Abstract
Tenofovir disoproxil fumarate (TDF) is an analog of adenosine monophosphate that inhibits HIV reverse transcriptase in HIV/AIDS. Despite its therapeutic success, renal tubular side effects are reported. The mechanisms and targets of tenofovir toxicity were determined using ‘2 × 2’ factorial protocols, and HIV transgenic (TG) and wild-type (WT) littermate mice with or without TDF (5 weeks). A parallel study used didanosine (ddI) instead of TDF. At termination, heart, kidney, and liver samples were retrieved. Mitochondrial DNA (mtDNA) abundance, and histo- and ultrastructural pathology were analyzed. Laser-capture microdissection (LCM) was used to isolate renal proximal tubules for molecular analyses. Tenofovir increased mtDNA abundance in TG whole kidneys, but not in their hearts or livers. In contrast, ddI decreased mtDNA abundance in the livers of WTs and TGs, but had no effect on their hearts or kidneys. Histological analyses of kidneys showed no disruption of glomeruli or proximal tubules with TDF or ddI treatments. Ultrastructural changes in renal proximal tubules from TDF-treated TGs included an increased number and irregular shape of mitochondria with sparse fragmented cristae. LCM-captured renal proximal tubules from TGs showed decreased mtDNA abundance with tenofovir. The results indicate that tenofovir targets mitochondrial toxicity on the renal proximal tubule in an AIDS model.
Similar content being viewed by others
Main
Pyrimidine and purine analogs called ‘nucleoside reverse transcriptase inhibitors’ (NRTIs) are drugs used in the treatment of HIV/AIDS. Tenofovir is an acyclic nucleotide phosphonate diester analog of adenosine monophosphate.1 Similar to many NRTIs, tenofovir inhibits HIV-1 reverse transcriptase by competing with the natural substrate deoxyadenosine 5′-triphosphate,2 one of the nucleotide pools used by virus in generating cDNA.
Despite the distinct benefits of NRTI-based therapies, toxicity is a limiting factor. In particular, a number of in vitro and in vivo studies showed cardiomyopathy and hepatic failure associated with specific NRTIs.3, 4, 5, 6 NRTI toxicities seem to be tissue specific.7, 8 Zidovudine and stavudine are toxic to striated muscle.4, 9 Didanosine (ddI) is toxic to the liver and pancreas.6, 10 An important form of tenofovir toxicity is tubular dysfunction,11, 12, 13, 14 but its mechanism or precise target has not been elucidated. Although the mechanisms of these specific antiretroviral drug-related toxicities remain unclear, it has been hypothesized that as analogs to native nucleosides, tenofovir and other NRTIs may potentially inhibit mammalian DNA polymerases, including mitochondrial DNA (mtDNA) polymerase-γ, and induce oxidative stress.15, 16, 17 Tenofovir is not a substrate of CYP450 enzymes, and is eliminated by glomerular filtration and active tubular secretion.18
HIV-associated nephropathy (HIVAN) is an AIDS-related disease of the kidney. NRTIs (similar to tenofovir) are used to treat HIV/AIDS. Tenofovir is the only NRTI that is associated with renal disease. Nevertheless, tenofovir tubular toxicity may be additive or synergistic with HIVAN. These studies parametrically assess the individual and combined effects of NRTIs (similar to tenofovir or ddI) using a genetically homogenous (albeit phenotypically heterogenous, possibly because of differences in transgene expression level) murine HIV transgenic (TG) model.19 Laser-capture microdissection (LCM) was used to anatomically isolate renal proximal tubules to define the effects of tenofovir on tubules in this HIV TG model.
