression compared with control non-DED mice (Figure 2a). IL-22 expression was further confirmed at protein level by performing enzyme-linked immunosorbent assay (ELISA) on the supernatants from LG lysates. A significant 5–6-fold increase in IL-22 protein was observed in DED mice compared with the control group (Figure 2b). Furthermore, we investigated the precise cellular source of IL-22 in the LG using immunohistochemistry. DED induction resulted in increased IL-22 expression and massive LG infiltration of leukocytes compared with control mice. But surprisingly, this increased IL-22 expression was associated primarily with the glandular acinar cells and not infiltrating leukocytes (Figure 2c,d). These IL-22-positive acinar cells were in close proximity of infiltrating immune cells.
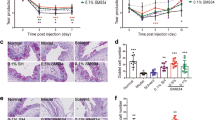
Expression of interleukin (IL)-22 in the lacrimal glands (LGs) of mice. LGs from control (CTL) and dry eye disease (DED) mice were harvested. (a) IL-22 mRNA expression in LG lysates was quantitated using real-time PCR. (b) IL-22 protein concentrations in LG lysates was measured by enzyme-linked immunosorbent assay. (c) Representative immunohistochemistry micrographs of LG cross-sections from two healthy and four DED mice, which were stained for IL-22 (blue arrowhead). Black arrows indicate infiltrated immune cells. (d) Bar chart showing quantitation of IL-22-producing cells as IL-22+ cell/high-power field. Data shown are means (bars)±s.e.m (error bars) of three independent experiments (n=5 mice per group; **P<0.001 by independent t-test). A full color version of this figure is available at the Mucosal Immunology journal online.
IL-22R expression on the ocular surface
The fact that receptor expression at the site of action is essential for cytokines to exert their function led us to investigate the IL-22R system at the ocular surface. IL-22R is a heterodimer of IL-22R1 and IL-10R2 subunits. Real-time PCR for IL-22R1 and IL-10R2 mRNA expression in total corneal and conjunctival lysates was performed. The results revealed that IL-22R1 is constitutively expressed at the ocular surface and its expression does not alter after DED induction. However, IL-10R2 expression was upregulated at the ocular surface in DED mice compared with control mice (Figure 3a). Similar to mRNA expression, protein expression analyses using flow cytometry and immunohistochemistry revealed that both IL-22R1 and IL-10R2 are expressed at the ocular surface (Figure 3b,c), and IL-10R2 was increased in mice with DED compared with healthy control.
Expression of interleukin (IL)-22 receptors on the ocular surface of mice. Corneas and conjunctivae from healthy (CTL) and dry eye disease (DED) mice were harvested 7 days after DED induction. (a) IL-22R1 and IL-10R2 transcripts levels were determined using real-time PCR. (b) Immunohistochemistry micrographs of corneal cross-sections showing the expression of IL-22R1 (black arrows) and IL-10R2 (arrowheads) by corneal epithelial cells. (c) Representative flow cytometric analysis of corneal and conjunctival single-cell suspension showing the expression of IL-22R1 and IL-10R2. The values shown are means (bars)±s.e.m (error bars) of three independent experiments (n=5 mice per group; **P<0.001 by independent t-test; NS, not significant). A full color version of this figure is available at the Mucosal Immunology journal online.
IL-22 inhibits the expression of inflammatory cytokines by ocular surface epithelial cells under hyperosmolar stress
Because IL-22 expression is increased in LGs in DED and its receptor is expressed on the ocular surface, we next examined the effect of IL-22 on the production of inflammatory cytokines by corneal epithelial cells in vitro under desiccating hyperosmolar stress. This assay mimics the pathophysiology of desiccating stress-induced ocular surface inflammation in DED.24 Primary human corneal epithelial cells (hCECs) were exposed to 380 mOsm medium to induce hyperosmolar stress in the presence and absence of IL-22. After 18 h, culture supernatants were collected and ELISA was performed to assess the expression of inflammatory cytokines IL-1β, TNF-α, and IL-8 (Figure 4a) and the Th17-inducer cytokines IL-6 and IL-23 (Figure 4b). Hyperosmolar stress induced the secretion of IL-1β, TNF-α, IL-8, IL-6, and IL-23 by hCECs, and this induction could be substantially suppressed by IL-22. These results indicate that IL-22 exerts anti-inflammatory effects on ocular surface epithelial cells.
Effect of interleukin (IL)-22 on human corneal epithelial cell (hCEC) response to desiccating hyperosmolar stress. hCECs were cultured in 380 mOsm medium for 18 h in the presence and absence of IL-22 (30 ng ml−1). Culture supernatants were collected and enzyme-linked immunosorbent assay was performed on the (a) inflammatory cytokines IL-1β, tumor necrosis factor (TNF)-α, and IL-8 as well as (b) the T helper type 17–inducer cytokines IL-6 and IL-23. Results are expressed as means±s.e.m (error bars) of two independent experiments (n=8). Dots indicate individual values (*P<0.01 and **P<0.001 by one-way analysis of variance test with Bonferroni’s correction; NS, not significant).
