Abstract
B-cell maturation antigen (BCMA) is a highly plasma cell-selective protein that is expressed on malignant plasma cells of multiple myeloma (MM) patients and therefore is an ideal target for T-cell redirecting therapies. We developed a bispecific T-cell engager (BiTE) targeting BCMA and CD3ɛ (BI 836909) and studied its therapeutic impacts on MM. BI 836909 induced selective lysis of BCMA-positive MM cells, activation of T cells, release of cytokines and T-cell proliferation; whereas BCMA-negative cells were not affected. Activity of BI 836909 was not influenced by the presence of bone marrow stromal cells, soluble BCMA or a proliferation-inducing ligand (APRIL). In ex vivo assays, BI 836909 induced potent autologous MM cell lysis in both, newly diagnosed and relapsed/refractory patient samples. In mouse xenograft studies, BI 836909 induced tumor cell depletion in a subcutaneous NCI-H929 xenograft model and prolonged survival in an orthotopic L-363 xenograft model. In a cynomolgus monkey study, administration of BI 836909 led to depletion of BCMA-positive plasma cells in the bone marrow. Taken together, these results show that BI 836909 is a highly potent and efficacious approach to selectively deplete BCMA-positive MM cells and represents a novel immunotherapeutic for the treatment of MM.
Similar content being viewed by others
Introduction
Multiple myeloma (MM) is the second most common hematological malignancy in USA and Europe. MM is characterized by uncontrolled proliferation of monoclonal plasma cells in the bone marrow, resulting in the over-production of monoclonal immunoglobulin and immunosuppression, as well as osteolysis and end-organ damage.1 Treatment advances in the past decade have significantly improved survival of MM patients, and recently the first two monoclonal antibodies have been approved, daratumumab and elotuzumab, targeting CD38 and CS-1/SLAMF7,2, 3, 4 respectively. Nonetheless, there is still unmet medical need for more effective treatments, in particular, for relapsed/refractory patients who are resistant to current therapies.
BiTE (bispecific T-cell engager) antibody constructs represent a novel class of immunotherapy. BiTE molecules bind concomitantly to T cells and tumor cells and direct the cytolytic activity of T cells selectively to tumor cells. After formation of a cytolytic synapse, the T cells release perforin and granzyme B, finally leading to apoptosis of the tumor cells.5 Activation of T cells leads to transient release of cytokines, which engages other immune cells and broadens the immune response against the tumor tissue and ultimately leads to proliferation of T cells and serial killing of tumor cells.5, 6, 7, 8 Due to their small size (55 kDa), BiTE antibody constructs are highly potent and efficacious molecules. In 2014, blinatumomab, the first BiTE, has been approved by the U.S. Food and Drug Administration for the treatment of Philadelphia chromosome-negative relapsed/refractory B-cell precursor acute lymphocytic leukemia.9
The BiTE mode of action requires target cell antigens that are selectively expressed in diseased cells to maximize the therapeutic window. Many known MM antigens, including some that are targeted by antibody-based therapies (for example, CD56, CD138, CD74), show overexpression in myeloma cells but are also known to be expressed in normal tissues,2, 4, 10, 11 thus may not be optimal targets for a T-cell re-direction approach.
B-cell maturation antigen (BCMA) is a highly plasma cell specific antigen which has a central role in regulating B-cell maturation and differentiation into plasma cells by engaging a proliferation-inducing ligand (APRIL), and is required for optimal survival of long-lived plasma cells in the bone marrow.12 BCMA−/− mice have impaired long-term plasma cell survival but do not show defects in short-term production of immunoglobulins, early humoral immune response and B-cell development.13, 14 BCMA is expressed on MM cell lines and malignant plasma cells with high prevalence and increased expression levels during disease progression from monoclonal gammopathy of undetermined significance (MGUS) to smoldering myeloma to active MM.15, 16, 17, 18, 19, 20, 21 BCMA is also expressed on plasmacytoid dendritic cells, which promote MM cell growth, survival and drug resistance.21, 22, 23 Expression levels on plasmacytoid dendritic cells are also elevated in MM patients versus normal donors.21 Apart from expression on peripheral and bone marrow resident plasma cells and plasmacytoid dendritic cells, BCMA is not expressed on naive and most memory B cells, CD34+ hematopoietic cells, or any other normal tissue cells.12, 14, 17, 24 Furthermore, BCMA overexpression or APRIL stimulation via BCMA in MM cells can directly upregulate key immune checkpoint molecules, which may contribute to the immunosuppressive bone marrow microenvironment.25
In this manuscript, we describe the preclinical profile of a novel BCMA BiTE antibody construct (BI 836909). BI 836909 shows selective and highly potent T-cell redirected lysis of MM cells in vitro, in vivo and ex vivo and has entered clinical trials for the treatment of MM (NCT02514239).
