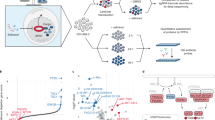
Abstract
Although TP53 mutations are rare in acute myeloid leukemia (AML), wild type p53 function is habitually annulled through overexpression of MDM2 or through various mechanisms including epigenetic silencing by histone deacetylases (HDACs). We hypothesized that co-inhibition of MDM2 and HDACs, with nutlin-3 and valproic acid (VPA) would additively inhibit growth in leukemic cells expressing wild type TP53 and induce p53-mediated apoptosis. In vitro studies with the combination demonstrated synergistic induction of apoptosis in AML cell lines and patient cells. Nutlin-3 and VPA co-treatment resulted in massive induction of p53, acetylated p53 and p53 target genes in comparison with either agent alone, followed by p53 dependent cell death with autophagic features. In primary AML cells, inhibition of proliferation by the combination therapy correlated with the CD34 expression level of AML blasts. To evaluate the combination in vivo, we developed an orthotopic, NOD/SCID IL2rγnull xenograft model of MOLM-13 (AML FAB M5a; wild type TP53) expressing firefly luciferase. Survival analysis and bioluminescent imaging demonstrated the superior in vivo efficacy of the dual inhibition of MDM2 and HDAC in comparison with controls. Our results suggest the concomitant targeting of MDM2-p53 and HDAC inhibition, may be an effective therapeutic strategy for the treatment of AML.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Burnett A, Wetzler M, Lowenberg B . Therapeutic advances in acute myeloid leukemia. J Clin Oncol 2011; 29: 487–494.
Estey E, Dohner H . Acute myeloid leukaemia. Lancet 2006; 368: 1894–1907.
Laubach J, Rao AV . Current and emerging strategies for the management of acute myeloid leukemia in the elderly. Oncologist 2008; 13: 1097–1108.
Wojcik I, Szybka M, Golanska E, Rieske P, Blonski JZ, Robak T et al. Abnormalities of the P53, MDM2, BCL2 and BAX genes in acute leukemias. Neoplasma 2005; 52: 318–324.
Claus R, Lubbert M . Epigenetic targets in hematopoietic malignancies. Oncogene 2003; 22: 6489–6496.
Vassilev LT, Vu BT, Graves B, Carvajal D, Podlaski F, Filipovic Z et al. In vivo activation of the p53 pathway by small-molecule antagonists of MDM2. Science 2004; 303: 844–848.
Kojima K, Konopleva M, Samudio IJ, Shikami M, Cabreira-Hansen M, McQueen T et al. MDM2 antagonists induce p53-dependent apoptosis in AML: implications for leukemia therapy. Blood 2005; 106: 3150–3159.
Gerstner T, Bell N, Konig S . Oral valproic acid for epilepsy--long-term experience in therapy and side effects. Expert Opin Pharmacother 2008; 9: 285–292.
Bruserud O, Stapnes C, Ersvaer E, Gjertsen BT, Ryningen A . Histone deacetylase inhibitors in cancer treatment: a review of the clinical toxicity and the modulation of gene expression in cancer cell. Curr Pharm Biotechnol 2007; 8: 388–400.
Ryningen A, Stapnes C, Lassalle P, Corbascio M, Gjertsen BT, Bruserud O . A subset of patients with high-risk acute myelogenous leukemia shows improved peripheral blood cell counts when treated with the combination of valproic acid, theophylline and all-trans retinoic acid. Leuk Res 2009; 33: 779–787.
Bellos F, Mahlknecht U . Valproic acid and all-trans retinoic acid: meta-analysis of a palliative treatment regimen in AML and MDS patients. Onkologie 2008; 31: 629–633.
Quintas-Cardama A, Santos FP, Garcia-Manero G . Histone deacetylase inhibitors for the treatment of myelodysplastic syndrome and acute myeloid leukemia. Leukemia 2011; 25: 226–235.
Xu WS, Parmigiani RB, Marks PA . Histone deacetylase inhibitors: molecular mechanisms of action. Oncogene 2007; 26: 5541–5552.
