Abstract
Objective:
A systematic review (2005) of observational studies has reported 87% reduction in the incidence of necrotizing enterocolitis (NEC) after introducing standardized feeding regimen (SFR) in preterm infants. Considering the many new studies in this field since 2005 and the continued health burden of NEC, we aimed to systematically review the incidence of NEC in preterm infants ‘before’ vs ‘after’ implementing a SFR.
Study Design:
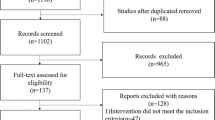
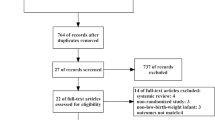
PubMed, EMBASE, CINAHL and E-abstracts from the Pediatric Academic Society meetings and other pediatric and neonatal conference proceedings were searched in May 2016. Observational studies reporting incidence of NEC before and after implementing a SFR were included. Relevant data were extracted independently by two reviewers. Meta-analysis was conducted using random effects model (REM) and results rechecked with fixed effects model.
Results:
Pooled results from 15 observational studies (N=18 160) using REM showed that SFR significantly reduced the incidence of NEC (risk ratio 0.22; 95% confidence interval 0.13 to 0.36; P<0.00001; I2=74%). The results remained significant after comparing studies in two epochs (1978 to 2003 vs 2004 to 2016).
Conclusion:
SFR continues to be an important tool in prevention of NEC in preterm infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Schulzke SM, Deshpande GC, Patole SK . Neurodevelopmental outcomes of very low-birth-weight infants with necrotizing enterocolitis: a systematic review of observational studies. Arch Pediatr Adolesc Med 2007; 161: 583–590.
Bedrick AD . Necrotizing enterocolitis: neurodevelopmental ‘risky business’. J Perinatol 2004; 24: 531–533.
Gupta A, Paria A . Etiology and medical management of NEC. Early Hum Dev 2016; 97: 17–23.
Lin HY, Chang JH, Chung M-Y, Lin HC . Prevention of necrotizing enterocolitis in preterm very low birth weight infants: Is it feasible? J Formos Med Assoc 2014; 113: 490–497.
Ofek Shlomai N, Deshpande G, Rao S, Patole S . Probiotics for preterm neonates: what will it take to change clinical practice? Neonatology 2014; 105: 64–70.
Rao SC, Athalye-Jape GK, Deshpande GC, Simmer KN, Patole SK . Probiotic supplementation and late-onset sepsis in preterm infants: a meta-analysis. Pediatrics 2016; 137: 1–16.
Olsen R, Greisen G, Schrøder M, Brok J . Prophylactic probiotics for preterm infants: a systematic review and meta-analysis of observational studies. Neonatology 2016; 109: 105–112.
Aceti A, Gori D, Barone G, Callegari ML, Di Mauro A, Fantini MP et al. Probiotics for prevention of necrotizing enterocolitis in preterm infants: systematic review and meta-analysis. Ital J Pediatr 2015; 41: 89.
Lau CS, Chamberlain RS . Probiotic administration can prevent necrotizing enterocolitis in preterm infants: a meta-analysis. J Pediatr Surg 2015; 50: 1405–1412.
Athalye-Jape G, Deshpande G, Rao S, Patole S . Benefits of probiotics on enteral nutrition in preterm neonates: a systematic review. Am J Clin Nutr 2014; 100: 1508–1519.
Yang Y, Guo Y, Kan Q, Zhou XG, Zhou XY, Li Y . A meta-analysis of probiotics for preventing necrotizing enterocolitis in preterm neonates. Braz J Med Biol Res 2014; 47: 804–810.
AlFaleh K, Anabrees J . Probiotics for prevention of necrotizing enterocolitis in preterm infants. Cochrane Database Syst Rev 2014; 4: CD005496.
Bertelli C, Pillonel T, Torregrossa A, Prod'hom G, Fischer CJ, Greub G et al. Bifidobacterium longum bacteremia in preterm infants receiving probiotics. Clin Infect Dis 2015; 60: 924–927.
Zbinden A, Zbinden R, Berger C, Arlettaz R . Case series of Bifidobacterium longum bacteremia in three preterm infants on probiotic therapy. Neonatology 2015; 107: 56–59.