Materials and methods
Expression and purification of BI 836909
BI 836909 was constructed by recombinant DNA technology and purified from the supernatants from transfected Chinese hamster ovary cells. Purification of the monomeric protein was performed in a two-step process using immobilized nickel chelate chromatography followed by size exclusion chromatography, as described for other BiTE antibody constructs.26, 27
Cell lines and cell culture
Cell lines were obtained from ATCC and DSMZ. The cells were cultured as described in the supplier’s description and tested to exclude mycoplasma contamination.
Blood and bone marrow samples
The blood samples from healthy volunteers were obtained from the Austrian Red Cross and Dana Farber Cancer Institute. They were obtained after informed consent in accordance with the Declaration of Helsinki and with approval of the cantonal ethical committee in Austria and Dana Farber Cancer Institute in the USA. MM patient bone marrow mononuclear cells were collected from fresh buffy coat of bone marrow aspirates obtained after informed consent, in accordance with the Declaration of Helsinki and under the auspices of a Dana Farber Cancer Institute Institutional Review Board approved protocol. Bone marrow stromal cells (BMSCs) were derived after 2-week culture of CD138-negative cells from bone marrow mononuclear cells as described previously.21
T-cell activation, cytotoxicity and T-cell proliferation assays
Redirected T-cell cytotoxicity was assayed by flow cytometry using human PBMCs (peripheral blood mononuclear cells) or purified T cells and various tumor cell lines or primary myeloma cells. Effector cells were co-incubated with target cells and serial dilutions of BI 836909. After incubation, anti-human CD138 antibody or anti-CD33 (for HL-60 cells) antibody (Miltenyi Biotec, San Diego, CA, USA) was added to the cells to distinguish target from effector cells. For detection of T-cell activation, the cells were stained with anti-CD4, anti-CD8, anti-CD25 and anti-CD69 antibodies (all from Becton Dickinson, Franklin Lakes, NJ, USA). For analysis of T-cell proliferation, the T cells were labeled with CFDA-SE (Becton Dickinson). The cells were analyzed by flow cytometry. Number of depleted target cells has been determined with the following formula: % Lysis=100−(viable cells of treatment group × 100/viable cells of untreated control group).
Quantification of cytokines in cell culture supernatants
Cytokine concentrations were analyzed from supernatants of cytotoxicity assays using the V-PLEX Proinflammatory Panel1 (human) Kit (Mesoscale Discovery, Rockville, MA, USA) following the manufacturer’s instructions.
Bioluminescence-based cell lysis assays
To determine lysis of INA6luc or MM1Sluc cells by T cells induced by BI 836909, serial dilutions of the drug were co-incubated with these MM cells, alone or with BMSCs derived from patients. The luciferase signal produced by surviving MM cells was determined after 24 h with a luminometer SpectraMax (Molecular Devices, Sunnyvale, CA, USA) within 20 min after the addition of 125 μg/ml beetle luciferin (Promega).
Mouse xenograft studies
Antitumor activity was evaluated in 7- to 8-week-old NOD.CB17-Prkdcscid/J mice purchased from Charles River (Charles River Laboratories, Sulzfeld, Germany). All the experiments were performed according to the German Animal Welfare Law with permission from the responsible local authorities.
NCI-H929 xenograft model
The NCI-H929 cells (5x106) were injected subcutaneously into the right dorsal flank of sublethally irradiated (2 Gy) female NOD/SCID mice. Eight days later, the animals received a single intravenous dose of anti-asialo GM1 (WAKO, Neuss, Germany) antibody. On day 9, 2 × 107 in vitro expanded human T cells (T-cell isolation, activation/expansion kits from Miltenyi Biotec) were injected into the peritoneal cavity. The animals were randomized based on tumor size on day 12 and treatment with BI 836909 was initiated on day 13. Tumor growth was monitored by caliper measurements. The study was terminated on day 30, when tumors of vehicle-treated mice exceeded 2000 mm3.
L-363 orthotopic model
The L-363 cells (1 × 107) were injected intravenously into irradiated NOD/SCID mice. Mice received anti-asialo antibody as described above. On day 5, the mice were reconstituted with human T cells, as described above. The animals were randomized and treatment with BI 836909 was started on day 8. Survival was statistically analyzed with the log-rank test. A P-value <0.05 was considered to be statistically significant.
Cynomolgus monkey studies
Groups (two or three animals/group) of male and female cynomolgus monkeys were given 0, 5, 15, 45 or 135 μg/kg/day of BI 836909 via continuous intravenous infusion at a dose volume of 20 ml/kg/day or 135 or 405 μg/kg/day at a dose volume of 2 ml/kg/day via subcutaneous injection for 7 days at WIL Research, Lyon, France. To evaluate effects on plasma cells, differential analysis of bone marrow cytological smears was performed microscopically on a minimum of 400 cells or ten × 1000 fields at Boehringer-Ingelheim, Ridgefield, CT, USA. The experiment was approved by the ethical committee of WIL Research as per the appropriate animal health and welfare guidelines.
