Abstract
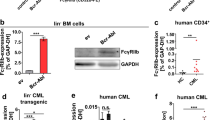
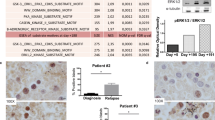
Chronic myeloid leukemia (CML) is characterized by expression of Bcr-abl, a tyrosine kinase oncogene. Clinical outcomes in CML were revolutionized by development of Bcr-abl-targeted tyrosine kinase inhibitors (TKIs), but CML is not cured by these agents. CML leukemia stem cells (LSCs) are relatively TKI insensitive and persist even in remission. LSC persistence results in relapse upon TKI discontinuation, or drug resistance or blast crisis (BC) during prolonged treatment. We hypothesize that increased expression of Fas-associated phosphatase 1 (Fap1) in CML contributes to LSC persistence and BC. As Fap1 substrates include Fas and glycogen synthase kinase-3β (Gsk3β), increased Fap1 activity in CML is anticipated to induce Fas resistance and stabilization of β-catenin protein. Resistance to Fas-induced apoptosis may contribute to CML LSC persistence, and β-catenin activity increases during BC. In the current study, we directly tested the role of Fap1 in CML LSC persistence using in an in vivo murine model. In TKI-treated mice, we found that inhibiting Fap1, using a tripeptide or small molecule, prevented TKI resistance, BC and relapse after TKI discontinuation; all events observed with TKI alone. In addition, Fap1 inhibition increased Fas sensitivity and decreased β-catenin activity in CD34+ bone marrow cells from human subjects with CML. Therapeutic Fap1 inhibition may permit TKI discontinuation and delay in progression in CML.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Rowley JD . Letter: A new consistent chromosomal abnormality in chronic myelogenous leukaemia identified by quinacrine fluorescence and Giemsa staining. Nature 1973; 243: 290–293.
Cortes J, Hochhaus A, Hughes T, Kantarjian H . Front-line and salvage therapies with tyrosine kinase inhibitors and other treatments in CML. J Clin Oncol 2011; 29: 524–531.
Yang K, Fu LW . Mechanisms of resistance to BCR-ABL TKIs and the therapeutic strategies: a review. Crit Rev Oncol Hematol 2015; 93: 277–292.
Erba HP . Molecular monitoring to improve outcomes in patients with chronic myeloid leukemia in chronic phase: importance of achieving treatment-free remission. Am J Hematol 2015; 90: 242–249.
Lau A, Seiter K . Second-line therapy for patients with chronic myeloid leukemia resistant to first-line imatinib. Clin Lymphoma Myeloma Leuk 2104; 14: 186–196.
Mahon FX, Réa D, Guilhot J, Guilhot F, Huguet F, Nicolini F et al. Discontinuation of IM in patients with CML who have maintained complete molecular remission for at least 2 years. Lancet Oncol 2010; 11: 1029–1035.
Horn M, Glauche I, Müller MC, Hehlmann R, Hochhaus A, Loeffler M et al. Model-based decision rules reduce the risk of molecular relapse after cessation of tyrosine kinase inhibitor therapy in chronic myeloid leukemia. Blood 2013; 121: 378–384.
Ross DM, Branford S, Seymour JF, Schwarer AP, Arthur C, Yeung DT et al. Safety and efficacy of imatinib cessation for CML patients with stable undetectable minimal residual disease: results from the TWISTER study. Blood 2013; 122: 515–522.
Drucker BJ, Guilhot F, O’Brien SG, Kantarjian H, Hochhaus A, Gabrilove JL et al. 5 year follow up of patients receiving imatinib for CML. N Engl J Med 2006; 355: 2408–2417.
Michor F, Hughes TP, Iwasa Y, Branford S, Shah NP, Sawyers CL et al. Dynamics of CML. Nature 2005; 435: 1267–1270.
