Abstract
Atherosclerosis is increasingly recognized as a chronic inflammatory disease. Angiotensin II (Ang II) is a critical factor in inflammatory responses, so as to promote the pathogenesis of atherosclerosis. Toll-like receptor 4 (TLR4) activates signaling pathways leading to the expression of pro-inflammatory cytokines implicated in the etiology of atherosclerosis. Peroxisome proliferator-activated receptor γ (PPARγ) agonists are considered to be important in modulating vascular inflammation and atherosclerosis. Herein, we investigated the modulatory effects of rosiglitazone on Ang II-mediated inflammatory responses both in vivo and in vitro. We also examined whether TLR4-dependent signaling pathway was involved in the inhibitory effects of rosiglitazone on Ang II-induced pro-inflammatory responses in vascular smooth muscle cells (VSMCs). Male Sprague–Dawley rats received Ang II by subcutaneous infusion and/or rosiglitazone per os for 7 days. Systolic blood pressure rise in Ang II-infused rats was attenuated by rosiglitazone. Rosiglitazone also reduced Ang II-induced generation of pro-inflammatory mediators (TLR4, matrix metalloproteinase-9 and tumor necrosis factor-α), but enhanced production of anti-inflammatory mediators (PPARγ and 6-keto-PGF1α) both in vivo and in vitro. Furthermore, treatment of VSMCs with both the TLR4 inhibitor and TLR4 small-interfering RNA (siRNA) showed that the modulatory effects of rosiglitazone on Ang II-mediated inflammatory responses in VSMCs were related to TLR4. Treatment of the cells with rosiglitazone had little effect on Ang II receptors expression (AT1 and AT2), but downregulated AT1-dependent ERK1/2 activation. Then, treatment of VSMCs with TLR4 siRNA, interferon-gamma-inducible protein 10 (IP-10) siRNA and with the special protein kinase C (PKC) inhibitor further revealed that the signaling pathway (TLR4/IP-10/PKC/NF-κB) was involved in the inhibitory effects of rosiglitazone on Ang II-induced pro-inflammatory responses in VSMCs. In conclusion, TLR4 may be a drug target involved in the ameliorative effects of PPARγ agonist, rosiglitazone, on Ang II-mediated inflammatory responses in VSMCs. Moreover, rosiglitazone exerts its anti-inflammatory effect by interfering with the TLR4-dependent signaling pathway (ERK1/2/TLR4/IP-10/PKC/NF-κB) to prevent and treat atherosclerotic diseases.
Similar content being viewed by others
Main
Cardiovascular diseases are the leading cause of morbidity and mortality all over the world. Atherosclerosis, the background for many cardiovascular diseases, is increasingly recognized as a chronic inflammatory disease.1, 2 Angiotensin II (Ang II), a vasoactive peptide hormone, has been implicated in vascular inflammation and progression of atherosclerosis.3, 4 Ang II causes proliferation and migration of vascular smooth muscle cells (VSMCs),5 release of inflammatory cytokines,6 decrease of prostacyclin (PGI2)7 and production of matrix metalloproteinases (MMPs).8 Therefore, Ang II is an essential factor in inflammatory responses so as to promote the pathogenesis of atherosclerosis, which is also related to activation of the immunological system.9
Recently accumulating interest emerges from the cardiovascular research field in toll-like receptors (TLRs) family. It is now becoming clear that TLRs not only serve as receptors for pathogen-associated molecular patterns, but are also involved in the initiation and progression of cardiovascular pathologies associated with the development of atherosclerosis. TLRs, particularly TLR4, are important players in initiating early inflammatory and functional responses to danger signals arising from inflammatory stimuli. Engagement of TLR4 on the cells by the specific ligand results in the enhancement of inflammatory mediators by nuclear factor-κB (NF-κB).10 Moreover, it has been reported that Ang II upregulates TLR4 and MMP-9 expressions in VSMCs,11, 12 suggesting a strong association between inflammatory responses and atherosclerosis.
The peroxisome proliferator-activated receptors (PPARs) are members of the nuclear receptor superfamily of transcription factors that control the expressions of a large array of genes.13 The PPAR family comprising three members, α, γ and β/δ plays a crucial role, not only in improving glucose and lipid homeostasis but also in the inhibition of vascular inflammation, oxidative stress and atherosclerosis.14, 15 In addition to targeting VSMCs, wherein they suppress proliferation and migration, MMPs production and Ang II receptor type 1 (AT1) expression,16, 17, 18 PPARγ agonists have recently been shown to possess anti-inflammatory and anti-arteriosclerotic properties by antagonizing Ang II effects.19, 20, 21
The TLR4 signaling activates mitogen-activated protein kinases and production of interferon-gamma-inducible protein 10 (IP-10), in turn activating protein kinase C (PKC) and finally resulting in the translocation of NF-κB.22, 23, 24 Recent studies have revealed that the TLR4 signaling plays a central role in atherosclerosis,25, 26, 27 thus providing an important link between inflammation, innate immunity and atherosclerosis. Although PPARγ agonists exert anti-inflammatory and anti-arteriosclerotic actions in the cardiovascular system, the exact mechanisms, whereby rosiglitazone affects Ang II-mediated inflammatory responses, and the TLR4-dependent signaling pathway involved are largely unknown. Accordingly, we examined the effects of rosiglitazone on Ang II-mediated inflammatory responses both in vivo and in vitro to explore the role of TLR4-dependent signaling pathway in the inhibitory effects of rosiglitazone on Ang II-induced inflammatory responses in VSMCs.
MATERIALS AND METHODS
Materials
Dulbecco's modified Eagle's medium (DMEM), fetal bovine serum (FBS), penicillin and streptomycin were purchased from Gibco BRL (Carlsbad, CA, USA). Ang II, lipopolysaccharide (LPS) from Escherichia coli 0111:B4, PD123319, PD098059, phorbol 12-myristate-13 acetate (PMA) and chelerythrine were purchased from Sigma (St Louis, MO, USA). Losartan was purchased from Merk (Merk Corp., Darmstadt, Germany). Rosiglitazone was from Cayman (Ann Arbor, MI, USA). Polyclonal anti-rat TLR4, anti-AT1, anti-PKC, anti-NF-κB and anti-α-smooth muscle actin antibodies were from Santa Cruz Biotechnology (Santa Cruz, CA, USA). Antibodies against PPARγ, PPARα, IP-10 and MMP-9 were from ABCAM (Cambridge, UK). Antibodies against phospho-ERK1/2 and total ERK1/2 were purchased from Cell Signaling Technology (Beverly, MA, USA). Monoclonal anti-TLR4 antibody (MTS510) was from eBioscience (San Diego, CA, USA). Rat tumor necrosis factor-α (TNF-α) ELISA kit was purchased from Bender (Bender MedSystems, CA, USA). Rat 6-keto prostaglandin F1α (6-keto-PGF1α) ELISA kit was purchased from Cayman. Small-interfering RNA (siRNA) specific for TLR4 (siGENOME SMARTpool, M-090819-00), siRNA specific for IP-10 (siGENOME SMARTpool, M-099124-00), negative control siRNA (NC siRNA) (siGENOME Non-Targeting siRNA Pool, D-001206-13-05) and DharmaFECT 2 transfection reagent (T-2002-02) were obtained from Dharmacon (Lafayette, CO, USA).