MATERIALS AND METHODS
Animals
Hemizygous HIV-1 TG mice established by Dickie20 were provided as compliments of Paul Klotman. Originally on FVB/n background, this TG line was bred congenically to C57/BL6 (and given the trivial name: MSB). The resultant TG that was made congenic to C57/BL6 did not develop HIVAN, compared with the original TG on FVB/n. This absence of HIVAN was an experimental feature that allowed us to detect changes related to drug toxicity, which otherwise might be overshadowed by HIVAN. This study used a ‘2 × 2’ factorial protocol and included TG and wild-type (WT) mice treated with vehicle or NRTI. Murine TG authenticity was confirmed for each generation using dot blot analysis and real-time PCR.21
Treatment Protocols
Procedures complied with the Emory IACUC and NIH guidelines. WT and TG littermates of both genders (male and female) were age matched (8–12 weeks) at the start of treatment. Food and water were provided ad libitum. Antiretroviral drugs were provided by the manufacturers (compliments of Professor Raymond Schinazi, VA Medical Center, Decatur, GA, USA and Emory Center for AIDS Research Pharmacology Core). To remain clinically relevant, dosing was done by daily gavage (morning) at doses that resembled human therapy on a mg/kg/day basis (eg, human tenofovir disoproxil fumarate (TDF) daily dose: 300 mg/60 kg human=5 mg/kg; ∼25 g mouse=0.125 mg/day). Treatments included TDF (0.125 mg/day), ddI (0.14 mg/day), or vehicle (buffered with 0.1 M NaOH). Each cohort consisted of ∼20 mice,12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22 ultimately depending on actual litter sizes from three replicate experiments. Mortality from the procedure was nil (100% survival). On the basis of a number of NRTI treatment protocols used in our laboratory,4, 9, 21, 22, 23, 24, 25 a treatment duration of 5 weeks was used in these initial studies. After 5 weeks of treatment, body weights were measured, animals terminated, and samples retrieved and stored for DNA extraction and analysis.
mtDNA and Nuclear DNA (nDNA) Quantitation in the Heart, Kidney, and Liver Tissues Using Real-Time PCR
Methods employed were modifications used by others,26 as employed by us in the past.21, 25 Total DNA was extracted from select tissues (∼10 mg wet weight) using a MagNA Pure System and reagents (Roche Life Sciences, Indianapolis, IN, USA). Alternatively, DNA was extracted from proximal tubules isolated with LCM (see procedure below).
DNA sequences for primers and probes used for quantitation of mtDNA and nDNA have been described earlier.25 Real-time PCR was performed in duplicate for each amplicon. Amplification was performed using LC 480 (Roche). Standard DNA curves for quantitation of the LC products were used. PCR products of mtDNA and nDNA were quantified using the corresponding external standard.
Histological Examination
Tissue samples were processed routinely. Sections (6 μm) were stained with hematoxylin and eosin (H&E) and examined microscopically by a blinded, trained pathologist (WL). Photomicrographs of glass slides were obtained using a Nikon photomicroscope (Nikon, Garden City, NY, USA).
Fine Structure of Kidney Tissues Using Electron Microscopy (EM)
EM was evaluated using reported methods.4 Sections (0.5 μm) were cut with glass knives and stained with Toluidine Blue for orientation. Ultrathin (900 Å) sections were cut with a diamond knife, stained with uranyl acetate and lead citrate and examined by EM (Philips Morgagni Model 201, Philips, Eindhoven, Amsterdam, The Netherlands), and evaluated and photographed. Each EM photomicrograph was reviewed independently by two investigators. Parameters included the presence of structurally abnormal mitochondria, increased numbers of mitochondrial profiles per field, intra-mitochondrial lamellar bodies, abnormal cristae density, cristae reduplication, mitochondrial swelling, and intra-mitochondrial paracrystals.27
Laser-Capture Microdissection
The inherent heterogeneity of kidney tissues (including glomeruli, proximal and distal tubule epithelial cells, blood vessels, and interstitium with its mix of resident and infiltrating cells) can affect the outcome and interpretation of molecular studies. LCM, a novel technique developed at the National Cancer Institute,28 allows for specific, single-cell isolation from fixed heterogenous tissues. Specifically, proximal renal tubular cells were isolated using the Arcturus LCM 1110 system (Arcturus Biosciences Inc., Mountain View, CA, USA). DNA was extracted from pooled renal tubular epithelial cells (∼100 cells) isolated from each embedded sample using the PicoPure™ DNA Extraction Kit (MDS Analytical Technologies, Sunnyvale, CA, USA).
Statistical Analysis
Data were expressed as the ratio of mean values for mtDNA to those of nDNA × 10−3. Resultant values were expressed as mean±s.e.m., normalized to the mean of vehicle-treated WTs (set at 1.0). A value of P<0.05 was considered statistically significant. Results from vehicle-treated TGs were combined statistically from the respective TDF and ddI ‘2 × 2’ studies to increase the power. Results from all groups were compared using one-way ANOVA.9 Alternatively, the Mann–Whitney unpaired t-test was applied to the data. In some cohorts, outliers (as determined using Grubb's test with P<0.05)29 were excluded from the cohort data set.