Roeder I, Horn M, Glauche I, Hochhaus A, Mueller MC, Loffler M . Dynamic modeling of imatinib-treated CML: functional insights & clinical implications. Nat Med 2005; 12: 1181–1184.
Michor F . Quantitative approaches to analyzing imatinib-treated CML. Trends Pharmacol Sci 2007; 28: 197–199.
Oncomine, Research Addition, University of Michigan, Ann Arbor www.oncomine.org).
Huang W, Bei L, Eklund EA . Fas associated phosphatase 1 (Fap1) influences βcatenin activity in myeloid progenitor cells expressing the Bcr-abl oncogene. J Biol Chem 2013; 288: 12766–12776.
Huang W, Zhu C, Wang H, Horvath E, Eklund EA . The interferon consensus sequence binding protein (ICSBP/IRF8) represses PTPN13 gene transcription in differentiating myeloid cells. J. Biol. Chem. 2008; 283: 7921–7935.
Huang W, Bei L, Eklund EA . Fas-associated phosphatase 1 (Fap1) mediates Fas-resistance in myeloid progenitor cells expressing the Bcr-abl oncogene. Leuk Lymphoma 2012; 54: 619–630.
Ysebaert L, Chicanne G, Demur C, De Toni F, Prade-Houdellier N, Ruidavets JB et al. Expression of Bcatenin by myeloid leukemia cells predicts clonogenic capacities and poor prognosis. Leukemia 2006; 20: 1211–1216.
Simon M, Grandage VL, Linch DC, Khwaja A . Constitutive activation of the Wnt/B catenin signaling pathway in myeloid leukemia. Oncogene 1995; 24: 2410–2420.
Schmidt M, Nagel S, Proba J, Thiede C, Ritter M, Waring JF et al. Lack of interferon consensus sequence binding protein transcripts in human myeloid leukemias. Blood 1998; 91: 22–29.
Hao SX, Ren R . Expression of ICSBP is down-regulated in bcr-abl-induced murine CML and forced co-expression of ICSBP inhibits bcr-abl-induced MPD. Mol Cell Biol 2000; 20: 1149–1161.
Holtschke T, Lohler J, Kanno J, Kanno Y, Fehr T, Giese N et al. Immuno-deficiency and chronic myelogenous leukemia-like syndrome in mice with a targeted mutation of the ICSBP gene. Cell 1996; 87: 307–317.
Konieczna I, Horvath E, Wang H, Lindsey S, Saberwal G, Bei L et al. Constitutive activation of SHP2 cooperates with ICSBP-deficiency to accelerate progression to acute myeloid leukemia. J Clin Invest 2008; 118: 853–867.
Saras J, Claesson-Welsh L, Heldin CH, Gonex LJ . Cloning and characterization of PTPL1, a PTP with similarities to cytoskeletal-associated proteins. J Biol Chem 1994; 269: 24082–24089.
Yanagisawa J, Takahashi M, Kanki H, Yano-Yanagisawa H, Tazunoki T, Sawa E et al. The molecular interaction of Fas and Fap1. J Biol Chem 1997; 272: 8539–8545.
Kozlov G, Banville D, Ghering K, Ekiel I . Solution structure of the PDZ2 domain from cytosolic human phosphatase hPTP1E complexed with a peptide reveals contribution of the B2-B3 loop to PDZ domain-ligand interactions. J Mol Biol 2002; 320: 813–820.
Zhang J, Sapienza PJ, Ke H, Chang A, Hengel SR, Wang H et al. Crystallographic and nuclear magnetic resonance evaluation of the impact of peptide binding to the second PDZ domain of protein tyrosine phosphatase 1E. Biochemistry 2010; 49: 9280–9291.
Minami Y, Stuart SA, Ikawa T, Jiang Y, Banno A, Hunton IC et al. BCR-ABL-transformed GMP as myeloid leukemic stem cells. Proc Natl Acad Sci USA 2008; 105: 17967–17972.