IL-22 deficiency enhances ocular surface infiltration of IL-17-secreting cells and epitheliopathy in DED
Finally, to determine the function of IL-22 in the pathogenesis of DED in vivo, we created IL-22 deficiency either using an IL-22-neutralizing antibody (αIL-22) or IL-22 knockout (KO) mice. αIL-22s were intravenously administered into mice during DED induction. Phosphate-buffered saline (PBS)-injected mice served as controls. Seven days after disease induction, ocular surface tissues (cornea and conjunctiva) were harvested to measure the frequencies of IL-17-secreting cells using flow cytometry. DED induction resulted in increased infiltration of IL-17-secreting cells, which was further augmented in αIL-22-treated mice as compared with PBS control (Figure 5a). IL-22 function in DED pathogenesis was further confirmed using genetically deficient IL-22 KO mice. DED was induced in IL-22 KO and wild-type (WT) mice. Then frequencies of IL-17-secreting cells on the ocular surface and progression of disease by grading corneal epithelial erosions were evaluated. Consistent with blocking IL-22 in vivo, IL-22 KO mice showed significantly enhanced ocular surface infiltration of IL-17-positive cells compared with WT mice (Figure 5b). Regarding the cellular origin of increased IL-17 secretion at the ocular surface in DED mice, flow cytometric analysis of ocular surface tissues revealed increased infiltration of CD4+IL-17+ cells (Th17; 14.00%) but not CD3ɛ-NK1.1+IL-17+ cells (natural killer (NK) cell; 1.67%) and CD11b+Gr-1+IL-17+ cells (neutrophils; 1.93%) (see Supplementary Figure). Using immunohistochemistry, effect of IL-22 on infiltration of IL-17-secreting CD4 cell was further confirmed in IL-22 KO mice after DED induction. Consistent with flow cytometric analysis, IL-22 deficiency resulted in increased infiltration of CD4+IL-17+ cells in conjunctival cross-sections after DED induction (Figure 5c, white arrows). Moreover, most of CD4+IL-17+ primarily infiltrated into conjunctival epithelia (Figure 5c, green arrows). As IL-6 and IL-23 are major cytokines that promote Th17 immune response,25, 26, 27, 28 we next estimated ocular surface levels of IL-6 and IL-23 in WT and IL-22 KO mice after DED induction. ELISA analysis on corneoconjunctival lysates showed elevated levels of IL-6 and IL-23 in WT DED mice compared with the normal control group. Similar to Th17 frequencies, IL-22 KO mice showed a significant 2.5-fold increase in the ocular surface level of IL-6 and IL-23 compared with WT after DED induction (Figure 5d). We next investigated the effect of IL-22 epitheliopathy by monitoring corneal erosions, which is a pathological characteristic of DED, in both WT and IL-22 KO mice. IL-22 KO mice showed a significant threefold increase of the corneal erosion grade during the early induction phase (day 1 and 3) compared with WT mice (Figure 5e). However, in the later stage of the disease (day 7 onward) the corneal erosion scores in IL-22 KO and WT mice were similar. Having shown earlier that non-immune acinar cells are a major source of IL-22, we next investigated whether IL-22 secretion by non-immune acinar cells is critical for the suppression of pathogenic Th17 cell responses during DED progression. Bone marrow (BM) chimera experiments were performed where WT and IL-22 KO irradiated mice were reconstituted with BM cells of IL-22 KO and WT mice, respectively (Figure 6a). At 7 days post-DED induction, flow cytometric analysis of corneoconjunctival cells revealed increased infiltration of ocular surface Th17 cells in the IL-22 KO host with WT BM compared with the WT host with IL-22 KO BM (Figure 6b). Consistently, the cornea erosion grades were higher for the IL-22 KO host with WT BM than the WT host with IL-22 KO BM during DED (Figure 6c). Collectively, these results suggest that non-immune cell–derived IL-22 is essential for the suppression of pathogenic Th17 infiltration after DED induction.
