Abstract
Tight junctions (TJs) restrict the transit of ions and molecules through the paracellular route and act as a barrier to regulate access of inflammatory cells into the airway lumen. The pathophysiology of cystic fibrosis (CF) lung disease is characterised by abnormal ion and fluid transport across the epithelium and polymorphonuclear (PMN) leukocyte-dominated inflammatory response. Na+/H+ exchanger regulatory factor 1 (NHERF1) is a protein involved in PKA-dependent activation of CFTR by interacting with CFTR via its PDZ domains and with ezrin via its C-terminal domain. We have previously found that the NHERF1-overexpression dependent rescue CFTR-dependent chloride secretion is due to the re-organisation of the actin cytoskeleton network induced by the formation of the multiprotein complex NHERF1–RhoA–ezrin–actin. In this context, we here studied whether NHERF1 and CFTR are involved in the organisation and function of TJs. F508del CFBE41o− monolayers presented nuclear localisation of zonula occludens (ZO-1) and occludin as well as disorganisation of claudin 1 and junction-associated adhesion molecule 1 as compared with wild-type 16HBE14o− monolayers, paralleled by increased permeability to dextrans and PMN transmigration. Overexpression of either NHERF1 or CFTR in CFBE41o− cells rescued TJ proteins to their proper intercellular location and decreased permeability and PMN transmigration, while this effect was not achieved by overexpressing either NHERF1 deprived of ezrin-binding domain. Further, expression of a phospho-dead ezrin mutant, T567A, increased permeability in both 16HBE14o− cells and in a CFBE clone stably overexpressing NHERF1 (CFBE/sNHERF1), whereas a constitutively active form of ezrin, T567D, achieved the opposite effect in CFBE41o− cells. A dominant-negative form of RhoA (RhoA-N19) also disrupted ZO-1 localisation at the intercellular contacts dislodging it to the nucleus and increased permeability in CFBE/sNHERF1. The inhibitor Y27632 of Rho kinase (ROCK) increased permeability as well. Overall, these data suggest a significant role for the multiprotein complex CFTR–NHERF1–ezrin–actin in maintaining TJ organisation and barrier function, and suggest that the RhoA/ROCK pathway is involved.
Similar content being viewed by others
Main
Cystic fibrosis (CF) is a lethal recessive autosomal disease due to mutations in the CFTR (cystic fibrosis transmembrane conductance regulator) gene on the long arm of chromosome 7. CF is a multiorgan disease whose pathological hallmark is the dehydration of epithelial secretions that form mucus plugs; however, the lung disease is the chief cause of morbidity and mortality in these patients. The most common mutation of the CFTR gene associated with CF causes deletion of phenylalanine at residue 508 (F508del CFTR) and an improperly folded CFTR protein, which, while being partially functional and responsive to cAMP/PKA regulation, is unable to reach the surface membrane due to retention and/or accelerated degradation in the ER. The lack of a functional CFTR protein on the apical side of the airway epithelium is thought to result in an impairment of mucociliary clearance1 and ensuing opportunistic bacterial infections.2 As a consequence, an atypical chronic inflammatory response against bacteria is mounted,3 with polymorphonuclear (PMN) cells being the predominant cell type infiltrating the airways.4
Apical localisation of CFTR protein and its chloride channel activity strictly depend on interactions of its PDZ (for postsynaptic density 95/disclarge/zona occludens)-interacting domain in the C terminus with other proteins primarily localised to the apical surfaces of epithelial cells, such as Na+/H+ exchanger regulatory factor 1 (NHERF1).5, 6, 7 Overexpression of NHERF1 in CF airway epithelial cells induces also apical localisation of F508del CFTR, recovering its chloride channel activity.7 NHERF1 is a scaffold protein that interacts through its ezrin/radixin/moesin (ERM) domain with ezrin, which associates with actin,8 and actin has been shown to regulate localisation and organisation of tight junction (TJ) proteins.9 The TJs, which are the most apical structure of the junctional complex, act as a selective permeability barrier to the paracellular space (gate function).10 In this way, the TJs are key regulators of ion and solute homeostasis. Furthermore, the TJs prevent the airborne contaminants that are carried into the lungs from entering the submucosa (barrier function), which is essential in the airway for lung defence.11 The TJ also has an important role in the migration of immune cells across the paracellular space during inflammation and immune surveillance.12, 13 TJs are multiprotein complexes composed of proteins that may be divided into three groups:11, 14 (1) integral TJ proteins that bridge the apical intercellular space and form a regulated permeability barrier (occludin, claudins, and junction-associated adhesion molecules (JAMs)); (2) TJ plaque proteins, many of which express PDZ domains that serve as links between the integral TJ proteins and the actin cytoskeleton, and as adaptors for the recruitment of cytosolic molecules implicated in cell signalling (proteins of the ZO family); (3) a miscellaneous group of cytosolic and nuclear proteins, including regulatory proteins, tumour suppressors, and transcriptional and posttranscriptional factors.
Previously, we have demonstrated that NHERF1 overexpression rescues CFTR-dependent chloride secretion by forming the RhoA–ROCK–ezrin–actin multiprotein complex that via actin cytoskeleton re-organisation stabilizes F508del CFTR on the apical membrane tethering it to the cytoskeleton.15 Here studying the role of NHERF1 and CFTR in TJ organisation and gate/barrier function using polarised cultures of human bronchial epithelial cell lines, we demonstrate that NHERF1 and CFTR overexpression in CF cell monolayers induces the re-organisation of TJ proteins to intercellular junctions, reduces the paracellular permeability to small solutes, and mitigate the elevated PMN transmigration across the epithelium.
MATERIALS AND METHODS
Cell Lines
Experiments were performed with the following human bronchial epithelial cell lines: 16HBE14o− cells obtained from a non-CF subject, CFBE41o− cells, homozygous for the F508del allele (a generous gift from Prof. D Gruenert, University of California, San Francisco, CA), and CFBE41o− cells stably transfected with the wild-type NHERF1 cDNA (sNHERF1) or with the empty vector pcDNA3.1 (spcDNA), as previously described.15 Cells were grown in Eagle’s minimal essential medium (MEM; Sigma-Aldrich, Milan, Italy) supplemented with 10% fetal bovine serum, L-glutamine, and penicillin/streptomycin (PAA Pasching, Austria) at 37 °C under 5% CO2. The stably transfected clones were maintained in presence of Hygromycin B (Calbiochem, Milan, Italy) positive selection. Cells were routinely grown on plastic flasks coated with an extracellular matrix containing fibronectin/vitrogen/bovine serum albumin. The extracellular matrix coating was prepared as follows: 10 μg/ml fibronectin adhesion-promoting peptide (BD Biosciences, Milan, Italy), 100 μg/ml albumin from bovine serum (Sigma-Aldrich), and 30 μg/ml bovine collagen type I (BD Biosciences) were dissolved in MEM. The mixture was sterilised by 0.2-μm filter. Each substrate plastic, glass, or permeable support was coated with the mixture for 2 h at 37 °C before cell seeding.
Reverse Transcription-PCR for TJ Genes
Total RNA (1 μg) from 16HBE14o− and CFBE41o− cells was extracted by TRIzol (Invitrogen, Milan, Italy) and retro-transcribed in the presence of 2.5 units Retro transcriptase (Applied Biosystems, Monza, Italy), 0.4 μM of primer, 4 mM of nucleotide mix and commercial buffer (Applied Biosystems) under the following conditions: initial incubation for 10 min at 25 °C, followed by 120 min at 37 °C and for 25 s at 85 °C. The primer sets for amplification were designed to work at the same PCR conditions and are presented in Supplementary Table 1. PCR was performed under the following conditions: initial denaturation for 2 min at 94 °C, followed by 25 cycles of denaturation (15 s, 94 °C), annealing (30 s, 58 °C) and extension (1 min, 72 °C). In the PCR, cDNAs (100 ng) were used in the presence of 1 unit Taq polymerase (Fermentas, Burlington, Canada), 0.4 μM of each primer (MWG, Germany), 0.2 mM of nucleotide mix and commercial buffer (Fermentas) containing 2.5 mM MgCl2 (Fermentas). The identity of amplified products was confirmed by determination of molecular size on agarose gel electrophoresis (1.5% agarose in buffer containing 40 mM Tris/acetate and 1 mM EDTA) and visualised by ethidium bromide staining (0.5 μg/ml) under ultraviolet light.
