Abstract
Objective:
To determine whether chronic oxygen dependency at the time of discharge from the neonatal intensive care unit (NICU) in infants with bronchopulmonary dysplasia (BPD) predicts respiratory outcomes at 3 years.
Study design:
Preterm infants ⩽1250 g without BPD, BPD and BPD with chronic oxygen dependency were identified from the Southern Alberta Perinatal Follow-up clinic database (1995–2007). Respiratory outcomes at 4, 8, 18 and 36 months corrected age following NICU discharge were examined. Univariate analyses were done.
Results:
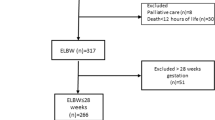
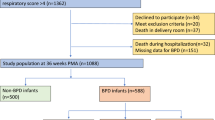
Out of 1563 infants admitted to the NICU, 1212 survived. Complete follow-up data at 36 months were available for 1030 (85%) children. Children with BPD with or without chronic oxygen dependency had significantly (P<0.001) lower birth weights and gestational ages, and greater post-natal steroid use, compared with those with no BPD. At 4, 8 and 18 months follow-up, the use of respiratory medications and supplemental oxygen were both significantly higher in the BPD infants with chronic oxygen dependency group compared with the no-BPD group and BPD group. At 36 months, children in the BPD with chronic oxygen dependency group were more likely to use respiratory medications and supplemental oxygen vs the no-BPD or the BPD groups. At 4, 8 and 36 months of age, more children in the BPD with chronic oxygen dependency group had post-neonatal chronic lung disease (PNCLD) than children in the other groups, but at 36 months the difference was significant only for the BPD with chronic oxygen dependency vs no-BPD group (P<0.001).
Conclusions:
At 36 months, children diagnosed with BPD with chronic oxygen dependency at NICU discharge were more likely to need respiratory medications and supplemental oxygen in the previous 12 months, as compared with no-BPD or BPD groups. They were also more likely to require frequent physician visits and have PNCLD at 3 years, as compared with the no-BPD group.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Vohr BR, Wright LL, Dusick AM, Perritt R, Poole WK, Tyson JE et al. Center differences and outcomes of extremely low birth weight infants. Pediatrics 2004; 113: 781–789.
Shennan AT, Dunn MS, Ohlsson A, Lennox K, Hoskins EM . Abnormal pulmonary outcomes in premature infants: prediction from oxygen requirement in the neonatal period. Pediatrics 1988; 82: 527–532.
Chess PR, D'Angio CT, Pryhuber GS, Maniscalco WM . Pathogenesis of bronchopulmonary dysplasia. Semin Perinatol 2006; 30: 171–178.
Koumbourlis AC, Motoyama EK, Mutich RL, Mallory GB, Walczak SA, Fertal K . Longitudinal follow-up of lung function from childhood to adolescence in prematurely born patients with neonatal chronic lung disease. Pediatr Pulmonol 1996; 21: 28–34.
Smith LJ, van Asperen PP, McKay KO, Selvadurai H, Fitzgerald DA . Reduced exercise capacity in children born very preterm. Pediatrics 2008; 122: e287–e293.
Carraro S, Filippone M, Da Dalt L, Ferraro V, Maretti M, Bressan S et al. Bronchopulmonary dysplasia: the earliest and perhaps the longest lasting obstructive lung disease in humans. Early Hum Dev 2013; 89 (Suppl 3): S3–S5.
Lodha A, Sauve R, Bhandari V, Tang S, Christianson H, Bhandari A et al. Need for supplemental oxygen at discharge in infants with bronchopulmonary dysplasia is not associated with worse neurodevelopmental outcomes at 3 years corrected age. PLoS One 2014; 9: e90843.
Lodha A, Zhu Q, Lee SK, Shah PS Canadian Neonatal Network. Neonatal outcomes of preterm infants in breech presentation according to mode of birth in Canadian NICUs. Postgrad Med J 2011; 87: 175–179.
CNN (2014). The Canadian Neonatal Network annual report 2013 [online]. Available at http://www.canadianneonatalnetwork.org/portal/.
Papile LA, Burstein J, Burstein R, Koffler H . Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr 1978; 92: 529–534.
An international classification of retinopathy of prematurity. The Committee for the Classification of Retinopathy of Prematurity. Pediatrics 1984; 74: 127–133.
Lee SK, Ye XY, Singhal N, De La Rue S, Lodha A, Shah PS . Higher altitude and risk of bronchopulmonary dysplasia among preterm infants. Am J Perinatol 2012; 30: 601–606.