Chrisanthar R, Knappskog S, Lokkevik E, Anker G, Ostenstad B, Lundgren S et al. CHEK2 mutations affecting kinase activity together with mutations in TP53 indicate a functional pathway associated with resistance to epirubicin in primary breast cancer. PLoS One 2008; 3: e3062.
Wergeland L, Sjoholt G, Haaland I, Hovland R, Bruserud O, Gjertsen BT . Pre-apoptotic response to therapeutic DNA damage involves protein modulation of Mcl-1, Hdm2 and Flt3 in acute myeloid leukemia cells. Mol Cancer 2007; 6: 33.
Bredholt T, Dimba EA, Hagland HR, Wergeland L, Skavland J, Fossan KO et al. Camptothecin and khat (Catha edulis Forsk.) induced distinct cell death phenotypes involving modulation of c-FLIPL, Mcl-1, procaspase-8 and mitochondrial function in acute myeloid leukemia cell lines. Mol Cancer 2009; 8: 101.
Lorens JB, Jang Y, Rossi AB, Payan DG, Bogenberger JM . Optimization of regulated LTR-mediated expression. Virology 2000; 272: 7–15.
Chou TC . Drug combination studies and their synergy quantification using the Chou-Talalay method. Cancer Res 2010; 70: 440–446.
Keith CT, Borisy AA, Stockwell BR . Multicomponent therapeutics for networked systems. Nat Rev Drug Discov 2005; 4: 71–78.
Kawagoe R, Kawagoe H, Sano K . Valproic acid induces apoptosis in human leukemia cells by stimulating both caspase-dependent and -independent apoptotic signaling pathways. Leuk Res 2002; 26: 495–502.
Bug G, Schwarz K, Schoch C, Kampfmann M, Henschler R, Hoelzer D et al. Effect of histone deacetylase inhibitor valproic acid on progenitor cells of acute myeloid leukemia. Haematologica 2007; 92: 542–545.
McCormack E, Micklem DR, Pindard LE, Silden E, Gallant P, Belenkov A et al. In vivo optical imaging of acute myeloid leukemia by green fluorescent protein: time-domain autofluorescence decoupling, fluorophore quantification, and localization. Mol Imaging 2007; 6: 193–204.
Kumamoto K, Spillare EA, Fujita K, Horikawa I, Yamashita T, Appella E et al. Nutlin-3a activates p53 to both down-regulate inhibitor of growth 2 and up-regulate mir-34a, mir-34b, and mir-34c expression, and induce senescence. Cancer Res 2008; 68: 3193–3203.
Li M, Luo J, Brooks CL, Gu W . Acetylation of p53 inhibits its ubiquitination by Mdm2. J Biol Chem 2002; 277: 50607–50611.
Palani C, Beck J, Sonnemann J . Histone deacetylase inhibitors enhance the anticancer activity of nutlin-3 and induce p53 hyperacetylation and downregulation of MDM2 and MDM4 gene expression. Invest New Drugs 2010; e-pub ahead of print 3 August 2010; doi:10.007/s10637-010-9510-7.
Tasdemir E, Chiara Maiuri M, Morselli E, Criollo A, D'Amelio M, Djavaheri-Mergny M et al. A dual role of p53 in the control of autophagy. Autophagy 2008; 4: 810–814.
Baehrecke EH . Autophagy: dual roles in life and death? Nat Rev Mol Cell Biol 2005; 6: 505–510.
Gu L, Zhu N, Findley HW, Zhou M . MDM2 antagonist nutlin-3 is a potent inducer of apoptosis in pediatric acute lymphoblastic leukemia cells with wild-type p53 and overexpression of MDM2. Leukemia 2008; 22: 730–739.
Ito A, Kawaguchi Y, Lai CH, Kovacs JJ, Higashimoto Y, Appella E et al. MDM2-HDAC1-mediated deacetylation of p53 is required for its degradation. Embo J 2002; 21: 6236–6245.
Lau LM, Nugent JK, Zhao X, Irwin MS . HDM2 antagonist Nutlin-3 disrupts p73-HDM2 binding and enhances p73 function. Oncogene 2008; 27: 997–1003.