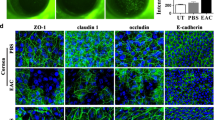
Effect of interleukin (IL)-22 deficiency on IL-17+ cell infiltration and epitheliopathy in mice with dry eye disease (DED). (a) IL-22-neutralizing antibodies or phosphate-buffered saline (PBS) were intraperitoneally injected into wild-type (WT) mice with DED and analyzed on day 7. Naive mice served as healthy controls (CTL). Single-cell suspension of cornea and conjunctiva were stained with anti-IL-17 antibodies and flow cytometry was performed. (b) Corneas and conjunctivae were harvested from WT and IL-22 knockout (KO) mice with DED, and IL-17+ cell frequencies (%) were analyzed using flow cytometry. The data shown are means (bars)±s.e.m (error bars) of three independent experiments (n=5 mice per group; *P<0.01 and **P<0.001 by one-way analysis of variance (ANOVA) test with Bonferroni’s correction). (c) Representative confocal micrographs of conjunctiva showing co-localization of CD4+ (red) and IL-17+ (green) cells (white arrow) and infiltration of these cells into conjunctival epithelia (green arrows) at 7-day post-DED induction. (d) Enzyme-linked immunosorbent assay for IL-6 and IL-23 concentration from corneoconjunctival tissue at 7 days after DED induction. The results shown are means (bars)±s.e.m (error bars) of three independent experiments (n=4 mice per group; **P<0.001 by one-way ANOVA test with Bonferroni’s correction). (e) Representative images of fluorescein-stained ocular surface and corneal erosion grade of WT (empty circle) and IL-22 KO (filled circle) after DED induction. Results are expressed as means (individual points)±s.e.m (error bars) of three independent experiments (n=4 mice per group; *P<0.01 and **P<0.001 by a linear mixed model with Bonferroni’s correction). A full color version of this figure is available at the Mucosal Immunology journal online.
Non-immune cell–derived interleukin (IL)-22 prevents ocular surface infiltration of pathogenic T helper type 17 cells during dry eye disease (DED). (a) Schematic illustration of bone marrow (BM) chimera experiments. (b) Representative histograms showing the frequencies of IL-17-secreting cell (gated within CD4+ cell) at the ocular surface of wild-type (WT) host with IL-22 knockout (KO) BM (blue) and IL-22 KO host with WT BM (red) after DED induction. (c) Representative images of fluorescein-stained ocular surface of BM chimeras after DED induction. The values shown are means (bars)±s.e.m (error bars) of two independent experiments (n=4 mice per group; *P<0.01 and **P<0.001 by independent t-test). A full color version of this figure is available at the Mucosal Immunology journal online.
Discussion
This study demonstrates the immunoregulatory function of IL-22 in suppressing IL-17-mediated ocular mucosal inflammation in DED. Specifically, we show herein that elevated secretion of IL-22 by the LG in DED patients negatively correlates with disease severity. Acinar cells of the LGs, and not infiltrating immune cells, produce IL-22, which protects ocular surface epithelium and inhibits infiltration of Th17 cells to the ocular surface in desiccating stress-induced DED.
In the pathogenesis of DED, T-cell cytokines, primarily IL-17 initiate the immune response and cause inflammation at the ocular surface.6, 11, 29 In addition to IL-17, IL-22 levels have also been reported to be increased in many autoimmune disorders.16, 30 We show that LF from DED patients has increased levels of IL-17 and IL-22, two Th17 cytokines that have been associated with the pathogenesis of various autoimmune disorders, including SS. In accordance with previous studies,11, 31 we observed that IL-17 levels positively correlate with disease severity. However, our study further shows that IL-22 levels in tears inversely correlate with severe disease symptoms, suggesting a protective role of IL-22 in the DED. As LF is diluted with secretions from meibomian glands and corneoconjunctival cells while constituting the TF at the ocular surface, we observed a moderate increase in IL-22 levels in TF of DED patients compared with healthy controls. IL-22 has been strongly associated with mucosal immune response owing to its secretion by immune cells and direct effect on mucosal surface of various organs, such as the pancreas, liver, kidney, and joints.18, 32 Because it is difficult to examine the exact cellular source of IL-22 in human subjects, we used a well-characterized mouse model of DED to explore the source and precise function of IL-22 in the pathogenesis of DED. Multiple reports suggest that IL-22 is primarily secreted by Th17, Th22, NK cells, and innate lymphoid cells.15, 33, 34 Our study provides novel evidence that non-immune cells such as acinar cells in the LGs secrete IL-22, and this secretion is augmented in DED condition. Moreover, results from BM chimera experiments suggest protective function of non-immune cells secreting IL-22 in DED (Figure 6).
We demonstrate an increased expression of IL-22Rs (heterodimer of IL-22R1 and IL-10R2) by the ocular surface epithelium, indicating the importance of an IL-22-mediated signaling cascade in the immunopathogenesis of DED. Expression of IL-22Rs has been shown previously on other non-ocular mucosal surfaces, such as the lung and intestine.35, 36 DED is associated with the increased expression of proinflammatory cytokines TNF-α, IL-1β, and IL-8 and Th17-inducing cytokines IL-6 and IL-23 at the ocular surface.5 Here we show that IL-22 inhibits the expression of such inflammatory cytokines and Th17-inducing cytokines IL-6 and IL-23 by ocular surface epithelial cells under desiccating (hyperosmotic) stress.
