Abstract
The identification of intestinal macrophages (mφs) and dendritic cells (DCs) is a matter of intense debate. Although CD103+ mononuclear phagocytes (MPs) appear to be genuine DCs, the nature and origins of CD103− MPs remain controversial. We show here that intestinal CD103−CD11b+ MPs can be separated clearly into DCs and mφs based on phenotype, gene profile, and kinetics. CD64−CD103−CD11b+ MPs are classical DCs, being derived from Flt3 ligand-dependent, DC-committed precursors, not Ly6Chi monocytes. Surprisingly, a significant proportion of these CD103−CD11b+ DCs express CCR2 and there is a selective decrease in CD103−CD11b+ DCs in mice lacking this chemokine receptor. CCR2+CD103− DCs are present in both the murine and human intestine, drive interleukin (IL)-17a production by T cells in vitro, and show constitutive expression of IL-12/IL-23p40. These data highlight the heterogeneity of intestinal DCs and reveal a bona fide population of CCR2+ DCs that is involved in priming mucosal T helper type 17 (Th17) responses.
Similar content being viewed by others
INTRODUCTION
The intestine is constantly exposed to many antigens and innate immune stimuli, including dietary constituents, commensal bacteria, and pathogens.1 The intestinal immune system must discriminate between these different agents, mounting protective immunity against pathogens, but developing active tolerance to harmless materials. If this process fails, inappropriate responses can lead to inflammatory bowel diseases and celiac disease. Mononuclear phagocytes (MPs) in the lamina propria (LP) such as dendritic cells (DCs) and macrophages (mφs) are central to these events, serving distinct, yet complementary functions. Whereas DCs migrate to draining lymph nodes and prime naive T cells,2, 3, 4, 5 mφs are sessile phagocytes that scavenge bacteria and damaged cells. They also maintain the expansion of antigen-specific regulatory T cells through the production of interleukin-10 (IL-10)6, 7 and promote epithelial barrier integrity.8
Because of their distinct functions, it is likely that mucosal DCs and mφs play different roles in disease, meaning they need to be characterized as precisely as possible. However, this has been the source of much confusion and controversy,4, 9, 10, 11, 12, 13, 14 largely because many of the phenotypic markers used to discriminate DCs and mφs are insufficiently specific. Initial studies defined intestinal DCs simply on the basis of CD11c and major histocompatibility complex II (MHCII) coexpression, but most if not all mφs in the mucosa also express these markers.3, 10, 13, 15, 16 More recent work has used CD103, CD11b, and CX3CR1 expression to identify three major populations of CD11c+MHCII+ MPs. Two of these express CD103, lack CX3CR1, and are either CD11b+ or CD11b−.3, 5, 17, 18 Based on their derivation from DC-committed precursors (pre-DCs) and genetic profiles, it is generally agreed that these CD103+ MPs are bona fide DCs.11, 19, 20 The third population of CD103−CD11b+ MPs is less well understood. Although they express CX3CR1,5, 16, 21 and were originally considered to be monocyte-derived DCs,19, 20 recent transcriptional analyses suggest they are more similar to mφs than DCs.9, 11 However, we recently identified CD103−CD11b+CX3CR1int cells migrating in pseudoafferent lymph that are bona fide CD103− DCs, based on their responsiveness to Flt3 ligand (Flt3L) and lack of mφ markers such as F4/80 or CD64 ( ref. 5 and our unpublished observations). Although analogous cells have been described in steady-state LP,5, 16, 22, 23 confusion remains over the relative contribution of DCs and mφs to the CD103−CD11b+ LP population and their developmental origin remains contentious. In previous work, we found that Ly6Chi monocytes could not generate CD103+ or CD103− subsets of bona fide DCs in steady-state colon.16, 24 However, a more recent study suggested that CD103− DCs in the mucosa are indeed monocyte derived, on the basis that their accumulation and/or development involves a CCR2-dependent precursor.23
Here, we identify a population of genuine CD103− DCs in the LP that are phenotypically, genetically, and kinetically distinct from mφs. Similar to their CD103+ counterparts, these CD103− DCs arise from Flt3L-dependent, DC-committed precursors and not from Ly6chi monocytes. Significantly, we also demonstrate the presence of CCR2-expressing CD103−CD11b+ DCs in the murine and human LP that have a selective ability to prime IL-17a-producing CD4+ T cells in vitro. The existence of this novel subset of bona fide DCs may help explain previous conflicting results and provide insights into functional compartmentalization among mucosal DC populations.
RESULTS
Expression of F4/80 and CD64 defines two distinct CD103−CD11b+ mononuclear phagocyte populations in intestinal LP
To begin to determine the origins of CD103− MPs in the small intestinal (SI) LP, we first set out to establish a gating strategy that would allow accurate discrimination between CD103− DCs and mφs. After first identifying intestinal MPs as CD11c+MHCII+ cells among live leukocytes, we found three discrete populations based on CD103 and CD11b expression; a majority population of CD103−CD11b+ cells, together with smaller numbers of CD103+CD11b+ and CD103+CD11b− cells (Figure 1a). A small population of CD103−CD11b− cells was also identified, but as these may derive from isolated lymphoid follicles, rather than the LP itself,5 we did not examine them further. To distinguish between DCs and mφs, MPs were next examined for expression of the pan-mφ marker F4/80, together with CD64 that has recently been described to be specific for mφs in the intestine.16, 24 Consistent with the general consensus that CD103+ MPs are classical DCs,3, 4, 18, 19, 20, 25 none of the CD103+ MPs expressed either F4/80 or CD64 (Figure 1a). In contrast, the CD11c+MHCII+CD103−CD11b+ cells were heterogeneous. Although ∼85% of this population were F4/80+CD64+ mφs, the remainder were entirely negative for both CD64 and F4/80, suggesting they may be DCs (Figure 1a,b). Identical subsets of CD64+ and CD64− MPs were present in steady-state colonic LP, although in different proportions, with the CD103+CD11b− and CD103−CD11b+ subsets both outnumbering the CD103+CD11b+ DCs in this tissue (Supplementary Figure S1a-c online). Interestingly, there was an inverse correlation between the proportions of CD103+CD11b+ DCs and CD64+ mφs throughout the length of the small and large intestine, whereas the proportions of the other DC subsets were not significantly different between the various segments of the small intestine, before increasing in the colon (Supplementary Figure S1b,c). All CD64− subsets could also be identified among migratory CD11c+MHCIIhi MPs in the steady-state mesenteric lymph nodes (MLNs), whereas CD64+ MPs were virtually absent (Supplementary Figure S1d,e).
