Abstract
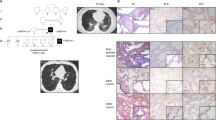
Inherited disorders of surfactant metabolism are manifested in neonatal period as a severe respiratory failure not responding to exogenous surfactant administration. We illustrate the case of a term newborn with respiratory failure because of compound heterozygous mutation in adenosine triphosphate-binding cassette transporter A3 (ABCA3)—in exon 24 M1227R and in exon 29 Ins1510fs/ter1519. These mutations of ABCA3 have not been described yet and expand the group of lethal ABCA3 variants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Hamvas A . Evaluation and management of inherited disorders of surfactant metabolism. Chin Med J 2010; 123 (20): 2943–2947.
Wert SE, Whitsett JA, Nogee LM . Genetic disorders of surfactant dysfunction. Pediatr Dev Pathol 2009; 12 (4): 253–274.
Matsumura Y, Ban N, Ueda K, Inagaki N . Characterization and classification of ATP-binding cassette transporter ABCA3 mutants in fatal surfactant deficiency. J Biol Chem 2006; 281: 34503–34514.
Shulenin S, Nogee LM, Annilo T, Wert SE, Whitsett JA, Dean M . ABCA3 Gene mutations in newborns with fatal surfactant deficiency. N Engl J Med 2004; 350: 1296–1303.
Flamein F, Riffault L, Muselet-Charlier C, Pernelle J, Feldmann D, Jonard L et al. Molecular and cellular characteristics of ABCA3 mutations associated with diffuse parenchymal lung diseases in children. Hum Mol Genet 2012; 21 (4): 765–775.
Bullard JE, Wert SE, Whitsett JA, Dean M, Nogee LM . ABCA3 mutations associated with pediatric interstitial lung disease. Am J Respir Crit Care Med 2005; 172: 1026–1031.
Wambach JA, Wegner DJ, DePass K, Heins H, Druley TE, Mitra RD et al. Single ABCA3 mutations increase risk for neonatal respiratory distress syndrome. Pediatrics 2012; 130 (6): e1575–e1582.
Jones KD, Dishop MK, Colby TV . Developmental and pediatric lung disease. In: Leslie KO, Wick MR (eds). Practical Pulmonary Pathology, 2nd edn, Saunders: Philadelphia, 2011; pp 91–116.
Adzhubei IA, Schmidt S, Peshkin L, Ramensky VE, Gerasimova A, Bork P et al. A method and server for predicting damaging missense mutations. Nat Methods 2010; 7 (4): 248–249.
Kumar P, Henikoff S, Ng PC . Predicting the effects of coding non-synonymous variants on protein function using the SIFT algorithm. Nat Protoc 2009; 4 (7): 1073–1081.
Thouvenin G, Nathan N, Epaud R, Clement A . Diffuse parenchymal lung disease caused by surfactant deficiency: dramatic improvement by azithromycin. BMJ Case Rep 2013; pii: bcr2013009988. doi:10.1136/bcr-2013-009988.
Cameron EJ, McSharry C, Chaudhuri R, Farrow S, Thomson NC . Long-term macrolide treatment of chronic inflammatory airway diseases: risks, benefits and future developments. Clin Exp Allergy 2012; 42 (9): 1302–1312.
Williamson M, Wallis C . Ten-year follow up of hydroxychloroquine treatment for ABCA3 deficiency. Pediatr Pulmonol 2014; 49: 299–301.
Kitazawa H, Moriya K, Niizuma H, Kawano K, Saito-Nanjo Y, Uchiyama T et al. Intersticial lung disease in two brothers with novel compound heterozygous ABCA3 mutations. Eur J Pediatr 2013; 172: 953–957.
Acknowledgements
We thank Professor Lawrence Nogee from Division of Neonatology, Department of Pediatrics, Johns Hopkins University School of Medicine, Baltimore, MD, USA, for the help in interpreting the results of DNA analysis. This study was supported by PRVOUK programme P37/12.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Malý, J., Navrátilová, M., Hornychová, H. et al. Respiratory failure in a term newborn due to compound heterozygous ABCA3 mutation: the case report of another lethal variant. J Perinatol 34, 951–953 (2014). https://doi.org/10.1038/jp.2014.132
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2014.132
This article is cited by
-
A novel synonymous ABCA3 variant identified in a Chinese family with lethal neonatal respiratory failure
BMC Medical Genomics (2021)
-
Fatal respiratory disease due to a homozygous intronic ABCA3 mutation: a case report
Journal of Medical Case Reports (2016)