RESULTS
General
All the TG and WT cohorts maintained overall health with normal body weights and levels of activity throughout the study duration, regardless of treatment.
mtDNA Abundance in Various Tissues after Treatment
To determine mitochondrial toxicity with TDF or ddI, mtDNA abundance was assessed using DNA extracts from various tissues of both TGs and WTs after 5 weeks of treatment with TDF, ddI, or vehicle. mtDNA abundance was determined in the heart, kidney, and liver tissues.
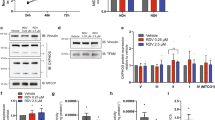
TDF treatment had no effect on mtDNA abundance in the hearts or livers from all cohorts (Figure 1a). Kidneys from TDF-treated TGs showed increased mtDNA abundance, compared with those of vehicle-treated TGs and WTs (Figure 1a). Treatment with ddI yielded different results. mtDNA abundance remained unchanged in all hearts and kidneys after ddI treatment, whereas liver mtDNA abundance decreased significantly in both TGs and WTs, compared with their vehicle-treated littermates (Figure 1b).
Tissue-specific changes in mtDNA abundance after TDF (a) or ddI (b) treatment: using ‘2 × 2’ protocols, cohorts of TG and WT mice were treated with TDF, ddI, or vehicle (5 weeks). After treatment, cardiac, kidney, and liver tissues were collected, and mtDNA abundance was determined for each cohort as normalized ratios of mtDNA–nDNA. Changes in mtDNA abundance were tissue and treatment specific.
Histological Analysis of Kidney Tissues
Kidneys from TGs and WTs were histologically assessed to determine whether treatment with TDF yielded microscopic changes in renal tubules or glomeruli. Vehicle- and ddI-treated kidney tissues were used comparatively. As expected, vehicle and ddI treatments resulted in no renal microscopic changes (Figure 2, top and bottom panels). Glomeruli and tubules also appeared to be intact in both TDF-treated WTs and in vehicle-treated TGs (Figure 2, middle panels). After 5 weeks of treatment with TDF or ddI, detectable renal tubular or glomerular damage was not found.
EM Features of Mitochondria in Tubular Epithelium with Tenofovir
To investigate the organelle-specific effect of tenofovir on renal proximal tubules, ultrastructural changes in renal tubular epithelial mitochondria were defined parametrically. Vehicle-treated WTs showed renal proximal tubular epithelial cells with characteristic, oval mitochondria having densely packed cristae (Figure 3, upper left panel). Renal tubule EM profiles from WTs treated with TDF or ddI also appeared unchanged from vehicle-treated littermates (Figure 3, top center and right panels).
Mitochondria from renal proximal tubular cells of vehicle-treated TGs were oblong, but resembled WTs with respect to the mitochondrial cristae (Figure 3, lower left panel). Renal tubular epithelia of TDF-treated TGs showed an increased number of mitochondria, with irregular mitochondrial shape, and sparse, fragmented cristae (Figure 3, lower middle panel, arrows). ddI caused no changes in the size and number of mitochondria in renal tubular epithelia (Figure 3, lower right panel).
LCM-Isolated Proximal Tubular mtDNA Abundance
Proximal tubules were microdissected from kidney sections using LCM (Figure 4a) to determine the specific effect of tenofovir on this histological compartment. Proximal tubules were defined histopathologically by staining with PAS to highlight the glycoprotein-rich brush border.
mtDNA abundance in LCM-retrieved renal proximal tubular epithelial cells after treatment. Histology sections were stained with PAS for identifying proximal tubules. Proximal tubules were selectively microdissected from formalin-fixed paraffin-embedded kidney tissues using LCM. (a) Captured images of renal tissue before (left) and after (center) sample microdissection along with resultant isolated proximal tubules (right; original magnification × 20). mtDNA abundance in LCM samples were determined using real-time PCR. (b) mtDNA abundance decreased in proximal tubules from TGS treated with TDF (Mann–Whitney unpaired t-test). ddI had no effect on proximal tubular mtDNA abundance.
mtDNA abundance in renal proximal tubules decreased in TGs treated with TDF, compared with that in vehicle-treated TGs and WT controls (Figure 4b, left graph). TDF treatment of WTs also resulted in decreased mtDNA abundance compared with that of vehicle-treated WTs, although not enough to be significant. In contrast, treatment with ddI had no effect on proximal tubular epithelial mtDNA abundance (Figure 4b, right graph). Thus, tenofovir toxicity depleted mtDNA in proximal tubules in comparison to its effects on total mtDNA in the homogenized tissue.