Animal Experiments
The investigation conforms to the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (NIH Publication No. 85–23, revised 1996). Male Sprague–Dawley rats (weight 200–220 g) were obtained from the Laboratory Animal Institute of School of Medicine of Xi'an Jiaotong University (Xi'an, China). Rats were infused subcutaneously with Ang II at a dose of 150 ng/kg/min or the same volume of 0.9% saline by use of Alzet osmotic minipumps (Alza Corp.) for 7 days. Rosiglitazone (5 or 10 mg/kg/day) dissolved in 0.9% saline was intragastrically administrated for 7 days, starting from the day of Ang II infusion. Systolic blood pressure (SBP) was measured by the tail-cuff method. The animals were killed by injecting excess amount of pentobarbital and the blood was collected from the abdominal aorta for analysis of serum TNF-α and plasma 6-keto-PGF1α levels. One portion of thoracic aorta was dissected and cleaned of fat, then frozen in liquid nitrogen for western blot assay and for RNA extraction, and other portion of thoracic aorta was fixed in 4% formaldehyde solution and embedded in paraffin. Tissue sections (5 μm thick) were prepared for confocal immunohistochemical evaluation.
Radioimmunity Analysis
To detect the effect of rosiglitazone on serum TNF-α and plasma 6-keto-PGF1α levels in Ang II-infused rats, a radioimmunity method was used to measure the contents with the TNF-α and 6-keto-PGF1α Detection Kits (Eastern Asia Radioimmunity Research Institute, Beijing, China) according to the manufacturer's instruction. Radioiodinated TNF-α was produced by the balance method, ranging from 0.3–24.3 ng/ml, to construct the standard curve. The sensitivity of the assay was 0.3 ng/ml. Intra- and inter-assay coefficients of variation were <5 and <8%, respectively. Concentrations of 6-keto-PGF1α, ranging from 25 to 1600 pg/ml, were used to construct the standard curve. The sensitivity of the assay was <25 pg/ml. Intra- and inter-assay coefficients of variation were <3.5 and <10%, respectively. The details of the procedures were reported earlier by Wen et al.28
Immunofluorescent Double Staining of Rat Vessels
For immunofluorescent double staining, deparaffinized sections were fixed in 100% cold methanol, and non-specific proteins were blocked with 1% bovine serum albumin. The sections were incubated with rabbit anti-rat TLR4 antibody (1:200) or anti-rat MMP-9 antibody (1:400), and mouse anti-rat α-actin antibody (1:100) at 4°C overnight. After incubation with appropriate fluorescence-labeled secondary antibody at the room temperature for 1 h, the sections were observed under a confocal microscope (Leica TCS SP2-AOB).
Cell Culture
The VSMCs were isolated from the thoracic aorta of male Sprague–Dawley rats by the explant technique as described earlier.29 The cells were grown in DMEM supplemented with 10% FBS, 100 U/ml penicillin and 100 μg/ml streptomycin in 5% CO2 at 37°C. The cells were used between passages 3 and 10 for all experiments. The cells exhibited the typical ‘hill and valley’ growth morphology and were confirmed positive (99%) for smooth muscle α-actin immunostaining. When the cells were grown to confluence, the medium was changed to serum-free medium for an additional 24 h before the experiments.
Small-Interfering RNA
The VSMCs (5 × 106) were seeded into six-well plates and were grown until 60–80% confluent. The cells were transiently transfected with 150 pM of TLR4 siRNA, 100 nM of IP-10 siRNA or NC siRNA and using DharmaFECT 2 transfection reagent according to the manufacturer's instructions. After 48 h, TLR4 mRNA levels were detected by quantitative real time-PCR and RT-PCR, and IP-10 protein expression was analyzed by western blotting. Transfection rates of 60–70% of the cells were accepted for all the experiments.
ELISA for TNF-α and 6-keto-PGF1α
The cells were seeded into six-well plates at a density of 5 × 106 cells per well, and untreated or incubated with rosiglitazone (2.5, 5 and 10 μM) and Ang II (10−7 M) for the indicated time. In another experiment, the cells were pretreated with anti-TLR4 antibody (1 μg/ml) for 1 h before the addition of rosiglitazone (10 μM) for 1 h, and subsequently stimulated with Ang II (10−7 M) or LPS (100 ng/ml) for 24 h. In addition, after application of NC siRNA or TLR4 siRNA for 48 h, VSMCs were exposed to rosiglitazone (10 μM) for another 1 h, and subsequently stimulated with Ang II (10−7 M) for 24 h. The 6-Keto-PGF1α, the stable degradation product of PGI2, and TNF-α in the culture supernatant of VSMCs were measured by ELISA kits according to the manufacturer's instructions.
Immunofluorescent Staining of VSMCs
To examine the effect of rosiglitazone on TLR4 and MMP-9 expression in Ang II-stimulated VSMCs, the cells were incubated with rosiglitazone (2.5, 5 and 10 μM) for 1 h and then, exposure to Ang II (10−7 M) for 24 h. After the treatment, the cells were fixed with 4% formaldehyde–PBS for 15 min. The cell membranes were fenestrated with 0.3%Triton-100–PBS and nonspecific binding sites were blocked with 10% goat serum. The cells were incubated with rabbit anti-rat TLR4 (1:200) or anti-rat MMP-9 antibody (1:400), and then incubated with the secondary antibody conjugated to fluorescein isothiocyanate. The immunolabeled cells were observed under fluorescence confocal microscopy (Leica TCS SP2-AOB).
Western Blotting
As described earlier,30 protein samples (20 μg) were separated on 12% SDS-PAGE gels and transferred onto a polyvinylidene difluoride membrane (Bio-Rad). The membranes were blocked with 5% nonfat dry milk in Tris-buffered saline containing 0.1% Tween 20, and incubated with specific antibodies against TLR4 (1:200), MMP-9 (1:400), PPARγ (1:400), PPARα (1:100), IP-10 (1:5000), PKC (1:400), NF-κB (1:400) and β-actin (1:400). The expression of β-actin was used as a loading control. Reagents (Pierce) for enhanced chemiluminescence were applied to the blots, and the light signals were detected by X-ray film. Optical densities of the bands were scanned and quantified with the Gel Doc 2000 (Bio-Rad).