Utilizing the loss of function approach, we finally determined the in vivo contribution of IL-22 in the pathogenies of DED. We blocked the endogenous IL-22 using a neutralizing antibody in a mouse model of DED. Our study shows that in vivo neutralization of IL-22 led to increased infiltration of IL-17-secreting cells at the ocular surface under desiccating stress, suggesting that IL-22 is essential for inhibiting Th17-mediated mucosal inflammation in DED. We confirmed the effect of IL-22 on Th17 cell infiltration and progression of DED pathogenesis using IL-22 KO mice. Consistent with our IL-22-neutralization assay, IL-22 KO mice with DED showed a profound infiltration of IL-17-positive cells to the ocular surface. Based on our previous results showing IL-22-mediated inhibition of the expression of Th17-inducers IL-6 and IL-23 by ocular surface epithelial cells (Figure 4b) and their increased expression in IL-22 KO mice (Figure 5d), we hypothesize that IL-22 deficiency promotes Th17 cell generation and infiltration in DED mice. In fact, a previous report has suggested that IL-22 suppresses the infiltration of Th17 cells in intestinal mucosa and maintains mucosal barrier function.25 Furthermore, our data shows that IL-22-mediated suppression of pathogenic IL17-secreting cells results in reduced DED, particularly in the early induction phase, as demonstrated by high clinical corneal erosion scores in IL-22 KO mice. However, similar high corneal erosion scores in the later stage of disease in both IL-22 KO and WT mice suggests that IL-22 might be inefficient in regulating severe IL-17-mediated ocular inflammation in chronic or later stage of DED. This could also be due to the low expression of IL-22 in severe inflammation similar to our DED severity and IL-22 correlation data (Figure 1c) in humans.
In summary, these findings provide new insights on both cellular source and function of IL-22 in the pathogenesis of DED. Inverse correlation of high levels of IL-22 in human tears and its inhibitory effect on Th17-mediated inflammation in mice indicate that IL-22 regulates ocular mucosal inflammation in DED. In addition, the demonstration that IL-22 blockade leads to amplification of Th17 immunity and ocular surface damage suggests its potential as a novel treatment approach. Strategies designed to augment IL-22 levels at the ocular surface, and thereby suppressing Th17 functionality, may be a viable therapeutic approach for DED.
Methods
Patient enrollment and determination of DED
The study was approved by the Institutional Review Board and followed the tenets of the Declaration of Helsinki, and informed consents were obtained from all patients. A total of 31 non-Sjögren-type DED patients (11 male, 20 female) with a mean age of 59.3±13.1 years (range: 35–78 years) completed the study. The inclusion criteria were as follows: one or more DED-related symptoms, including tightness, foreign body sensation, irritation, red eye, itching sensation, blurring, or pain; Schirmer’s test (without anesthesia) of 5 mm in ⩽5 min in both eyes; tear break-up time of ⩽5 s in both eyes; and typical DED pattern of superficial punctuate erosion of conjunctiva or cornea. The control group was composed of 18 healthy, age- and sex-matched subjects (6 male, 12 female) who had no history of ocular or systemic disease. The mean age of controls was 57.4±14.1 years (range: 39–71 years).
For baseline evaluations, the tear break-up time, Schirmer’s test, fluorescein staining using biomicroscopy, tear sampling, and intraocular pressure were assessed on both eyes of DED patients and healthy controls. We also obtained symptom severity scores from DED patients using the OSDI score. During the data collection period, all evaluations were performed in a blinded manner. DED parameters and tear sampling were performed by H.S.H. and Y.W.J., blinded to the patient’s disease status, and collected tears and prepared them for analysis. The data were then analyzed by E.J.C. who was also blinded to the patient’s disease status.
Tear collection and measurements of IL-22 and IL-17 levels
To measure the concentration of IL-22 and IL-17 in patients’ tears, a bonded 2.0 × 10 mm2 polyester fiber rods was used to collect total TF from conjunctival sac, as previously reported.37, 38 Briefly, a polyester wick was applied to tear meniscus of lower conjunctival sac and the collected samples were stored at −70 °C for mass spectrophotometric analysis. In addition to the TF, which is a mixed fluid of the secretion from the LGs, meibomian glands, and corneoconjunctival cells, pure LF was collected. The detailed methods for collecting LF are shown in Supplementary Video.