Results
Structural characteristics, production and binding properties of BI 836909
BI 836909 is a bispecific single-chain variable fragment consisting of two linked single-chain variable fragments (scFvs). The BCMA scFv is positioned N-terminally, and the CD3ɛ scFv C-terminally followed by a hexahistidine (His6 tag) (Supplementary Figure S1a). Purity of purified monomeric BI 836909 protein was demonstrated by SDS-PAGE and anti-His6 western blot (Supplementary Figures S1b, c). BI 836909 binds monovalent to BCMA and CD3ɛ and is cross-reactive to cynomolgus monkey BCMA and CD3ɛ as shown in FACS analysis of human or cynomolgus monkey-transfected Chinese hamster ovary cells and human and cynomolgus monkey T cells (Supplementary Figure S2).
BI 836909 induces BCMA-dependent T-cell activation and cytokine release resulting in apoptosis of MM cells and proliferation of T cells
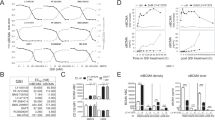
Upon simultaneous binding to BCMA-positive MM cells and CD3-positive T cells, BI 836909 forces cross-linking of both cell types, formation of a cytolytic synapse and subsequently activation of T cells and lysis of BCMA-positive MM cells. As shown in Figure 1, BI 836909 induces activation of T cells, as indicated by upregulation of expression of CD25 and CD69 expression, lysis of MM.1R cells and secretion of cytokines, a hallmark of T-cell activation upon target cell lysis. The tumor cells were incubated with PBMCs (n=3) for 24 h followed by FACS analysis to determine the activation status of T cells and the survival of CD138/BCMA-positive MM.1R cells or CD33-positive/BCMA-negative HL-60 cells. In the presence of BCMA-positive MM.1R cells but not BCMA-negative HL-60 cells, BI 836909 induced activation of both CD4 and CD8 T cells in a dose-dependent manner, as evidenced by upregulation of CD25 and CD69 expression (Figure 1a). Importantly, BI 836909 induces highly potent (mean EC50 value of 4.3 pg/ml) and selective lysis of MM.1R but not of HL-60 cells (Figure 1b). In total, 12 MM and plasma cell leukemia cell lines were analyzed, and EC50 values ranged from 4 to 589 pg/ml with a mean of 180 pg/ml (Supplementary Table S1). Using MM.1R cells and purified T cells, activity of BI 836909-mediated lysis was observed at effector to target (E:T) cell ratios of 1:100 or higher, and maximal tumor lysis was achieved at E:T ratios of 1:1 or higher, with EC50 values decreasing with increasing E:T cell ratios (Supplementary Figure S3). Using a luciferase activity assay in a Luciferase-transfected INA6 (INA6luc) MM cell line, BI 836909 only induced significant MM cell lysis when PBMCs and target cells were present (Figure 1c). Without PBMC effector cells, BI 836909 did not induce any lysis of NCI-H929 MM cells even with the highest levels of BCMA among all MM cell lines21 (Figure 1d). Furthermore, BI 836909 induced a dose-dependent secretion of cytokines (IFNγ, IL-2, IL-6, IL-10, TNFα), a hallmark of T-cell activation (Figure 1e).
BI 836909 induces highly potent and BCMA-dependent tumor cell lysis via activation of T cells. BCMA-positive MM.1R cells (black curves) or BCMA-negative HL-60 cells (gray curves) were incubated with PBMCs from three donors (circle, square, triangle) at an E:T of 6:1 in the presence of increasing concentrations of BI 836909 for 24 h. (a) Activation markers CD25 and CD69 on CD4-positive and CD8-positive T cells as well as (b) % of tumor target lysis in CD138-positive (MM.1R) and CD33-positive (HL-60) cells was determined by flow cytometric analysis. (c) INA6luc MM cells, alone or with PBMCs, were treated with BI 836909 for 24 h and viable cells were determined by luciferase activity assay. (d) NCI-H929 MM cells, alone or with PBMCs were treated with BI 836909 for 24 h at an E:T of 10:1 followed by flow cytometry analysis. (e) Cytokine levels were determined in cell culture supernatant.
CD4, as well as CD8 T cells contribute to cytotoxicity of BI 836909. Lysis activity by CD4-positive T cells was slightly lower than with CD8-positive T cells after 8 h of incubation. After 16 to 24 h, cytotoxicity activity was comparable between CD4-positive (0.02/0.007 ng/ml, respectively) and CD8-positive (0.008/0.004 ng/ml respectively) T cells (Figure 2a). Treatment with BI 836909 induced translocation of phosphatidylserine from the inner to the outer leaflet of the plasma membrane, as shown by Annexin V binding (Figure 2b). Activation of T cells, cytolytic activity and subsequent cytokine release ultimately led to the proliferation of T cells after 4 days of incubation (Figure 2c). Treatment of BCMA-negative cells did not trigger any of the activities described above demonstrating that the cytotoxic activity of BI 836909 is highly selective to BCMA expressing cells.