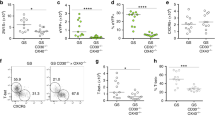
CD64−CD103−CD11b+ intestinal mononuclear phagocytes (MPs) are bona fide dendritic cells (DCs). (a) Intestinal MPs were defined as CD11c+MHCII+ cells among live CD45+ lamina propria cells, analyzed for CD103 and CD11b expression, and the resulting populations of MP were examined for CD64 and F4/80 expression. (b) Proportions of MP populations among total CD11c+MHCII+ cells. Data are representative of at least 15 independent experiments with n=3/4 per experiment. (c) Small intestinal lamina propria (SI LP) MP populations were fluorescence-activated cell sorter (FACS)-purified and Zbtb46 expression assessed by real-time PCR. The results shown are expressed relative to HPRT using the 2−ΔΔct method with macrophages (mφs) set to 1 and are pooled from 2 independent experiments with cells pooled from 9 to 12 mice on each occasion. (d) Total SI LP digests were incubated at 37 °C or 4 °C with pHrodo Escherichia coli bioparticles for 15 min and assessed for phagocytic ability. Bar chart shows mean ΔMFI (MFI 37 °C–MFI 4 °C)+1 s.d., n=4. MFI, mean fluorescence intensity. ***P<0.001 vs. mφs, one-way analysis of variance (ANOVA) with Bonferroni posttest. (e) Expression of CD272, CD26, MerTK, CD14, and CX3CR1 on SI LP MP populations (colored) compared with appropriate background controls (shaded gray). (f) Populations of SI LP MP as a proportion of total live leukocytes in wild-type (WT) and Flt3L−/− mice. Data are pooled from two independent experiments. ***P<0.005, Student’s t-test. (g, h) Mice received one injection of 1 mg ml−1 5-bromodeoxyuridine (BrdU) intraperitoneally (i.p.), followed by 0.8 mg ml−1 BrdU in the drinking water for 3 days, before being returned to normal drinking water. Mice were culled immediately following cessation of BrdU feeding, or 3 or 9 days later and MP subsets identified in (g) SI LP and among migratory DCs in the (h) mesenteric lymph nodes (MLNs). Data are the proportions of BrdU+ cells among each subset and are representative of two independent experiments with n=3/4 per time point. Black asterisks represent significant differences between D3 and D3+9 for all DC populations, whereas colored asterisks represent significant differences between D3 and D3+3 in MLNs. ***P<0.001, **P<0.01, *P<0.05 Student’s t-test. NS, nonsignificant.
CD64−CD103−CD11b+ MPs are bona fide DCs
To clarify further the nature of the CD103−CD11b+ cells, we examined other features that define DCs and mφs. Unlike the CD64+ mφs, all subsets of CD64− MPs, including the CD103−CD11b+ cells, expressed mRNA for the DC-specific transcription factor Zbtb46 (Figure 1c)26, 27 and were not phagocytic as assessed by the ability to take up bacterial particles into acidified vesicles (Figure 1d). Whereas all the CD64+F4/80+CD103−CD11b+ mφs expressed the mφ-specific markers MerTK and CD14,9, 11 the CD64−F4/80−CD103−CD11b+ MPs lacked expression of these markers, as did the prototypic CD103+ DCs. Conversely, CD64−F4/80−CD103−CD11b+ MPs expressed the recently defined DC-specific markers CD26 and CD272, whereas CD64+F4/80+CD103−CD11b+ MPs did not (Figure 1e). Consistent with previous studies,3, 16, 18, 21, 24, 28 CX3CR1 was expressed at high or intermediate levels on CD64+F4/80+CD103−CD11b+ mφs, but was absent from CD103+ DCs (Figure 1e). However, the CD64−CD103−CD11b+ MPs within the mucosa all expressed intermediate levels of CX3CR1 (Figure 1e), consistent with the CD103−CD11b+ DCs we identified recently in pseudoafferent intestinal lymph.5
Finally, we examined the dependence of the different MP subsets on the DC-specific growth factor Flt3L.29, 30 As expected, normal numbers of CD11c+CD64+ mφs were present in the intestine of Flt3L−/− mice (Figure 1f). In contrast, all CD11c+CD64− subsets including the CD64−CD103−CD11b+ MPs were dramatically reduced in the LP of Flt3L−/− mice compared with wild-type (WT) controls (Figure 1f). Taken together, these data confirm the presence of bona fide CD103−CD11b+ DCs in the steady-state LP.
Intestinal DCs divide in situ and turn over rapidly in the steady state
Previous work has shown that intestinal mφs and CD103+ DCs have distinct population dynamics in vivo.3, 18 However, these studies considered all CD103−CD11b+ MPs to be mφs. Having now identified bona fide CD103−CD11b+ DCs in LP, we used 5-bromodeoxyuridine (BrdU) pulsing to determine their population dynamics compared with mφs and CD103+ DCs in vivo.
To examine this, BrdU was administered continuously for 3 days and its incorporation was assessed immediately after its withdrawal and again 9 days thereafter. After 3 days of BrdU feeding, a substantial majority (70–85%) of both subsets of CD103+ DCs was BrdU+, whereas only 15–25% of CD64+ mφs had been labeled at this time (Figure 1g). Importantly, CD103−CD11b+ DCs displayed BrdU labeling identical to the CD103+ DC subsets and very distinct from CD64+ mφs (Figure 1g). At 9 days after BrdU withdrawal, the proportion of BrdU+ cells among all CD64− DC subsets had decreased to <10%, whereas the proportion of BrdU+ CD64+ mφs remained steady, indicating relative longevity compared with DCs (Figure 1g). In contrast to LP, where maximal BrdU labeling was achieved upon BrdU withdrawal at day 3, only 30–50% of the CD64−CD103+ and CD103− populations among the CD11c+MHCIIhi migratory cells in MLNs were BrdU+ at this time (Figure 1h). The frequency of BrdU+ cells among migratory DCs in the MLNs increased further 72 h after BrdU withdrawal, consistent with migration of BrdU+ cells from the LP. Consistent with the short lifespan of DCs, only 15–20% of MLN DCs remained BrdU+ 9 days after BrdU+ withdrawal. Resident CD11c+MHCIIint DCs in MLNs had a distinct BrdU profile, achieving maximal labeling before withdrawal of BrdU (data not shown).
CD103−CD11b+ intestinal DCs arise from committed DC precursors
Previous studies that did not take the heterogeneity of CD103−CD11b+ MPs into account suggested that they were derived exclusively from Ly6Chi monocytes.19, 20, 31 Thus, we next investigated the origin of the bona fide CD103−CD11b+ DCs, first by adoptive transfer of Ly6Chi monocytes from CX3CR1+/gfp mice into monocytopenic CCR2−/− mice (Supplementary Figure S2a,b). At 5 days after transfer, donor Ly6Chi monocytes and their progeny could be identified in the SI LP by their expression of CD45.1 and CX3CR1-GFP. At this time, all donor cells were CD11c+MHCII+F4/80+, with none being found within the CD11c+F4/80− DC gate (Figure 2a). Furthermore, no progeny of transferred Ly6Chi monocytes could be found in the MLNs (data not shown). Thus, in our hands, Ly6Chi monocytes cannot act as progenitors for rigorously defined CD103− DCs in the steady-state intestine, nor can monocyte-derived MPs migrate to the MLNs from the LP under these conditions.
CD64−CD103−CD11b+ dendritic cells (DCs) arise from DC-committed precursors. (a) 1 × 106 Ly6Chi monocytes sorted from the bone marrow (BM) of CX3CR1+/GFP CD45.1+ × CD45.2+ mice were transferred into resting CCR2−/− CD45.2+ recipients. After 5 days, donor-derived cells were identified among live small intestinal lamina propria (SI LP) cells as CD45.1+CX3CR1-GFP+ and examined for expression of CD11c, MHCII, and F4/80. Data are representative of two recipient mice from a single experiment. (b) CD45.2+ wild-type (WT) mice were injected with 2 × 106 Flt3 ligand (Flt3L)-secreting B16 tumor cells. After 10–14 days, DC precursors (pre-DCs) were fluorescence-activated cell sorter (FACS)-sorted, labeled with CellTrace Violet proliferation dye, and transferred intravenously (i.v.) into CD45.1+ congenic mice. After 5 days, donor-derived cells were identified among live SI LP cells as CD45.2+CD45.1−CellTrace Violet+ and examined for expression of CD11c, MHCII, and F4/80. (c) Representative CD103 and CD11b staining by CD11c+MHCII+ donor cells in the SI LP compared with endogenous CD11chiMHCII+ cells. (d) Scatter plot shows proportion of CD11c+MHCII+ donor cells in each population defined by CD103 and CD11b expression as gated in c. Data are pooled from three independent experiments with n=10. MHCII, major histocompatibility complex II; PBS, phosphate-buffered saline.