Quantitative Real-Time PCR and RT-PCR
The mRNA expression was determined by a modification of our earlier method.31 Total RNA was isolated with TRIzol reagent kit (Invitrogen, CA, USA). The cDNA was synthesized from 1 μg sample of total RNA by using Revert Aid First Strand cDNA Synthesis Kit (Fermentas, St Leon-Rot, Germany) following the manufacturer's instructions. Real-time PCR was carried out with the SuperScript III Platinum SYBR-Green One-Step qRT-PCR kit (Invitrogen) on an Mx3000P QPCR System (Stratagene, LaJolla, CA, USA) following the manufacturer's instructions. Primers for rat TLR4, MMP-9, PPARγ, PPARα and β-actin were designed with Beacon designer v 4.0 (Premier Biosoft, USA) (see Table 1 for the sequences). β-actin was used as an endogenous control. Traditional PCR was carried out according to the manufacturer's instructions. The RT-PCR products were analyzed by electrophoresis through 2% agarose gels containing ethidium bromide. A melting point dissociation curve generated by the instrument was used to confirm that only a single product was present. Quantization of relative gene expression was calculated by the comparative Ct method
) as described by the manufacturer.
Statistical Analysis
Data were expressed as mean±s.e.m. Differences were determined by unpaired Student's t-test and one- or two-way ANOVA followed by Dunnett test. A value of P<0.05 was considered to be statistically significant.
RESULTS
Effect of Rosiglitazone on TNF-α and 6-keto-PGF1α Generations in Ang II-Infused Rats
To investigate the effect of rosiglitazone on TNF-α and 6-keto-PGF1α generations in Ang II-infused rats, we measured serum TNF-α and plasma 6-keto-PGF1α levels by a radioimmunity method. In rosiglitazone (5 and 10 mg/kg)-treated groups, there was evident decrease in TNF-α level (Figure 1a) and increase in 6-keto-PGF1α secretion compared with Ang II-treated group (Figure 1b). The results indicate that rosiglitazone reduces TNF-α production and enhances 6-keto-PGF1α release in Ang II-infused rats.
Contents of serum TNF-α (a) and plasma 6-keto-PGF1α (b) in Ang II-infused rats treated without or with rosiglitazone (Ros) for 7 days as measured by a radioimmunity method. (c) Systolic blood pressure in Ang II-infused rats treated without or with Ros for before (Pre), 3 and 7 days. Results are expressed as mean±s.e.m. (n=6). *P<0.05, **P<0.01 vs control; #P<0.05, ##P<0.01 vs Ang II; †P<0.05 vs Pre in the same group or Ang II+Ros (5 mg/kg).
SBP in Ang II-Infused Rats
The SBP of the rats was evaluated at before, 3 and 7 days after infusion of the Ang II. On the third day, there was not significant difference in SBP among the groups (Figure 1c). After infusion of Ang II for 7 days, SBP was increased, but rosiglitazone at the dose of 5 and 10 mg/kg significantly lowered the rise of SBP.
Immunofluorescent Double Staining of Rat Vessels for TLR4 and MMP-9
Expressions of TLR4 and MMP-9 in the thoracic aorta were identified with immunofluorescent double staining and were observed using a confocal microscope. Representative graphs of each group were shown in Figure 2. Compared with the control group, stronger TLR4 staining on the luminal surface and MMP-9 expression on the media were seen in the Ang II group, whereas TLR4 and MMP-9 expressions were significantly attenuated by rosiglitazone. Identification of smooth muscle cells with the antibody to α-actin to showed that TLR4 and MMP-9 were expressed predominantly in smooth muscle cells in each group. These results show that rosiglitazone remarkably reduces expressions of TLR4 and MMP-9 in the aortic VSMCs in Ang II-infused rats.
Immunofluorescent double staining of vascular smooth muscle tissue with antibodies to TLR4 and MMP-9 in the thoracic aorta of rats receiving Ang II infusion (150 ng/kg/min) for 7 days without or with rosiglitazone (Ros) treatment. Representative TLR4 expression was shown in the smooth muscle cells of the neointima in the control group (a), Ang II group (b), Ang II+Ros (5 mg/kg) group (c) and Ang II+Ros (10 mg/kg) group (d). Representative MMP-9 expression was observed in the smooth muscle cells of the media in control group (e), Ang II group (f), Ang II +Ros (5 mg/kg) group (g) and Ang II+Ros (10 mg/kg) group (h). TLR4 and MMP-9 were expressed predominantly in smooth muscle cells, as identified by antibody against α-actin. Yellow color in the right is the merged fields of red (for α-actin) and green (for TLR4 or MMP-9). The shown is representative of six rats in each group. Bar, 80 μm.
Effects of Rosiglitazone on Protein and mRNA Expressions of TLR4, MMP-9, PPARγ and PPARα in the Thoracic Aorta in Ang II-Infused Rats
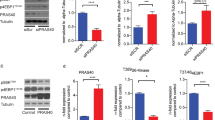
Under suggestion of the above-mentioned results with the immunofluorescent method, we further evaluated effects of rosiglitazone on protein and mRNA expressions of TLR4, MMP-9, PPARγ and PPARα in the thoracic aorta in Ang II-infused rats. As shown in Figure 3, rosiglitazone downregulated protein and mRNA expressions of TLR4 (Figure 3a and e) and MMP-9 (Figure 3b and f), and upregulated PPARγ expression (Figure 3c and g) in the thoracic aorta in Ang II-infused rats with the maximal effect achieved at 10 mg/kg of rosiglitazone. However, rosiglitazone showed little effect on PPARα expression (Figure 3d and h).
Protein and mRNA expressions of TLR4, MMP-9, PPARγ and PPARα in the thoracic aorta of Ang II-infused rats treated without or with rosiglitazone for 7 days. Protein expressions of TLR4 (a), MMP-9 (b), PPARγ (c) and PPARα (d) were measured by western blotting. The mRNA levels of TLR4 (e), MMP-9 (f), PPARγ (g) and PPARα (h) were analyzed by RT-PCR and quantitative real-time PCR after normalization to β-actin mRNA. Results are presented as mean±s.e.m. (n=6). *P<0.05, ***P<0.001 vs control; #P<0.05, ##P<0.01, ###P<0.001 vs Ang II ; †P<0.05, ††P<0.01, †††P<0.001 vs Ang II+Ros (5 mg/kg).