In vitro MoA studies. (a) MM.1R cells were co-cultivated for up to 24 h with purified CD4 or CD8 T cells at an E:T ratio of 10:1, and increasing concentrations of BI 836909. (b) MM.1R cells were incubated with purified human T cells at an E:T cell ratio of 10:1 without and with BI 836909 (100 ng/ml) for 24 h before staining with Annexin/PI. (c) Purified T cells were labeled with the CFDA-SE and subsequently incubated at an E:T cell ratio of 10:1 in the presence (1 μg/ml) or absence of BI 836909 for 4 days.
BI 836909 is active against myeloma cells co-cultured with BMSCs
As BMSCs protect MM cells from drug treatment and significantly induce MM cell growth and survival, we determined whether BI 836909 still induces killing of MM cells when co-cultured with BMSCs derived from MM patients. Using a luciferase activity assay following 1 day co-cultures of either INA6luc or MM.1Sluc target cells with patient PBMCs in the presence of BMSCs, BI 836909 remains active and lyse MM cells (Figure 3a). There was no difference in responses to the drug with or without BMSCs. In an additional FACS-based assay, BI 836909-mediated redirected lysis of NCI-H929 cells was only slightly reduced in the presence of BMSCs following 48 h of incubation (Supplementary Figure S4). The EC50 values were 2.2 and 0.5 ng/ml with and without BMSCs, respectively. Furthermore, after 24 h incubation of U266 MM cell line with purified T cells in the presence of BMSCs, BI 836909 induced cell surface CD107a expression on CD8-gated T cells in a dose-dependent manner (Figure 3b), indicating significant MM cell lysis in the bone marrow microenvironment.
Presence of BMSCs does not influence activity of BI 836909. (a) BMSCs derived from patients were plated in culture plates 1 day before the addition of INA6luc (left) or MM1Sluc (right) MM cells, in the presence or absence of PBMCs with increasing concentrations of BI 836909. The cells were collected following 1 day incubation and %bioluminescence+live cells was measured. (b) U266 MM cells and purified human T cells were added into BMSC-plated 96-well tissue culture plates for 3 h. FACS analysis for CD107a was done on CD8-gated T cells to determine % degranulated T cells.
Soluble APRIL and BCMA have only a minor impact on BI 836909 activity
Presence of soluble forms of APRIL15 and BCMA20 in the serum of MM patients have been described. A cytotoxicity assay with NCI-H929 and purified T cells in the presence and absence of pathological APRIL levels (100 ng/ml) showed that cytolytic activity of BI 836909 is not impacted in the presence of recombinant APRIL (Figure 4a). Further biochemical studies demonstrated that BI 836909 can replace APRIL that is bound to BCMA (Supplementary Figure S5a) and that BI 836909 inhibits binding of APRIL to BCMA (Supplementary Figure S5b). Soluble BCMA-containing medium was collected from BCMA-positive cell lines (Supplementary Figure S6), and cytotoxicity assays with MM.1R cells and PBMCs were subsequently performed in conditioned medium containing different levels of soluble BCMA. Soluble BCMA slightly influenced the potency (shift in EC50 values) but not the maximal lysis mediated by BI 836909 (Figure 4b). Presence of soluble BCMA had no effect on off-target activity of BI 836909, as no lysis of BCMA-negative HL-60 cells was observed in the presence of soluble BCMA, while L-363 cells showed similar results as MM.1R cells (Figure 4c).
Influence of soluble APRIL and BCMA on cytolytic activity of BI 836909. (a) T cells, NCI-H929 cells and increasing concentrations of BI 836909 were incubated in the presence of 100 ng/ml recombinant soluble APRIL. (b) NCI-H929 cells were incubated with T cells and increasing BI 836909 concentrations in conditioned medium containing different levels of soluble BCMA produced by NCI-H929 (containing soluble BCMA) and HL-60 (without soluble BCMA) cells. (c) L-363 and HL-60 cells were incubated with T cells and increasing BI 836909 in conditioned medium from BCMA-positive and -negative cells. All assays have been performed at an E:T ratio of 6:1 with 24 h incubation and depletion of target cells was measured by FACS analysis after 24 h of incubation.
BI 836909 potently induces autologous tumor cell lysis
We next assessed tumor lysis activity of BI 836909 against autologous patient MM cells. The bone marrow mononuclear cells were purified from BM aspirates collected from MM patients and incubated with autologous PBMCs at an E:T ratio of 10:1 and in the presence of serial dilutions of BI 836909 for 24 h, followed by FACS analysis to determine percentage of viable CD138-positive cells. BI 836909, in a dose-dependent manner, induced autologous lysis of CD138-positive cells from patients with both, newly diagnosed (n=4) and relapsed/refractory (RR) MM (n=4; Figure 5a). BI 836909 potently induces patient MM cell lysis, regardless of disease status. In all tested MM patient samples, BI 836909 at 40 ng/ml induced maximal autologous patient MM cell lysis following 24 h ex vivo culture (Figure 5b). As expected, the intensity of BCMA expression was high in CD138-positive plasma cells in MM patients, as observed in previous reports.21 These results suggest that BI 836909 has potent cytolytic activity in MM patients, regardless of disease status.