Given their independence from monocytes, we next tested whether CD103−CD11b+ DCs were derived from committed pre-DCs,32, 33, 34 as has been shown for mucosal CD103+ DCs.19, 20 Pre-DCs from bone marrow (Lin−CD11cintCCR9−B220−CD135+SIRPαintCD117−; Supplementary Figure S2b,c) were fluorescence-activated cell sorter (FACS)-purified from CD45.2+ mice that had received B16 tumors secreting Flt3L 10 days earlier, labeled with CellTrace Violet dye, and transferred into unmanipulated, steady-state, congenic CD45.1+ recipients. Donor-derived cells could already be found in the LP 24 h after transfer, at which time most had begun to upregulate both MHCII and CD11c (Supplementary Figure S2d,e). The expression of both these markers then increased progressively until their levels became equivalent to those on endogenous DCs. By 5 days after transfer, most donor cells had acquired MHCII expression and upregulated CD11c, but remained F4/80−, consistent with them being DCs (Figure 2b and Supplementary Figure S2d,e). The transferred pre-DCs not only gave rise to both CD103+CD11b− and CD103+CD11b+ DC populations in LP, but there was also a clear population of CD103−CD11b+ donor-derived cells that lacked F4/80 expression, demonstrating directly that pre-DC can give rise to CD103−CD11b+ DCs (Figure 2c,d). Donor pre-DCs also gave rise to all three DC populations among CD11c+MHCIIhi migratory DCs in the MLNs, as well as in the colonic LP (data not shown).
CD103−CD11b+ DCs are partially dependent on CCR2
Our results indicate that CD64−CD103−CD11b+ intestinal MPs are DCs and are distinct from monocyte-derived mφs. However, a recent study has identified a similar population of CX3CR1intCD11c+MHCII+ MPs in inflamed mucosa that were characterized as monocyte-derived DCs on the basis of their expression of Zbtb46 and CCR2 dependence.23 On this basis it was concluded that some CD103− DCs differentiate from monocytes that require CCR2 for their egress from the bone marrow (BM).35 Therefore, we examined whether deletion of CCR2 affected the abundance of our DC subsets in the steady-state mucosa. Compared with WT controls, CCR2−/− mice had normal proportions and absolute numbers of CD103+ DCs. However, they had a significant reduction in CD64−CD103−CD11b+ DCs in the SI LP, and this was mirrored by a reduction in the CD103− subset of CD11c+MHCIIhi migratory DCs in the MLNs (Figure 3a,b). A small reduction in the number of CD103+CD11b− DCs was also observed among migratory DCs in the MLNs (Figure 3b). The selective CCR2 dependence of CD103−CD11b+ DCs and CD64+ mφs was cell intrinsic, as it was replicated when these populations were derived from CCR2−/− precursors in CD45.1 WT:CD45.2 CCR2−/− mixed BM (Figure 3c). Whereas WT and CCR2−/− BM had a roughly equivalent ability to populate the CD103+ subsets of DCs, comparable with CCR2-independent eosinophils, the repopulation of CD103−CD11b+ DCs was biased toward WT BM, with a WT:CCR2−/− ratio of ∼3 (Figure 3c,d). Similar results were observed for CD103−CD11b+ DCs among migratory DCs in the MLNs of chimeric mice (Figure 3d). Consistent with their dependence on replenishment by CCR2-dependent Ly6Chi monocytes in the steady state,16, 24 there was a substantial reduction in the numbers of CD64+ mφs in CCR2−/− LP and virtually all mφs in the LP of the mixed chimeras were of WT origin, similar to the pattern seen with blood Ly6Chi monocytes (Figure 3a,d).
Partial dependence of CD103−CD11b+ lamina propria (LP) dendritic cells (DCs) on CCR2. (a) Small intestinal (SI) LP DCs from CCR2−/− and wild-type (WT) mice were examined for expression of CD103 and CD11b, with the numbers representing the frequency of each population as a percentage of total CD11c+MHCII+CD64− DCs. MHCII, major histocompatibility complex II. Scatter plot shows absolute numbers of each mononuclear phagocyte (MP) population in SI LP of CCR2−/− and WT mice. (b) Migratory (Mig.) mesenteric lymph node (MLN) DCs from CCR2−/− and WT mice were examined for expression of CD103 and CD11b, with the numbers representing the frequency of each population as a percentage of total mig. DCs. Scatter plot shows absolute numbers of each mig. DC population in the MLNs of CCR2−/− and WT mice. Data are representative of two independent experiments with n=3/4 per experiment *P<0.05, **P<0.005, Student’s t-test. (c) CD45.1+/CD45.2+ WT mice were lethally irradiated and reconstituted with a 50:50 mix of bone marrow (BM) from CD45.1+ WT and CD45.2+ CCR2−/− mice. Chimerism among the populations of CD11c+MHCII+ MPs from SI LP was assessed 8 weeks later. (d) Ratio of CD45.1 WT:CD45.2 CCR2−/−-derived cells among CD11c+MHCII+ MPs and eosinophils from SI LP, blood Ly6Chi monocytes (mo), and migratory DCs in the MLNs of chimeric mice. ***P<0.001 vs. macrophages (mφs), one-way analysis of variance (ANOVA) with Bonferroni posttest. Data are representative of two independent experiments with n=3 per experiment.
Two populations of CD103−CD11b+ intestinal DCs can be defined by CCR2 expression
We reasoned that this partial dependence on CCR2 could reflect heterogeneity among the CD103−CD11b+ subset of DCs and therefore analyzed CCR2 expression by the DC subsets in SI LP. Whereas CD103+ DCs were mainly CCR2−, there were two clear populations of CD103−CD11b+ DCs, with the majority (∼75–85%) being CCR2− and a smaller but distinct fraction being CCR2+ (Figure 4a). Because of this heterogeneity, we thought it important to examine whether pre-DCs could give rise to both CCR2− and CCR2+ CD103−CD11b+ DCs, which had been investigated as a single population in our earlier analyses. As with the endogenous population, CD103−CD11b+ DCs derived from transferred pre-DCs were heterogeneous for CCR2 expression 5 days after transfer, confirming that the CCR2+ DCs were derived from pre-DCs (Figure 4b). FACS-purified CCR2+CD103−CD11b+ DCs also expressed mRNA for Zbtb46 and Flt3 at levels equivalent to CD103+ DCs and their CCR2−CD103− DC counterparts, confirming their DC lineage (Figure 4c). Furthermore, both the CCR2− and CCR2+ subsets of CD103−CD11b+ DCs in the LP expressed mRNA for CCR7 at similar levels to CD103+ DCs, showing they have the potential to migrate out of the mucosa to the MLNs (Figure 4c). Consistent with this, CCR2+CD103−CD11b+ DCs could be identified among migratory DCs in the steady-state MLNs (Figure 4d).