DISCUSSION
These studies offer novel and mechanistic data to clarify subcellular events in clinical tenofovir renal toxicity. They provide evidence that tenofovir causes renal proximal tubular mitochondrial ultrastructural abnormalities that are parallel to mtDNA depletion in the same cells. Isolation of renal proximal tubules using LCM provided tissue-specific evidence of the compartmentalized toxic effects of tenofovir on renal tubules, and localized the toxic site anatomically and molecularly. To our knowledge, this is the first time that mitochondrial toxicity is localized to an anatomically and functionally distinct tissue in a complex organ.
A paradoxical increase in steady-state mtDNA abundance was found in homogenized whole kidneys. As mtDNA abundance, as reported here, is a ratio between mtDNA and nDNA, the resultant change in mtDNA abundance may be the result of a change in the level of mtDNA or in the level of nDNA. Thus, an increase in mtDNA or decrease in nDNA could yield an increase in that ratio. Histologically, nuclei appeared to be as intact and as abundant in the TDF-treated TG renal tissue as was seen in the littermate controls. Renal tubules are characteristically multinucleated, and a detailed enumeration of nuclei was determined in these studies. Alternatively, there was direct EM evidence of an increase in mitochondria with irregular shape and fragmented cristae in the TDF-treated TGs, compared with that in the WT controls. Thus, it is possible to suggest the mtDNA in these studies were altered (mtDNA level increased), whereas the nDNA remained intact (nDNA level remained constant), resulting in the identified change in mtDNA abundance. This result extends earlier studies17, 21, 24, 25 that focused on disruption of mtDNA biogenesis, potentially at the level of the mitochondrial nucleotide pools.
The compartmentalized toxicity of tenofovir at the organelle level of mitochondria in renal proximal tubules suggests that tenofovir toxicity may be directly related to its metabolic processing. As tenofovir is eliminated by active secretion through the renal tubules, impaired or delayed elimination of tenofovir would lead to its accumulation. Increased tenofovir abundance in the proximal tubules and its phosphorylation in those cells could create an imbalance in nucleotide pools,30 thereby disrupting mitochondrial biogenesis.31
HIVAN was first described in 1984 with HIV infection,32 before any antiretroviral agents were available. Therefore, it seems likely that tenofovir tubular disease and HIVAN are separate events with distinct mechanisms, because HIVAN was reported over a decade before TDF was used. In both human and experimental HIVAN, all tissue compartments are affected, including glomeruli with collapsing focal segmental glomerulosclerosis and tubular and interstitial cells with tubulointerstitial disease.33, 34, 35 In contrast, tenofovir primarily targets proximal tubules. An HIV TG model was used here to delineate the individual and combined effects of TG and tenofovir.
Neither TG nor TDF treatment alone induced detectable molecular or ultrastructural changes within the short-term study of 5 weeks. Vehicle-treated TGs had no change in mtDNA abundance in whole-kidney tissues from WTs. These data confirm the absence of HIVAN in a C57/BL6 background. TDF treatment of WTs caused no change in mtDNA abundance. Only TDF treatment in TGs resulted in a significant change in mtDNA abundance, compared with that in vehicle-treated WTs. A logical conclusion is that this observed synergy is the result of local HIV gene expression and tenofovir.
It may be possible that neither TG nor TDF treatment alone is sufficient within 5 weeks (short term) to yield detectable changes. Expanding studies of longer treatment duration may result in detectable changes in TDF-treated WTs, supporting cumulative toxicity. Moreover, coexistence of the TG with TDF treatment may cause the phenotype to occur more robustly or earlier.
The NRTI toxicity in these studies was both tissue and treatment specific (ie, renal proximal tubule and TDF). It must be noted that TDF treatment had no effect on either cardiac or liver mtDNA abundance, and toxicity of TDF is not reported in those organs. In contrast, ddI hepatotoxicity occurred. The outcome with ddI treatment supports earlier studies.36, 37
In summary, tenofovir caused renal proximal tubular ultrastructural defects (mitochondria) and depleted mtDNA in that specialized tissue. Tenofovir caused no such change in the heart or liver, and ddI caused no such change in the kidney. The data of these studies support the hypothesis that specific NRTIs for HIV/AIDS show toxicity to mitochondria in specific tissues. The findings provide a nexus between tissue and organelle toxicity. Additional studies may help define why individual NRTIs show relatively selective organ toxicity, yet seem to involve mitochondria in diverse tissues.
References
Lyseng-Williamson KA, Reynolds NA, Plosker GL . Tenofovir disoproxil fumarate: a review of its use in the management of HIV infection. Drugs 2005;65:413–432.