BI 836909 significantly induced autologous patient MM cell lysis via activated T cells. (a) Bone marrow mononuclear cells (BMMCs) from a newly diagnosed (ND, upper panel) and relapsed and refractory (RR) patients (lower panel RR1-2) were incubated with PBMCs derived from the same individual at a ratio of 1 to 10 in the presence of serial dilutions of BI 836909 (0–40 ng/ml). After 1 day, the cells were then subjected to flow cytometry analysis to determine % of viable CD138+ MM cells. (b) BMMCs collected from additional three ND (MM1–3) and four RR (RR1–4) MM patients were tested and results are shown on the left and middle panels. BCMA antigen-binding capacity using quantitative flow cytometry is shown on the right.
In vivo activity of BI 836909
BI 836909 is cross-reactive to cynomolgus monkey but does not recognize the cognate antigens in rodent species, therefore the in vivo efficacy experiments have been conducted in mouse xenograft models reconstituted with human T cells. The antitumor activity was initially assessed using a human MM (NCI-H929) xenograft model. In this model NCI-H929 cells were injected subcutaneously into the NOD/SCID mice followed by intraperitoneal transfer of purified and in vitro expanded T cells once tumors reached a median size of 107 mm3. Treatment with BI 836909 or vehicle was started on day 13, 4 days after T-cell transfer when tumors had reached a median size of 207 mm3. Treatment with BI 836909 at a daily dose of 0.5 mg/kg/day led to continuous tumor shrinkage in 6 of 10 animals, with all 6 responders tumor free at the end of the study (Figure 6a). Four out of 10 animals did not respond to treatment and had tumor volumes in the same range as the vehicle control group (Figure 6a).
BI 836909 eradicates established xenograft tumors and significantly prolongs survival. (a) Antitumor activity of BI 836909 in an NCI-H929 human multiple myeloma xenograft model. NCI-H929 xenografts were grown subcutaneously for 10 days until they reached a volume of approximately 100 mm3. Then mice were injected with activated and ex vivo expanded human T cells into the peritoneal cavity. Three days later (day 13), when tumor volumes had reached approximately 207 mm3 without significant deviations among study groups, the mice were treated once daily for 19 days with 0.5 mg/kg of BI 836909 or vehicle by intravenous bolus injection. Tumor growth was determined by external caliper measurements and tumor volumes were calculated using a standard hemiellipsoid formula. Dunnett’s posttest; z, no tumors were visible at necroscopy in three animals of the subcutaneously-treated group. Remaining tumor tissue, spleen and bone marrow from four non-responding animals (NR1–4) and one responding animal (R1) was analyzed for the presence of T cells (staining with anti-CD3 antibody) and tumor tissues for expression of BCMA (staining with anti-BCMA antibody) by flow cytometry (b) Orthotopic L-363 xenograft model. Human L-363 cells (1 × 107 cells/mouse) were injected intravenously into female NOD/SCID mice. In vitro expanded and activated human T cells were transplanted into the peritoneal cavity of mice on day 5, and treatment was initiated on day 8. BI 836909 BiTE antibody construct was administered by intravenous bolus injections for a maximum of 26 consecutive days, depending on individual survival. The control animals were treated intravenously with vehicle. Asterisks in the figure legend denote statistically significant differences (log-rank test; NS: not significant; *P<0.05) between vehicle- and BI 836909-treated groups.
Subsequent analysis of bone marrow, spleen and tumor tissue of non-responding mice (when available) revealed that BCMA expression on tumor cells of non-responders is maintained but that engraftment of T cells failed in non-responding animals. FACS analysis of tumor tissue of these non-responding mice (NR1–4) demonstrated that in all four mice >98% of tumor cells express BCMA. Tumor tissue of all four non-responding mice were also examined for the presence of T cells: in three mice (NR1, 3, 4), no T cells were detected in the tumor tissue and in one mouse (NR2) only very few T cells were detected in the tumor tissue. A tissue sample from the site of the previous tumor from a responding animal (R1) was also examined; although no tumor cells were observed in this tissue sample, a high amount of human T cells was detectable in this tissue sample. In addition, bone marrow and spleen from two non-responding mice (NR2, NR4) and one responding mouse (R1) were analyzed for presence of T cells. In the responding animal, T cells were present in spleen and bone marrow, whereas in the non-responding animals no T cells were detected in the bone marrow and spleen (Figure 6a).
In vivo activity of BI 836909 was also tested in an orthotopic L-363 xenograft model. In this model, L-363 cells were injected intravenously into the lateral tail vein, on day 5, before in vitro expanded T cells were injected into the peritoneal cavity of animals. Treatment with BI 836909 was started on day 8, with daily intravenous bolus injection for 26 consecutive days. BI 836909 significantly prolonged survival of the animals at dose levels of 0.005 mg/kg/day day or higher. Treatment with BI 836909 resulted in prolonged median survival of 43.5 days (for the 0.5 and 0.05 mg/kg/day cohorts) and 43 days (for 0.005 mg/kg/day cohort) compared with 34 days in the vehicle-treated group (Figure 6b).