Transfections
Cells were seeded on 6.5-mm diameter Transwell (Corning, Acton, MA, USA) at 1 × 105 per filter and grown with medium in the upper and lower chambers. After 5–6 days, cells were transiently transfected with 2.5 μg of plamidic DNA by using Escort IV or Lipofectamine 2000 reagent (for the ezrin constructs) according to the manufacturer’s protocol, and the experiments were conducted 48 h later.
Transepithelial Resistance Measurement
The transepithelial resistance (TER) of cells grown on Transwells was monitored daily with a volt-ohm meter (Millicell-ERS; Millipore, Vimodrone, Italy) and recorded for each well before and after the transfection of each cell monolayer at days 5–6. The average TER measurement of Transwells in the absence of a cell monolayer was 25 Ω·cm2. Prior to transfections, TER values in 16HBE14o− and CFBE41o− cells were 489±50 and 101±8.7 Ω·cm2, respectively (n=20 for each cell line), after subtracting blank values obtained with empty Transwells.
Plasmids
Wild-type NHERF1 and NHERF1-ΔERM encoding NHERF1 truncated of the last 30 amino acids inserted in pcDNA3.1/Hygro+ vector were generously provided by Prof. EJ Weinman (University of Maryland Hospital, Baltimore, MD). The dominant-negative RhoA, RhoA-N19 3xHA tagged (N-terminus), inserted into pcDNA3.1/Hygro+ vector, was provided by Missouri S&T cDNA Resource Center (Rolla, MO), and the constitutively active form of RhoA, RhoA-V14, inserted into pEGFP-C1, was generously provided by Prof. E Klussmann (Leibniz-Institut fur Molekulare Pharmakologie, Berlin, Germany). Wild-type CFTR inserted in pcDNA3.1 was already described.16 CFTR K1468X lacking the 12 C-terminal amino acids,17 inserted into pTM1, was generously provided by Prof. MJ Welsh (University of Iowa, Iowa City, USA). Human ezrin cDNA constructs (wild-type, active (T567D), and negative (T567A)-dominant form) were in the pEGFP-N1 vector as described by Favia et al15 and Di Sole et al.18
CFTR 1–633 aa was generated as follows: pBQ6.2 plasmid (gently provided by Dr Johanna Rommens, Hospital for Sick Children, Toronto, Canada) containing full-length CFTR was digested with SmaI and BamHI, and the resulting cDNA (first 1430 bp of CFTR) was inserted into pRRL.CMV.MCS.MM vector provided by Dr L Naldini (HS Raffaele Scientific Institute, Milan, Italy). A PCR product corresponding to 1431–1899 bp of CFTR was generated using the following primers: 5′-GATAGAAAGAGGACAGTTGTTG-3′ (forward) and 5′-GTGGCTAGCGAGTTCTGAAAATGT-3′ (reverse) using pBQ6.2 plasmid as template and cloned in pBSMYC2 (pBluescript containing a myc-tag, gently provided by Dr L Naldini) via BamHI and NheI in frame with a myc-tag. Then, this portion of CFTR (1431–1899 bp) fused with myc was inserted in frame in pRRL.CMV.MCS.MM containing first 1430 bp of CFTR. The transfection of 293T cells (which do not express endogenous CFTR) resulted in both c-myc and CFTR intracellular staining (data not shown).
Immunofluorescence
Monolayers were washed three times with PBS, fixed in 3% paraformaldehyde and 2% sucrose in PBS and permeabilised with ice-cold Triton HEPES buffer (20 mM HEPES, 300 mM sucrose, 50 mM NaCl, 3 mM MgCl2, 0.5% Triton X-100, pH 7.4) for 5 min at room temperature. Cells were incubated with blocking solution (2% BSA and 2% FBS), for 15 min at 37 °C, then with fluorescein isothiocyanate (FITC)-conjugated mouse anti-zonula occluden (ZO-1) antibody or FITC-conjugated mouse anti-occludin antibody (dilution 1:50; Zymed Laboratories, San Francisco, CA, USA) for 30 min at 37 °C, or with unconjugated mouse anti-claudin 1 and unconjugated rabbit anti-JAM-1 antibodies (both dilution 1:50; Zymed) followed by FITC-conjugated secondary antibodies directed against the primary antibodies (dilution 1:100; Sigma-Aldrich). Cells were rinsed three times with 0.2% BSA, then filters were excised and placed side up on a glass slide, and overlayed with a drop of Fluorescent mounting medium (Dako, Milan, Italy) followed by a coverslip. Cells were analysed using Nikon TE2000 microscope coupled to a Radiance 2100 confocal dual-laser scanning microscopy system (Bio-Rad, Segrate, Italy). Specimens were viewed through a × 60 oil-immersion objective. The microscope was equipped with a FITC filter (excitation 395 nm, emission 509 nm). Digital images were processed using the programme Laser Sharp 2000 (Bio-Rad).
In order to evaluate the localisation of TJ proteins to the plasma membrane, monolayers were fixed, treated with TRITC-conjugated Wheat Germ Agglutinin (50 μg/ml in PBS, Sigma-Aldrich) for 10 min at room temperature, washed extensively for 1 h with PBS, permeabilised and finally incubated with either anti-ZO-1 or anti-occludin antibody, both FITC-conjugated, in the conditions above described. Localisation to the nuclei was investigated by fixation, permeabilisation, incubation with FITC-conjugated antibodies, and subsequent treatment with propidium iodide (0.1 μg/ml in PBS) for 5 min at room temperature. Confocal analysis was performed as above described.
Western Blotting Analysis
Untransfected CFBE and CFBE transfected with several plasmidic DNA grown on polyethylene terephthalate permeable filters (0.4-μm-pore size, 4.2 cm2 of growth area; BD Falcon) were lysed in lysis buffer (110 mM NaCl, 50 mM Tris, 0.5% Triton X-100 and 0.5% Igepal CA-630, pH 8.0, added with protease inhibitors), as previously described.7 Thirty micrograms of proteins for each sample were separated on 6% SDS–polyacrylamide gels. Proteins were transferred to polyvinylidene difluoride membranes, blocked with Tris-buffered saline with Tween 20 (T-TBS; containing 10 mM Tris (pH 7.4), 150 mM NaCl, and 5 mM KCl with 0.1% (vol/vol) Tween 20) with 5% (wt/vol) milk. Blots were incubated over night at 4 °C with specific primary antibodies: mouse monoclonal anti-ZO-1 (Invitrogen, clone ZO1-1A12) diluted 1:500 or mouse monoclonal anti-β-tubulin (Sigma-Aldrich) diluted 1:5000. After washing, blots were incubated with anti-mouse secondary antibody conjugated to horseradish peroxidase (Sigma-Aldrich) diluted 1:2000. Detection of bound antibodies was performed with the ECL plus reagent (GE Healthcare Life Sciences), and densitometric quantification and image processing were carried out using Adobe Photoshop and the Image software package (version 1.61, National Institutes of Health, Bethesda, MD).
Paracellular Permeability
FITC-conjugated dextrans were added to the apical compartment 48 h after transfection of monolayers, and then the fluorescence in the basolateral compartment was measured at different times as described.19 FITC-dextrans of different molecular weight (10 kDa (10 s) and 2000, kDa (2000, s); Sigma-Aldrich) were added to the apical side of monolayers and after 10, 30, and 50 min the apparent permeability (pAPP) was calculated by measuring the fluorescence in the basal medium. Cytochalasin D (Sigma-Aldrich) treatment was performed for 30 min (10 μM); ROCK inhibitor Y27632 (Sigma-Aldrich) was used at 1 μM for 12 h prior to paracellular permeability analysis.