Vivet-Boudou V, Didierjean J, Isel C, et al.. Nucleoside and nucleotide inhibitors of HIV-1 replication. Cell Mol Life Sci 2006;63:163–186.
Lewis W, Gonzalez B, Chomyn A, et al.. Zidovudine induces molecular, biochemical, and ultrastructural changes in rat skeletal muscle mitochondria. J Clin Invest 1992;89:1354–1360.
Lewis W, Grupp IL, Grupp G, et al.. Cardiac dysfunction occurs in the HIV-1 transgenic mouse treated with zidovudine. Lab Invest 2000;80:187–197.
Lewis W . Mitochondrial DNA replication, nucleoside reverse-transcriptase inhibitors, and AIDS cardiomyopathy. Prog Cardiovasc Dis 2003;45:305–318.
Sulkowski MS, Mehta SH, Torbenson M, et al.. Hepatic steatosis and antiretroviral drug use among adults coinfected with HIV and hepatitis C virus. Aids 2005;19:585–592.
Lund KC, Peterson LL, Wallace KB . Absence of a universal mechanism of mitochondrial toxicity by nucleoside analogs. Antimicrob Agents Chemother 2007;51:2531–2539.
Bruggeman LA, Thomson MM, Nelson PJ, et al.. Patterns of HIV-1 mRNA expression in transgenic mice are tissue-dependent. Virology 1994;202:940–948.
Lewis W, Haase CP, Raidel SM, et al.. Combined antiretroviral therapy causes cardiomyopathy and elevates plasma lactate in transgenic AIDS mice. Lab Invest 2001;81:1527–1536.
Price CJ, George JD, Marr MC, et al.. Prenatal developmental toxicity evaluation of 2′,3′-dideoxyinosine (ddI) and 2′,3′-didehydro-3′-deoxythymidine (d4T) co-administered to Swiss Albino (CD-1) mice. Birth Defects Res B Dev Reprod Toxicol 2006;77:207–215.
Fux CA, Christen A, Zgraggen S, et al.. Effect of tenofovir on renal glomerular and tubular function. Aids 2007;21:1483–1485.
Mocroft A, Kirk O, Gatell J, et al.. Chronic renal failure among HIV-1-infected patients. Aids 2007;21:1119–1127.
Cote HC, Magil AB, Harris M, et al.. Exploring mitochondrial nephrotoxicity as a potential mechanism of kidney dysfunction among HIV-infected patients on highly active antiretroviral therapy. Antivir Ther 2006;11:79–86.
Vidal F, Domingo JC, Guallar J, et al.. In vitro cytotoxicity and mitochondrial toxicity of tenofovir alone and in combination with other antiretrovirals in human renal proximal tubule cells. Antimicrob Agents Chemother 2006;50:3824–3832.
Birkus G, Hajek M, Kramata P, et al.. Tenofovir diphosphate is a poor substrate and a weak inhibitor of rat DNA polymerases alpha, delta, and epsilon*. Antimicrob Agents Chemother 2002;46:1610–1613.
Lewis W . Mitochondrial dysfunction and nucleoside reverse transcriptase inhibitor therapy: experimental clarifications and persistent clinical questions. Antiviral Res 2003;58:189–197.
Lewis W, Copeland WC, Day B . Mitochondrial DNA depletion, oxidative stress and mutation: mechanisms of nucleoside reverse transcriptase inhibitor toxicity. Lab Invest 2001;81:777–790.
Delaney WEt, Ray AS, Yang H, et al.. Intracellular metabolism and in vitro activity of tenofovir against hepatitis B virus. Antimicrob Agents Chemother 2006;50:2471–2477.
Lu TC, He JC, Klotman P . Animal models of HIV-associated nephropathy. Curr Opin Nephrol Hypertens 2006;15:233–237.
Dickie P, Felser J, Eckhaus M, et al.. HIV-associated nephropathy in transgenic mice expressing HIV-1 genes. Virology 1991;185:109–119.
Lewis W, Day BJ, Kohler JJ, et al.. Decreased mtDNA, oxidative stress, cardiomyopathy, and death from transgenic cardiac targeted human mutant polymerase gamma. Lab Invest 2007;87:326–335.
Lewis W, Haase CP, Miller YK, et al.. Transgenic expression of the deoxynucleotide carrier causes mitochondrial damage that is enhanced by NRTIs for AIDS. Lab Invest 2005;85:972–981.
