Abstract
Objective:
Non-invasive high-frequency ventilation (NIHFV), a relatively new modality, is gaining popularity despite limited data. We sought to evaluate the effectiveness of NIHFV versus bi-phasic continuous positive airway pressure (BP-CPAP) in preterm infants failing CPAP.
Study Design:
Infants with BW<1250 g on CPAP were randomly assigned to NIHFV or BP-CPAP if they met pre-determined criteria for CPAP failure. Infants were eligible for randomization after 72 h age and until 2000 g. Guidelines for adjustment of settings and criteria for failure of assigned mode were implemented. The primary aim was to assess feasibility of a larger trial. In addition, failure of assigned non-invasive respiratory support (NRS) mode, invasive mechanical ventilation (MV) 72 h and 7 days post-randomization, and bronchopulmonary dysplasia (BPD) were assessed.
Results:
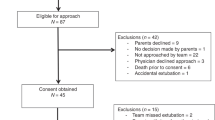
Thirty-nine infants were randomized to NIHFV (N=16) or BP-CPAP (N=23). There were no significant differences in mean (s.d.) postmenstrual age (28.6 (1.5) versus 29.0 (2.3) weeks, P=0.47), mean (s.d.) weight at randomization (965.0 (227.0) versus 958.1 (310.4) g, P=0.94) or other baseline demographics between the groups. Failure of assigned NRS mode was lower with NIHFV (37.5 versus 65.2%, P=0.09), although not statistically significant. There were no differences in rates of invasive MV 72 h and 7 days post-randomization or BPD.
Conclusion:
NIHFV was not superior to BP-CPAP in this pilot study. Effectiveness of NIHFV needs to be proven in larger multi-center, appropriately powered trials before widespread implementation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Donn SM, Sinha SK . Minimising ventilator induced lung injury in preterm infants. Arch Dis Child Fetal Neonatal Ed 2006; 91 (3): F226–F230.
Hart SM, McNair M, Gamsu HR, Price JF . Pulmonary interstitial emphysema in very low birthweight infants. Arch Dis Child 1983; 58 (8): 612–615.
Fan E, Villar J, Slutsky AS . Novel approaches to minimize ventilator-induced lung injury. BMC Med 2013; 11: 85.
Schmidt B, Asztalos EV, Roberts RS, Robertson CM, Sauve RS, Whitfield MF . Impact of bronchopulmonary dysplasia, brain injury, and severe retinopathy on the outcome of extremely low-birth-weight infants at 18 months: results from the trial of indomethacin prophylaxis in preterms. JAMA 2003; 289 (9): 1124–1129.
Owen LS, Morley CJ, Davis PG . Neonatal nasal intermittent positive pressure ventilation: a survey of practice in England. Arch Dis Child Fetal Neonatal Ed 2008; 93 (2): F148–F150.
Mahmoud RA, Roehr CC, Schmalisch G . Current methods of non-invasive ventilatory support for neonates. Paediatr Respir Rev 2011; 12 (3): 196–205.
Roberts CT, Davis PG, Owen LS . Neonatal non-invasive respiratory support: synchronised NIPPV, non-synchronised NIPPV or bi-level CPAP: what is the evidence in 2013? Neonatology 2013; 104 (3): 203–209.
Shah PS, Sankaran K, Aziz K, Allen AC, Seshia M, Ohlsson A et al. Canadian Neonatal Network. Outcomes of preterm infants <29 weeks gestation over 10-year period in Canada: a cause for concern? J Perinatol 2012; 32 (2): 132–138.
Stoll BJ, Hansen NI, Bell EF, Walsh MC, Carlo WA, Shankaran S . Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network. Trends in Care Practices, Morbidity, and Mortality of Extremely Preterm Neonates, 1993-2012. JAMA 2015; 314 (10): 1039–1051.
Chang HK, Harf A . High-frequency ventilation: a review. Respir Physiol 1984; 57 (2): 135–152.
Pillow JJ . High-frequency oscillatory ventilation: mechanisms of gas exchange and lung mechanics. Crit Care Med 2005; 33 (3 Suppl): S135–S141.
Mukerji A, Singh B, Helou SE, Fusch C, Dunn M, Belik J et al. Use of noninvasive high-frequency ventilation in the neonatal intensive care unit: a retrospective review. Am J Perinatol 2015; 30 (2): 171–176.