PMN Transmigration
Normal human PMNs were isolated from noncoagulated citrated blood by Ficoll-Paque (Amersham Pharmacia Biotech, Uppsala, Sweden) density sedimentation as per the manufacturer’s instructions and were suspended in HBSS (Sigma-Aldrich).
The transmigration through the epithelium was evaluated in physiologically relevant basolateral to apical direction (the so-called ‘down’ mode) in monolayers grown on 3-μm-pore filters as previously described.20 Briefly, 7 × 104 cells were plated on the bottom of Transwells (Corning) for 48 h and then the filters were inverted. Medium was added both in the lower and upper compartments. After 6–8 days from seeding of epithelial cells, PMNs were added in the upper compartment (106 per filter), ie, from the basolateral side, while in the lower compartment, ie, from the apical side, 1 μM N-formyl-methionyl-leucyl-phenylalanin (Sigma-Aldrich) was added. After 150 min, PMNs that crossed the epithelium were recovered in the lower compartment and quantified by flow cytometry, and data were expressed as percentage of total PMN added in the upper compartment.
Data Analysis
Data are presented as mean±s.d. for the number of samples indicated (n). Statistical comparisons were made using Mann–Whitney test. Differences were considered significant when P<0.05.
RESULTS
Expression and Localisation of TJ Proteins
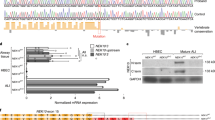
To obtain a detailed picture of which TJ proteins are expressed by both 16HBE14o− (16HBE) and CFBE41o− (CFBE) cells, we first performed a prior RT-PCR analysis. As ZO-1, occludin, JAM-1, and claudins 1, 3, 4, 5 are expressed by the respiratory human epithelium in situ,19, 21 sense and antisense primers for these genes were designed. Supplementary Figure 1 displays the mRNA expression of TJ proteins upon formation of polarised monolayers. Both CFBE and 16HBE cells expressed claudin 1, ZO-1, occludin, and JAM-1, whereas only 16HBE cells expressed claudin 4. On the basis of these results, we chose to carry on the evaluation of ZO-1, occludin, claudin 1, and JAM-1 proteins by confocal microscopy.
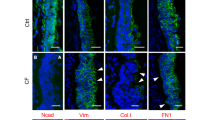
16HBE cells, expressing wild-type CFTR, showed a typical chicken-wire pattern of ZO-1 expression on the xy axis, whereas CFBE cells, homozygous for the F508del mutation, were characterised by a dislocation of ZO-1 in the cytosol and nucleus (Figure 1a). The xz axis projection shows that ZO-1 localises at the apical region of 16HBE cells. Furthermore, 16HBE cells display the same pattern for occludin, claudin 1, and JAM-1 expression on the xy axis, with the xz axis showing that these proteins localise at the apical region (Supplementary Figures 2–4). In CFBE cells, these proteins are not expressed in an organised manner and this could be appreciated in both xy and xz views. In particular, occludin has a nuclear distribution (Supplementary Figure 2), claudin 1 is poorly expressed on the plasma membrane (Supplementary Figure 3), and JAM-1 expression is barely detectable (Supplementary Figure 4). These results were compatible with the different TER recorded in the two cell lines, with higher TER values in 16HBE cells than in CFBE cells (489±50 and 101±8.7 Ω·cm2, respectively, n=20 for each cell line).
Effect of CFTR and NHERF1 overexpression on ZO-1 organisation. (a) Confocal analysis on cell monolayers was performed with a FITC-conjugated anti-ZO-1 antibody in 16HBE, untransfected CFBE, and 48 h after transfection of CFBE cells with CFTR or NHERF1 or with truncated form NHERF1/ΔERM or truncated form CFTR-NH2. 16HBE control cells, expressing wild-type CFTR, showed a typical chicken-wire pattern of ZO-1 expression on the xy axis, whereas CFBE cells, homozygous for the F508del mutation, were characterised by a diffuse cytosol/nuclear staining. Overexpression of wild-type NHERF1 or CFTR partially recovered the localisation of ZO-1 at the TJ location, while transfection of NHERF1/ΔERM did not exert any effect. Transfection of CFTR-NH2 had a less pronounced effect than wild-type CFTR, leading to a cytosolic localisation of ZO-1. xy, horizontal section; xz, vertical section. Arrow in each xy panel indicates the level of xz reslice. Images were obtained with an original magnification of × 60 and after zooming ( × 2.5). Scale bar: 10 μm. (b) ZO-1 protein expression in untransfected CFBE and CFBE transfected with NHERF1, NHERF1/ΔERM, or CFTR grown on permeable filters. (i) Representative western blot. ZO-1 antibody detected a band at 225 kDa and the equality of loading is shown with β-tubulin. (ii) Semi-quantitative data of the ZO-1 signal from (i) was normalised with β-tubulin signal. Data from three experiments are shown as mean±s.d. The mean value of CFBE is used as arbitral value of 1.
In order to establish the localisation of ZO-1 and occludin in the two cell lines, we performed confocal analysis to co-localise the specific signal of TJ proteins with either plasma membrane or nuclei counter-staining. As shown in Supplementary Figure 5, in 16HBE cells, ZO-1 localised to the plasma membrane and was not found at the nuclear level, while occludin signal was mostly found at the plasma membrane and some in the nuclei. In contrast, in CFBE cells, ZO-1 and occludin were localised to the nuclei, whereas the plasma membrane signal was negligible. Overall, these data indicate that CFBE cells present a dislocation of TJ proteins at the nuclear level in basal condition.
NHERF1 and CFTR Overexpression Restores Protein Localisation at the TJs of CFBE Cells
In order to determine the effect of overexpression of NHERF1 and CFTR on TJ organisation, we performed transient transfections on CFBE cell monolayers with plasmids encoding for: (1) wild-type NHERF1; (2) wild-type CFTR; (3) N-terminal portion of CFTR (CFTR-NH2, corresponding to amino acids 1–633), which is able to transcomplement and rescue the processing of the F508del CFTR22; and (4) NHERF1, in which the C-terminus domain that interacts with ezrin is deleted (NHERF1/ΔERM). Then, 48 h after transfections, we performed an immunofluorescence assay on transfected cells with FITC-conjugated anti-ZO-1 antibody and analysed samples by confocal microscopy.
As shown in Figure 1a, overexpression of wild-type NHERF1 as well as transfection of wild-type CFTR cDNA recovered the localisation of ZO-1 at the TJ location in CFBE cell monolayers, mostly in a cytosolic juxtamembranar domain, while overexpression of NHERF1/ΔERM did not exert any effect. On the other hand, transfection of CFTR-NH2 had a less pronounced effect than wild-type CFTR, leading to cytosolic localisation of ZO-1.
In addition, to evaluate if this ZO-1 distribution consequent to transfection was associated to different protein expression levels we performed western blot analysis in CFBE cells grown on permeable filters. Transfection of CFBE cells with NHERF1, CFTR, or ΔERM did not provoke a change in ZO-1 protein levels as compared with untransfected cells (Figure 1b). Overall, these data indicate a role for multiprotein complex CFTR–NHERF1–ezrin in the re-localisation of TJ proteins with no effect at their protein expression level.