BI 836909 induces depletion of BCMA-positive plasma cells in cynomolgus monkeys
In vitro activity of BI 836909 in cynomolgus monkey was determined in a cytotoxicity assay using purified cynomolgus monkey T cells as effector cells and Chinese hamster ovary cells stably transfected with cynomolgus monkey BCMA as target cells. Figure 7a shows representative examples with three different PBMC donors where the mean EC50 value was 0.2 ng/ml (range 0.08–0.3 ng/ml).
BI 836909 is cross-reactive to cynomolgus monkey BCMA and CD3 and induces depletion of BCMA-positive plasma cells in the bone marrow of cynomolgus monkey. (a) Cynomolgus monkey T cells, Chinese hamster ovary (CHO) cells transfected with cynomolgus monkey BCMA and increasing concentrations of BI 836909 were incubated for 48 h at an effector to target cell ratio of 10:1. The assay was performed with three different PBMC donors indicated by different symbols. (b) BI 836909 was administered to cynomolgus monkeys at doses up to 135 μg/kg/day via continuous intravenous infusion, and up to 405 μg/kg/day via daily subcutaneous injection. Plasma cell numbers in bone marrow were determined by cytological evaluation of bone marrow smears.
In a 7-day dose-range finding study, groups (two or three animals/group) of male and female cynomolgus monkeys were given 5, 15, 45 or 135 μg/kg/day of BI 836909 via continuous intravenous infusion at a dose volume of 20 ml/kg/day or 135 or 405 μg/kg/day via subcutaneous injection at a dose volume of 2 ml/kg/day for 7 consecutive days. The administration of BI 836909 was well tolerated. All the animals survived until the scheduled termination. Clinical signs of toxicity were limited to vomiting and increased body temperature at 4 to 8 h after the start of administration at dose levels⩾15 μg/kg/day and were accompanied by transient increases in serum cytokines (MCP-1, IL-2, IFNγ and/or IL-6). Cytokine levels returned to background level at 24 h.
Dose-dependent decreases in bone marrow plasma cells were detected in animals given BI 836909 at doses ⩾15 μg/kg/day continuous intravenous infusion or ⩾135 μg/kg/day subcutaneous (Figure 7b). At these lowest dose levels tested with either route of administration, two of three animals had plasma cell values below published ranges (0.7–2.3%)28 and the values in all animals at any of these dose levels were below the lowest value detected in the intravenously treated vehicle group.
Discussion
BI 836909 induces highly selective lysis of BCMA-positive MM cells in vitro, ex vivo and in vivo.
In vitro assays using purified CD4- and CD8-positive T-cell subsets indicate that both T-cell subpopulations contribute to BI 836909-mediated redirected lysis of MM.1R cells. Maximal target cells lysis by CD4-positive T cells was slightly lower after 8 h compared with CD8-positive T cells, but comparable at later time points. This is in line with previously published data with an EpCAM/CD3 BiTE demonstrating that both T-cell subsets contribute to the lysis activity with slightly different kinetics.5 Maximal cytotoxic activity was reached after 16 to 24 h and we show that T cells are proliferating after 4 days. We observed (data not shown) that the T cells reach their maximal cell size after 72 h of incubation, assuming that this time is needed for the T cells to prepare for progressing through the cell cycle. This finding is in line with published data showing T-cell proliferation after 5 days, whereas cell lysis was already seen after 24 h.29
BMSCs are known to protect MM cells from apoptosis and can be involved in drug resistance,23 therefore we tested BI 836909 in in vitro assays where we co-cultured BMSCs with two different MM cell lines and PBMCs. Importantly, the presence of BMSCs did not influence the activity of BI 836909. In addition, published data indicate that there are high levels of soluble APRIL and BCMA in MM patient serum, which could potentially interfere with the binding of BI 836909 to BCMA or act as a drug sink. Our data demonstrate that the presence of pathological levels of soluble APRIL and BCMA has only a small impact on potency of BI 836909 and thus are unlikely to limit the clinical activity.
In vitro assays using MM cell lines and PBMCs or purified T cells from a normal blood donor have some limitations and do not fully reflect the nature of patient-derived target as well as effector cells. Therefore we performed ex vivo assays using MM cells and T cells from the same patients (autologous system) that mimic the situation in patients more closely than in vitro assays. BI 836909 potently stimulates and redirects patient T cells from newly diagnosed, as well as relapsed/refractory patients to lyse autologous MM cells, regardless of the disease status. These experiments demonstrate that T cells from MM patients, both newly diagnosed and relapsed/refractory patients, are engaged by BI 836909 and that their cytolytic activity lyses MM cells, supporting the clinical evaluation of BI 836909 in both treatment lines.
BI 836909 treatment led to the depletion of BCMA-positive plasma cells in the bone marrow of cynomolgus monkeys. This represents an important preclinical PD read-out of activity that supports the selection of the optimal therapeutic dose. To date, two additional BCMA-targeting concepts have shown promising preclinical activity and have entered clinical trials, anti-BCMA chimeric antigen receptor T cells (BCMA-CAR),17, 30 and a BCMA antibody drug conjugate (GSK2857916).21 However, the optimal therapeutic concept for targeting BCMA to treat MM patients still needs to be fully evaluated in clinical trials.