Blaheta RA, Michaelis M, Natsheh I, Hasenberg C, Weich E, Relja B et al. Valproic acid inhibits adhesion of vincristine- and cisplatin-resistant neuroblastoma tumour cells to endothelium. Br J Cancer 2007; 96: 1699–1706.
Long J, Parkin B, Ouillette P, Bixby D, Shedden K, Erba H et al. Multiple distinct molecular mechanisms influence sensitivity and resistance to MDM2 inhibitors in adult acute myelogenous leukemia. Blood 2010; 116: 71–80.
Hu B, Gilkes DM, Farooqi B, Sebti SM, Chen J . MDMX overexpression prevents p53 activation by the MDM2 inhibitor Nutlin. J Biol Chem 2006; 281: 33030–33035.
Khanim FL, Bradbury CA, Arrazi J, Hayden RE, Rye A, Basu S et al. Elevated FOSB-expression; a potential marker of valproate sensitivity in AML. Br J Haematol 2009; 144: 332–341.
McCormack E, Bruserud O, Gjertsen BT . Animal models of acute myelogenous leukaemia—development, application and future perspectives. Leukemia 2005; 19: 687–706.
Pearce DJ, Taussig D, Zibara K, Smith LL, Ridler CM, Preudhomme C et al. AML engraftment in the NOD/SCID assay reflects the outcome of AML: implications for our understanding of the heterogeneity of AML. Blood 2006; 107: 1166–1173.
Agliano A, Martin-Padura I, Mancuso P, Marighetti P, Rabascio C, Pruneri G et al. Human acute leukemia cells injected in NOD/LtSz-scid/IL-2Rgamma null mice generate a faster and more efficient disease compared to other NOD/scid-related strains. Int J Cancer 2008; 123: 2222–2227.
Sarek G, Ojala PM . p53 reactivation kills KSHV lymphomas efficiently in vitro and in vivo: new hope for treating aggressive viral lymphomas. Cell Cycle 2007; 6: 2205–2209.
Acknowledgements
This study was supported by The Norwegian Cancer Society (Kreftforeningen), The Western Norway Regional Health Authority (E.Mc.C. and B.T.G.) and Bergen Research Foundation. We thank Lena F Hansen, Lene M Vikebø, Michaela Popa, Maren Boge, Kjetil Jacobsen, Jørn Skavland, Bjarte S Erikstein, Andre Sulen, Paulina Ruurs, Lasse Evensen, Marianne Enger, Randi Hovland, Harald Valen, Lars Helgeland, Edith Fick, Line Bjørge, Liv Cecilie Vestrheim and Reidar Myklebust for discussion, expert advice and technical assistance. The optical imaging and transmission electron microscopy was performed at the Molecular Imaging Center (FUGE, Norwegian Research Council), University of Bergen.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Leukemia website
Supplementary information
Rights and permissions
About this article
Cite this article
McCormack, E., Haaland, I., Venås, G. et al. Synergistic induction of p53 mediated apoptosis by valproic acid and nutlin-3 in acute myeloid leukemia. Leukemia 26, 910–917 (2012). https://doi.org/10.1038/leu.2011.315
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2011.315
Keywords
This article is cited by
-
A proteolysis-targeting chimera molecule selectively degrades ENL and inhibits malignant gene expression and tumor growth
Journal of Hematology & Oncology (2022)
-
Modulation of phospho-proteins by interferon-alpha and valproic acid in acute myeloid leukemia
Journal of Cancer Research and Clinical Oncology (2019)
-
Gene and protein analysis reveals that p53 pathway is functionally inactivated in cytogenetically normal Acute Myeloid Leukemia and Acute Promyelocytic Leukemia
BMC Medical Genomics (2017)
-
CITED2 affects leukemic cell survival by interfering with p53 activation
Cell Death & Disease (2017)
-
Anti-proliferative activity of the NPM1 interacting natural product avrainvillamide in acute myeloid leukemia
Cell Death & Disease (2016)