Colaizy TT, Younis UM, Bell EF, Klein JM . Nasal high-frequency ventilation for premature infants. Acta Paediatr 2008; 97 (11): 1518–1522.
Dumas, De La Roque E, Bertrand C, Tandonnet O, Rebola M, Roquand E et al. Nasal high frequency percussive ventilation versus nasal continuous positive airway pressure in transient tachypnea of the newborn: a pilot randomized controlled trial (NCT00556738). Pediatr Pulmonol 2011; 46 (3): 218–223.
van der Hoeven M, Brouwer E, Blanco CE . Nasal high frequency ventilation in neonates with moderate respiratory insufficiency. Arch Dis Child Fetal Neonatal Ed 1998; 79 (1): F61–F63.
Schulz KF, Altman DG, Moher D . CONSORT 2010 Statement: updated guidelines for reporting parallel group randomised trials. J Clin Epidemiol 2010; 63 (8): 834–840.
Papile LA, Burstein J, Burstein R, Koffler H . Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr 1978; 92 (4): 529–534.
Kugelman A, Durand M . A comprehensive approach to the prevention of bronchopulmonary dysplasia. Pediatr Pulmonol 2011; 46 (12): 1153–1165.
De Luca D, Carnielli VP, Conti G, Piastra M . Noninvasive high frequency oscillatory ventilation through nasal prongs: bench evaluation of efficacy and mechanics. Intensive Care Med 2010; 36 (12): 2094–2100.
De Luca D, Piastra M, Pietrini D, Conti G . Effect of amplitude and inspiratory time in a bench model of non-invasive HFOV through nasal prongs. Pediatr Pulmonol 2012; 47 (10): 1012–1018.
Mukerji A, Finelli M, Belik J . Nasal high-frequency oscillation for lung carbon dioxide clearance in the newborn. Neonatology 2013; 103 (3): 161–165.
Null DM, Alvord J, Leavitt W, Wint A, Dahl MJ, Presson AP et al. High-frequency nasal ventilation for 21 d maintains gas exchange with lower respiratory pressures and promotes alveolarization in preterm lambs. Pediatr Res 2014; 75 (4): 507–516.
Rehan VK, Fong J, Lee R, Sakurai R, Wang ZM, Dahl MJ et al. Mechanism of reduced lung injury by high-frequency nasal ventilation in a preterm lamb model of neonatal chronic lung disease. Pediatr Res 2011; 70 (5): 462–466.
Acknowledgements
We acknowledge NICU registered respiratory therapists at Mount Sinai Hospital, Toronto, Canada for assistance with recruitment and randomization. Sources of funding/grants from Sandra Schmirler Foundation. Clinicaltrials.gov ID: NCT02051491.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Data from this study were presented at Pediatric Academic Societies 2015.
Supplementary Information accompanies the paper on the Journal of Perinatology website .
Supplementary information
Rights and permissions
About this article
Cite this article
Mukerji, A., Sarmiento, K., Lee, B. et al. Non-invasive high-frequency ventilation versus bi-phasic continuous positive airway pressure (BP-CPAP) following CPAP failure in infants <1250 g: a pilot randomized controlled trial. J Perinatol 37, 49–53 (2017). https://doi.org/10.1038/jp.2016.172
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.172
This article is cited by
-
Nasal high-frequency oscillatory ventilation versus nasal continuous positive airway pressure as primary respiratory support strategies for respiratory distress syndrome in preterm infants: a systematic review and meta-analysis
European Journal of Pediatrics (2022)
-
Continuous positive airway pressure (CPAP) vs noninvasive positive pressure ventilation (NIPPV) vs noninvasive high frequency oscillation ventilation (NHFOV) as post-extubation support in preterm neonates: protocol for an assessor-blinded, multicenter, randomized controlled trial
BMC Pediatrics (2019)
-
Noninvasive high-frequency oscillatory ventilation as respiratory support in preterm infants: a meta-analysis of randomized controlled trials
Respiratory Research (2019)
-
Hazards to avoid in future neonatal studies of nasal high-frequency oscillatory ventilation: lessons from an early terminated trial
BMC Research Notes (2019)
-
Response to ‘Non-invasive high frequency ventilation and the errors from the past: designing simple trials neglecting complex respiratory physiology’
Journal of Perinatology (2017)