Abstract
Objective:
Closing patent ductus arteriosus (PDA) is a widely accepted approach in the management of very low birth weight (VLBW) infants. Our objective is to test the hypothesis that conservative management (no treatment) of PDA will not affect survival without chronic lung diseases (CLD).
Study Design:
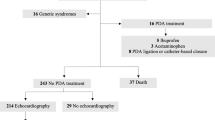
This retrospective study utilizes a prospectively collected database to compare two cohorts of VLBW infants. Infants in the first group (2001 to 2009) had their PDA treated with pharmacological and if necessary with surgical ligation. PDA in the second group (2010 to 2014) was not treated with medical or surgical intervention. The primary outcome was survival without oxygen requirement at 36 weeks. Pulmonary and non-pulmonary morbidities were also compared. Logistic regression analyses were performed to control for confounders.
Results:
This study included 643 VLBW infants, of them 415 infants in the Treat group and 228 in the No-Treat group. The rate of survival without CLD did not differ between Treat and No-Treat groups (78.4% vs 83.9%, respectively; adjusted odds ratio (aOR)=1.72, confidence interval (CI): 0.92 to 3.23, P=0.09). Mortality declined in No-Treat group (15.2% vs 10.5%, aOR=0.51, CI: 0.25 to 0.99, P=0.049), but the two groups did not differ in the incidence of CLD among survivors (5.8% vs 5.0%,=P0.47). Pulmonary complications and non-pulmonary morbidities did not differ between groups.
Conclusions:
Conservative management (no treatment) of PDA may not compromise survival without CLD and is not associated with increased morbidities in VLBW infants. Prospective physiological studies are needed to determine the sector of VLBW infants, if any, who could benefit from PDA treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Kitterman JA . Patent ductus arteriosus: current clinical status. Arch Dis Child 1980; 55 (2): 106–109.
Kitterman JA, Edmunds LH Jr, Gregory GA, Heymann MA, Tooley WH, Rudolph AM . Patent ducts arteriosus in premature infants. Incidence, relation to pulmonary disease and management. N Engl J Med 1972; 287 (10): 473–477.
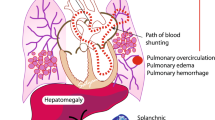
Kluckow M, Evans N . Ductal shunting, high pulmonary blood flow, and pulmonary hemorrhage. J Pediatr 2000; 137 (1): 68–72.
Dollberg S, Lusky A, Reichman B . Patent ductus arteriosus, indomethacin and necrotizing enterocolitis in very low birth weight infants: a population-based study. J Pediatr Gastroenterol Nutr 2005; 40 (2): 184–188.
Evans N, Kluckow M . Early ductal shunting and intraventricular haemorrhage in ventilated preterm infants. Arch Dis Child Fetal Neonatal Ed 1996; 75 (3): F183–F186.
Laughon MM, Simmons MA, Bose CL . Patency of the ductus arteriosus in the premature infant: is it pathologic? Should it be treated? Curr Opin Pediatr 2004; 16 (2): 146–151.
Morrow WR, Taylor AF, Kinsella JP, Lally KP, Gerstmann DR, deLemos RA . Effect of ductal patency on organ blood flow and pulmonary function in the preterm baboon with hyaline membrane disease. Crit Care Med 1995; 23 (1): 179–186.
Meyers RL, Alpan G, Lin E, Clyman RI . Patent ductus arteriosus, indomethacin, and intestinal distension: effects on intestinal blood flow and oxygen consumption. Pediatr Res 1991; 29 (6): 569–574.
Benitz WE . Treatment of persistent patent ductus arteriosus in preterm infants: time to accept the null hypothesis. J Perinatol 2010; 30 (4): 241–252.
Peckham GJ, Miettinen OS, Ellison RC, Kraybill EN, Gersony WM, Zierler S et al. Clinical course to 1 year of age in premature infants with patent ductus arteriosus: results of a multicenter randomized trial of indomethacin. J Pediatr 1984; 105 (2): 285–291.
Schmidt B, Roberts RS, Fanaroff A, Davis P, Kirpalani HM, Nwaesei C et al. Indomethacin prophylaxis, patent ductus arteriosus, and the risk of bronchopulmonary dysplasia: further analyses from the Trial of Indomethacin Prophylaxis in Preterms (TIPP). J Pediatr 2006; 148: 6.
Fanos V, Benini D, Verlato G, Errico G, Cuzzolin L . Efficacy and renal tolerability of ibuprofen vs. indomethacin in preterm infants with patent ductus arteriosus. Fundam Clin Pharmacol 2005; 19 (2): 187–193.
Shorter NA, Liu JY, Mooney DP, Harmon BJ . Indomethacin-associated bowel perforations: a study of possible risk factors. J Pediatr Surg 1999; 34 (3): 442–444.
Watterberg KL, Gerdes JS, Cole CH, Aucott SW, Thilo EH, Mammel MC et al. Prophylaxis of early adrenal insufficiency to prevent bronchopulmonary dysplasia: a multicenter trial. Pediatrics 2004; 114 (6): 1649–1657.
Van Bel F, Van de Bor M, Stijnen T, Baan J, Ruys JH . Cerebral blood flow velocity changes in preterm infants after a single dose of indomethacin: duration of its effect. Pediatrics 1989; 84 (5): 802–807.
Ohlsson A, Walia R, Shah SS . Ibuprofen for the treatment of patent ductus arteriosus in preterm or low birth weight (or both) infants. Cochrane Database Syst Rev 2015; 2: Cd003481.
Sekar KC, Corff KE . Treatment of patent ductus arteriosus: indomethacin or ibuprofen? J Perinatol 2008; 28 (Suppl 1): S60–S62.
