Abstract
Objective:
To compare the symptomatology of pregnant women with suspected listeriosis to culture confirmed listeriosis.
Study Design:
All cases of suspected and culture confirmed pregnancy-associated listeriosis from a single center were retrospectively reviewed assessing demographics, clinical, laboratory and pathological findings, and maternal, fetal and neonatal outcomes.
Results:
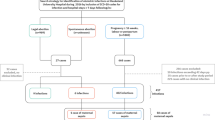
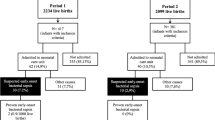
Listeriosis was identified in seven patients, none of whom belonged to the 117 women with suspected listeriosis. Women with confirmed infection were more likely to exhibit fever (P=0.01), flu-like symptoms (P=0.006), threatened preterm labor (P=0.05) and inflammatory markers (P=0.02), but less likely to exhibit gastrointestinal complaints (P=0.004) in comparison with suspected non-confirmed cases. Confirmed cases resulted in preterm delivery (n=5) and stillbirth (n=2). Neonatal complications included meningitis, respiratory disease and sepsis. Maternal outcomes were favorable.
Conclusion:
Although ‘febrile gastroenteritis’ is a poor predictor of listeriosis in pregnancy, fever, premature contractions and inflammatory markers are important risk indices prompting workup and adequate empiric treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Benshushan A, Tsafrir A, Arbel R, Rahav G, Ariel I, Rojansky N . Listeria infection during pregnancy: a 10 year experience. Isr Med Assoc J 2002; 4 (10): 776–780.
Soni DK, Singh DV, Dubey SK . Pregnancy—associated human listeriosis: virulence and genotypic analysis of Listeria monocytogenes from clinical samples. J Microbiol 2015; 53 (9): 653–660.
Crim SM, Iwamoto M, Huang JY, Griffin PM, Gilliss D, Tauxe R et al. Preliminary incidence and trends of infection with pathogens transmitted commonly through food—Foodborne Diseases Active Surveillance Network, 10 U.S. sites, 2006-2014. MMWR Morb Mortal Wkly Rep 2015; 64 (18): 495–499.
Silk BJ, Date KA, Pouillot R, Holt KH, Graves LM, Kanyin LO et al. Invasive listeriosis in the Foodborne Diseases Active Surveillance Network (FoodNet), 2004-2009: further targeted prevention needed for higher-risk groups. Clin Infect Dis 2012; 54 (Suppl 5): S396–S404.
Committee on Obstetric Practice AeCoOaG. Committee Opinion No. 614: Management of pregnant women with presumptive exposure to Listeria monocytogenes. Obstet Gynecol 2014; 124 (6): 1241–1244.
Hof H . An update on the medical management of listeriosis. Expert Opin Pharmacother 2004; 5 (8): 1727–1735.
Lamont RF, Sobel J, Mazaki-Tovi S, Kim SK, Uldbjerg N, Romero R et al. Listeriosis in human pregnancy: a systematic review. J Perinat Med 2011; 39 (3): 227–236.
Temple ME, Nahata MC . Treatment of listeriosis. Ann Pharmacother 2000; 34 (5): 656–661.
Gerner-Smidt P, Ethelberg S, Schiellerup P, Jensen A, Petersen AM, Bruun BG et al. Invasive listeriosis in Denmark 1994-2003: a review of 299 cases with special emphasis on risk factors for mortality. Clin Microbiol Infect 2005; 11 (8): 618–624.
Mylonakis E, Paliou M, Hohmann EL, Calderwood SB, Wing EJ . Listeriosis during pregnancy: a case series and review of 222 cases. Medicine (Baltimore) 2002; 81 (4): 260–269.
Elinav H, Hershko-Klement A, Valinsky L, Jaffe J, Wiseman A, Shimon H et al. Pregnancy-associated listeriosis: clinical characteristics and geospatial analysis of a 10-year period in Israel. Clin Infect Dis 2014; 59 (7): 953–961.
Ludvigsson JF . Effect of gastroenteritis during pregnancy on neonatal outcome. Eur J Clin Microbiol Infect Dis 2001; 20 (12): 843–849.
Angelo KM, Jackson KA, Wong KK, Hoekstra RM, Jackson BR . Assessment of the incubation period for invasive listeriosis. Clin Infect Dis 2016; 63 (11): 1487–1489.
Silver HM . Listeriosis during pregnancy. Obstet Gynecol Surv 1998; 53 (12): 737–740.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Fouks, Y., Amit, S., Many, A. et al. Listeriosis in pregnancy: under-diagnosis despite over-treatment. J Perinatol 38, 26–30 (2018). https://doi.org/10.1038/jp.2017.145
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2017.145
This article is cited by
-
Listeriosis during pregnancy: a retrospective cohort study
BMC Pregnancy and Childbirth (2022)