Concentration-Dependent Effects of Rosiglitazone on TNF-α and 6-keto-PGF1α Productions in Ang II-Stimulated VSMCs
To further confirm the effects of rosiglitazone on Ang II-induced TNF-α and 6-keto-PGF1α productions, VSMCs were pretreated with rosiglitazone (2.5, 5 and 10 μM) for 1 h, and then stimulated with Ang II (10−7 M) for the indicated time (12, 24, 36 and 48 h). As shown in Figure 4a, rosiglitazone concentration-dependently suppressed TNF-α production and increased 6-keto-PGF1α secretion in Ang II-stimulated VSMCs (Figure 4b).
Effect of rosiglitazone on TNF-α and 6-keto-PGF1α productions in Ang II-stimulated VSMCs. The cells were pretreated for 1 h with different concentrations of rosiglitazone (2.5, 5 and 10 μM) before exposure to Ang II (10−7 M) for the indicated time (12, 24, 36 and 48 h). The conditioned media were collected, and TNF-α and 6-keto-PGF1α were determined by ELISA. (a) Concentration-dependent reduction of TNF-α production in Ang II-stimulated VSMCs by rosiglitazone (Ros). (b) Concentration-dependent enhancement of 6-keto-PGF1α secretion in Ang II-stimulated VSMCs by rosiglitazone. Results are presented as mean±s.e.m. from three independent experiments.
Attenuation by Rosiglitazone of TLR4 and MMP-9 Expressions in Ang II-Stimulated VSMCs with Immunofluorescence Analysis
In light of the above-mentioned results in vivo, effects of rosiglitazone on TLR4 and MMP-9 expressions in Ang II-stimulated VSMCs were further determined. The cells were pretreated for 1 h with rosiglitazone (2.5, 5 and 10 μM) before exposure to Ang II (10−7 M) for 24 h and then, TLR4 and MMP-9 expressions were identified with immunocytofluorescence and observed using a confocal microscope. The results showed that rosiglitazone also attenuated TLR4 and MMP-9 expressions in Ang II-stimulated VSMCs in a concentration-dependent manner (Figure 5).
Immunofluorescence analysis of TLR4 and MMP-9 expressions in Ang II-stimulated VSMCs treated without or with rosiglitazone (Ros). VSMCs were pretreated for 1 h with different concentrations of rosiglitazone (2.5, 5 and 10 μM) before exposure to Ang II (10−7 M) for 24 h, and then TLR4 (a) and MMP-9 (b) expressions were identified with immunocytofluorescence and observed using confocal microscope. Fluorescence intensity of TLR4 (c) and MMP-9 (d) were also detected. Results are presented as mean±s.e.m. from three independent experiments. ***P<0.001 vs control; #P<0.05, ##P<0.01, ###P<0.001 vs Ang II.
Effects of Rosiglitazone on Protein and mRNA Expressions of TLR4, MMP-9, PPARγ and PPARα in Ang II-Stimulated VSMCs
We also further observed the effects of rosiglitazone on protein and mRNA expressions of TLR4, MMP-9, PPARγ and PPARα in Ang II-stimulated VSMCs. As shown in Figure 6, rosiglitazone concentration-dependently downregulated protein and mRNA expressions of TLR4 and MMP-9, upregulated protein and mRNA expressions of PPARγ, but had little effect on PPARα expression in Ang II-stimulated VSMCs.
Effect of rosiglitazone on Ang II-induced protein and mRNA expressions of TLR4, MMP-9, PPARα and PPARγ in rat VSMCs. VSMCs were pretreated without or with different concentrations of rosiglitazone (2.5, 5 and 10 μM) for 1 h, and stimulated with Ang II (10−7 M) for 24 h. Protein expressions of TLR4 (a), MMP-9 (b), PPARγ (c) and PPARα (d) were measured by western blotting. The mRNA levels of TLR4 (e), MMP-9 (f), PPARγ (g) and PPARα (h) were measured by RT-PCR and quantitative real-time PCR after normalization to β-actin mRNA. Results are presented as mean±s.e.m. from three independent experiments. *P<0.05, **P<0.01, ***P<0.001 vs control; #P<0.05, ##P<0.01, ###P<0.001 vs Ang II.
Relationship Between Effects of Rosiglitazone on Ang II-Induced Inflammatory Responses in VSMCs and TLR4
The above-mentioned results show that rosiglitazone may reduce TNF-α production and enhance 6-keto-PGF1α release, and downregulate TLR4 expression in Ang II-stimulated VSMCs in vivo and in vitro. To evaluate whether rosiglitazone inhibits the inflammatory responses through TLR4, VSMCs were pretreated without or with anti-TLR4 antibody (1 μg/ml) for 1 h before the addition of rosiglitazone (10 μM) for 1 h, and subsequently stimulated with Ang II (10−7 M) or LPS (100 ng/ml) for 24 h. As shown in Figure 7a and b, compared with the control, stimulating the cells with Ang II or LPS resulted in TNF-α elevation and 6-keto-PGF1α reduction, whereas the TLR4 inhibitor and rosiglitazone partially reversed the Ang II- and LPS-induced effects in VSMCs. Moreover, treatment of the cells with a combination of the TLR4 blocker and rosiglitazone synergistically reversed Ang II-induced changes of TNF-α production and 6-keto-PGF1α release in comparison with treatment of the TLR4 blocker or rosiglitazone alone. Considering that the TLR4 blocker antagonizes effects of Ang II and LPS on TNF-α and 6-keto-PGF1α, and rosiglitazone downregulates TLR4 expression in VSMCs, consequently, the modulatory effects of rosiglitazone on TNF-α production and 6-keto-PGF1α release in Ang II-induced VSMCs are associated with TLR4.
Relationship between effects of rosiglitazone (Ros) on Ang II-mediated inflammatory responses in VSMCs and TLR4. VSMCs were pretreated without or with anti-TLR4 antibody (1 μg/ml) for 1 h before the addition of Ros (10 μM) for 1 h, and subsequently stimulated with Ang II (10−7 M) or LPS (100 ng/ml) for 24 h. The conditioned media were collected and concentrations of TNF-α (a) and 6-keto-PGF1α (b) were determined by ELISA. Expressions of MMP-9, PPARγ and PPARα were analyzed by western blotting (c). Results are presented as mean±s.e.m. from three independent experiments. *P<0.05, **P<0.01, ***P<0.001 vs control; #P<0.05, ##P<0.01, ###P<0.001 vs Ang II; †P<0.05, ††P<0.01, †††P<0.001 vs LPS; ‡P<0.01 vs Ang II+ anti-TLR4; $$P<0.01 vs Ang II+ Ros.