However, transfection of CFBE cells with wild-type NHERF1 or CFTR cDNA, although partially re-organising ZO-1 expression at the TJ location, did not modify TER (data not shown), suggesting that a total re-organisation of TJs is necessary to obtain a TER equivalent to that of non-CF cells. Indeed, it has been previously suggested that TER, a measure of the ‘gate’ function, does not strictly correlate with distribution of either occludin or ZO-1 at the TJs.23
To confirm that NHERF1 overexpression determines ZO-1 re-organisation in CFBE cells, we analysed CFBE/sNHERF1 cells that showed ZO-1 at the correct TJ location in comparison with a control transfected clone pcDNA3.1 (not shown). Although CFBE/sNHERF1 presented a distinct pattern (increased apical CFTR expression and activity and phospho-ezrin expression at the level of the apical membrane, increased RhoA activity),15 which made this clone similar to wild-type 16HBE cells, CFBE/sNHERF1 and the control clone CFBE/spcDNA exhibited a similar TER (107±12 and 93±6 Ω·cm2, respectively, n=15 for each cell line). Again, the results of these measurements strongly suggest that TER might not be a sensitive marker for TJ re-organisation.
Overall, these data indicate that CFTR and NHERF1 overexpression recover the disorganised location of ZO-1 protein in CF cells and suggest that this effect depends on the interaction between the CFTR C-terminus and NHERF1, and on the capability of NHERF1 to interact with the actin cytoskeleton via the mediation of ezrin.
To see whether the effect of NHERF1 or CFTR overexpression determined an overall re-organisation of TJs, claudin 1, occludin, and JAM-1 localisation was evaluated by confocal microscopy. Overexpression of wild-type NHERF1 and wild-type CFTR cDNAs partially recovered the localisation of these proteins at the TJ location (Supplementary Figures 2–4). Transfection of CFTR-NH2 and K1468X gave no effect on occludin, while in case of claudin 1 and JAM-1 it produced a less pronounced effect than transfection of wild-type CFTR and NHERF1 (Supplementary Figures 2–4). Overall, these results confirm a possible role for the C-terminus of CFTR in the re-organisation of TJs.
Effect of CFTR and NHERF1 Overexpression on TJ Permeability
To evaluate whether the re-organisation of TJs induced by overexpression of NHERF1 and CFTR could affect TJ function, paracellular permeability to small solutes such as dextrans of different molecular weight (10 kDa (10s) and 2000, kDa (2000s)) was measured. FITC-conjugated dextrans were added to the apical compartment 48 h after transfection of monolayers, and the fluorescence in the basolateral compartment was measured at different times as described.19 Passage of dextrans from apical to basolateral compartment was expressed as pAPP. The two dextrans with such difference in molecular weight were chosen to pick up subtle differences in TJ permeability. 16HBE cells showed a significantly lower pAPP in comparison with CFBE cells with both dextrans, confirming a higher organisation of TJs (Figure 2). Overexpression of NHERF1-ΔERM in 16HBE and CFBE/sNHERF1 cells resulted in a significant increased permeability only with the smallest 10s dextran. In CFBE cells, 48 h after transfection with wild-type NHERF1 and CFTR a significant decrease in pAPP was observed with both dextrans, indicating a lower permeability to small solutes. CFBE/sNHERF1 showed a significant lower permeability to 10s dextran in comparison with stably transfected empty vector pcDNA3.1 clone (CFBE/spcDNA), whereas the decrease with 2000s dextran was not significant (Figure 2). Overall, these data strongly indicate a role for CFTR and NHERF1 in mediating TJ organisation and function. The increase in apparent permeability in 16HBE and CFBE/sNHERF1 after transfection with NHERF1 truncated of its ERM domain (Figure 2) confirms the role of NHERF1 in stabilising TJs and fostering their barrier function via the formation of the multiprotein complex NHERF1–ezrin–actin.
Effect of wild-type NHERF1, NHERF1/ΔERM, and CFTR overexpression on pAPP in 16HBE and CFBE cells. FITC-dextrans (10s, upper panel or 2000s, lower panel) were added to the apical side of monolayers, and after 10, 30, and 50 min the apparent permeability (pAPP) was calculated by measuring the fluorescence in the basal medium. pAPP was measured in: untreated CFBE cells and 48 h after transfection with wild-type CFTR or wild-type NHERF1 constructs; untreated 16HBE cells and 48 h after transfection with ΔERM; untreated clone stably expressing wild-type NHERF1 (CFBE/sNHERF1) and 48 h after transfection with ΔERM and in untreated control clone stably transfected with pcDNA3.1 (CFBE/spcDNA). Each bar represents the mean±s.d.
Effect of NHERF1 Overexpression on PMN Transmigration
We then studied the effect of TJ organisation and function on the capacity of PMN in crossing the epithelial monolayer. The transmigration through the epithelium has been evaluated in the physiologically relevant basolateral to apical direction (‘down’ mode) in monolayers grown on 3 μm-pore filters as previously described.20 As expected, fMLP increased the rate of migration across all cell monolayers (Figure 3). CFBE and CFBE/spcDNA monolayers had a three- to fourfold higher rate of PMN transmigration than 16HBE cells both in the absence or presence of fMLP. Importantly, the overexpression of NHERF1 in CFBE significantly reduced the transmigration rate, confirming the important role of NHERF1 in the barrier function of TJs.
Effect of TJ organisation on the capacity of PMN in crossing the epithelial monolayer. The transmigration through the epithelium has been evaluated in physiologically relevant basolateral to apical direction (‘down’ mode) in monolayers grown on 3-μm-pore filters. Cells were plated on the bottom of Transwells (7 × 104) for 48 h and then the filters were inverted. After 6–8 days from seeding of epithelial cells, PMN (1 × 106 for filter) were added in the upper compartment, ie, from the basolateral side. In the lower compartment, ie, from the apical side, 1 μM N-formyl-methionyl-leucyl-phenylalanin (fMLP), a neutrophils chemoattractant, was added (black bars) or not (white bars). After 150 min, PMNs that crossed the epithelium were recovered in the lower compartment and quantified by flow cytometry, and data were expressed as percentage of total PMN added in the upper compartment. Each bar represents the mean±s.d.
Role of Ezrin in TJ Organisation and Function
We had previously shown in CFBE/sNHERF1 cells that transfection with cDNA encoding for the phospho-dead ezrin mutant, T567A, which cannot be phosphorylated, resulted in a significantly lower interaction between NHERF1 and actin,15 demonstrating that the phosphorylation of ezrin at Thr567 is a key step in the formation of the multiprotein complex NHERF1–ezrin–actin. Therefore, we sought to determine whether the inactive T567A form of ezrin could disrupt TJ function. Cytochalasin D treatment, used as positive control, determined an increase of permeability in both 16HBE and CFBE/sNHERF1 cell monolayers (Figure 4). The overexpression of the T567A construct in both 16HBE and CFBE/sNHERF1 monolayers determined a significant increase in the TJ permeability with both dextrans (Figure 4). Note that in 16HBE cells the difference was significant also with 2000s dextran, although the very close values (4.54 × 10−8±1.44 × 10−8 vs 8.09 × 10−8±8.50 × 10−9, n=6 and n=4, respectively). The overexpression of phospho-dead ezrin mutant did not cause any effect on pAPP in CFBE cells with both dextrans (Figure 4). These data indicate that the effect of NHERF1 on TJ structure and function is mediated by the ezrin activation and its influence on F-actin organisation (Ref. 12 and M Favia et al, manuscript in preparation). On the basis of the these results, we next investigated the effect of the overexpression of the constitutively active form of ezrin (T567D) on the permeability of TJ in CFBE cells. The overexpression of ezrin T567D as well as of wild-type ezrin resulted in a significant decrease in TJ permeability (Figure 4), further supporting the importance of ezrin phosphorylation in the stabilisation of the cytoskeleton–TJ complex.