All Nano-liquid chromatography-tandem mass spectrometry (LC-MS/MS) experiments were carried out on an Applied Biosystem/MDS Sciex 4000 Qtrap quadrupole mass spectrometer (AB/MDS Sciex, Concord, Ontario, Canada) that was equipped with a turbo-ion spray source. The mass spectrometer was coupled with an Agilent 1200 series HPLC system (Agilent Technologies, Santa Clara, CA). Data were acquired and processed using the Analyst software (version 1.4.2, AB/MDS Sciex). The chromatographic separation was achieved with a Synergi Hydro-RP (C18) 50 × 2.1 mm I.D., 4-μm 80-Å particle column (Phenomenex, Torrance, CA) at 40 °C. The mobile phase was a binary gradient using 40% acetonitrile as solution A and 100% methanol as solution B. The flow rate was 0.6 ml min−1. In addition to the IL-22 and IL-17, total protein concentrations in LF (Control: 6.2±3.6 mg ml−1; DED: 4.1±3.8 mg ml−1, P=0.033 by Mann–Whitney U-test) and TF (Control: 7.9±3.2 mg ml−1; DED: 13.9±5.2 mg ml−1, P=0.029 by Mann–Whitney U-test) were also estimated using LC-MS/MS.
Mouse model of DED
Six- to 8-week-old male C57BL/6 mice (Charles River Laboratory, Wilmington, MA) and IL-22 KO mice (UC Davis MMRRC, Davis, CA) were used in accordance with the standards of the Association for Research in Vision and Ophthalmology Statement for the Use of Animals in Ophthalmic and Vision Research. The research protocol was approved by the Yonsei University College of Medicine. The in vivo mouse experiments were performed at the Institute of Vision Research at the Yonsei University College of Medicine. DED was induced in mice as described previously.6, 7, 39, 40 In brief, mice were exposed to a controlled environment chamber, which allows the controlled regulation and maintenance of the temperature (21–23 °C), relative humidity (<30%), and airflow (15 liter min−1). Clinical signs such as corneal erosions were assessed by corneal fluorescein staining using 1% fluorescein (Sigma-Aldrich, St Louis, MO) according to the standard National Eye Institute scoring system. One week after DED induction, mice were killed and tissues were collected for immunohistochemistry and molecular studies. For in vivo IL-22 blockade experiments, 100 μg per mouse of αIL-22 (AF582, R&D Systems, Minneapolis, MN) or PBS were intravenously injected into WT mouse at 2 h before placing them into the controlled environment chamber and then daily for 3 days.
BM chimera experiments
WT B6 and IL-22 KO mice between 6 and 8 weeks of age were used to make BM chimera. At the day of BM transfer, mice were given lethal total body irradiation (950–1000 rad) from a 137 Cs source. Four hours later, they were reconstituted with WT or IL-22 KO mice BM cells (1 × 107) that had been harvested from the femurs of age-matched mice. Experimental transfers were as follows: WT BM cells into irradiated IL-22 KO mice (WT BM→IL-22 KO host) and IL-22 KO BM cells into irradiated WT mice (IL-22 KO BM→WT host). Animals were allowed to reconstitute for 45 days. Before DED induction, only healthy mice with no obvious signs of graft-vs-host disease or other illness were used in experiments. DED induction, killing, and securement of the tissues were performed as described above. At day 7 post-DED induction, the cornea and conjunctiva were harvested to analyze the infiltration of Th17 cells using flow cytometry.
Immunohistochemistry
Whole corneas and LGs were fixed in 4% paraformaldehyde and histological cross-sections (7-μm thick) were mounted on poly-L-lysine-coated slides. Cross sections were then deparaffinized and stained with anti-mouse primary (IL-22, GTX109659, GeneTex, Zeeland, MI; IL-22R1, ab211675, Abcam, Cambridge, UK; IL-10R2, SC-271969, Santa Cruz Biotechnology, Santa Cruz, CA) overnight at 4 °C. Sections were then incubated with peroxidase-conjugated streptavidin for 20 min at room temperature. Protein expression was detected using diaminobenzidine chromogen and 0.05% H2O2 and evaluated under a florescent microscope (BX51-FL, Olympus, Tokyo, Japan). The sections were also counterstained with Meyer’s hematoxylin (DAKO, Glostrup, Denmark). Human skin and colon tissue were used as positive controls (data not shown). Sections were observed under a light microscope (Axio Imager 2, Carl Zeiss, Oberkochen, Germany). For immunofluorescence staining, anti-mouse IL-17 antibody (ab79056, Abcam), Goat anti-rabbit immunoglobulin G (ab150077, Abcam), and Alexa Fluor 594–conjugated anti-mouse CD4 antibody (100446, BioLegend, San Diego, CA) were used. The sections were observed with the confocal microscopy (LSM 800, Carl Zeiss).
