Abstract
Objective:
To determine acceptance of donor human milk (DM) for feeding preterm infants and whether offering DM, alters mothers’ milk (MM) feeding.
Study Design:
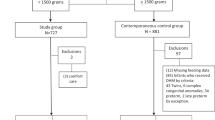
Infant feeding data were collected from medical records of 650 very preterm infants enrolled between 2006–2011 in two hospital level III neonatal intensive care units (NICUs) in Cincinnati, Ohio. The study was conducted during the implementation of a program offering 14 days of DM.
Result:
From 2006–2011, any DM use increased from 8 to 77% of infants, largely replacing formula for the first 2 weeks of life; provision of MM did not change. DM was more likely to be given in the first 2 weeks of life, if infants never received MM or were >1000 g birth weight, but DM use did not differ by sociodemographic factors.
Conclusion:
Offering DM dramatically increased human milk feeding and decreased formula use, but did not alter MM feeding in hospital.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
AAP. Breastfeeding and the use of human milk. American Academy of Pediatrics. Work group on breastfeeding. Pediatrics 1997; 100: 1035–1039.
Quigley MA, Henderson G, Anthony MY, McGuire W . Formula milk versus donor breast milk for feeding preterm or low birth weight infants. Cochrane Database Syst Rev. 2007; 17: CD002971.
Schanler RJ . Mother’s own milk, donor human milk, and preterm formulas in the feeding of extremely premature infants. J Pediatr Gastroenterol Nutr 2007; 45: S175–S177.
Schanler RJ, Shulman RJ, Lau C . Feeding strategies for premature infants: beneficial outcomes of feeding fortified human milk versus preterm formula. Pediatrics 1999; 103: 1150–1157.
Sullivan S, Schanler RJ, Kim JH, Patel AL, Trawöger R, Kiechl-Kohlendorfer U et al. An exclusively human milk-based diet is associated with a lower rate of necrotizing enterocolitis than a diet of human milk and bovine milk-based products. J Pediatr 2010; 156: 562–567 e561.
Porcelli PJ, Weaver RG . The influence of early postnatal nutrition on retinopathy of prematurity in extremely low birth weight infants. Early Hum Dev 2010; 86: 391–396.
Cregan MD, De Mello TR, Kershaw D, McDougall K, Hartmann PE . Initiation of lactation in women after preterm delivery. Acta Obstet Gynecol Scand 2002; 81: 870–877.
Orun E, Yalcin SS, Madendag Y, Ustunyurt-Eras Z, Kutluk S, Yurdakok K . Factors associated with breastfeeding initiation time in a baby-friendly hospital. Turk J Pediatr. 2010; 52: 10–16.
Schanler RJ, Lau C, Hurst NM, Smith EO . Randomized trial of donor human milk versus preterm formula as substitutes for mothers’ own milk in the feeding of extremely premature infants. Pediatrics 2005; 116: 400–406.
Bertino E, Giuliani F, Occhi L, Coscia A, Tonetto P, Marchino F et al. Benefits of donor human milk for preterm infants: current evidence. Early Hum Dev 2009; 85: S9–S10.
U.S. Department of Health and Human Services. The Surgeon General’s Call to Action to Support Breastfeeding. No. Office of the Surgeon General, 2011. http://www.surgeongeneral.gov/topics/breastfeeding/calltoactiontosupportbreastfeeding.pdf (Accessed November 7, 2011).
Ward L, Auer C, Smith C, Schoettker PJ, Pruett R, Shah NY et al. The human milk project: a quality improvement initiative to increase human milk consumption in very low birth weight infants. Breastfeeding Medicine 2012; 7: 234–240.
Lu MC, Lange L, Slusser W, Hamilton J, Halfon N . Provider encouragement of breast-feeding: evidence from a national survey. Obstet Gynecol 2001; 97: 290–295.
Wight NE . Donor human milk for preterm infants. J of perinatol 2001; 21: 249–254.
Ganapathy V, Hay JW, Kim JH . Costs of necrotizing enterocolitis and cost-effectiveness of exclusively human milk-based products in feeding extremely premature infants. Breastfeeding medicine 2012; 7: 29–37.