Effect of ezrin phosphorylation on pAPP. FITC-dextrans (10s, upper panel or 2000s, lower panel) were added to the apical side of monolayers, and after 10, 30, and 50 min the apparent permeability (pAPP) was calculated by measuring the fluorescence in the basal medium. pAPP was measured in: untreated CFBE cells and 48 h after transfection with ezrin T567D, ezrin T567A, or wild-type ezrin constructs; untreated 16HBE cells and 48 h after transfection with T567A ezrin; untreated clone stably expressing wild-type NHERF1 (CFBE/sNHERF1) and 48 h after transfection with ezrin T567A. As a positive control, cytochalasin D treatment determined an increase of permeability in both 16HBE and CFBE/sNHERF1 cells. Each bar represents the mean±s.d.
To further confirm the role of ezrin in TJ organisation, we performed an immunofluorescence assay on filters to detect the organisation of ZO-1, 48 h after the transfection of CFBE with T567D or wild-type ezrin. We observed that the overexpression of ezrin T567D induced a partial re-organisation of ZO-1 protein at the level of TJs, as evaluated by confocal microscopy in comparison with CFBE and CFBE cells transfected with wild-type ezrin (Figure 5). Transfection with wild-type ezrin resulted in a moderate ZO-1 re-organisation.
Effect of ezrin overexpression on ZO-1 localisation in CFBE cell monolayers. Confocal analysis was performed 48 h after the transfection of CFBE cells with ezrin T567D or wild-type ezrin. The overexpression of ezrin T567D induced a partial re-organisation of ZO-1 protein at the level of TJs in comparison with untransfected CFBE cells. Transfection with wild-type ezrin resulted in a very moderate ZO-1 re-organisation. xy, horizontal section; xz, vertical section. Arrow in each xy panel indicates the level of xz reslice. Images were obtained with an original magnification of × 60 and after zooming ( × 2.5). Scale bar: 10 μm.
Role of RhoA in TJ Organisation and Function
We have previously shown that RhoA is involved in the NHERF1-induced assembling of actin stress fibres in CF cells.15 Thus, we sought to determine the involvement of RhoA in TJ re-organisation and function. The role of RhoA in TJ re-organisation was investigated in the CFBE clone stably expressing NHERF1. While in the control clone (stably transfected with empty pcDNA3.1 vector) ZO-1 was confined to the nuclei, CFBE/sNHERF1 cells exhibited a cytosolic juxtamembranar localisation of ZO-1 (Figure 6). NHERF1-ΔERM expression resulted in the loss of ZO-1 from the intercellular location and its accumulation in the nucleus. Interestingly, also the dominant-negative form of RhoA (RhoA-N19) disrupted ZO-1 localisation at the intercellular contacts relocating ZO-1 to the nuclear level, whereas this effect was not observed with the dominant-positive form of RhoA (RhoA-V14).
Involvement of RhoA in ZO-1 organisation in CFBE/sNHERF1 cell monolayers. Confocal analysis detected that CFBE/sNHERF1 cells exhibited a plasma membrane localisation of ZO-1, whereas the control CFBE/spcDNA clone showed a nuclear signal. The overexpression of NHERF1/ΔERM determined the loss of ZO-1 from the intercellular location with nuclear localisation. The dominant-negative form of RhoA (RhoA-N19) disrupted ZO-1 localisation at the intercellular contacts with accumulation in the nuclei, whereas this effect was not observed with the dominant-positive form of RhoA (RhoA-V14). xy, horizontal section; xz, vertical section. Arrow in each xy panel indicates the level of xz reslice. Images were obtained with an original magnification of × 60 and after zooming ( × 2.5). Scale bar: 10 μm.
The change in ZO-1 localisation in CFBE stably expressing NHERF1 upon overexpression of RhoA dominant forms was correlated with pAPP measurement. With 10s dextran, RhoA-N19 increased significantly TJ permeability, while RhoA-V14 had no such effect (Figure 7). As a control, the effect of RhoA-V14 was investigated in CFBE cells and results showed that pAPP was significantly decreased with 10s dextran, while RhoA-N19 was without effect (Figure 7). With 2000s dextran, the effect of Rho-N19 was not noted in any cell line. Permeability increased after treatment with 1 μM Rho Kinase (ROCK) selective inhibitor (Y27632)24 using both 10s and 2000s dextrans in CFBE/sNHERF1 and also in 16HBE cells, despite very close pAPP values with the 2000s dextran (4.52 × 10−8±1.22 × 10−8 vs 8.99 × 10−8±7.21 × 10−9, n=6 and n=4, respectively). These data corroborate the role of RhoA in the regulation of the structure and the barrier function of TJs, as it has been demonstrated in other cell types.25, 26
Effect of RhoA on pAPP in 16HBE, CFBE/sNHERF1, and CFBE cells. FITC-dextrans (10s, upper panel or 2000s, lower panel) were added to the apical side of monolayers. pAPP was measured in: untreated monolayers cells and 48 h after transfection with RhoA-N19 or RhoA-V14. 16HBE and CFBE/sNHERF1 monolayers were also treated with 1 μM Rho Kinase (ROCK) selective inhibitor Y27632 for 12 h prior to measure paracellular permeability. Each bar represents the mean±s.d.
DISCUSSION
NHERF1–CFTR Interaction is Involved in TJ Organisation and Gate Function
CFTR localisation to the apical plasma membrane and its function are regulated by a macromolecular complex, mainly mediated by the binding of CFTR to several PDZ-domain-containing proteins, including NHERF1, NHERF2, and CAP70 (CFTR-associated protein, 70 kDa, also known as NHERF3).27 NHERF1 and NHERF2 have a C-terminal ERM-binding domain, which interacts with ezrin, radixin, or moesin to tether CFTR to the apical actin cytoskeleton in polarised epithelial cells,28, 29 and CFTR in the plasma membrane is stabilised by NHERF1 and ezrin, through its binding to the submembrane actin network. Thus, NHERF1 seems to have a central role in the intracellular trafficking and function of wild-type CFTR, and we have also highlighted the importance of NHERF1 in CF airway epithelial cells. Indeed, F508del CFTR can be coaxed to the plasma membrane by the overexpression of NHERF1,7 an effect mediated by the increase of actin cytoskeleton organisation.15
As TJ cytoplasmatic plaque proteins function as a bridge between the TJ and the actin cytoskeleton,11, 30 we have extended our study of the role of NHERF1 to TJ organisation and function. Indeed, we report here that, in comparison to non-CF 16HBE cells, CFBE cells have a reduced localisation of ZO-1 and other proteins at the TJs, along with confinement of ZO-1 and occludin in the nucleus, and a correspondingly higher permeability to both dextrans and PMN transmigration. Wild-type NHERF1 and CFTR overexpression in CF airway epithelial cells can determine a relocation of TJ proteins to the intercellular borders that is mirrored by the reconstitution of the gate function of TJs. To validate these differences in a homogeneous genetic background, we compared the morphological and functional properties of TJs between a CFBE clone overexpressing NHERF1 and a control clone, confirming the correction of the pathological features in the NHERF1-overexpressing clone. The overexpression of NHERF1-ΔERM inhibited NHERF1-induced correction of ZO-1 localisation (Figure 6), bringing to a phenotype similar to CFBE cells (as shown in Figure 1a). On the basis of our data, we suggest that the CFTR carboxyl terminus and the ERM domain of NHERF1 are involved not only in the formation of actin fibres,15 but also in the re-organisation of TJ structure and resumption of altered TJ function, likely by forming a multiprotein complex located in the cortical region of the cell.