Quantitative PCR
Corneas and LGs were harvested from control and DED mice. RNA was isolated using the RNeasy Micro Kit (Qiagen, Valencia, CA) and reversed transcribed into cDNA with the Superscript III Kit (Invitrogen, Carlsbad, CA). Quantitative PCR was performed using SYBR Premix Ex Taq (Takara Bio, Shiga, Japan) with preformulated primers and StepOnePlus Real-Time PCR detection system (Applied Biosystems, Foster City, CA). The results were analyzed by the comparative threshold cycle method. GAPDH (glyceraldehyde 3-phosphate dehydrogenase) was used as an internal control, and data were normalized to untreated controls.
hCEC culture and hyperosmotic stimulation
Human corneal limbal tissue was harvested from donor corneal buttons following keratoplasty, in accordance with the tenets of the Declaration of Helsinki and with the permission of the Institutional Review board. Corneal limbal tissues were prepared and cultured as described previously.41, 42 In brief, cells were cultured for a period of 18 h in a hyperosmolar serum-free media (380 m osmol; achieved by adding sodium chloride) in the presence or absence of murine recombinant IL-22 (BioLegend). The actual osmolality of medium was confirmed with an ohmmeter (Model 3320, Advanced instrument, Norwood, MA).
Flow cytometry
Single-cell suspensions of harvested corneas were prepared by collagenase digestion and blocked with an anti-FcR monoclonal antibody for 30 min at 4 °C in 1% bovine serum albumin/0.02% NaN3/PBS. Isolated cells were stained with fluorochrome-conjugated antibodies and appropriate isotype controls (BioLegend) for 45 min at 4 °C. For intracellular staining, cells were first stimulated with Phorbol 12-myristate 13-acetate/ionomycin (Sigma-Aldrich) for 6 h in the presence of GolgiStop (BD Biosciences, San Jose, CA), and then fixed and permeabilized using Fix/Perm (eBioscience, San Diego, CA). Stained cells were analyzed with a FACSAria flow cytometer (BD Biosciences).
ELISA
Protein levels of cytokines in mouse LG tissues and in culture supernatant of hCECs were quantified using commercially available ELISA kits: human IL-17 and IL-22 (D1700 and D2200, respectively; R&D Systems), human IL-1β, IL-6, IL-8, IL-23, and TNF-α (437005, 430505, 431505, 435407, and 430205, respectively; BioLegend), and mouse IL-6, IL-17, IL-22, and IL-23 (431305, 436205, 436305, and 433704, respectively; BioLegend).
Statistical analysis
Statistical analyses were performed using SPSS for Windows (version 21.0; SPSS, Chicago, IL). Testing for the normality of distribution was performed by using the Kolmogorov–Smirnov test. For in vivo and in vitro data that was normally distributed, independent t-test was performed to compare the differences between the two groups and one-way analysis of variance test with Bonferroni’s correction was used to make comparisons among three or more groups. A linear mixed model with Bonferroni’s correction for repeated-measures covariance pattern with unstructured covariance within samples was used for estimating significant differences between groups over time. As the majority of the clinical data including tear cytokine levels did not show a normal distribution, non-parametric tests were adopted. Analyses included the frequency for categorical data and the median with IQR for continuous data. Mann–Whitney U-test was performed to compare the differences between the two groups and Kruskal–Wallis test with Bonferroni–Dunn’s procedure was used to compare the groups for continuous variables. Correlation between tear cytokine levels and dry eye symptoms was assessed using Spearman’s correlation test. A P-value of <0.05 was considered significantly different. Results are presented as mean±s.e.m.
References
Barabino, S., Chen, Y., Chauhan, S. & Dana, R. Ocular surface immunity: homeostatic mechanisms and their disruption in dry eye disease. Prog. Retin. Eye Res. 31, 271–285 (2012).
Chauhan, S.K. & Dana, R. Role of Th17 cells in the immunopathogenesis of dry eye disease. Mucosal Immunol. 2, 375–376 (2009).
Johnson, M.E. & Murphy, P.J. Changes in the tear film and ocular surface from dry eye syndrome. Prog. Retin. Eye Res. 23, 449–474 (2004).
Niederkorn, J.Y. et al. Desiccating stress induces T cell-mediated Sjogren's Syndrome-like lacrimal keratoconjunctivitis. J. Immunol. 176, 3950–3957 (2006).
De Paiva, C.S. et al. IL-17 disrupts corneal barrier following desiccating stress. Mucosal Immunol. 2, 243–253 (2009).
Chauhan, S.K. et al. Autoimmunity in dry eye is due to resistance of Th17 to Treg suppression. J. Immunol. 182, 1247–1252 (2009).
Chen, Y., Chauhan, S.K., Lee, H.S., Saban, D.R. & Dana, R. Chronic dry eye disease is principally mediated by effector memory Th17 cells. Mucosal Immunol. 7, 38–45 (2014).
Chauhan, S.K. et al. A novel pro-lymphangiogenic function for Th17/IL-17. Blood 118, 4630–4634 (2011).