Bhandari A, McGrath-Morrow S . Long-term pulmonary outcomes of patients with bronchopulmonary dysplasia. Semin Perinatol 2013; 37: 132–137.
Tapia JL, Agost D, Alegria A, Standen J, Escobar M, Grandi C et al. Bronchopulmonary dysplasia: incidence, risk factors and resource utilization in a population of South American very low birth weight infants. J Pediatr (Rio J) 2006; 82: 15–20.
Johnson TJ, Patel AL, Jegier BJ, Engstrom JL, Meier PP . Cost of morbidities in very low birth weight infants. J Pediatr 2013; 162: 243–249 e241.
Qiu X, Lodha A, Shah PS, Sankaran K, Seshia MM, Yee W et al. Neonatal outcomes of small for gestational age preterm infants in Canada. Am J Perinatol 2012; 29: 87–94.
Stroustrup A, Trasande L . Epidemiological characteristics and resource use in neonates with bronchopulmonary dysplasia: 1993-2006. Pediatrics 2010; 126: 291–297.
Heron M, Sutton PD, Xu J, Ventura SJ, Strobino DM, Guyer B . Annual summary of vital statistics: 2007. Pediatrics 2010; 125: 4–15.
Ehrenkranz RA, Walsh MC, Vohr BR, Jobe AH, Wright LL, Fanaroff AA et al. Validation of the National Institutes of Health consensus definition of bronchopulmonary dysplasia. Pediatrics 2005; 116: 1353–1360.
Bhandari A, Bhandari V . Pitfalls, problems, and progress in bronchopulmonary dysplasia. Pediatrics 2009; 123: 1562–1573.
Gien J, Kinsella JP . Pathogenesis and treatment of bronchopulmonary dysplasia. Curr Opin Pediatr 2011; 23: 305–313.
Kinsella JP, Greenough A, Abman SH . Bronchopulmonary dysplasia. Lancet 2006; 367: 1421–1431.
Doyle LW, Casalaz D Victorian Infant Collaborative Study Group. Outcome at 14 years of extremely low birthweight infants: a regional study. Arch Dis Child Fetal Neonatal Ed 2001; 85: F159–F164.
Lista G, Castoldi F, Bianchi S, Lupo E, Cavigioli F, Farolfi A et al. Lung function and respiratory health at school age in ventilated very low birth weight infants. Indian J Pediatr 2014; 81: 275–278.
Anand D, Stevenson CJ, West CR, Pharoah PO . Lung function and respiratory health in adolescents of very low birth weight. Arch Dis Child 2003; 88: 135–138.
Hennessy EM, Bracewell MA, Wood N, Wolke D, Costeloe K, Gibson A et al. Respiratory health in pre-school and school age children following extremely preterm birth. Arch Dis Child 2008; 93: 1037–1043.
Fawke J, Lum S, Kirkby J, Hennessy E, Marlow N, Rowell V et al. Lung function and respiratory symptoms at 11 years in children born extremely preterm: the EPICure study. Am J Respir Crit Care Med 2010; 182: 237–245.
Greenough A, Alexander J, Boorman J, Chetcuti PA, Cliff I, Lenney W et al. Respiratory morbidity, healthcare utilisation and cost of care at school age related to home oxygen status. Eur J Pediatr 2011; 170: 969–975.
Landry JS, Croitoru D, Jin Y, Schwartzman K, Benedetti A, Menzies D . Health care utilization by preterm infants with respiratory complications in Quebec. Can Respir J 2012; 19: 255–260.
Underwood MA, Danielsen B, Gilbert WM . Cost, causes and rates of rehospitalization of preterm infants. J Perinatol 2007; 27: 614–619.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Lodha, A., Ediger, K., Rabi, Y. et al. Does chronic oxygen dependency in preterm infants with bronchopulmonary dysplasia at NICU discharge predict respiratory outcomes at 3 years of age?. J Perinatol 35, 530–536 (2015). https://doi.org/10.1038/jp.2015.7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2015.7
This article is cited by
-
Polysomnography in Preterm Infants with Bronchopulmonary Dysplasia for Monitoring Sleep-Disordered Breathing and Pulmonary Reserve
Current Sleep Medicine Reports (2019)
-
Inter-center variation in death or tracheostomy placement in infants with severe bronchopulmonary dysplasia
Journal of Perinatology (2017)
-
In-hospital outcomes of premature infants with severe bronchopulmonary dysplasia
Journal of Perinatology (2017)