The diminished location of ZO-1 and occludin proteins at the level of the TJs in CFBE cells could be the result of minor expression, as also suggested by the RT-PCR data (Supplementary Figure 1), although this assay served only to demonstrate mRNA expression of TJ proteins and was not quantitative. However, other data point out to a differential localisation of ZO-1 and occludin proteins in CFBE cells rather than to a differential protein level: (i) counter-staining used in confocal analysis showing ZO-1 and occludin cytosol and nuclear localisation (Supplementary Figure 5); (ii) western blotting analysis demonstrating that NHERF1 or CFTR overexpression in CFBE cells did not modify ZO-1 levels (Figure 1b) in face of a functional recovery of CFBE cells as TJ permeability function (Figure 2). Occludin nuclear localisation has been described, and its relocation to cell junctions, together with ZO-1, is associated with reaction to cyclic strain in the vascular endothelium,31 suggesting that the switch between nuclear sequestration and junctional complexes could be a major molecular rearrangement in response to physical strain. This could be of major importance in CF, as the surface airway epithelium is constantly subjected to cyclic mechanical strain.32
While the role of CFTR in the transcellular transport of ions is well known, its the role in paracellular permeability and gate function of the airway epithelium is less known but is at present an intensive field of investigation.33, 34, 35 Although we did not analyse here the role of NHERF1 and CFTR in the paracellular permeability to ions, our results are in line with those obtained by LeSimple et al,33 who demonstrated that the presence of membrane CFTR is required for normal epithelial gate function, and with Weiser et al,35 who recently showed that CFBE cell monolayers exhibit a higher paracellular permeability and lower TER (as in our study here) as compared with 16HBE monolayers. In particular, LeSimple et al33 argued that CFTR trafficking is required for the normal organisation and function of TJs, although the increase in gate function upon overexpression of CFTR was not affected by the CFTR inhibitor CFTRinh-172 or low-chloride medium, implying that the effect of CFTR on TJ function was unrelated to its ion channel activity. This observation may be coupled with the coaxing of CFTR to the plasma membrane and reduction in its turnover (ie, longer permanence of CFTR at this level) induced by NHERF1 overexpression demonstrated by us,15 although we do not know the effect of CFTR inhibition on the resumption of TJ permeability defect in CFBE cells upon NHERF1 overexpression. On the same line, Weiser et al35 showed that while cAMP induced an increase of paracellular permeability in 16HBE cells, in contrast CFBE cells respond to cAMP stimulation with a decrease of paracellular permeability paralleled by slight increase of TER, indicating that there is a link between CFTR dysfunction and an improper regulation of the paracellular transport route. Finally, Nilsson et al34 tried to link paracellular ion transport, CFTR activity, and cellular cytoskeleton organisation. In keeping with our previous findings,15 they show that CFBE cells display disorganised actin stress fibres and a blurred network at the cell boundaries, while 16HBE cells are characterised by organised actin fibres at the cell borders. However, in contrast CFBE monolayers exhibited a higher TER and lower permeability as compared with CFBE corrected with CFTR expressed stably by a Epstein–Barr virus-based expression vector. These findings are difficult to reconcile with the results presented in this paper, as we found a significant higher permeability in CFBE monolayers in comparison with wild-type 16HBE cells and a resumption of the permeability upon NHERF1 or CFTR overexpression. It could be that the use of different methods to recover the CF defect (adenoviral vs plasmid-derived overexpression) as well as the transgene (CFTR vs NHERF1) could be responsible for the difference in the results. Additionally, TJ protein localisation was not tested by Nilsson et al.34
At least two classes of trans-TJ pathways with differing size and charge selectivity exist: a high-capacity, charge selective pore pathway that is able to carry large quantities of small uncharged solutes, and a low-capacity leak pathway that allows only small quantities of larger molecules to pass, regardless of charge.36 As Na+ and Cl− flux are responsible for the transepithelial current and they do not discriminate between pore and leak pathways, TER cannot be used to measure TJ size or charge selectivity. For this reason, increased permeability of either pathway reduces TER. In our hands, CFBE and the CFBE clone stably expressing NHERF1 displayed very similar low TER, whereas there was a significant difference in the barrier function to macromolecules such as dextrans. Whether CFBE cells modify their TJ configuration from a leak pathway to a pore one upon overexpression of NHERF1 is still to be determined. In the case of the TJs of CFBE it is possible to see that the 2000s dextran could better permeate CFBE cell monolayers as compared with 16HBE cells (Figures 2, 4, and 7). The large 2000s dextran may be less sensitive to smaller changes in the pore permeability, thus the different treatments have less effect on the permeation of this macromolecule than that obtained with the small 10s dextran. This in accordance with the fact that larger paracellular permeability for molecules with smaller effective hydrodynamic radius has been shown.34
CFTR–NHERF1 Interaction is Involved in the TJ Barrier Function and PMN Transmigration
In CF, the dysregulated innate inflammatory/immune response of CF airway epithelial cells may result from either the direct effects of CFTR on cellular signalling or inflammatory mediator production, or from indirect effects resulting from the absence of CFTR apical membrane channel function.37 While the exaggerated PMN influx in the airway lumen of CF patients4 is due to increased cytokine and chemokine levels,38, 39, 40 the mechanism of PMN transmigration has not been yet studied. Here we provide evidence that CF airway epithelial cell monolayers have a leaky barrier function, allowing a pathophysiologically relevant higher PMN migration, ie, from the serosal to the luminal surface. Our data strongly indicate that NHERF1 overexpression-directed CFTR relocation to the apical plasma membrane induced relocation of TJ proteins paralleled by restoration of the barrier function towards normal levels. Our results are different from those obtained by Pizurki and Morris41 who evaluated PMN transmigration in a F508del CFTR cell line with high TER (200–800 Ω·cm2). They observed that adenovirus-mediated transduction of either wild-type CFTR or F508del CFTR did not produce any difference in PMN migration rate. The lack of effect might be due to the high TER presented by the CF cell line used in their study. Future studies should be directed to determine whether the leaky barrier in CF cells could be due to altered interaction between PMN and epithelial cells,20 as suggested by the increased phosphorylation of the regulatory L-chain of myosin II (MLC) at the actomyosin ring, which is likely involved in TJ opening to allow PMN passage. The detailed knowledge of the steps of the transepithelial migration process could be relevant to design drugs to inhibit the proinflammatory process typical of CF.
Ezrin and the RhoA/ROCK Pathway are Implicated in NHERF1-Mediated Effect on TJs in CF Cells
The ERM protein, ezrin, is a linker between cell membranes and the cytoskeleton, and is localised in the apical actin-rich regions of polarised epithelial cells where it promotes stress fibre assembly and cortical actin polymerisation in response to activation of RhoA.42 It has been found that the active, open form of ezrin co-localises with NHERF1 at or near the plasma membrane of polarised cells where they reciprocally stabilise each other and function together in organising macromolecular complexes.43 Ezrin activity is regulated by intramolecular interactions between its own N-(FERM) and C-terminal binding sites.8 In the inactive, cytosolic state this intramolecular interaction masks its NHERF1 and actin-binding sites, and two events appear to be required for ERM protein activation: interaction of phosphatidylinositol 4,5-bisphosphate (PIP2) with the FERM domain of ezrin and phosphorylation of T567 in the COOH terminal region.8, 44 PIP2 is a general regulator of actin polymerisation at the plasma membrane,45 and it has been demonstrated to be required for the activation and translocation of ERM proteins to the membrane, while T567 phosphorylation is required for maintaining its active state.46 Active RhoA-GTP affects ezrin activation by the involvement of its effectors ROCK and/or phosphatidylinositol-4-phosphate 5-kinase (PIPK).47, 48 RhoA-mediated activation of PIPK elevates the intracellular level of PIP2, which, in turn, stabilizes the ERM proteins in an open conformation, thereby permitting phosphorylation at T567. We previously demonstrated the role of ezrin phosphorylation in the recruitment of F508del CFTR to the apical plasma membrane by inducing the formation of the multiprotein CFTR–NHERF1–ezrin–actin complex. The increase in apparent permeability in 16HBE and CFBE/sNHERF1 cells by overexpression of phospho-dead mutant of ezrin and corresponding decrease when the active mutant was expressed (Figure 4), strongly indicate that phospho-ezrin is also involved in a multiprotein complex directing re-organisation of TJ proteins.