Dohlman, T.H. et al. The CCR6/CCL20 axis mediates Th17 cell migration to the ocular surface in dry eye disease. Invest. Ophthalmol. Vis. Sci. 54, 4081–4091 (2013).
Zheng, X., de Paiva, C.S., Li, D.Q., Farley, W.J. & Pflugfelder, S.C. Desiccating stress promotion of Th17 differentiation by ocular surface tissues through a dendritic cell-mediated pathway. Invest. Ophthalmol. Vis. Sci. 51, 3083–3091 (2010).
Tan, X. et al. Analysis of Th17-associated cytokines in tears of patients with dry eye syndrome. Eye (Lond) 28, 608–613 (2014).
Song, X.J. et al. Neurturin-deficient mice develop dry eye and keratoconjunctivitis sicca. Invest. Ophthalmol. Vis. Sci. 44, 4223–4229 (2003).
Lam, H., Bleiden, L., de Paiva, C.S., Farley, W., Stern, M.E. & Pflugfelder, S.C. Tear cytokine profiles in dysfunctional tear syndrome. Am. J. Ophthalmol. 147, 198–205 e191 (2009).
Ji, Y.W. et al. Neutralization of ocular surface TNF-alpha reduces ocular surface and lacrimal gland inflammation induced by in vivo dry eye. Invest. Ophthalmol. Vis. Sci. 54, 7557–7566 (2013).
Rubino, S.J., Geddes, K. & Girardin, S.E. Innate IL-17 and IL-22 responses to enteric bacterial pathogens. Trends Immunol. 33, 112–118 (2012).
Yang, X. & Zheng, S.G. Interleukin-22: a likely target for treatment of autoimmune diseases. Autoimmun. Rev. 13, 615–620 (2014).
Rutz, S., Eidenschenk, C. & Ouyang, W. IL-22, not simply a Th17 cytokine. Immunol. Rev. 252, 116–132 (2013).
Sonnenberg, G.F., Fouser, L.A. & Artis, D. Border patrol: regulation of immunity, inflammation and tissue homeostasis at barrier surfaces by IL-22. Nat. Immunol. 12, 383–390 (2011).
Lavoie, T.N., Stewart, C.M., Berg, K.M., Li, Y. & Nguyen, C.Q. Expression of interleukin-22 in Sjogren's syndrome: significant correlation with disease parameters. Scand. J. Immunol. 74, 377–382 (2011).
Ciccia, F. et al. Rituximab modulates the expression of IL-22 in the salivary glands of patients with primary Sjogren's syndrome. Ann. Rheum. Dis. 72, 782–783 (2013).
Pan, H.F., Li, X.P., Zheng, S.G. & Ye, D.Q. Emerging role of interleukin-22 in autoimmune diseases. Cytokine Growth Factor Rev. 24, 51–57 (2013).
Ciccia, F. et al. Potential involvement of IL-22 and IL-22-producing cells in the inflamed salivary glands of patients with Sjogren's syndrome. Ann. Rheum. Dis. 71, 295–301 (2012).
Li, Z., Burns, A.R., Miller, S.B. & Smith, C.W. CCL20, gammadelta T cells, and IL-22 in corneal epithelial healing. FASEB J. 25, 2659–2668 (2011).
Deng, R. et al. Oxidative stress markers induced by hyperosmolarity in primary human corneal epithelial cells. PLoS One 10, e0126561 (2015).
Shih, V.F. et al. Homeostatic IL-23 receptor signaling limits Th17 response through IL-22-mediated containment of commensal microbiota. Proc. Natl. Acad. Sci. USA 111, 13942–13947 (2014).
Qu, N. et al. Pivotal roles of T-helper 17-related cytokines, IL-17, IL-22, and IL-23, in inflammatory diseases. Clin. Dev. Immunol. 2013, 968549 (2013).
Tanaka, T., Narazaki, M. & Kishimoto, T. Therapeutic targeting of the interleukin-6 receptor. Annu. Rev. Pharmacol. Toxicol. 52, 199–219 (2012).
Waldner, M.J. & Neurath, M.F. Master regulator of intestinal disease: IL-6 in chronic inflammation and cancer development. Semin. Immunol. 26, 75–79 (2014).
Pflugfelder, S.C., Corrales, R.M. & de Paiva, C.S. T helper cytokines in dry eye disease. Exp. Eye Res. 117, 118–125 (2013).
Kumar, P. & Subramaniyam, G. Molecular underpinnings of Th17 immune-regulation and their implications in autoimmune diabetes. Cytokine 71, 366–376 (2014).
Kang, M.H., Kim, M.K., Lee, H.J., Lee, H.I., Wee, W.R. & Lee, J.H. Interleukin-17 in various ocular surface inflammatory diseases. J. Korean Med. Sci. 26, 938–944 (2011).