The experiment also found that the TLR4 inhibitor reduced MMP-9 expression, and enhanced PPARγ and PPARα expressions in Ang II-and LPS-stimulated VSMCs. Rosiglitazone also produced similar effects on MMP-9 and PPARγ expressions to the TLR4 inhibitor, but had little effect on PPARα expression. Treatment of the cells with both the TLR4 blocker and rosiglitazone also synergistically reversed Ang II-induced changes of MMP-9 and PPARγ expressions (Figure 7c). Therefore, the modulatory effects of rosiglitazone on MMP-9 and PPARγ protein expressions in Ang II-stimulated VSMCs are also associated with TLR4. Taken together, these imply that the inhibitory effects of rosiglitazone on Ang II-induced inflammatory responses in VSMCs are related to TLR4.
Effects of TLR4 siRNA on Anti-Inflammatory Action of Rosiglitazone in Ang II-Stimulated VSMCs
The TLR4 siRNA was applied to VSMCs to further confirm the role of this membrane receptor in Ang II-induced inflammatory responses in VSMCs and in anti-inflammatory mechanism of rosiglitazone. After VSMCs were transiently transfected with TLR4 siRNA for 48 h, TLR4 mRNA levels were obviously downregulated (Figure 8a). The knockdown efficiency of TLR4 was 64%, as determined by quantitative real-time PCR. The transfected VSMCs were pretreated with rosiglitazone (10 μM) for 1 h, and then stimulated with Ang II (10−7 M) for 24 h. Lack of TLR4 decreased Ang II-induced TNF-α production and increased 6-keto-PGF1α release when compared with negative control, thereby showing that Ang II regulates TNF-α and 6-keto-PGF1α productions through TLR4. Rosiglitazone reduced Ang II-induced TNF-α production and increased Ang II-decreased 6-keto-PGF1α release in negative control, but the effects of rosiglitazone were nearly abolished in TLR4 siRNA control (Figure 8b and c), suggesting that regulation of TNF-α and 6-keto-PGF1α productions by rosiglitazone depends on the existence of TLR4. The results also showed that rosiglitazone did not change basal TNF-α production, but significantly increased 6-keto-PGF1α level in the unstimulated VSMCs. The results similar to TNF-α were achieved for mRNA expression of MMP-9 (Figure 8d). Furthermore, we found that TLR4 siRNA also abolished Ang II-induced decrease of mRNA expressions of PPARγ and PPARα when compared with negative control, thereby showing that Ang II inhibits expressions of PPARγ and PPARα through TLR4. Rosiglitazone regulated PPARγ mRNA levels in negative control both in the normal and in Ang II-stimulated VSMCs, but TLR4 siRNA did not change the effect of rosiglitazone on PPARγ (Figure 8e), indicating that increase of PPARγ expression by rosiglitazone is not completely related to TLR4. In addition, rosiglitazone did not produce significant effect on mRNA levels of PPARα in negative control and in TLR4 siRNA control (Figure 8f).
Effects of TLR4 siRNA on anti-inflammatory action of rosiglitazone (Ros) in Ang II-stimulated VSMCs. After application of negative control siRNA (NC siRNA) or TLR4 siRNA for 48 h, VSMCs were exposed to rosiglitazone (10 μM) for another 1 h, and subsequently stimulated with Ang II (10−7 M) for 24 h. (a) TLR4 mRNA levels in VSMCs were detected by RT-PCR and quantitative real-time PCR at 48 h post-transfection. (b and c) Concentrations of TNF-α and 6-keto-PGF1α were determined by ELISA. (d) MMP-9, (e) PPARγ and (f) PPARα mRNA levels were measured by RT-PCR and quantitative real-time PCR after normalization to β-actin mRNA. Results are presented as mean±s.e.m. from three independent experiments. *P<0.05, **P<0.01, ***P<0.001 vs NC siRNA.
Inhibitory Effect of Rosiglitazone on Ang II-Induced TLR4 Expression in VSMCs by Blockade of ERK1/2
To clarify whether AT1 and ERK1/2 signaling were involved in the inhibitory effect of rosiglitazone on Ang II-induced TLR4 expression in VSMCs, the cells were subjected to losartan (10−6 M), PD123319 (10−5 M) and PD098059 (10−6 M) for 30 min, followed by treatment of rosiglitazone (10 μM) for further 1 h, and subsequently stimulated with Ang II (10−7 M) for 24 h. As shown in Figure 9a, AT1 antagonist, losartan, and ERK1/2 antagonist, PD098059, inhibited Ang II-induced TLR4 expression in VSMCs, whereas AT2 antagonist, PD123319, had no effect. Rosiglitazone alone also inhibited Ang II-induced TLR4 expression in VSMCs, and did not have any additional effects on AT1 or AT2 blockade. However, rosiglitazone produced an additional effect on PD098059 blockade, suggesting that its inhibitory effect on Ang II-induced TLR4 expression is mainly dependent on suppression of ERK1/2. Furthermore, rosiglitazone remarkably inhibited ERK1/2 phosphorylation induced by Ang II treatment (10−7 M) for 5 min, but did not affect ERK1/2 phosphorylation in the unstimulated cells (Figure 9b). Treatment of VSMCs with Ang II (10−7 M) for 24 h significantly downregulated the AT1 protein expression. Although it also inhibited AT1 expression in the normal VSMCs, rosiglitazone did not produce an additional inhibitory effect on AT1 expression in Ang II-treated cells (Figure 9c). These data suggest that inhibitory effect of rosiglitazone on Ang II-induced TLR4 expression in VSMCs mainly involves blockade of ERK1/2.
Inhibitory effect of rosiglitazone (Ros) on Ang II-induced TLR4 expression in VSMCs by blockade of ERK1/2. (a) Inhibitory effect of rosiglitazone on Ang II-induced TLR4 protein expression possibly by inhibition of ERK1/2. (b) Inhibitory effect of rosiglitazone on Ang II-induced activation of ERK1/2 in VSMCs. (c) Effect of rosiglitazone on AT1 protein expression in Ang II-stimulated VSMCs. Results are presented as mean± s.e.m. from three independent experiments. *P<0.05, **P<0.01, ***P<0.001 vs control; #P<0.05, ##P<0.01, ###P<0.001 vs Ang II; †P<0.05 vs Ang II+PD098059; $P<0.05 vs Ang II+Ros.