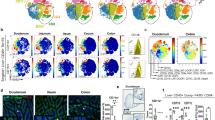
CCR2 expression defines two populations of intestinal CD103−CD11b+ dendritic cells (DCs). (a) Representative CCR2 staining on CD11c+MHCII+CD64− DC populations from small intestinal lamina propria (SI LP) of wild-type (WT) mice, compared with total DCs from CCR2−/− mice as a control. The scatter plot shows the proportion of CCR2+ cells in each SI LP DC population as a percentage of total CD11c+MHCII+CD64− cells, with each point representing a mouse and the horizontal line representing the mean. Data are representative of three independent experiments with n=4 per experiment. (b) Representative CCR2 staining on CD103−CD11b+ DCs among endogenous (CD11c+MHCII+CD64−) and donor-derived (Violet+, CD45.2+, CD11c+, MHCII+) cells in the SI LP 5 days after transfer of CD45.2+ DC precursors (pre-DCs) into unmanipulated CD45.1+ WT recipients. (c) Quantitative PCR (Q-PCR) analysis of mRNA for Zbtb46, Flt3, and Ccr7 by CCR2+ and CCR2− subsets of CD103−CD11b+ DCs fluorescence-activated cell sorter (FACS)-purified from the SI LP of WT mice, compared with CD103+ DC subsets and CD64+ macrophages (mφs). Data are from a single experiment with 10 mice pooled and are expressed relative to HPRT using the 2−ΔΔct method with mφs set to 1. (d) Representative CCR2 staining on subsets of DCs among CD11c+MHCIIhi migratory (Mig.) DCs in wild-type mesenteric lymph nodes (MLNs), and in total migratory DCs from CCR2−/− mice used as a control. Scatter plot shows the proportion of CCR2+ cells in each SI LP DC population among total CD11c+MHCII+CD64− cells, with each point representing a mouse and the horizontal line representing the mean. Data are representative of two independent experiments with n=4 per experiment.
CCR2+ and CCR2− CD103−CD11b+ intestinal DCs are functionally distinct
Having identified two distinct populations of CD103−CD11b+ DCs based on their expression of CCR2, we next sought to determine the functional consequences of this heterogeneity. Thus, SI LP DC subsets were FACS-purified, pulsed with ovalbumin protein, and cocultured with carboxyfluorescein succinimidyl ester-labeled, ovalbumin-specific T-cell receptor transgenic naive CD4+ T cells. All DC subsets, including the CCR2+ and CCR2− populations of CD103−CD11b+ DCs, induced similar levels of OTII T-cell proliferation, as assessed by carboxyfluorescein succinimidyl ester dilution (Figure 5a–c). The two subsets of CD103+ DCs generated regulatory T cells in vitro as determined by intracellular expression of FoxP3 (forkhead box P3) and this appeared to be somewhat more efficient than either of the CCR2+ and CCR2− subsets of CD103−CD11b+ DCs that had similar activity (Figure 5a). CD103+CD11b− DCs induced the differentiation of considerably more interferon-γ-producing CD4+ T cells than all other DC subsets; there were no differences between the CD103+CD11b+ DCs and the CCR2+ or CCR2− subsets of CD103−CD11b+ DCs in this respect (Figure 5b). However, the CCR2+CD103−CD11b+ DCs were more effective than the other subsets at driving the differentiation of helper type 17 (Th17) cells in vitro (Figure 5c). Notably, this property within the CD103−CD11b+ DCs was masked when they were compared with other subsets as a single population (data not shown).
CCR2-expressing CD103−CD11b+ intestinal dendritic cells (DCs) drive T helper type 17 (Th17) responses. 3 × 104 Fluorescence-activated cell sorter (FACS)-purified DC subsets from small intestinal lamina propria (SI LP) were pulsed with 2 mg ml−1 ovalbumin (OVA) protein and cocultured for 4 days with 1 × 105 FACS-purified naive carboxyfluorescein succinimidyl ester (CFSE)-labeled OTII T cells. (a) Forkhead box P3 (FoxP3), (b) interferon-γ (IFNγ), and (c) interleukin-17a (IL-17a) expression by live T cells was assessed by intracellular staining. Scatter plots show fold change in (a) FoxP3, (b) IFNγ, and (c) IL-17a production induced by each DC population compared with that induced by CCR2−CD103−CD11b+ DCs. Mean values (+1 s.d.) for the CCR2− DCs were 0.341% (0.181), 1.051% (0.798), and 0.291% (0.09) among total CD4+ T cells for FoxP3, IFNγ, and IL17a expression, respectively. Data are shown as mean±1 s.d. pooled from three independent experiments. *P<0.05, **P<0.01, ***P<0.001, one-way analysis of variance (ANOVA) with Bonferroni posttest. (d, e) Whole SI LP digests were incubated for 4.5 h in the presence (+lipopolysaccharide (LPS)) or absence (unstimulated (Unstim.)) of 100 ng ml−1 LPS with brefeldin A and monensin. Scatter plot shows percentage of (d) IL-6+ or (e) IL-12/IL-23p40+ cells among CCR2− or CCR2+CD103−CD11b+ DCs assessed by intracellular cytokine staining. *P<0.05, **P<0.01, ***P<0.001 vs. CCR2+CD103−CD11b+ DCs. Data are representative of one or two independent experiments with n=3/4 per experiment.
Efficient generation of Th17 cells by the CCR2+ subset of CD103−CD11b+ DCs is associated with higher frequency of IL-12/IL23p40 producing cells
In an attempt to understand why CCR2+CD103−CD11b+ DCs were effective in priming Th17 cells, we examined their production of Th17-polarizing cytokines. Intracellular cytokine staining showed that there were ample proportions of IL-6-producing cells among all DC subsets under steady-state conditions and, if anything, these were slightly lower for the CCR2+CD103−CD11b+ DCs than the CCR2−CD103−CD11b+ or CD103+CD11b+ subsets (Figure 5d and data not shown). However, the CCR2+CD103−CD11b+ population was the only one in SI LP to contain IL-12/IL-23p40-producing DCs under steady-state conditions, as well as showing the most robust increase in the frequency of IL-12/IL-23p40-producing cells in response to Toll-like receptor 4 stimulation. Under these conditions, ∼30% IL-12/IL-23p40+ DCs were found within this subset, compared with ∼10% in other subsets (Figure 5e). Toll-like receptor 4 stimulation had no effect on the already high frequencies of IL-6-producing cells among any subset (Figure 5d). Given that the CCR2-expressing CD103−CD11b+ DCs did not show any difference in their ability to prime Th1 responses, these findings indicate that their preferential effect on Th17 cells may be explained most readily by an enhanced ability to produce IL-23.