Nommsen-Rivers LA, Chantry CJ, Cohen RJ, Dewey KG . Comfort with the idea of formula feeding helps explain ethnic disparity in breastfeeding intentions among expectant first-time mothers. Breastfeed Med. 2010; 5: 25–33.
Guerrero ML, Morrow RC, Calva JJ, Ortega-Gallegos H, Weller SC, Ruiz-Palacios GM et al. Rapid ethnographic assessment of breastfeeding practices in periurban Mexico City. Bull World Health Organ. 1999; 77: 323–330.
Lee HC, Gould JB . Factors influencing breast milk versus formula feeding at discharge for very low birth weight infants in California. J Pediatr. 2009; 155: 657–662 e651-652.
Pineda RG . Predictors of breastfeeding and breastmilk feeding among very low birth weight infants. Breastfeeding medicine 2011; 6: 15–19.
Ostlund A, Nordstrom M, Dykes F, Flacking R . Breastfeeding in preterm and term twins--maternal factors associated with early cessation: a population-based study. J of hum lactat 2010; 26: 235–241 quiz 327-239.
McInnes RJ, Shepherd AJ, Cheyne H, Niven C . Infant feeding in the neonatal unit. Matern Child Nutr. 2010; 6: 306–317.
Mathur NB, Dhingra D . Perceived breast milk insufficiency in mothers of neonates hospitalized in neonatal intensive care unit. Indian J Pediatr. 2009; 76: 1003–1006.
Meier PP, Engstrom JL, Patel AL, Jegier BJ, Bruns NE . Improving the use of human milk during and after the NICU stay. Clin Perinatol. 2010; 37: 217–245.
Valentine CJ, Morrow G, Morrow AL . Promoting Pasteurized Donor Human Milk Use in the Neonatal Intensive Care Unit (NICU) as an Adjunct to Care and to Prevent Necrotizing Enterocolitis and shorten length of Stay In: Division of Dockets Management (HFA-305) FDA. (eds). FDA: Rockville, MD 20852, 2010 p. 389. http://www.fda.gov/downloads/AdvisoryCommittees/CommitteesMeetingMaterials/PediatricAdvisoryCommittee/UCM251799.pdf.
Vohr BR, Poindexter BB, Dusick AM, McKinley LT, Wright LL, Langer JC et al. Beneficial effects of breast milk in the neonatal intensive care unit on the developmental outcome of extremely low birth weight infants at 18 months of age. Pediatrics 2006; 118: e115–e123.
Montjaux-Regis N, Cristini C, Arnaud C, Glorieux I, Vanpee M, Casper C . Improved growth of preterm infants receiving mother's own raw milk compared with pasteurized donor milk. Acta Paediatr. 2011; 100: 1548–1554.
Acknowledgements
This study was partially supported by NIH grant funding, as follows: P01 HD13021 (ALM), R01 HD059140 (ALM and KRS), the Medical Student Summer Research Program under T35 DK060444 (ND) and NIH/NCRR 5UL1RR026314. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIH. We appreciate the expert review of the manuscript by Dr Laurie Nommsen-Rivers and gratefully acknowledge the work of Estelle Fischer, Cathy Grisby, Barbara Alexander, Lenora Jackson, Kristin Kirker, Greg Muthig and Donna Wuest.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Delfosse, N., Ward, L., Lagomarcino, A. et al. Donor human milk largely replaces formula-feeding of preterm infants in two urban hospitals. J Perinatol 33, 446–451 (2013). https://doi.org/10.1038/jp.2012.153
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2012.153
Keywords
This article is cited by
-
Introducing Donor Milk in a Neonatal Intensive Care Unit: A Developing Country’s Perspective
The Indian Journal of Pediatrics (2016)
-
Human Milk is the Feeding Strategy to Prevent Necrotizing Enterocolitis
Current Pediatrics Reports (2014)
-
Donor Human Milk: No Longer A Place For Formula in the Neonatal Intensive Care Unit?
Current Pediatrics Reports (2014)