Abstract
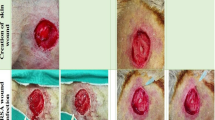
Preterm, critically ill neonates represent a challenge in wound healing. Many factors predispose infants to skin injuries, including decreased epidermal–dermal cohesion, deficient stratum corneum, relatively alkaline pH of skin surface, impaired nutrition and presence of multiple devices on the skin. We present a case series describing the use of medical-grade honey—Leptospermum honey (Medihoney), for successful treatment of slowly healing neonatal wounds, specifically stage 3 pressure ulcer, dehiscent and infected sternal wound, and full-thickness wound from an extravasation injury.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Singer AJ, Clark RA . Cutaneous wound healing. N Engl J Med 1999; 341 (10): 738–746.
Flanagan M . Improving accuracy of wound measurement in clinical practice. Ostomy Wound Manage 2003; 49 (10): 28–40.
Bergstrom N, Altman R, Alvarez O, Bennett A, Carson C, Frantz R et al Treatment of Pressure Ulcers. Clinical Practice Guideline, Number 15. AHCPR Publication no.95-0652. Rockville, Md.: Agency for Health Care Policy and Research, Public Health Service, U.S. Department of Health and Human Services 1994; 12.
Bell AL, Cavorai J . Noncontact ultrasound therapy for adjunctive treatment of nonhealing wounds: retrospective analysis. Phys Ther 2008; 68: 1517–1524.
Acton C, Dunwoody G . Honey: where should it be placed on the wound care formulary? Proceedings of the European Wound Management Association Conference: Lisbon, Portugal, 2008 Poster.
Acton C . Medihoney: a complete wound bed preparation product. Br J Nurs 2008; 17 (11): S44–S48.
Molan PC . Re-introducing honey in the management of wounds and ulcers-theory and practice. Ostomy Wound Manage 2002; 48 (1): 28–40.
Molan PC . Mode of Action In: White RJ, Cooper RA (eds). Honey: A Modern Wound Management Product. Wounds 2005. UK, Aberdeen.
Gethin G, Cowman S, Conroy R . The impact of Manuka honey dressings on the surface pH of chronic wounds. Int Wound J 2008; 5 (2): 185–194.
Yoon YM, Newlands C . Quality standards of medical grade Manuka honey In: White RJ, Cooper RA (eds). Honey: A Modern Wound Management Product. Wounds 2005. UK, Aberdeen.
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Boyar, V., Handa, D., Clemens, K. et al. Clinical experience with Leptospermum honey use for treatment of hard to heal neonatal wounds: case series. J Perinatol 34, 161–163 (2014). https://doi.org/10.1038/jp.2013.158
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2013.158
Keywords
This article is cited by
-
Honey and Wound Healing: An Update
American Journal of Clinical Dermatology (2017)