CCR2+CD103−CD11b+ LP DCs both express and are dependent on the transcription factor IRF4
A defining feature of the CD11b+ lineage of conventional DCs in mice is dependence on the interferon regulatory factor 4 (IRF4) transcription factor for their development,22, 25, 36, 37, 38, 39 and we and others have shown recently that lack of IRF4 expression in CD11c+ cells leads to a selective defect in CD103+CD11b+ intestinal DCs that correlates with impaired Th17 responses in vivo.22, 36 As these results appear to contrast with our discovery of a CCR2+ subset of CD103−CD11b+ DCs that is more efficient in inducing Th17 cell differentiation than the other subsets, we thought it important to assess how IRF4 might control their development. Similar to CD103+CD11b+ DCs in LP, both the CCR2+ and CCR2− subsets of CD103−CD11b+ DCs expressed IRF4, but not IRF8 (Figure 6a). Conversely, and as expected, the CD103+CD11b− DCs showed the opposite pattern, expressing IRF8, but not IRF4 (Figure 6a). As we found previously, CD11c-cre x IRF4fl/+ mice had a substantial decrease in the numbers and proportions of CD103+CD11b+ DCs in SI LP and, interestingly, these animals also showed a significant defect in the CCR2+ subset of CD103−CD11b+ DCs (Figure 6b). In contrast, CD103+CD11b− and CCR2−CD103−CD11b+ DCs were unaffected in CD11c-cre × IRF4fl/+ LP. Thus, the loss of CCR2+CD103−CD11b+ DCs may contribute to the defective Th17 cell generation in these mice.
CCR2+CD103−CD11b+ dendritic cells (DCs) express interferon regulatory factor 4 (IRF4) and require it for their existence in the lamina propria (LP). (a) DCs in the small intestinal (SI) LP were examined for their intracellular expression of IRF4 and IRF8 and compared with isotype controls. (b) Representative fluorescence-activated cell sorter (FACS) plots and mean proportions and numbers of DC subsets in the SI LP of CD11c-cre− × IRF4Fl/+ (CRE−) or CD11c-cre+ × IRF4Fl/+ (CRE+) mice. *P<0.05, **P<0.01, ***P<0.001 Student’s t-test. Data are representative of 2–3 independent experiments with n=3–6 per experiment.
Putative CCR2-expressing CD103− DC equivalents in the human intestine
Having identified CCR2+CD103−CD11b+ DCs in the murine intestine, we next sought to determine whether equivalent cells were present in the human intestinal LP. By excluding CD14+CD64+ cells that represent mφs,24 DCs were readily identifiable in human colonic LP among live CD45+CD11c+HLA-DR+ cells (Figure 7). As in mouse LP, examination of CD103 and SIRPα expression identified three distinct populations of human DC populations and the CD103−SIRPα+ DCs were heterogeneous for CCR2 expression (Figure 7). Thus, the CCR2-based heterogeneity of CD103− mucosal DCs is maintained across species.
Putative CCR2+CD103−CD11b+ dendritic cell (DC) equivalents exist in healthy human colonic lamina propria (LP). DCs were identified in healthy human colon as live, CD45+, CD14−, CD64−, CD11c+, and HLA-DR+ and expression of CD103 and SIRPα was assessed. CD103−SIRPα+ DCs were then examined for CCR2 expression compared with CCR2 isotype control. Data are representative of two independent experiments.
DISCUSSION
The nature and origins of intestinal DCs have been contentious for several years. Although the presence of two CD103+ DC subsets based on CD11b expression has been recognized for some time and they are generally accepted to be conventional DCs,3, 17, 19, 20, 40, 41, 42 the existence of genuine CD103− DCs among CD11c+MHCII+ MPs has been less certain. Initially considered to be proinflammatory “DCs”,19, 20, 43 later studies defined CD103−CD11b+ MPs as mφs, on the assumption that CD103 and CX3CR1 were mutually exclusive markers of DCs and mφs, respectively.3 Here, we demonstrate that more rigorous strategies reveal heterogeneity within this population in the steady-state intestine. In addition to confirming recent findings that the majority of CD103−CD11b+ express the mφ markers CD64 and F4/80,16, 22, 24, 44 we show definitively that a population of CD64−CD103−CD11b+ DCs is present in steady-state LP. A similar subset can be found in pseudoafferent intestinal lymph.44 Similar to their CD103+ counterparts, the CD103−CD11b+ DCs in LP expressed Zbtb46,26, 27 as well as CD26 and CD272, markers identified by the Immunological Genome Consortium as being specific to DCs.11 Conversely, they lacked the mφ-restricted markers CD14 and MerTK,9 and showed poor phagocytic activity compared with CD64+ mφs. Importantly, the CD64−CD103− DCs expressed Flt3 and were virtually absent in the LP of Flt3L−/− mice. The CD103−CD11b+ DCs also had a short half-life in vivo and showed evidence of proliferation in situ, properties identical to DCs in other peripheral tissues25 and to their CD103+ counterparts in the SI LP. In stark contrast, CD64+CD103−CD11b+ mφs were long-lived and noncycling.
Our studies using adoptively transferred precursors underlined the heterogeneity of intestinal CD103− MPs, by demonstrating that CD103−CD11b+ intestinal DCs derived from DC-committed precursors. This contrasts with previous reports that concluded that CD103− “DCs” were derived from Ly6Chi monocytes. However, these studies used less precise phenotyping strategies and used intense depletion of endogenous myeloid cells that may alter the fate of donor cells and their progeny.19, 20, 21, 23 In our hands, Ly6Chi monocytes were unable to generate CD103−CD11b+ DCs and gave rise only to F4/80+ mφs in healthy mucosa. Because we were limited by the numbers of monocytes available for transfer, we cannot exclude the possibility that some genuine DCs might arise if there is expanded entry of monocytes into the mucosa. However, our studies suggest that this is likely to be a rare event under steady-state conditions. In contrast, pre-DCs could clearly give rise to all populations of DCs, including the novel CCR2+CD103−CD11b+ subset we identified. Whether these distinct subsets arise from the same or multiple subsets of these progenitors remains unclear. A recent study has suggested that β7 integrin-expressing DC precursors had a preferential ability to repopulate mucosal CD103+ DCs,45 but it is currently unclear how these “pre-mucosal” DCs relate to the pre-DCs used here and in other studies.34, 45 Although our transferred pre-DCs lacked the B220 expression reported on the “pre-mucosal” DCs, a proportion were β7+ (our unpublished observations) and therefore some progenitors with selective gut-homing properties may be present in our populations. How these β7+ precursors specifically contribute to intestinal DC populations remains to be investigated. The idea that there might be independent precursors of each DC subset could explain why the proportions of donor-derived DCs in the intestine did not always mimic those found among host DCs at different times after transfer, as each lineage may develop at different rates. Alternatively, these time-dependent differences might reflect developmental relationships within the same lineage and these issues will be the subject of future investigations.
At first sight, our conclusions that all mucosal DCs derive from pre-DCs appear to contradict a recent study by Zigmond et al.,23 in which a population of mucosal Ly6CloCD11b+Zbtb46+ cells, likely to comprise our CD103− DCs, was depleted by in vivo administration of anti-CCR2 antibody. As a result, it was concluded that these DCs were derived from CCR2-dependent Ly6Chi monocytes. An explanation for this apparent discrepancy comes from our discovery of a population of pre-DC-derived, CCR2-expressing CD103−CD11b+ DCs that have all the properties of the other bona fide DCs in LP and are found among migratory DC populations in the MLNs. Importantly, CCR2-deficient mice displayed a selective reduction in the numbers of CD103−CD11b+ DCs and this was intrinsic to the DCs, as it was replicated among the progeny of CCR2−/− BM in mixed WT:CCR2−/− BM chimeras.
