Abstract
Objective:
To explore the association of urinary N-terminal pro-brain natriuretic peptide (NT-proBNP) concentrations and closure of patent ductus arteriosus (PDA) in preterm infants.
Study design:
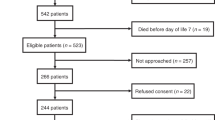
Blinded prospective study involving 136 preterm infants (median (interquartile range) gestational age 28 (26 to 30) weeks; birth weight 1030 (780 to 1270) g). NT-proBNP was determined in urine collected on day of life (DOL) 2, 7, 14 and 28.
Result:
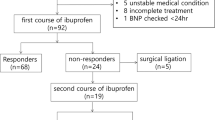
Urinary NT-proBNP/creatinine ratios declined continuously between DOL 2 (74 (17 to 248) μg g−1) and DOL 28 (4 (2 to 12) μg g−1) and were significantly elevated in ventilated infants on DOL 2, 7 and 14, and in ventilated infants with a hemodynamically significant PDA on DOL 2. Furthermore, urinary NT-proBNP/creatinine ratios on day 14 were higher in 14 ventilated infants who did not respond to pharmacological treatment and subsequently required surgical PDA closure (247 (214 to 547) μg g−1) than in ventilated infants (n=7) with successful pharmacological PDA closure (55 (21 to 114) μg g−1; P<0.05). A cutoff >210 μg g−1 on day 14 had a sensitivity of 75% and specificity of 100% for predicting non-responsiveness to pharmacological treatment.
Conclusion:
Measurement of urinary NT-proBNP is a new and simple non-invasive test for preterm infants, which may be helpful in guiding PDA treatment decisions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Hamrick SE, Hansmann G . Patent ductus arteriosus of the preterm infant. Pediatrics 2010; 125: 1020–1030.
Bancalari E, Claure N, Gonzalez A . Patent ductus arteriosus and respiratory outcome in premature infants. Biol Neonate 2005; 88: 192–201.
Chiruvolu A, Jaleel MA . Pathophysiology of patent ductus arteriosus in premature neonates. Early Hum Dev 2009; 85: 143–146.
Koch J, Hensley G, Roy L, Brown S, Ramaciotti C, Rosenfeld CR . Prevalence of spontaneous closure of the ductus arteriosus in neonates at a birth weight of 1000 grams or less. Pediatrics 2006; 117: 1113–1121.
Kwinta P, Rudzinski A, Kruczek P, Kordon Z, Pietrzyk JJ . Can early echocardiographic findings predict patent ductus arteriosus? Neonatology 2009; 95: 141–148.
Kluckow M, Seri I, Evans N . Functional echocardiography: an emerging clinical tool for the neonatologist. J Pediatr 2007; 150: 125–130.
Puddy VF, Amirmansour C, Williams AF, Singer DR . Plasma brain natriuretic peptide as a predictor of haemodynamically significant patent ductus arteriosus in preterm infants. Clin Sci (Lond) 2002; 103: 75–77.
Holmstrom H, Hall C, Thaulow E . Plasma levels of natriuretic peptides and hemodynamic assessment of patent ductus arteriosus in preterm infants. Acta Paediatr 2001; 90: 184–191.
Sanjeev S, Pettersen M, Lua J, Thomas R, Shankaran S, L’Ecuyer T . Role of plasma B-type natriuretic peptide in screening for hemodynamically significant patent ductus arteriosus in preterm neonates. J Perinatol 2005; 25: 709–713.
Flynn PA, da Graca RL, Auld PA, Nesin M, Kleinman CS . The use of a bedside assay for plasma B-type natriuretic peptide as a biomarker in the management of patent ductus arteriosus in premature neonates. J Pediatr 2005; 147: 38–42.
Ramakrishnan S, Heung YM, Round J, Morris TP, Collinson P, Williams AF . Early N-terminal pro-brain natriuretic peptide measurements predict clinically significant ductus arteriosus in preterm infants. Acta Paediatr 2009; 98: 1254–1259.
Nuntnarumit P, Khositseth A, Thanomsingh P . N-terminal probrain natriuretic peptide and patent ductus arteriosus in preterm infants. J Perinatol 2009; 29: 137–142.
Czernik C, Lemmer J, Metze B, Koehne PS, Mueller C, Obladen M . B-type natriuretic peptide to predict ductus intervention in infants <28 weeks. Pediatr Res 2008; 64: 286–290.
Farombi-Oghuvbu I, Matthews T, Mayne PD, Guerin H, Corcoran JD . N-terminal pro-B-type natriuretic peptide: a measure of significant patent ductus arteriosus. Arch Dis Child Fetal Neonatal Ed 2008; 93: F257–F260.