In summary, the preclinical data presented in this manuscript show that BI 836909 selectively and potently redirects T cells to MM cells, and supports clinical testing in MM patients.
References
Dimopoulos MA, Richardson PG, Moreau P, Anderson KC . Current treatment landscape for relapsed and/or refractory multiple myeloma. Nat Rev Clin Oncol 2015; 12: 42–54.
Phipps C, Chen Y, Gopalakrishnan S, Tan D . Daratumumab and its potential in the treatment of multiple myeloma: overview of the preclinical and clinical development. Ther Adv Hematol 2015; 6: 120–127.
Lonial S, Dimopoulos M, Palumbo A, White D, Grosicki S, Spicka I et al. Elotuzumab therapy for relapsed or refractory multiple myeloma. N Engl J Med 2015; 373: 621–631.
Palumbo A, Sonneveld P . Preclinical and clinical evaluation of elotuzumab, a SLAMF7-targeted humanized monoclonal antibody in development for multiple myeloma. Expert Rev Hematol 2015; 8: 481–491.
Brischwein K, Schlereth B, Guller B, Steiger C, Wolf A, Lutterbuese R et al. MT110: a novel bispecific single-chain antibody construct with high efficacy in eradicating established tumors. Mol Immunol 2006; 43: 1129–1143.
Hoffmann P, Hofmeister R, Brischwein K, Brandl C, Crommer S, Bargou R et al. Serial killing of tumor cells by cytotoxic T cells redirected with a CD19-/CD3-bispecific single-chain antibody construct. Int J Cancer 2005; 115: 98–104.
Gruen M, Bommert K, Bargou RC . T-cell-mediated lysis of B cells induced by a CD19xCD3 bispecific single-chain antibody is perforin dependent and death receptor independent. Cancer Immunol Immunother 2004; 53: 625–632.
Baeuerle PA, Kufer P, Bargou R . BiTE: teaching antibodies to engage T-cells for cancer therapy. Curr Opin Mol Ther 2009; 11: 22–30.
Sanford M . Blinatumomab: first global approval. Drugs 2015; 75: 321–327.
Kambham N, Kong C, Longacre TA, Natkunam Y . Utility of syndecan-1 (CD138) expression in the diagnosis of undifferentiated malignant neoplasms: a tissue microarray study of 1,754 cases. Appl Immunohistochem Mol Morphol 2005; 13: 304–310.
Lima M, Leander M, Santos M, Santos AH, Lau C, Queiros ML et al. Chemokine receptor expression on normal blood CD56(+) NK-cells elucidates cell partners that comigrate during the innate and adaptive immune responses and identifies a transitional NK-cell population. J Immunol Res 2015; 2015: 839684.
Tai YT, Anderson KC . Targeting B-cell maturation antigen in multiple myeloma. Immunotherapy 2015; 7: 1187–1199.
Xu S, Lam KP . B-cell maturation protein, which binds the tumor necrosis factor family members BAFF and APRIL, is dispensable for humoral immune responses. Mol Cell Biol 2001; 21: 4067–4074.
O'Connor BP, Raman VS, Erickson LD, Cook WJ, Weaver LK, Ahonen C et al. BCMA is essential for the survival of long-lived bone marrow plasma cells. J Exp Med 2004; 199: 91–98.
Moreaux J, Legouffe E, Jourdan E, Quittet P, Reme T, Lugagne C et al. BAFF and APRIL protect myeloma cells from apoptosis induced by interleukin 6 deprivation and dexamethasone. Blood 2004; 103: 3148–3157.
Novak AJ, Darce JR, Arendt BK, Harder B, Henderson K, Kindsvogel W et al. Expression of BCMA, TACI, and BAFF-R in multiple myeloma: a mechanism for growth and survival. Blood 2004; 103: 689–694.
Carpenter RO, Evbuomwan MO, Pittaluga S, Rose JJ, Raffeld M, Yang S et al. B-cell maturation antigen is a promising target for adoptive T-cell therapy of multiple myeloma. Clin Cancer Res 2013; 19: 2048–2060.
Yong KL, Germaschewski FM, Rodriguez-Justo M, Bounds D, Lee L, Mayes PA et al. Evaluation Of BCMA as a therapeutic target in multiple myeloma using an antibody-drug conjugate. Blood 2013; 122: 4447–4447.
Quinn J, Glassford J, Percy L, Munson P, Marafioti T, Rodriguez-Justo M et al. APRIL promotes cell-cycle progression in primary multiple myeloma cells: influence of D-type cyclin group and translocation status. Blood 2011; 117: 890–901.
Sanchez E, Li M, Kitto A, Li J, Wang CS, Kirk DT et al. Serum B-cell maturation antigen is elevated in multiple myeloma and correlates with disease status and survival. Br J Haematol 2012; 158: 727–738.