Similar to CD103+ DCs, CD103−CD11b+ DCs efficiently induced the proliferation of antigen-specific CD4+ T cells after antigen loading ex vivo. Significantly, the CCR2-expressing CD103−CD11b+ DCs induced the polarization of Th17 cells in vitro, a function previously associated with CD103+CD11b+ DCs. This idea was based on evidence from mice lacking IRF4, Notch-2, or human langerin in CD11c+ cells that showed concomitant, selective defects in CD103+CD11b+ DCs and Th17 cells in the intestine.22, 36, 46, 47 Importantly, our novel population of Th17-inducing, CCR2+CD103−CD11b+ DCs expressed IRF4 and their numbers were reduced in CD11c-cre-IRF4fl mice, suggesting that this previously unrecognized subset could contribute to the impairment of Th17 cell generation in these animals. Indeed, a very recent study has demonstrated that the role of CD103+CD11b+ DCs in Th17 cell homeostasis in the LP may be to act as an accessory cell, rather than to interact with T cells in a cognate manner.47 More work is clearly warranted to explore how these various subsets of DCs may cooperate in the priming of T-cell responses in vivo. The presence of apparently intrinsically proinflammatory cells among the CD103− DC population could also help explain why CD103− “DCs” were often previously associated with inflammation when less well-defined cell populations were used.43, 48 Finally, it should be noted that CD103−CD11b+ DCs have been shown to drive Th17 polarization in other tissues such as the lung.22 As the expression of CD103 by CD11b+ DCs is unique to the intestine, it remains possible that the Th17-polarizing CCR2+CD103−CD11b+ DCs we have identified are intermediate stages within the development of CD103+CD11b+ DCs, whose ultimate differentiation involves the loss of CCR2 and acquisition of CD103, perhaps following their conditioning by the intestinal microenvironment.49
Although previous studies have correlated the ability of intestinal DCs to prime Th17 cells with their production of IL-6,36 we found similar frequencies of IL-6-producing cells among CCR2− and CCR2+CD103− DCs. However, the CCR2-expressing DCs included more cells containing intracellular IL-12/IL-23p40, both in steady state and even more markedly after Toll-like receptor 4 ligation in vitro. As there were no differences in the ability of the various subsets of CD103−CD11b+ DCs to prime Th1 responses in vitro, we propose that the increased levels of IL-12/IL-23p40 in the CCR2-expressing CD103−CD11b+ DCs reflect enhanced production of IL-23 and that this explains their Th17-polarizing properties. However, the difficulties associated with obtaining high numbers of DCs when cultured alone, together with the current lack of a mouse model that lacks CCR2+CD103−CD11b+ DCs specifically, mean that further work is required to confirm this hypothesis directly.
The potential clinical implications of our results are highlighted by our finding of similar heterogeneity of CCR2 expression among CD103− SIRPα+ DCs in steady-state human intestine, a population that appears to be equivalent to CD103−CD11b+ DCs in mice.22 It will be of interest to examine the function of this subset particularly in disorders associated with Th17 cells such as Crohn’s disease. Furthermore, our results showing that CCR2 dependence is not a reliable indicator of monocytic origin and that DCs and mφs are truly derived from distinct precursors raise important issues that need to be considered in the clinical situations where monocyte-derived cells and myeloid cell growth factors are being trialed.
In conclusion, we show definitively that CD103−CD11b+ MPs in the murine intestinal LP include a population of genuine DCs that are derived exclusively from DC-committed precursors, rather than Ly6Chi monocytes as previously assumed. This subset of DCs is itself heterogeneous, containing a population of CCR2-expressing DCs with proinflammatory properties. These results provide novel insights that may help explain recent discrepancies on the origins and nature of CD103−CD11b+ MPs. An analogous subset is present in human intestine, indicating that this heterogeneity of DCs may be relevant across species barriers.
METHODS
Mice and human tissues. WT C57Bl/6 (B6) mice were purchased from Harlan Olac (Bicester, UK). CX3CR1+/gfp mice50 and C57Bl/6.SJL (CD45.1+) mice were bred originally at Lund University (Lund, Sweden). CCR2−/− mice51 mice were obtained from Professor R. Nibbs (University of Glasgow, Glasgow, UK). OTII mice were bred in-house. All these strains were maintained at the University of Glasgow animal facilities. Flt3L−/−,52 CD11c-cre × IRF4floxed mice,36 and C57Bl/6 WT mice were bred and maintained at the VIB Ghent University (Ghent, Belgium). CD11c-cre × IRF4floxed mice were also bred and maintained at Lund University. All mice were backcrossed for at least 9 generations on to the B6 background, maintained under specific pathogen-free conditions, and were used between 6 and 12 weeks of age. Animal experiments were performed in accordance with UK Home Office guidelines.
Histologically normal samples of human colon were obtained from patients undergoing surgical resections for adenocarcinoma. Tissues were obtained with informed consent and experiments performed in accordance with the NHS Greater Glasgow and Clyde (NHS GGC) Bio-repository ethics application number 65.
Murine cell isolation. LP cells were obtained from murine intestines by enzymatic digestion as described previously.5, 28 Cells were isolated from MLNs by enzymatic digestion with 1 mg ml−1 collagenase D (Roche Diagnostics GmbH, Mannheim, Germany) in calcium magnesium free (CMF) Hank’s balanced salt solution (HBSS; Gibco, Invitrogen, Paisley, UK) for 45 min. After isolation, cells were passed through a 100 μm and a 40 μm filter before use (Corning Scientific Laboratory Supplies, Coatbridge, UK).
Human cell isolation. Underlying fat and muscle layers were removed, tissue was washed in CMF HBSS 2% fetal calf serum (Sigma, Poole, UK), and cut into 0.5 cm sections. The tissue was then shaken vigorously in 10 ml HBSS/2% fetal calf serum and the supernatant discarded. To remove the epithelial layer, 10 ml fresh CMF HBSS containing 2 mM EDTA (Sigma) was added, and the tube was placed in a shaking incubator for 15 mins at 37 °C before being shaken vigorously, and the supernatant was discarded. The intestinal tissue was washed in CMF HBSS and the EDTA step repeated twice more. The remaining tissue was digested with prewarmed complete RPMI-1640 supplemented with 2 mM L-glutamine, 100 μg ml−1 penicillin, 100 μg ml−1 streptomycin, 1.25 μg ml−1 Fungizone (all from Gibco, Invitrogen), and 10% fetal calf serum containing collagenase VIII (1 mg ml−1, Sigma), Collagenase D (1.25 mg ml−1, Roche), Dispase (1 mg ml−1, Gibco, Invitrogen), and DNase (30 μg ml−1, Roche) for 45 min in a shaking incubator at 37 °C. The resulting cell suspension was removed and the digestion was repeated until all tissues were dispersed. Cell suspensions were passed through a 40 μm cell strainer (BD Biosciences, Oxford, UK), washed twice in complete RPMI, and kept on ice until use.
Flow cytometric analysis and sorting. Cells were stained at 4 °C in the dark as described previously28 using the antibodies listed in Supplementary Experimental Procedures online. For intracellular cytokine staining, whole LP digests were incubated for 4.5 h with 5 μg ml−1 brefeldin A and 2 μM monensin (both from Biolegend, London, UK) in the presence or absence of 100 ng lipopolysaccharide from Salmonella typhimurium (Sigma) before fixation and permeabilization. In all analyses, following doublet exclusion, live cells were identified using 7-AAD (Biolegend) or fixable viability dye (eBioscience, Hatfield, UK). Data were acquired on an LSR II, Fortessa, FACSAria I or FACSAria III (BD Biosciences) and analyzed using FlowJo software (Tree Star, Ashland, OR).