Inhibition by Rosiglitazone of Ang II-Mediated Inflammatory Responses by Interference with TLR4-Dependent Signaling Pathway in VSMCs
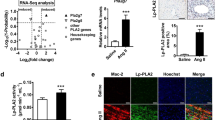
The effect of TLR4 siRNA on Ang II-induced IP-10 expression in VSMCs treated with rosiglitazone was examined. As shown in Figure 10a, lack of TLR4 reduced Ang II-induced IP-10 protein expression compared with negative control. Rosiglitazone obviously inhibited Ang II-induced IP-10 protein expression in negative control, but did not further reduce the Ang II-induced IP-10 protein expression in TLR4 siRNA control, thereby showing inhibition by rosiglitazone of Ang II-induced IP-10 protein expression through TLR4-dependent signaling pathway. After VSMCs were transfected with IP-10 siRNA for 48 h, IP-10 protein expression was potently downregulated in comparison with negative control (Figure 10b). Figure 10c showed that IP-10 siRNA diminished Ang II-induced PKC protein expression. Although rosiglitazone depressed Ang II-induced PKC protein expression, lack of IP-10 abolished the inhibitory effect of rosiglitazone. Finally, we observed whether the blockade of PKC was required for inhibitory effect of rosiglitazone on Ang II-induced NF-κB protein expression. VSMCs were pretreated without or with the specific PKC inhibitor, chelerythrine (CH, 5 μM), for 1 h before the addition of rosiglitazone (10 μM) for 1 h, and subsequently stimulated with Ang II (10−7 M) or the specific PKC activator, PMA (100 nM), for 24 h. As shown in Figure 10d, rosiglitazone significantly suppressed Ang II- and PMA-induced NF-κB protein expression in VSMCs, and potentiated the inhibitory effect of the specific PKC inhibitor. These show that the inhibitory effect of rosiglitazone on NF-κB protein expression in VSMCs is associated with PKC. In combination, these results suggest that rosiglitazone may inhibit Ang II-induced inflammatory responses in VSMCs by interfering with ERK1/2/TLR4/IP-10/PKC/NF-κB signaling pathway.
Inhibition by rosiglitazone (Ros) of Ang II-induced inflammatory responses in VSMCs by interference with TLR4-dependent signaling pathway. (a) TLR4 siRNA abolished effect of Ros on Ang II-induced IP-10 expression in VSMCs. (b) Effect of IP-10 siRNA on IP-10 protein expression in VSMCs at 48 h post-transfection. (c) IP-10 siRNA abolished effect of Ros on Ang II-induced PKC protein expression in VSMCs. (d) Inhibition by rosiglitazone of Ang II-induced NF-κB protein expression through blockade of PKC. Results are presented as mean±s.e.m. from three independent experiments. CH and PMA indicate chelerythrine and phorbol 12-myristate-13 acetate, respectively. *P<0.05, **P<0.01, ***P<0.001 vs NC control or control; #P<0.05, ##P<0.01 vs Ang II; ††P<0.01, †††P<0.001 vs PMA; ‡P<0.01 vs Ang II +CH. $P<0.05 vs Ang II+Ros.
DISCUSSION
This study shows that PPARγ agonist, rosiglitazone, reduces Ang II-mediated productions of TLR4, MMP-9 and TNF-α, and enhances generation of PPARγ and PGI2, both in vivo and in vitro. Our result also shows that rosiglitazone prevents hypertension in Ang II-infused rats. Furthermore, our findings suggest that the inhibitory effects of rosiglitazone on Ang II-mediated inflammatory responses in VSMCs closely involved TLR4. Another novel finding is the capability of rosiglitazone to inhibit Ang II-induced inflammatory responses in VSMCs by interfering with the TLR4-dependent signaling pathway.
Atherosclerosis is a complex multifactorial disease of the large arteries and is related to a chronic inflammatory process.32 Inflammation is increasingly recognized as a key driving force of atherogenesis. TNF-α, an inflammatory mediator, enhances release of the other inflammatory cytokines and expression of adhesion molecules. PGI2, a potent modulator of inflammation, also exerts airway smooth muscle relaxation and reduces inflammation.33, 34 MMP-9 is a proteolytic enzyme that remodels the extracellular matrix as a part of inflammatory response, which leads to plaque destablization and triggers atherosclerotic diseases.35 This study showed that in vivo and in vitro treatment with PPARγ agonist, rosiglitazone, reduced Ang II-induced TNF-α production and MMP-9 expression and enhanced PGI2 secretion, suggesting that rosiglitazone exerts direct anti-inflammatory effects in both Ang II-infused rats and Ang II-stimulated VSMCs to prevent development of atherosclerosis. Moreover, PPARs activation may limit inflammation and atherosclerosis by altering expression of the master transcription factor, NF-κ B, to result in inhibition of inflammatory target genes.36, 37 In this study, rosiglitazone significantly enhanced PPARγ mRNA and protein expressions, but showed little effect on PPARα expression in Ang II-stimulated VSMCs. The results further indicate that PPARγ expression itself is another site of interaction between PPARγ agonist and inflammatory mediators.
Rosiglitazone has also been shown to lower blood pressure in the Ang II-infused rats to prevent vascular structural changes, endothelial dysfunction and inflammatory responses in the model. However, the vasodilator, hydralazine, produces hypotensive effect without any effect on vascular structure or inflammatory mediators, thus supporting that anti-inflammatory property of rosiglitazone is not related to the hypotensive effect.38 In this study, rats received continuous infusion of exogenous Ang II to maintain circulating Ang II at a constant level, which probably exerted vascular inflammation and accelerated atherosclerotic process. In addition, we found that rosiglitazone relived Ang II-induced inflammatory responses, except for lowering blood pressure in the animal study, and produced direct effects on Ang II-mediated inflammatory responses in the in vitro study. In light of these findings, we speculate that rosiglitazone exerts an inhibitory effect on vascular inflammation that is independent of BP levels.
Lipopolysaccharide triggers the TLR4-dependent activation of NF-κB and other transcription factors to induce the expression of pro-inflammatory target genes through upregulating TLR4 in atherogenesis.39 Furthermore, recent reports have revealed that TLR4 in VSMCs is also activated by Ang II,11 and PPARγ activators antagonize the effect induced by Ang II in vivo and in vitro to exert anti-oxidant and anti-inflammatory actions on the cardiovascular system.40 This study provided a direct evidence that rosiglitazone alleviated Ang II-induced TLR4 expression in VSMCs both in vivo and in vitro. However, there is still much to learn about the relationship between the inhibitory effects of rosiglitazone on Ang II-induced inflammatory responses in VSMCs and TLR4. Accordingly, both the TLR4 inhibitor and TLR4 siRNA were applied to VSMCs to clarify whether TLR4 is involved in the inhibitory effects of rosiglitazone. We found that the TLR4-specific monoclonal antibody partially antagonized the Ang II-induced inflammatory responses, which were potentiated by rosiglitazone. In addition, Ang II-mediated inflammatory responses require TLR4 at least in part, as Ang II-induced productions of MMP-9, PPARγ, PPARα, TNF-α and PGI2 were regulated by TLR4 siRNA. As LPS is a special ligand of TLR4,41 rosiglitazone relieved LPS-mediated inflammatory responses and directly downregulated Ang II-induced TLR4 expression, further suggesting that TLR4 is associated with the inhibitory effects of rosiglitazone on Ang II-induced inflammatory responses in VSMCs. In combination of the finding that lack of TLR4 almost abolishes the inhibitory effect of rosiglitazone on Ang II-mediated inflammatory responses, TLR4 is a target involved in inhibition of Ang II-induced inflammation in VSMCs by PPARγ agonist.