Peng C, Li S . CML mouse model in translational research. Methods Mol Biol 2010; 602: 253–266.
Huang W, Zhou W, Saberwal G, Konieczna I, Horvath E, Katsoulidis E et al. The interferon consensus sequence binding protein (ICSBP) decreases Bcatenin-activity in myeloid cells by repressing GAS2 transcription. Mol Cell Biol 2010; 30: 4575–4594.
Huang W, Hu L, Bei L, Hjort E, Eklund EA . The leukemia-associated fusion-protein Tel-platelet derived growth factor receptor B (Tel-PdgfRB) inhibits transcriptional repression of the PTPN13 gene by the interferon consensus sequence binding protein (Icsbp). J Biol Chem 2012; 287: 8110–8125.
Eklund EA, Kakar R . Identification of TF1phox, a DNA binding protein that increases expression of gp91phox in myeloid leukemia cells. J Biol Chem 1997; 272: 9344–9355.
Lichty BD, Keating A, Callum J, Yee K, Croxford R, Corpus G et al. Expression of p210 and p190 BCR-ABL due to alternative splicing in chronic myelogenous leukaemia. Br J Haematol 1998; 103: 711–715.
Eash KJ, Greenbaum AM, Gopalan PK, Link DC . CXCR2 and CXCR4 antagonistically regulate neutrophil trafficking from murine bone marrow. J Clin Invest 2010; 120: 2423–2431.
Rossi AM, Taylor CW . Analysis of protein-ligand interactions by fluorescence polarization. Nat Protoc 2011; 6: 365–387.
Layton CJ, Hellinga HW . Quantitation of protein-protein interactions by thermal stability shift analysis. Protein Sci 2011; 20: 1439–1450.
Pantoliano MW, Petrella EC, Kwasnoski JD, Lobanov VS, Myslik J, Graf E et al. High-density miniaturized thermal shift assays as a general strategy for drug discovery. J Biomol Screen 2001; 6: 429–440.
Gruszecka-Kowalik E, Haugwitz RD, Zalkow LH . Quinobene, a new potent anti-HIV agent. Biochem Biophys Res Commun 1992; 187: 1409–1417.
Bigelow J, Mathews L, McCormack J . Analytical studies and murine pharmacokinetics of quinobene. Proc Am Assoc Cancer Res Annu Meet 1993; 34: 397.
Turkina AG, Logacheva NP, Stromskaya TP, Zabotina TN, Kuznetzov SV, Sachibzadaeva KK et al. Studies of some mechanisms of drug resistance in CML. Adv Exp Med Biol 1999; 457: 477–488.
Jamieson CH, Ailles LE, Dylla SJ, Muijtjens M, Jones C, Zehnder JL et al. Granulocyte-macrophage progenitors as candidate leukemic stem cells in blast-crisis CML. N Engl J Med 2004; 351: 657–667.
Acknowledgements
This work was supported by NIH-CA174205 and VA-BX002067 (to EAE), NIH-CA77816 and VA-I01CX000916 (to LCP) and NIH-HL75826 (to KMS).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Leukemia website
Rights and permissions
About this article
Cite this article
Huang, W., Luan, CH., Hjort, E. et al. The role of Fas-associated phosphatase 1 in leukemia stem cell persistence during tyrosine kinase inhibitor treatment of chronic myeloid leukemia. Leukemia 30, 1502–1509 (2016). https://doi.org/10.1038/leu.2016.66
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2016.66
This article is cited by
-
Chronic myeloid leukemia stem cells: targeting therapeutic implications
Stem Cell Research & Therapy (2021)
-
Investigating the role of the innate immune response in relapse or blast crisis in chronic myeloid leukemia
Leukemia (2020)
-
DYRK2 controls a key regulatory network in chronic myeloid leukemia stem cells
Experimental & Molecular Medicine (2020)
-
Chronic myeloid leukemia stem cells
Leukemia (2019)