Adoptive transfer of BM precursors. For pre-DCs, WT mice were injected with 2 × 106 flt3L-secreting B16 tumor cells subcutaneously (a kind gift from Dr Oliver Pabst, Hannover, Germany) and 10–14 days later BM was isolated and RBC lysed (Stem Cell Technologies, Grenoble, France). Cells were labeled with eFluor450 CellTrace Violet proliferation dye (eBioscience) and pre-DCs identified as Lin−CD11cintCCR9−B220loCD135+ cells. Next, 7 × 105 FACS sorted pre-DCs were injected into unmanipulated congenic recipients, or into mice that had received 1.2% DSS ad libitum in the drinking water for 3 days before transfer. For monocyte transfers, 1 × 106 FACS-purified Ly6Chi monocytes (CD11b+CD117−Ly6G−Ly6ChiCX3CR1int) from the BM of CX3CR1+/gfp CD45.1+/CD45.2+ mice were transferred into CD45.2 CCR2−/− mice.
Antigen-specific T-cell proliferation in vitro. DC subsets were FACS-purified and pulsed with 2 mg ml−1 ovalbumin (Grade VI, Sigma) for 2 h before being washed extensively and cocultured for 4 days with carboxyfluorescein succinimidyl ester-labeled, naive CD62LhiCD25−CD4+ T cells FACS-purified from the lymph nodes of OTII mice. For intracellular cytokine staining, cultured cells were placed in a stimulation cocktail (eBioscience) containing phorbol myristate acetate, ionomycin, brefeldin A, and monensin for 4.5 h before fixation, permeabilization, and staining with antibodies against IL-17a, interferon-γ, and FoxP3.
Quantitation of gene expression by real-time reverse-transcription PCR. Total RNA was purified from sorted LP cells using the RNeasy Micro kit (Qiagen, Manchester, UK). RNA was reverse transcribed to complementary DNA and gene expression was assayed by quantitative reverse-transcription PCR as described previously.16 The primer sequences used are detailed in Supplementary Experimental Procedures online.
Generation of WT:CCR2−/− mixed BM chimeras. CD45.1/CD45.2 WT mice received two doses of 5 Gy, 2 h apart, before receiving 5 × 106 BM cells intravenously from CD45.1 WT and CD45.2 CCR2−/− BM in a 50:50 ratio. Chimerism was assessed 8 weeks after reconstitution.
Assessment of phagocytosis. 3 × 106 Cells were assessed for phagocytosis of pHrodo Escherichia coli bioparticles (Molecular Probes, Life Technologies, Paisley, UK) according to the manufacturer’s guidelines and analyzed by flow cytometry.
Assessment of BrdU incorporation in vivo. Mice were injected once intraperitoneally with 1 mg BrdU (BD Biosciences) and in some experiments received 0.8 mg ml−1 BrdU (Sigma) in their drinking water for 3 days. The incorporation of BrdU by isolated cells was assessed using the BD BrdU Flow kit (BD Biosciences).
Statistical analysis. Results are presented as means ±1 s.d. unless otherwise stated and groups were compared using Student’s t-test or, for multiple groups, one-way analysis of variance followed by Bonferroni posttest using Prism Software (GraphPad Software, San Diego, CA).
References
Mowat, A.M. Anatomical basis of tolerance and immunity to intestinal antigens. Nat. Rev. Immunol. 3, 331–341 (2003).
Coombes, J.L. & Powrie, F. Dendritic cells in intestinal immune regulation. Nat. Rev. Immunol. 8, 435–446 (2008).
Schulz, O. et al. Intestinal CD103+, but not CX3CR1+, antigen sampling cells migrate in lymph and serve classical dendritic cell functions. J. Exp. Med. 206, 3101–3114 (2009).
Persson, E.K., Jaensson, E. & Agace, W.W. The diverse ontogeny and function of murine small intestinal dendritic cell/macrophage subsets. Immunobiology 215, 692–697 (2010).
Cerovic, V. et al. Intestinal CD103(-) dendritic cells migrate in lymph and prime effector T cells. Mucosal Immunol. 6, 104–113 (2013).
Murai, M. et al. Interleukin 10 acts on regulatory T cells to maintain expression of the transcription factor Foxp3 and suppressive function in mice with colitis. Nat. Immunol. 10, 1178–1184 (2009).
Hadis, U. et al. Intestinal tolerance requires gut homing and expansion of FoxP3+ regulatory T cells in the lamina propria. Immunity 34, 237–246 (2011).
Pull, S.L. Activated macrophages are an adaptive element of the colonic epithelial progenitor niche necessary for regenerative responses to injury. Proc. Natl. Acad. Sci. USA 102, 99–104 (2005).
Gautier, E.L. et al. Gene-expression profiles and transcriptional regulatory pathways that underlie the identity and diversity of mouse tissue macrophages. Nat. Immunol. 13, 1118–1128 (2012).
Geissmann, F., Gordon, S., Hume, D.A., Mowat, A.M. & Randolph, G.J. Unravelling mononuclear phagocyte heterogeneity. Nat. Rev. Immunol. 10, 453–460 (2010).
Miller, J.C. et al. Deciphering the transcriptional network of the dendritic cell lineage. Nat. Immunol. 13, 888–899 (2012).
Pabst, O. & Bernhardt, G. The puzzle of intestinal lamina propria dendritic cells and macrophages. Eur. J. Immunol. 40, 2107–2111 (2010).
Hume, D.A. Differentiation and heterogeneity in the mononuclear phagocyte system. Mucosal Immunol. 1, 432–441 (2008).
Kelsall, B. Recent progress in understanding the phenotype and function of intestinal dendritic cells and macrophages. Mucosal Immunol. 1, 460–469 (2008).
Pavli, P., Woodhams, C.E., Doe, W.F. & Hume, D.A. Isolation and characterization of antigen-presenting dendritic cells from the mouse intestinal lamina propria. Immunology 70, 40 (1990).
Bain, C.C. et al. Resident and pro-inflammatory macrophages in the colon represent alternative context-dependent fates of the same Ly6Chi monocyte precursors. Mucosal Immunol. 6, 498–510 (2013).
Fujimoto, K. et al. A new subset of CD103+CD8alpha+ dendritic cells in the small intestine expresses TLR3, TLR7, and TLR9 and induces Th1 response and CTL activity. J. Immunol. 186, 6287–6295 (2011).
Jaensson, E. et al. Small intestinal CD103+ dendritic cells display unique functional properties that are conserved between mice and humans. J. Exp. Med. 205, 2139–2149 (2008).
Bogunovic, M. et al. Origin of the lamina propria dendritic cell network. Immunity 31, 513–525 (2009).
Varol, C. et al. Intestinal lamina propria dendritic cell subsets have different origin and functions. Immunity 31, 502–512 (2009).
Rivollier, A., He, J., Kole, A., Valatas, V. & Kelsall, B.L. Inflammation switches the differentiation program of Ly6Chi monocytes from antiinflammatory macrophages to inflammatory dendritic cells in the colon. J. Exp. Med. 209, 139–155 (2012).