Penel-Sotirakis, K., Simonazzi, E., Peguet-Navarro, J. & Rozieres, A. Differential capacity of human skin dendritic cells to polarize CD4+ T cells into IL-17, IL-21 and IL-22 producing cells. PLoS One 7, e45680 (2012).
Guo, X. et al. Induction of innate lymphoid cell-derived interleukin-22 by the transcription factor STAT3 mediates protection against intestinal infection. Immunity 40, 25–39 (2014).
Korn, L.L. et al. Conventional CD4+ T cells regulate IL-22-producing intestinal innate lymphoid cells. Mucosal Immunol. 7, 1045–1057 (2014).
Sabat, R., Ouyang, W. & Wolk, K. Therapeutic opportunities of the IL-22-IL-22R1 system. Nat. Rev. Drug Discov. 13, 21–38 (2014).
Wolk, K., Kunz, S., Witte, E., Friedrich, M., Asadullah, K. & Sabat, R. IL-22 increases the innate immunity of tissues. Immunity 21, 241–254 (2004).
Lee, H.K., Ryu, I.H., Seo, K.Y., Hong, S., Kim, H.C. & Kim, E.K. Topical 0.1% prednisolone lowers nerve growth factor expression in keratoconjunctivitis sicca patients. Ophthalmology 113, 198–205 (2006).
Shim, J. et al. Change in prostaglandin expression levels and synthesizing activities in dry eye disease. Ophthalmology 119, 2211–2219 (2012).
Seo, Y. et al. Activation of HIF-1alpha (hypoxia inducible factor-1alpha) prevents dry eye-induced acinar cell death in the lacrimal gland. Cell Death Dis. 5, e1309 (2014).
Ji, Y.W. et al. Dry eye-induced CCR7+CD11b+ cell lymph node homing is induced by COX-2 activities. Invest. Ophthalmol. Vis. Sci. 55, 6829–6838 (2014).
Lee, J.H., Kim, M., Im, Y.S., Choi, W., Byeon, S.H. & Lee, H.K. NFAT5 induction and its role in hyperosmolar stressed human limbal epithelial cells. Invest. Ophthalmol. Vis. Sci. 49, 1827–1835 (2008).
Lee, J.H., Kim, J.W., Im, Y.S., Seong, G.J. & Lee, H.K. Cyclosporine A induces nerve growth factor expression via activation of MAPK p38 and NFAT5. Cornea 30, S19–S24 (2011).
Acknowledgements
We thank Hyeon Chang Kim, MD, PhD (Department of Preventive Medicine, Yonsei University College of Medicine, Seoul, Korea) for excellent discussion that assisted in statistical analysis and Hyeong-jae Jeong, MT (Department of Pathology, Yonsei University College of Medicine, Seoul, Korea) for assistance in the preparation of histological specimens of LGs and corneoconjunctival tissues. This work was supported in part by grants from the Korea Health Industry Development Institute (HI13C0055 to H.K.L.) and National Institute of Health (EY024602 to S.K.C.).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Additional information
Author contributions
Y.W.J. designed the study, collected the patients’ tear samples, performed animal experiments, and wrote the manuscript. S.K.M. assisted in designing experiments, analyzed the data, and wrote the manuscript. H.S.H. collected patients’ tear samples. E.J.C. performed LC-MS/MS experiments and assisted in molecular experiments. J.H.L. helped to design and conceive of the in vivo study. Y.S. performed immunostaining experiments. A.Y. performed flow cytometry and molecular experiments. H.N. managed and generated all animal models. H.S.L. assisted in statistical analysis of data. S.K.C. and H.K.L. designed the study, analyzed data, interpreted the results, and wrote and reviewed this manuscript.
SUPPLEMENTARY MATERIAL is linked to the online version of the paper
Supplementary information
Rights and permissions
About this article
Cite this article
Ji, Y., Mittal, S., Hwang, H. et al. Lacrimal gland–derived IL-22 regulates IL-17-mediated ocular mucosal inflammation. Mucosal Immunol 10, 1202–1210 (2017). https://doi.org/10.1038/mi.2016.119
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2016.119
This article is cited by
-
Amplified fluorogenic immunoassay for early diagnosis and monitoring of Alzheimer’s disease from tear fluid
Nature Communications (2023)
-
Mucosal immunology of the ocular surface
Mucosal Immunology (2022)
-
Mass spectrometry analysis of human tear fluid biomarkers specific for ocular and systemic diseases in the context of 3P medicine
EPMA Journal (2021)
-
Review of Biomarkers in Ocular Matrices: Challenges and Opportunities
Pharmaceutical Research (2019)
-
The mouse autonomic nervous system modulates inflammation and epithelial renewal after corneal abrasion through the activation of distinct local macrophages
Mucosal Immunology (2018)