Hsu JH, Yang SN, Chen HL, Tseng HI, Dai ZK, Wu JR . B-type natriuretic peptide predicts responses to indomethacin in premature neonates with patent ductus arteriosus. J Pediatr 2010; 157: 79–84.
El-Khuffash AF, Amoruso M, Culliton M, Molloy EJ . N-terminal pro-B-type natriuretic peptide as a marker of ductal haemodynamic significance in preterm infants: a prospective observational study. Arch Dis Child Fetal Neonatal Ed 2007; 92: F421–F422.
Cortes R, Portoles M, Salvador A, Bertomeu V, Garcia de Burgos F, Martinez-Dolz L et al. Diagnostic and prognostic value of urine NT-proBNP levels in heart failure patients. Eur J Heart Fail 2006; 8: 621–627.
Linssen GC, Damman K, Hillege HL, Navis G, van Veldhuisen DJ, Voors AA . Urinary N-terminal prohormone brain natriuretic peptide excretion in patients with chronic heart failure. Circulation 2009; 120: 35–41.
Czernik C, Metze B, Müller C, Müller B, Bührer C . Urinary N-terminal B-type natriuretic peptide predicts severe retinopathy of prematurity. Pediatrics 2011; 128: 545–549.
Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA et al. Recommendations for chamber quantification: a report from the American Society of Echocardiography's guidelines and standards committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr 2005; 18: 1440–1463.
Skinner J . Diagnosis of patent ductus arteriosus. Semin Neonatol 2001; 6: 49–61.
Bland JM, Altman DG . Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986; 1: 307–310.
Ng LL, Geeranavar S, Jennings SC, Loke I, O’Brien RJ . Diagnosis of heart failure using urinary natriuretic peptides. Clin Sci (Lond) 2004; 106: 129–133.
Kroll MH, Srisawasdi P . The clearance of BNP modeled using the NT-proBNP-BNP relationship. Biosystems 2007; 88: 147–155.
Gournay V, Roze JC, Kuster A, Daoud P, Cambonie G, Hascoet JM et al. Prophylactic ibuprofen versus placebo in very premature infants: a randomised, double-blind, placebo-controlled trial. Lancet 2004; 364: 1939–1944.
Schmidt B, Davis P, Moddemann D, Ohlsson A, Roberts RS, Saigal S et al. Long-term effects of indomethacin prophylaxis in extremely-low-birth-weight infants. N Engl J Med 2001; 344: 1966–1972.
Madan JC, Kendrick D, Hagadorn JI, Frantz ID . Patent ductus arteriosus therapy: impact on neonatal and 18-month outcome. Pediatrics 2009; 123: 674–681.
Bose CL, Laughon MM . Patent ductus arteriosus: lack of evidence for common treatments. Arch Dis Child Fetal Neonatal Ed 2007; 92: F498–F502.
Laughon MM, Simmons MA, Bose CL . Patency of the ductus arteriosus in the premature infant: is it pathologic? Should it be treated? Curr Opin Pediatr 2004; 16: 146–151.
Van Overmeire B, Van de Broek H, Van Laer P, Weyler J, Vanhaesebrouck P . Early versus late indomethacin treatment for patent ductus arteriosus in premature infants with respiratory distress syndrome. J Pediatr 2001; 138: 205–211.
Daniels LB, Maisel AS . Natriuretic peptides. J Am Coll Cardiol 2007; 50: 2357–2368.
Toyoshima K, Momma K, Imamura S, Nakanishi T . In vivo dilatation of the postnatal ductus arteriosus by atrial natriuretic peptide in the rat. Neonatology 2007; 92: 139–144.
Acknowledgements
This study was supported by Roche Diagnostics, Mannheim, Germany. The assay manufacturer had no influence on study design, data analysis or interpretation or the content of this manuscript. We thank the Neonatal Intensive Care Unit nurses and doctors for their assistance during the examinations, and Janett Reiche and Fabian Holert of the Research Laboratory for technical support. We are very grateful to Sarah Smithson-Compton, MA for editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Czernik, C., Metze, B., Müller, C. et al. Urinary NT-proBNP and ductal closure in preterm infants. J Perinatol 33, 212–217 (2013). https://doi.org/10.1038/jp.2012.86
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2012.86
Keywords
This article is cited by
-
Base excess and hematocrit predict response to indomethacin in very low birth weight infants with patent ductus arteriosus
Italian Journal of Pediatrics (2019)
-
Early NT-proBNP levels as a screening tool for the detection of hemodynamically significant patent ductus arteriosus during the first week of life in very low birth weight infants
Journal of Perinatology (2018)
-
Urinary NT-proBNP levels and echocardiographic parameters for patent ductus arteriosus
Journal of Perinatology (2017)