Schlitzer, A. et al. IRF4 transcription factor-dependent CD11b(+) dendritic cells in human and mouse control mucosal IL-17 cytokine responses. Immunity 38, 970–983 (2013).
Zigmond, E. et al. Ly6C(hi) monocytes in the inflamed colon give rise to proinflammatory effector cells and migratory antigen-presenting cells. Immunity 37, 1076–1090 (2012).
Tamoutounour, S. et al. CD64 distinguishes macrophages from dendritic cells in the gut and reveals the Th1-inducing role of mesenteric lymph node macrophages during colitis. Eur. J. Immunol. 42, 3150–3166 (2012).
Ginhoux, F. et al. The origin and development of nonlymphoid tissue CD103+ DCs. J. Exp. Med. 206, 3115–3130 (2009).
Satpathy, A.T. et al. Zbtb46 expression distinguishes classical dendritic cells and their committed progenitors from other immune lineages. J. Exp. Med. 209, 1135–1152 (2012).
Meredith, M.M. et al. Expression of the zinc finger transcription factor zDC (Zbtb46, Btbd4) defines the classical dendritic cell lineage. J. Exp. Med. 209, 1153–1165 (2012).
Bain, C.C. & Mowat, A.M. CD200 receptor and macrophage function in the intestine. Immunobiology 217, 643–651 (2012).
Merad, M. & Manz, M.G. Dendritic cell homeostasis. Blood 113, 3418–3427 (2009).
Onai, N., Obata-Onai, A., Schmid, M.A. & Manz, M.G. Flt3 in regulation of type I interferon-producing cell and dendritic cell development. Ann. NY Acad. Sci. 1106, 253–261 (2007).
Varol, C. et al. Monocytes give rise to mucosal, but not splenic, conventional dendritic cells. J. Exp. Med. 204, 171–180 (2007).
Geissmann, F. et al. Development of monocytes, macrophages, and dendritic cells. Science 327, 656–661 (2010).
Naik, S.H. et al. Intrasplenic steady-state dendritic cell precursors that are distinct from monocytes. Nat. Immunol. 7, 663–671 (2006).
Liu, K. et al. In vivo analysis of dendritic cell development and homeostasis. Science 324, 392–397 (2009).
Serbina, N.V. & Pamer, E.G. Monocyte emigration from bone marrow during bacterial infection requires signals mediated by chemokine receptor CCR2. Nat. Immunol. 7, 311–317 (2006).
Persson, E.K. et al. IRF4 transcription-factor-dependent CD103(+)CD11b(+) dendritic cells drive mucosal T helper 17 cell differentiation. Immunity 38, 958–969 (2013).
Bajaña, S., Roach, K., Turner, S., Paul, J. & Kovats, S. IRF4 promotes cutaneous dendritic cell migration to lymph nodes during homeostasis and inflammation. J. Immunol. 189, 3368–3377 (2012).
Edelson, B.T. et al. Peripheral CD103+ dendritic cells form a unified subset developmentally related to CD8alpha+ conventional dendritic cells. J. Exp. Med. 207, 823–836 (2010).
Vander Lugt, B. et al. Transcriptional programming of dendritic cells for enhanced MHC class II antigen presentation. Nat. Immunol. 15, 161–167 (2014).
Denning, T.L., Wang, Y.-C., Patel, S.R., Williams, I.R. & Pulendran, B. Lamina propria macrophages and dendritic cells differentially induce regulatory and interleukin 17-producing T cell responses. Nat. Immunol. 8, 1086–1094 (2007).
Denning, T.L. et al. Functional specializations of intestinal dendritic cell and macrophage subsets that control Th17 and regulatory T cell responses are dependent on the T cell/APC ratio, source of mouse strain, and regional localization. J. Immunol. 187, 733–747 (2011).
Uematsu, S. et al. Regulation of humoral and cellular gut immunity by lamina propria dendritic cells expressing Toll-like receptor 5. Nat. Immunol. 9, 769–776 (2008).
Siddiqui, K.R.R., Laffont, S. & Powrie, F. E-cadherin marks a subset of inflammatory dendritic cells that promote T cell-mediated colitis. Immunity 32, 557–567 (2010).
Cerovic, V. et al. Intestinal CD103(-) dendritic cells migrate in lymph and prime effector T cells. Mucosal Immunol. 6, 104–113 (2012).
Zeng, R. et al. Retinoic acid regulates the development of a gut-homing precursor for intestinal dendritic cells. Mucosal Immunol. 6, 847–856 (2012).
Lewis, K.L. et al. Notch2 receptor signaling controls functional differentiation of dendritic cells in the spleen and intestine. Immunity 35, 780–791 (2011).
Welty, N.E. et al. Intestinal lamina propria dendritic cells maintain T cell homeostasis but do not affect commensalism. J. Exp. Med. 210, 2011–2024 (2013).
Coombes, J.L. et al. A functionally specialized population of mucosal CD103+ DCs induces Foxp3+ regulatory T cells via a TGF-beta and retinoic acid-dependent mechanism. J. Exp. Med. 204, 1757–1764 (2007).
Scott, C.L., Aumeunier, A.M. & Mowat, A.M. Intestinal CD103+ dendritic cells: master regulators of tolerance? Trends Immunol. 32, 412–419 (2011).
Jung, S. et al. Analysis of fractalkine receptor CX3CR1 function by targeted deletion and green fluorescent protein reporter gene insertion. Mol. Cell. Biol. 20, 4106–4114 (2000).
Kurihara, T., Warr, G., Loy, J. & Bravo, R. Defects in macrophage recruitment and host defense in mice lacking the CCR2 chemokine receptor. J. Exp. Med. 186, 1757–1762 (1997).
McKenna, H.J. et al. Mice lacking flt3 ligand have deficient hematopoiesis affecting hematopoietic progenitor cells, dendritic cells, and natural killer cells. Blood 95, 3489–3497 (2000).
Acknowledgements
We thank the clinicians and patients for supplying clinical samples and also the staff at the NHS GGC Bio-repository, the staff at the Beatson Institute, University of Glasgow, for the irradiation of mice, and the staff at the CRF and JRF facilities for animal husbandry. We thank Drs Oliver Pabst and Vuk Cerovic for critical review of the manuscript. This work was supported by the Wellcome Trust (to C.L.S., C.C.B., and A.M.M.), the Nuffield Foundation (P.B.W.), and the MRC (to S.W.F.M.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Additional information
Supplementary Material is linked to the online version of the paper
Supplementary information
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Scott, C., Bain, C., Wright, P. et al. CCR2+CD103− intestinal dendritic cells develop from DC-committed precursors and induce interleukin-17 production by T cells. Mucosal Immunol 8, 327–339 (2015). https://doi.org/10.1038/mi.2014.70
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2014.70
This article is cited by
-
MHCII expression on gut macrophages supports T cell homeostasis and is regulated by microbiota and ontogeny
Scientific Reports (2023)
-
Dendritic cell functions in the inductive and effector sites of intestinal immunity
Mucosal Immunology (2022)
-
Kidney dendritic cells: fundamental biology and functional roles in health and disease
Nature Reviews Nephrology (2020)
-
Transcriptional profiling reveals monocyte-related macrophages phenotypically resembling DC in human intestine
Mucosal Immunology (2018)
-
To respond or not to respond — a personal perspective of intestinal tolerance
Nature Reviews Immunology (2018)