On the basis of the results mentioned above, we further investigated the TLR4-dependent signaling pathway involved in anti-inflammatory effect of rosiglitazone in Ang II-stimulated VSMCs. Earlier studies suggest that Ang II binding to AT1 receptors in VSMCs is linked to ERK1/2-dependent pathways.31, 42 Here, we also show that Ang II-induced TLR4 expression in VSMCs was mediated by the AT1/ERK1/2 signaling, and inhibitory effect of rosiglitazone on Ang II-induced TLR4 expression in VSMCs mainly involves blockade of ERK1/2. Moreover, activation of TLR4 may stimulate both a myeloid differentiation factor (MyD88)-dependent and a MyD88-independent pathway. The MyD88-dependent pathway is largely responsible for controlling the expression of inflammatory cytokines, such as TNF-α, IL-6 and IL-12, through activation of NF-κB, whereas the MyD88-independent pathway induces expression of IFN-inducible genes, such as IP-10.43 In this study, the TLR4 siRNA reduced Ang II-induced IP-10 protein expression. Rosiglitazone significantly downregulated the Ang II-induced IP-10 expression, thus suggesting that anti-inflammatory effects of rosiglitazone involve the blockade of TLR4/IP-10 pathway. Furthermore, we proved that IP-10 may lie upstream from PKC in the signal cascades, because IP-10 siRNA almost completely abolished the increase of Ang II-induced PKC expression. Rosiglitazone evidently depressed Ang II-induced PKC expression. In addition, it has been shown that PKC is able to mediate nuclear translocation of NF-κB.44 Our study further showed that rosiglitazone served its anti-inflammatory actions by interfering with the PKC and NF-κB signalings, which are also firmly supported by the earlier findings.45, 46
In summary, PPARγ agonist, rosiglitazone, exerts its anti-inflammatory effect by interfering with the TLR4-dependent signaling pathway (ERK1/2/TLR4/IP-10/PKC/NF-κB). These findings provide new mechanisms to beneficial effects of rosiglitazone in the prevention and treatment of cardiovascular disease including atherosclerosis.
References
Monaco C, Paleolog E . Nuclear factor κB: a potential therapeutic target in atherosclerosis and thrombosis. Cardiovasc Res 2004;61:671–682.
Ross R . Atherosclerosis–an inflammatory disease. N Engl J Med 1999;340:115–126.
Weiss D, Sorescu D, Taylor WR . Angiotensin II and atherosclerosis. Am J Cardiol 2001;87:25C–32C.
Strawn WB, Ferrario C . Mechanisms linking angiotensin II and atherogenesis. Curr Opin Lipidol 2002;13:505–512.
Miyazaki M, Takai S . Tissue angiotensin II generating system by angiotensin-converting enzyme and chymase. J Pharmacol Sci 2006;100:391–397.
Kranzhöfer R, Schmidt J, Pfeiffer CA, et al. Angiotensin induces inflammatory activation of human vascular smooth muscle cells. Arterioscler Thromb Vasc Biol 1999;19:1623–1629.
Kim S, Whelan J, Claycombe K, et al. Angiotensin II increases leptin secretion by 3T3-L1 and human adipocytes via a prostaglandin-independent mechanism. J Nutr 2002;132:1135–1140.
Muramatsu M, Katada J, Hayashi I, et al. Chymase as a proangiogenic factor: a possible involvement of chymase angiotensin-dependent pathway in the hamster sponge angiogenesis model. J Biol Chem 2000;275:5545–5552.
Nicoletti A, Caliguri G, Paulosson G . Functionality of specific immunity in atherosclerosis. Am Heart J 1999;138:438–443.
Trinchieri G, Sher A . Cooperation of Toll-like receptor signals in innate immune defence. Nat Rev Immunol 2007;7:179–190.
Otsui K, Inoue N, Kobayashi S, et al. Enhanced expression of TLR4 in smooth muscle cells in human atherosclerotic coronary arteries. Heart Vessels 2007;22:416–422.
Guo RW, Yang LX, Wang H, et al. Angiotensin II induces matrix metalloproteinase-9 expression via a nuclear factor-kappa B-dependent pathway in vascular smooth muscle cells. Regul Pept 2008;147:37–44.
Evans RM, Barish GD, Wang YX . PPARs and the complex journey to obesity. Nat Med 2004;10:355–361.
Lee CH, Olson P, Evans RM . Minireview: lipid metabolism, metabolic diseases, and peroxisome proliferator-activated receptors. Endocrinology 2003;144:2201–2207.
Yano Y, Hoshide S, Ishikawa J, et al. The differential effects of angiotensin II type 1 receptor blockers on microalbuminuria in relation to low-grade inflammation in metabolic hypertensive patients. Am J Hypertens 2007;20:565–572.
Law RE, Hsueh WA . PPARγ and atherosclerosis: effects on cell growth and movement. Arterioscler Thromb Vasc Biol 2001;21:1891–1895.
Ishibashi M, Egashira K, Hiasa K, et al. Anti-inflammatory and anti-arteriosclerotic effects of pioglitazone. Hypertension 2002;40:687–693.
Diep QN, El Mabrouk M, Cohn JS, et al. Structure, endothelial function, cell growth, and inflammation in blood vessels of angiotensin II-infused rats: role of peroxisome proliferator-activated receptor-γ. Circulation 2002;105:2296–2302.
Abdelrahman M, Sivarajah A, Thiemermann C . Beneficial effects of PPAR-γ ligands in ischemia–reperfusion injury, inflammation and shock. Cardiovasc Res 2005;65:772–781.
Ryan MJ, Didion SP, Mathur S, et al. PPARγ agonist rosiglitazone improves vascular function and lowers blood pressure in hypertensive transgenic mice. Hypertension 2004;43:661–666.