Ohlsson A, Shah PS . Paracetamol (acetaminophen) for patent ductus arteriosus in preterm or low-birth-weight infants. Cochrane Database Syst Rev 2015; 3: Cd010061.
Chorne N, Leonard C, Piecuch R, Clyman RI . Patent ductus arteriosus and its treatment as risk factors for neonatal and neurodevelopmental morbidity. Pediatrics 2007; 119 (6): 1165–1174.
The Victorian Infant Collaborative Study Group. Surgery and the tiny baby: sensorineural outcome at 5 years of age. J Paediatr Child Health 1996; 32 (2):167–172.
Kabra NS, Schmidt B, Roberts RS, Doyle LW, Papile L, Fanaroff A . Neurosensory impairment after surgical closure of patent ductus arteriosus in extremely low birth weight infants: results from the trial of indomethacin prophylaxis in preterms. J Pediatr 2007; 150 (3): 229–234, 234.e1.
Wickremasinghe AC, Rogers EE, Piecuch RE, Johnson BC, Golden S, Moon-Grady AJ et al. Neurodevelopmental outcomes following two different treatment approaches (early ligation and selective ligation) for patent ductus arteriosus. J Pediatr 2012; 161 (6): 1065–1072.
Clement WA, El-Hakim H, Phillipos EZ, Coté JJ . Unilateral vocal cord paralysis following patent ductus arteriosus ligation in extremely low-birth-weight infants. Arch Otolaryngol Head Neck Surg 2008; 134 (1): 28–33.
Smith ME, King JD, Elsherif A, Muntz HR, Park AH, Kouretas PC . Should all newborns who undergo patent ductus arteriosus ligation be examined for vocal fold mobility? Laryngoscope 2009; 119 (8): 1606–1609.
Mandhan P, Brown S, Kukkady A, Samarakkody U . Surgical closure of patent ductus arteriosus in preterm low birth weight infants. Congenit Heart Dis 2009; 4 (1): 34–37.
Lippmann M, Nelson RJ, Emmanouilides GC, Diskin J, Thibeault DW . Ligation of patent ductus arteriosus in premature infants. Br J Anaesth 1976; 48 (4): 365–369.
Gould DS, Montenegro LM, Gaynor JW, Lacy SP, Ittenbach R, Stephens P et al. A comparison of on-site and off-site patent ductus arteriosus ligation in premature infants. Pediatrics 2003; 112 (6 I): 1298–1301.
Roclawski M, Sabiniewicz R, Potaz P, Smoczynski A, Pankowski R, Mazurek T et al. Scoliosis in patients with aortic coarctation and patent ductus arteriosus: does standard posterolateral thoracotomy play a role in the development of the lateral curve of the spine? Pediatr Cardiol 2009; 30 (7): 941–945.
Shelton JE, Julian R, Walburgh E, Schneider E . Functional scoliosis as a long-term complication of surgical ligation for patent ductus arteriosus in premature infants. J Pediatr Surg 1986; 21 (10): 855–857.
Clyman R, Cassady G, Kirklin JK, Collins M, Philips Iii JB . The role of patent ductus arteriosus ligation in bronchopulmonary dysplasia: reexamining a randomized controlled trial. J Pediatr 2009; 154 (6): 873–876.
Malviya MN, Ohlsson A, Shah SS . Surgical versus medical treatment with cyclooxygenase inhibitors for symptomatic patent ductus arteriosus in preterm infants. Cochrane Database Syst Rev 2013; 3: Cd003951.
Benitz WE . Patent ductus arteriosus in preterm infants. Pediatrics 2016; 137 (1):e20153730.
Jhaveri N, Moon-Grady A, Clyman RI . Early surgical ligation versus a conservative approach for management of patent ductus arteriosus that fails to close after indomethacin treatment. J Pediatr 2010; 157 (3): 381–387, 387.e381.
Aly H, Massaro AN, Patel K, El-Mohandes AA . Is it safer to intubate premature infants in the delivery room? Pediatrics 2005; 115 (6): 1660–1665.
Patel RM, Kandefer S, Walsh MC, Bell EF, Carlo WA, Laptook AR et al. Causes and timing of death in extremely premature infants from 2000 through 2011. N Engl J Med 2015; 372 (4): 331–340.
Aly H, Milner JD, Patel K, El-Mohandes AA . Does the experience with the use of nasal continuous positive airway pressure improve over time in extremely low birth weight infants? Pediatrics 2004; 114 (3): 697–702.
Schmidt B, Davis P, Moddemann D, Ohlsson A, Roberts RS, Saigal S et al. Long-term effects of indomethacin prophylaxis in extremely-low-birth-weight infants. N Engl J Med 2001; 344 (26): 1966–1972.
Acknowledgements
We thank Veronica Amaya for her assistance in editing the manuscript and making figures.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Mohamed, M., El-Dib, M., Alqahtani, S. et al. Patent ductus arteriosus in premature infants: to treat or not to treat?. J Perinatol 37, 652–657 (2017). https://doi.org/10.1038/jp.2017.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2017.4
This article is cited by
-
Patent ductus arteriosus treatment trends and associated morbidities in neonates
Scientific Reports (2021)
-
An experience with a bubble CPAP bundle: is chronic lung disease preventable?
Pediatric Research (2020)
-
Patent ductus arteriosus ligation on neurodevelopmental outcomes at corrected 2 years
Italian Journal of Pediatrics (2019)
-
Pharmacological closure of the patent ductus arteriosus: when treatment still makes sense
Journal of Perinatology (2019)
-
Letter to the editor: Treatment of patent ductus arteriosus in premature infants
Journal of Perinatology (2018)