Tai YT, Mayes PA, Acharya C, Zhong MY, Cea M, Cagnetta A et al. Novel anti-B-cell maturation antigen antibody-drug conjugate (GSK2857916) selectively induces killing of multiple myeloma. Blood 2014; 123: 3128–3138.
Chauhan D, Singh AV, Brahmandam M, Carrasco R, Bandi M, Hideshima T et al. Functional interaction of plasmacytoid dendritic cells with multiple myeloma cells: a therapeutic target. Cancer Cell 2009; 16: 309–323.
Markovina S, Callander NS, O'Connor SL, Xu G, Shi Y, Leith CP et al. Bone marrow stromal cells from multiple myeloma patients uniquely induce bortezomib resistant NF-kappaB activity in myeloma cells. Mol Cancer 2010; 9: 176.
Elgueta R, de Vries VC, Noelle RJ . The immortality of humoral immunity. Immunol Rev 2010; 236: 139–150.
Tai YT, Acharya C, An G, Moschetta M, Zhong MY, Feng X et al. APRIL and BCMA promote human multiple myeloma growth, chemoresistance, and immunosuppression in the bone marrow microenvironment. Blood 2016; 127: 3225–3236.
Friedrich M, Henn A, Raum T, Bajtus M, Matthes K, Hendrich L et al. Preclinical characterization of AMG 330, a CD3/CD33-bispecific T-cell-engaging antibody with potential for treatment of acute myelogenous leukemia. Mol Cancer Ther 2014; 13: 1549–1557.
Friedrich M, Raum T, Lutterbuese R, Voelkel M, Deegen P, Rau D et al. Regression of human prostate cancer xenografts in mice by AMG 212/BAY2010112, a novel PSMA/CD3-Bispecific BiTE antibody cross-reactive with non-human primate antigens. Mol Cancer Ther 2012; 11: 2664–2673.
Bolliger AP, Fontaine M . Cytological examination and cellular composition of bone marrow in healthy, adult, cynomolgus monkeys (Macaca fascicularis). Comparative Haematol Int 1998; 8: 183–190.
Brandl C, Haas C, d'Argouges S, Fisch T, Kufer P, Brischwein K et al. The effect of dexamethasone on polyclonal T cell activation and redirected target cell lysis as induced by a CD19/CD3-bispecific single-chain antibody construct. Cancer Immunol Immunother 2007; 56: 1551–1563.
Ali SA, Shi V, Maric I, Wang M, Stroncek D, Brudno JN et al. Remissions of multiple myeloma during a first-in-humans clinical trial of T cells expressing an anti-B-cell maturation antigen chimeric antigen receptor. Blood 2015; 128: 1688–1700.
Acknowledgements
We thank Kathrin Bauer from Boehringer Ingelheim; Markus Voelkel, Katja Matthes, Andrea Pullner and Sandra Kerstan from Amgen (Research) Munich; and Chirag Acharya and Kenneth Wen from the Dana Farber Cancer Institute for excellent technical support. We also thank all clinical members of the Jerome Lipper Multiple Myeloma Center of the Dana Farber Cancer Institute for their support and help for this study. This work was also supported by National Institutes of Health Grants RO1050947, R01-CA178264, PO1-CA078378 and DF/HCC SPORE in Multiple Myeloma P50CA100707; KA is an American Cancer Society Clinical Research Professor.
Author contributions
SH, PA, Y-TT, KA, BR and MF conceptualized the research, and formed the hypothesis of this paper. SH, PD and Y-TT designed the in vitro experiments, collected and analyzed the data. DB, JW, MF, OT and BR designed, performed and analyzed the animal work. SH and Y-TT wrote the manuscript. All the authors have critically evaluated the manuscript and approved the final version.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
SH, PJA and DB are employees of Boehringer Ingelheim. PD, JW, OT, BR and MF are Amgen employees and have received stock. KA serves on advisory boards to Takeda, Celgene, Gilead, and is a scientific founder of Acetylon, Oncopep and C4 Therapeutics. The remaining author declares no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Leukemia website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Hipp, S., Tai, YT., Blanset, D. et al. A novel BCMA/CD3 bispecific T-cell engager for the treatment of multiple myeloma induces selective lysis in vitro and in vivo. Leukemia 31, 1743–1751 (2017). https://doi.org/10.1038/leu.2016.388
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2016.388
This article is cited by
-
Efficacy and safety of bispecific antibodies vs. immune checkpoint blockade combination therapy in cancer: a real-world comparison
Molecular Cancer (2024)
-
GPRC5D as a novel target for the treatment of multiple myeloma: a narrative review
Blood Cancer Journal (2024)
-
A novel T cell-redirecting anti-GPRC5D × CD3 bispecific antibody with potent antitumor activity in multiple myeloma preclinical models
Scientific Reports (2024)
-
The present and future of bispecific antibodies for cancer therapy
Nature Reviews Drug Discovery (2024)
-
Revolutionizing cancer treatment: comprehensive insights into immunotherapeutic strategies
Medical Oncology (2024)