The small GTPase RhoA is an important regulator of actin-based cytoskeletal organisation.49 We have found15 that NHERF1 overexpression in CFBE induced RhoA activation and, additionally, that transfection of CFBE cells with the dominant active mutant of RhoA, RhoA-V14, increased (i) phosphorylated ezrin in the membrane fraction (ii) F-actin content, and importantly, (iii) rescued CFTR-dependent chloride efflux of CFBE cells similarly to that observed during NHERF1 overexpression. In this study, the dominant-negative form of RhoA (RhoA-N19) disrupted ZO-1 localisation at the TJ level and increased permeability to dextrans restoring the CFBE phenotype, an effect not observed with the dominant active RhoA-V14. Our results are in agreement with previous studies, in which the inhibition of RhoA either by C3 transferase (a Clostridium botulinum toxin that selectively blocks RhoA-effector coupling by ADP-ribosylation), or overexpression of dominant-negative RhoA resulted in the disassembly of TJs in various epithelial cell lines.23, 25, 26, 50 Furthermore, the ROCK inhibitor Y27632 has been shown to increase permeability in various cell types,24, 51 although in one study treatment of 16HBE cells with Y27632 resulted in decreased Staphylococcus aureus transmigration across monolayers.52 While this opposite result could be due to the use of a different method to investigate epithelial permeability, another important difference is that the signal cascade elicited by S. aureus mediated not a re-organisation of TJ proteins but their proteolysis. Therefore, the different signalling cascade caused by bacterial infection, involving EGFR, MAPK pathway activation and MLC phosphorylation, might account for this opposite effect, as in our case NHERF1 overexpression seems to dictate another pathway involving ezrin and actin in undamaged cells. The investigation of MLC phosphorylation in CFBE before and after NHERF1 overexpression should clarify this issue.
It remains to be clarified which mediators are at work in linking RhoA/ROCK to the TJ organisation and function. A significant body of evidence has accumulated in recent years indicating that the crosstalk of diverse signalling pathways modulate the barrier function of TJs.53 Assembly of TJs is directly regulated by phosphorylation of ZO-1, claudins, and occludin and indirectly by phosphorylation of MLC.53 During the formation of intercellular junctions, the phosphorylation of TJ proteins is mainly due to protein kinase C and the small GTPase RhoA through its effector ROCK,51, 54 whereas both ROCK and MLC kinase are primarily responsible for MLC phosphorylation.55, 56
In conclusion, the work presented here highlights the close relationship among CFTR, NHERF1, and TJ organisation and function. The correction of the CF phenotype by NHERF1 overexpression in terms of gate/barrier function holds promise for identifying novel gene and drug-based approaches for the correction of the basic defect in CF and inflammatory responses.
References
Boucher RC . Cystic fibrosis: a disease of vulnerability to airway surface dehydration. Trends Mol Med 2007;13:231–240.
Campodonico VL, Gadjeva M, Paradis-Bleau C et al. Airway epithelial control of Pseudomonas aeruginosa infection in cystic fibrosis. Trends Mol Med 2008;14:120–133.
Conese M, Copreni E, Di Gioia S et al. Neutrophil recruitment and airway epithelial cell involvement in chronic cystic fibrosis lung disease. J Cyst Fibros 2003;2:129–135.
Hubeau C, Lorenzato M, Couetil JP et al. Quantitative analysis of inflammatory cells infiltrating the cystic fibrosis airway mucosa. Clin Exp Immunol 2001;124:69–76.
Moyer BD, Denton J, Karlson KH et al. A PDZ-interacting domain in CFTR is an apical membrane polarization signal. J Clin Invest 1999;104:1353–1361.
Li C, Naren AP . Macromolecular complexes of cystic fibrosis transmembrane conductance regulator and its interacting partners. Pharmacol Ther 2005;108:208–223.
Guerra L, Fanelli T, Favia M et al. Na+/H+ exchanger regulatory factor isoform 1 overexpression modulates cystic fibrosis transmembrane conductance regulator (CFTR) expression and activity in human airway 16HBE14o− cells and rescues DeltaF508 CFTR functional expression in cystic fibrosis cells. J Biol Chem 2005;280:40925–40933.
Bretscher A, Edwards K, Fehon RG . ERM proteins and merlin: integrators at the cell cortex. Nat Rev Mol Cell Biol 2002;3:586–599.
Ivanov AI, Hunt D, Utech M et al. Differential roles for actin polymerization and a myosin II motor in assembly of the epithelial apical junctional complex. Mol Biol Cell 2005;16:2636–2650.
Van Itallie CM, Anderson JM . The role of claudins in determining paracellular charge selectivity. Proc Am Thorac Soc 2004;1:38–41.
Schneeberger EE, Lynch RD . The tight junction: a multifunctional complex. Am J Physiol Cell Physiol 2004;286:C1213–1228.
Edens HA, Parkos CA . Modulation of epithelial and endothelial paracellular permeability by leukocytes. Adv Drug Deliv Rev 2000;41:315–328.
Chin AC, Parkos CA . Pathobiology of neutrophil transepithelial migration: implications in mediating epithelial injury. Annu Rev Pathol 2007;2:111–143.
Forster C . Tight junctions and the modulation of barrier function in disease. Histochem Cell Biol 2008;130:55–70.
Favia M, Guerra L, Fanelli T et al. Na+/H+ exchanger regulatory factor 1 overexpression-dependent increase of cytoskeleton organization is fundamental in the rescue of F508del cystic fibrosis transmembrane conductance regulator in human airway CFBE41o− cells. Mol Biol Cell 2010;21:73–86.
Biffi A, Sersale G, Cassetti A et al. Restoration of bacterial killing activity of human respiratory cystic fibrosis cells through cationic vector-mediated CFTR gene transfer. Hum Gene Ther 1999;10:1923–1930.
Hall RA, Ostedgaard LS, Premont RT et al. A C-terminal motif found in the β2-adrenergic receptor, P2Y1 receptor and cystic fibrosis transmembrane conductance regulator determines binding to the Na+/H+ exchanger regulatory factor family of PDZ proteins. Proc Natl Acad Sci USA 1998;95:8496–8501.
Di Sole F, Babich V, Moe OW . The calcineurin homologous protein-1 increases Na(+)/H(+)-exchanger 3 trafficking via ezrin phosphorylation. J Am Soc Nephrol 2009;20:1776–1786.
Coyne CB, Vanhook MK, Gambling TM et al. Regulation of airway tight junctions by proinflammatory cytokines. Mol Biol Cell 2002;13:3218–3234.
Edens HA, Levi BP, Jaye DL et al. Neutrophil transepithelial migration: evidence for sequential, contact-dependent signaling events and enhanced paracellular permeability independent of transjunctional migration. J Immunol 2002;169:476–486.
Coyne CB, Gambling TM, Boucher RC et al. Role of claudin interactions in airway tight junctional permeability. Am J Physiol Lung Cell Mol Physiol 2003;285:L1166–1178.
Cormet-Boyaka E, Hong JS, Berdiev BK et al. A truncated CFTR protein rescues endogenous DeltaF508-CFTR and corrects chloride transport in mice. FASEB J 2009;23:3743–3751.
Jou TS, Schneeberger EE, Nelson WJ . Structural and functional regulation of tight junctions by RhoA and Rac1 small GTPases. J Cell Biol 1998;142:101–115.
Walsh SV, Hopkins AM, Chen J et al. Rho kinase regulates tight junction function and is necessary for tight junction assembly in polarized intestinal epithelia. Gastroenterology 2001;121:566–579.
Gopalakrishnan S, Raman N, Atkinson SJ et al. Rho GTPase signaling regulates tight junction assembly and protects tight junctions during ATP depletion. Am J Physiol 1998;275:C798–809.
Nusrat A, Giry M, Turner JR et al. Rho protein regulates tight junctions and perijunctional actin organization in polarized epithelia. Proc Natl Acad Sci USA 1995;92:10629–10633.