Sadowska-Krawczenko I, Paprzycka M, Korbal P, Wiatrzyk A, Krysztopa-Grzybowska K, Polak M et al. Lactobacillus rhamnosus GG suspected infection in a newborn with intrauterine growth restriction. Benef Microbes 2014; 5: 397–402.
Modi N . Probiotics and necrotising enterocolitis: the devil (as always) is in the detail. Commentary on N. Ofek Shlomai et al.: Probiotics for preterm neonates: what will it take to change clinical practice? (Neonatology 2014;105:64-70). Neonatology 2014; 105: 71–73.
Tarnow-Mordi W, Soll RF . Probiotic supplementation in preterm infants: it is time to change practice. J Pediatr 2014; 164: 959–960.
Pammi M, Abrams SA . Oral lactoferrin for the prevention of sepsis and necrotizing enterocolitis in preterm infants. Cochrane Database Syst Rev 2015; 2: CD007137.
Mitchell K, Lyttle A, Amin H, Shaireen H, Robertson HL, Lodha AK . Arginine supplementation in prevention of necrotizing enterocolitis in the premature infant: an updated systematic review. BMC Pediatr 2014; 14: 226.
Uauy RD, Fanaroff AA, Korones SB, Phillips EA, Phillips JB, Wright LL . Necrotizing enterocolitis in very low birth weight infants: biodemographic and clinical correlates. National Institute of Child Health and Human Development Neonatal Research Network. J Pediatr 1991; 119: 630–638.
Kamitsuka MD, Horton MK, Williams MA . The incidence of necrotizing enterocolitis after introducing standardized feeding schedules for infants between 1250 and 2500 grams and less than 35 weeks of gestation. Pediatrics 2000; 105: 379–384.
Patole S, McGlone L, Muller R . Virtual elimination of necrotising enterocolitis for 5 years: reasons? Med Hypotheses 2003; 61: 617–622.
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L et al. Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg 1978; 187: 1–7.
Patole SK, de Klerk N . Impact of standardised feeding regimens on incidence of neonatal necrotising enterocolitis: a systematic review and meta-analysis of observational studies. Arch Dis Child Fetal Neonatal Ed 2005; 90: F147–F151.
Kuzma-O’Reilly B, Duenas ML, Greecher C, Kimberlin L, Mujsce D, Miller D et al. Evaluation, development, and implementation of potentially better practices in neonatal intensive care nutrition. Pediatrics 2003; 111: e461–e470.
Street JS, Montgomery D, Alder SC, Lambert DK, Gerstmann DR, Christensen RD . Implementing feeding guidelines for NICU patients <2000 g results in less variability in nutritional outcomes. J Parenter Enteral Nutr 2006; 30: 515–518.
Christensen RD, Havraneck T, Gerstmann DR, Calhoun DA . Enteral administration of a simulated amniotic fluid to very low birth weight neonates. J Perinatol 2005; 25: 380–385.
Barney CK, Lambert DK, Alder SC, Scoffield SH, Schmutz N, Christensen RD . Treating feeding intolerance with an enteral solution patterned after human amniotic fluid: a randomized, controlled, masked, trial. J Perinatol 2007; 27: 28–31.
Patel AL, Trivedi S, Bhandari NP, Ruf A, Scala CM, Witowitch G et al. Reducing necrotizing enterocolitis in very low birth weight infants using quality-improvement methods. J Perinatol 2014; 34: 850–857.
Stefanescu BM, Gillam-Krakauer M, Stefanescu AR, Markham M, Kosinski JL . Very low birth weight infant care: adherence to a new nutrition protocol improves growth outcomes and reduces infectious risk. Early Hum Dev 2016; 94: 25–30.
Wiedmeier SE, Henry E, Baer VL, Stoddard RA, Eggert LD, Lambert DK et al. Center differences in NEC within one health-care system may depend on feeding protocol. Am J Perinatol 2008; 25: 5–11.
Viswanathan S, McNelis K, Super D, Einstadter D, Groh-Wargo S, Collin M . Standardized Slow Enteral Feeding Protocol and the Incidence of Necrotizing Enterocolitis in Extremely Low Birth Weight Infants. JPEN J Parenter Enteral Nutr 2015; 39: 644–654.