Goetze S, Xi XP, Graf K, et al. Troglitazone inhibits angiotensin II-induced extracellular signal-regulated kinase1/2 nuclear translocation and activation in vascular smooth muscle cells. FEBS Lett 1999;452:277–282.
Palsson-McDermott EM, O'Neill LA . Signal transduction by the lipopolysaccharide receptor Toll-like receptor-4. Immunology 2004;113:153–162.
Re F, Strominger JL . IL-10 released by concomitant TLR2 stimulation blocks the induction of a subset of Th1 cytokines that are specifically induced by TLR4 or TLR3 in human dendritic cells. J Immunol 2004;173:7548–7555.
Lucas PC, McAllister-Lucas LM, Nunez G . NF-kappa B signaling in lymphocytes: a new cast of characters. J Cell Sci 2004;117 (Part 1): 31–39.
De Kleijn D, Pasterkamp G . Toll-like receptors in cardiovascular diseases. Cardiovasc Res 2003;60:58–67.
Björkbacka H, Kunjathoor VV, Moore KJ, et al. Reduced atherosclerosis in MyD88-null mice links elevated serum cholesterol levels to activation of innate immunity signaling pathways. Nat Med 2004;10:416–421.
Michelsen KS, Wong MH, Shah PK, et al. Lack of Toll-like receptor 4 or myeloid differentiation factor 88 reduces atherosclerosis and alters plaque phenotype in mice deficient in apolipoprotein E. Proc Natl Acad Sci USA 2004;101:10679–10684.
Wen SJ, Zhao LM, Li P, et al. Blood vessel tissue engineering: seeding vascular smooth muscle cells and endothelial cells sequentially on biodegradable scaffold in vitro. Natl Med J China 2005;85:816–818 (In Chinese).
Griendling KK, Taubman MB, Akers M, et al. Characterization of phosphatidylinositol-specific phospholipase C from cultured vascular smooth muscle cells. J Biol Chem 1991;266:15498–15504.
Gao DF, Niu XL, Hao GH, et al. Rosiglitazone inhibits angiotensin II-induced CTGF expression in vascular smooth muscle cells—role of PPAR-gamma in vascular fibrosis. Biochem Pharmacol 2007;73: 185–197.
Peng N, Liu JT, Gao DF, et al. Angiotensin II-induced C-reactive protein generation: inflammatory role of vascular smooth muscle cells in atherosclerosis. Atherosclerosis 2007;193:292–298.
Braunwald E . Shattuck lecture-cardiovascular medicine at the turn of the millennium: triumphs, concerns, and opportunities. N Engl J Med 1997;337:1360–1369.
Wang M, Song WL, Cheng Y, et al. Microsomal prostaglandin E synthase-1 inhibition in cardiovascular inflammatory disease. J Intern Med 2008;263:500–505.
Bezdecny SA, Cao J, Li X . Antiasthma herbal medicine intervention (ashmi) modulates prostanoid release from human tracheal airway smooth muscle cells (hasmc). J Allergy Clin Immunol 2008;121:S49.
Marc F, Mark S, Martin G, et al. Matrix metalloproteinases in cerebrovascular diseases. Cerebrovasc Dis 2005;20:141–151.
Duval C, Chinetti G, Trottein F, et al. The role of PPARs in atherosclerosis. Trends Mol Med 2002;8:422–430.
Castrillo A, Tontonoz P . Nuclear receptors in macrophage biology: at the crossroads of lipid metabolism and inflammation. Annu Rev Cell Dev Biol 2004;20:455–480.
Diep QN, El Mabrouk M, Cohn JS, et al. Structure, endothelial function, cell growth, and inflammation in blood vessels of angiotensin II-infused rats: role of peroxisome proliferator-activated receptor-gamma. Circulation 2002;105:2296–2302.
Michelsen KS, Doherty TM, Shah PK, et al. TLR signaling: an emerging bridge from innate immunity to atherogenesis. J Immunol 2004;173:5901–5907.
Schiffrin EL . Peroxisome proliferator-activated receptors and cardiovascular remodeling. Am J Physiol Heart Circ Physiol 2005;288:H1037–H1043.
Paik YH, Lee KS, Lee HJ, et al. Hepatic stellate cells primed with cytokines upregulate inflammation in response to peptidoglycan or lipoteichoic acid. Lab Invest 2006;86:676–686.
Pinzar E, Wang T, Garrido MR, et al. Angiotensin II induces tyrosine nitration and activation of ERK1/2 in vascular smooth muscle cells. FEBS Lett 2005;579:5100–5104.
Dauphinee SM, Karsan A . Lipopolysaccharide signaling in endothelial cells. Lab Invest 2006;86:9–22.
Li RC, Ping P, Zhang J, et al. PKCepsilon modulates NF-kappa B and AP-1 via mitogen-activated protein kinases in adult rabbit cardiomyocytes. Am J Physiol Heart Circ Physiol 2000;279:H1679–H1689.
Hattori Y, Akimoto K, Kasai K . The effects of thiazolidinediones on vascular smooth muscle cell activation by angiotensin II. Biochem Biophys Res Commun 2000;273:1144–1149.
Rival Y, Benéteau N, Taillandier T, et al. PPARalpha and PPARdelta activators inhibit cytokine-induced nuclear translocation of NF-kappa B and expression of VCAM-1 in EAhy926 endothelial cells. Eur J Pharmacol 2002;435:143–151.
Acknowledgements
This study was supported by Grant 30772567 from the National Natural Science Foundation of China.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ji, Y., Liu, J., Wang, Z. et al. PPARγ agonist, rosiglitazone, regulates angiotensin II-induced vascular inflammation through the TLR4-dependent signaling pathway. Lab Invest 89, 887–902 (2009). https://doi.org/10.1038/labinvest.2009.45
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2009.45
Keywords
This article is cited by
-
The Possible Role of the Angiotensin System in the Pathophysiology of Schizophrenia: Implications for Pharmacotherapy
CNS Drugs (2019)
-
Interrelationship between diabetes mellitus and heart failure: the role of peroxisome proliferator-activated receptors in left ventricle performance
Heart Failure Reviews (2018)
-
Telmisartan attenuates hydrogen peroxide-induced apoptosis in differentiated PC12 cells
Metabolic Brain Disease (2018)
-
MD2 mediates angiotensin II-induced cardiac inflammation and remodeling via directly binding to Ang II and activating TLR4/NF-κB signaling pathway
Basic Research in Cardiology (2017)
-
Epigallocatechin-3-gallate inhibits angiotensin II-induced C-reactive protein generation through interfering with the AT1-ROS-ERK1/2 signaling pathway in hepatocytes
Naunyn-Schmiedeberg's Archives of Pharmacology (2016)