Guggino WB, Stanton BA . New insights into cystic fibrosis: molecular switches that regulate CFTR. Nat Rev Mol Cell Biol 2006;7:426–436.
Short DB, Trotter KW, Reczek D et al. An apical PDZ protein anchors the cystic fibrosis transmembrane conductance regulator to the cytoskeleton. J Biol Chem 1998;273:19797–19801.
Sun F, Hug MJ, Lewarchik CM et al. E3KARP mediates the association of ezrin and protein kinase A with the cystic fibrosis transmembrane conductance regulator in airway cells. J Biol Chem 2000;275:29539–29546.
Gonzalez-Mariscal L, Betanzos A, Nava P et al. Tight junction proteins. Prog Biophys Mol Biol 2003;81:1–44.
Collins NT, Cummins PM, Colgan OC et al. Cyclic strain-mediated regulation of vascular endothelial occludin and ZO-1: influence on intercellular tight junction assembly and function. Arterioscler Thromb Vasc Biol 2006;26:62–68.
Liu M, Tanswell AK, Post M . Mechanical force-induced signal transduction in lung cells. Am J Physiol 1999;277:L667–683.
LeSimple P, Liao J, Robert R et al. Cystic fibrosis transmembrane conductance regulator trafficking modulates the barrier function of airway epithelial cell monolayers. J Physiol 2010;588:1195–1209.
Nilsson HE, Dragomir A, Lazorova L et al. CFTR and tight junctions in cultured bronchial epithelial cells. Exp Mol Pathol 2010;88:118–127.
Weiser N, Molenda N, Urbanova K et al. Paracellular permeability of bronchial epithelium is controlled by CFTR. Cell Physiol Biochem 2011;28:289–296.
Shen L, Weber CR, Raleigh DR et al. Tight junction pore and leak pathways: a dynamic duo. Annu Rev Physiol 2011;73:283–309.
Machen TE . Innate immune response in CF airway epithelia: hyperinflammatory? Am J Physiol Cell Physiol 2006;291:C218–230.
Muhlebach MS, Stewart PW, Leigh MW et al. Quantitation of inflammatory responses to bacteria in young cystic fibrosis and control patients. Am J Respir Crit Care Med 1999;160:186–191.
Muhlebach MS, Noah TL . Endotoxin activity and inflammatory markers in the airways of young patients with cystic fibrosis. Am J Respir Crit Care Med 2002;165:911–915.
McAllister F, Henry A, Kreindler JL et al. Role of IL-17A, IL-17F, and the IL-17 receptor in regulating growth-related oncogene-alpha and granulocyte colony-stimulating factor in bronchial epithelium: implications for airway inflammation in cystic fibrosis. J Immunol 2005;175:404–412.
Pizurki L, Morris MA, Chanson M et al. Cystic fibrosis transmembrane conductance regulator does not affect neutrophil migration across cystic fibrosis airway epithelial monolayers. Am J Pathol 2000;156:1407–1416.
Mackay DJ, Esch F, Furthmayr H et al. Rho- and rac-dependent assembly of focal adhesion complexes and actin filaments in permeabilized fibroblasts: an essential role for ezrin/radixin/moesin proteins. J Cell Biol 1997;138:927–938.
Morales FC, Takahashi Y, Kreimann EL et al. Ezrin-radixin-moesin (ERM)-binding phosphoprotein 50 organizes ERM proteins at the apical membrane of polarized epithelia. Proc Natl Acad Sci USA 2004;101:17705–17710.
Ivetic A, Ridley AJ . Ezrin/radixin/moesin proteins and Rho GTPase signalling in leucocytes. Immunology 2004;112:165–176.
Hilpela P, Vartiainen MK, Lappalainen P . Regulation of the actin cytoskeleton by PI(4,5)P2 and PI(3,4,5)P3. Curr Top Microbiol Immunol 2004;282:117–163.
Yonemura S, Matsui T, Tsukita S . Rho-dependent and -independent activation mechanisms of ezrin/radixin/moesin proteins: an essential role for polyphosphoinositides in vivo. J Cell Sci 2002;115:2569–2580.
Matsui T, Maeda M, Doi Y et al. Rho-kinase phosphorylates COOH-terminal threonines of ezrin/radixin/moesin (ERM) proteins and regulates their head-to-tail association. J Cell Biol 1998;140:647–657.
Matsui T, Yonemura S, Tsukita S et al. Activation of ERM proteins in vivo by Rho involves phosphatidyl-inositol 4-phosphate 5-kinase and not ROCK kinases. Curr Biol 1999;9:1259–1262.
Tapon N, Rho Hall A . Rac and Cdc42 GTPases regulate the organization of the actin cytoskeleton. Curr Opin Cell Biol 1997;9:86–92.
Bruewer M, Hopkins AM, Hobert ME et al. RhoA Rac1, and Cdc42 exert distinct effects on epithelial barrier via selective structural and biochemical modulation of junctional proteins and F-actin. Am J Physiol Cell Physiol 2004;287:C327–335.
Fujita H, Katoh H, Hasegawa H et al. Molecular decipherment of Rho effector pathways regulating tight-junction permeability. Biochem J 2000;346 (Part 3):617–622.
Soong G, Martin FJ, Chun J et al. Staphylococcus aureus protein A mediates invasion across airway epithelial cells through activation of RhoA GTPase signaling and proteolytic activity. J Biol Chem 2011;286:35891–35898.
Gonzalez-Mariscal L, Tapia R, Chamorro D . Crosstalk of tight junction components with signaling pathways. Biochim Biophys Acta 2008;1778:729–756.
Hirase T, Kawashima S, Wong EY et al. Regulation of tight junction permeability and occludin phosphorylation by Rhoa-p160ROCK-dependent and -independent mechanisms. J Biol Chem 2001;276:10423–10431.
Adelstein RS . Calmodulin and the regulation of the actin-myosin interaction in smooth muscle and nonmuscle cells. Cell 1982;30:349–350.
Amano M, Ito M, Kimura K et al. Phosphorylation and activation of myosin by Rho-associated kinase (Rho-kinase). J Biol Chem 1996;271:20246–20249.
Acknowledgements
This work was supported by the Italian Cystic Fibrosis Research Foundation (grant no. FFC1/2009) with the contribution of the ‘Delegazione FFC della Valdadige’; ‘Nicola Petruzzi e Delegazione FFC di Molfetta’; ‘Gli amici di Thomas con la Delegazione FFC di Vibo Valentia’; ‘Delegazione FFC ‘La Bottega delle Donne’ di Montebelluna Treviso’. We thank Stephan Joel Reshkin for critically reading of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Laboratory Investigation website
The abnormal cystic fibrosis (CF) airway epithelial cell tight junctions (TJs) allow excessive neutrophil migration. The role of the multiprotein apical complex CFTR-NHERF1-ezrin-actin in maintaining TJ organization and barrier function implicates the RhoA/ROCK pathway. These findings may help identify novel pathways in the inflammatory reaction in CF.
Rights and permissions
About this article
Cite this article
Castellani, S., Guerra, L., Favia, M. et al. NHERF1 and CFTR restore tight junction organisation and function in cystic fibrosis airway epithelial cells: role of ezrin and the RhoA/ROCK pathway. Lab Invest 92, 1527–1540 (2012). https://doi.org/10.1038/labinvest.2012.123
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2012.123
Keywords
This article is cited by
-
Polarity scaffolds signaling in epithelial cell permeability
Inflammation Research (2021)
-
Mutant CFTR Drives TWIST1 mediated epithelial–mesenchymal transition
Cell Death & Disease (2020)
-
Insulin-like growth factor-6 (IGFBP-6) stimulates neutrophil oxidative burst, degranulation and chemotaxis
Inflammation Research (2018)
-
Strategies for the etiological therapy of cystic fibrosis
Cell Death & Differentiation (2017)
-
Disrupted tight junctions in the small intestine of cystic fibrosis mice
Cell and Tissue Research (2014)