McCallie KR, Lee HC, Mayer O, Cohen RS, Hintz SR, Rhine WD . Improved outcomes with a standardized feeding protocol for very low birth weight infants. J Perinatol 2011; 31: S61–S67.
Hanson C, Sundermeier J, Dugick L, Lyden E, Anderson-Berry AL . Implementation, process, and outcomes of nutrition best practices for infants <1500 g. Nutr Clin Pract 2011; 26: 614–624.
Talavera MM, Bixler G, Cozzi C, Dail J, Miller RR, McClead R Jr et al. Quality improvement initiative to reduce the necrotizing enterocolitis rate in premature infants. Pediatrics 2016; 137 (5): e1-e8.
Higgins J, Green S (eds). Cochrane Handbook for Systematic Reviews of Interventions. Version 5.1.0 (updated March 2011). The Cochrane Collaboration: London, UK, 2011. Available at www.cochrane-handbook.org.
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 2000; 283: 2008–2012.
Sánchez-Tamayo T, Espinosa Fernández MG, Affumicato L, González López M, Fernández Romero V, Moreno Algarra MC et al. Reduction in necrotising enterocolitis after implementing an evidence-based enteral nutrition protocol in very low birth weight newborns. An Pediatr (Barc) 2016; 85: 291–299.
Brown EG, Sweet AY . Preventing necrotizing enterocolitis in neonates. JAMA 1978; 240: 2452–2454.
Spritzer R, Koolen AM, Baerts W, Fetter WP, Lafeber HN, Sauer PJ . A prolonged decline in the incidence of necrotizing enterocolitis after the introduction of a cautious feeding regimen. Acta Paediatr Scand 1988; 77: 909–911.
Patole SK, Kadalraja R, Tuladhar R, Almonte R, Muller R, Whitehall JS . Benefits of a standardised feeding regimen during a clinical trial in preterm neonates. Int J Clin Pract 2000; 54: 429–431.
Premji SS, Chessell L, Paes B, Pinelli J, Jacobson K . A matched cohort study of feeding practice guidelines for infants weighing less than 1,500 g. Adv Neonatal Care 2002; 2: 27–36.
Christensen RD, Gordon PV, Besner GE . Can we cut the incidence of necrotizing enterocolitis in half—today? Fetal Pediatr Pathol 2010; 29: 185–198.
Premji SS . Standardised feeding regimens: hope for reducing the risk of necrotising enterocolitis. Arch Dis Child Fetal Neonatal Ed 2005; 90: F192–F193.
Chauhan M, Henderson G, McGuire W . Enteral feeding for very low birth weight infants: reducing the risk of necrotising enterocolitis. Arch Dis Child Fetal Neonatal Ed 2008; 93: F162–F166.
Schnabl KL, Aerde JEV, Thomson AB, Clandinin MT . Necrotizing enterocolitis: a multifactorial disease with no cure. World J Gastroenterol 2008; 14: 2142–2161.
Obladen M . Necrotizing enterocolitis—150 years of fruitless search for the cause. Neonatology 2009; 96: 203–210.
Swanson JR . Necrotizing enterocolitis: is it time for zero tolerance? J Perinatol 2013; 33: 1–2.
Acknowledgements
Author contributions
All the authors contributed toward the design, concept and preparation of the manuscript. BJ and SP conducted literature search, included the eligible trials, analyzed the data and prepared the initial manuscript. SP was responsible for the intellectual content, concept of the study and finalized the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Jasani, B., Patole, S. Standardized feeding regimen for reducing necrotizing enterocolitis in preterm infants: an updated systematic review. J Perinatol 37, 827–833 (2017). https://doi.org/10.1038/jp.2017.37
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2017.37
This article is cited by
-
Multidisciplinary evidence-based tools for improving consistency of care and neonatal nutrition
Journal of Perinatology (2024)
-
Neonatal Necrotizing Enterocolitis: An Update on Pathophysiology, Treatment, and Prevention
Pediatric Drugs (2024)
-
Dilemmas in establishing preterm enteral feeding: where do we start and how fast do we go?
Journal of Perinatology (2023)
-
A quality improvement initiative to standardize time to initiation of enteral feeds after non-surgical necrotizing enterocolitis using a consensus-based guideline
Journal of Perinatology (2022)
-
Advancements in neonatology through quality improvement
Journal of Perinatology (2022)