Lewis W, Kohler JJ, Hosseini SH, et al.. Antiretroviral nucleosides, deoxynucleotide carrier and mitochondrial DNA: evidence supporting the DNA pol gamma hypothesis. Aids 2006;20:675–684.
Kohler JJ, Hosseini SH, Green E, et al.. Cardiac-targeted transgenic mutant mitochondrial enzymes: mtDNA defects, antiretroviral toxicity and cardiomyopathy. Cardiovasc Toxicol 2008;8:57–69.
Hosseini SH, Kohler JJ, Haase CP, et al.. Targeted transgenic overexpression of mitochondrial thymidine kinase (TK2) alters mitochondrial DNA (mtDNA) and mitochondrial polypeptide abundance: transgenic TK2, mtDNA, and antiretrovirals. Am J Pathol 2007;170:865–874.
Cote HC, Yip B, Asselin JJ, et al.. Mitochondrial:nuclear DNA ratios in peripheral blood cells from human immunodeficiency virus (HIV)-infected patients who received selected HIV antiretroviral drug regimens. J Infect Dis 2003;187:1972–1976.
Dalakas MC, Illa I, Pezeshkpour GH, et al.. Mitochondrial myopathy caused by long-term zidovudine therapy. N Engl J Med 1990;322:1098–1105.
Emmert-Buck MR, Bonner RF, Smith PD, et al.. Laser capture microdissection. Science 1996;274:998–1001.
Barnett V, Lewis T . Outliers in Statistical Data. Wiley: Hoboken, 1994.
Bianchi V . Nucleotide pool unbalance induced in cultured cells by treatments with different chemicals. Toxicology 1982;25:13–18.
Mercy L, Pauw A, Payen L, et al.. Mitochondrial biogenesis in mtDNA-depleted cells involves a Ca2+-dependent pathway and a reduced mitochondrial protein import. FEBS J 2005;272:5031–5055.
Herman ES, Klotman PE . HIV-associated nephropathy: epidemiology, pathogenesis, and treatment. Semin Nephrol 2003;23:200–208.
Shah SN, He CJ, Klotman P . Update on HIV-associated nephropathy. Curr Opin Nephrol Hypertens 2006;15:450–455.
Pope SD, Johnson MD, May DB . Pharmacotherapy for human immunodeficiency virus-associated nephropathy. Pharmacotherapy 2005;25:1761–1772.
Wyatt CM, Rosenstiel PE, Klotman PE . HIV-associated nephropathy. Contrib Nephrol 2008;159:151–161.
Youssef JA, Badr MZ . Disruption of mitochondrial energetics and DNA synthesis by the anti-AIDS drug dideoxyinosine. Toxicol Lett 1992;60:197–202.
Walker UA, Setzer B, Venhoff N . Increased long-term mitochondrial toxicity in combinations of nucleoside analogue reverse-transcriptase inhibitors. Aids 2002;16:2165–2173.
Acknowledgements
The authors thank the Emory Center for AIDS Research and the Department of Pathology Experimental Core Laboratory for their support. Dr Vanessa Bijol is also thanked for her expertise and guidance in analyzing the renal tissues.
Author information
Authors and Affiliations
Corresponding author
Additional information
The studies were supported by Grants R01 HL059798 and R01 HL079867 to WL. JJK was supported by Grant K01 DK078513.
Rights and permissions
About this article
Cite this article
Kohler, J., Hosseini, S., Hoying-Brandt, A. et al. Tenofovir renal toxicity targets mitochondria of renal proximal tubules. Lab Invest 89, 513–519 (2009). https://doi.org/10.1038/labinvest.2009.14
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2009.14
Keywords
This article is cited by
-
Pathophysiological and Genetic Basis of Tenofovir-Induced Acute Renal Dysfunction: Strategies and Recent Developments for Better Clinical Outcomes
Current Pharmacology Reports (2022)
-
Longitudinal renal changes in chronic hepatitis B patients treated with entecavir versus TDF: a REAL-B study
Hepatology International (2022)
-
ABCC4 single-nucleotide polymorphisms as markers of tenofovir disoproxil fumarate-induced kidney impairment
The Pharmacogenomics Journal (2021)
-
Identifying the role of PrimPol in TDF-induced toxicity and implications of its loss of function mutation in an HIV+ patient
Scientific Reports (2020)
-
Utility of urinary liver-type fatty acid-binding protein as a predictor of renal dysfunction in Japanese patients with HIV receiving tenofovir disoproxil fumarate with low urinary β2 microglobulin levels: a retrospective observational study
Journal of Pharmaceutical Health Care and Sciences (2019)