Abstract
Objective:
Chronic hypertension (CHTN) is a risk factor for both intrauterine growth restriction (IUGR) as well as preeclampsia. This study was performed to: (1) describe the prevalence of IUGR in women with preeclampsia (with and without CHTN) compared with controls, (2) investigate the relationship between preeclampsia and maternal CHTN with IUGR, and (3) investigate the relationship between IUGR and severity of preeclampsia.
Study Design:
A case–control study was performed. Cases were patients identified with preeclampsia. Controls were patients presenting for delivery at term (⩾37 weeks). IUGR prevalence by case–control status, or severity of disease was evaluated using Pearson χ2 tests. Multivariable logistic regression was used to control for confounders.
Result:
In all, 430 cases and 568 controls were studied. Preeclamptic women have a 2.7 (CI (1.94 to 3.86)) and 4.3 (CI (2.58 to 7.17)) times increased odds of having a fetus with IUGR at <10 and <5% compared with controls in adjusted analyses. There was a significant interaction between CHTN and IUGR. Therefore, in women without CHTN, women with PEC had increased odds of IUGR, whereas in women with CHTN, there was no difference in odds of IUGR in women with or without preeclampsia. Within the cases, severe preeclampsia was associated with IUGR<10% (AOR=1.82 (1.11 to 2.97)) but not IUGR<5% (AOR=1.6 (0.85 to 2.86)).
Conclusion:
Preeclampsia is independently associated with the development of IUGR. As suggested earlier, women with CHTN do not have the highest prevalence of IUGR, suggesting disparate pathways by which IUGR develops in women with superimposed preeclampsia compared with preeclampsia alone.
Similar content being viewed by others
Introduction
Preeclampsia is a syndrome broadly defined by hypertension and proteinuria that affects 5 to 7% of all pregnancies. However, the diagnosis of preeclampsia encompasses a diverse maternal phenotype. Severe disease is not well defined but incorporates those patients with end organ manifestations, severe hypertension, coagulopathy, and/or those with preterm disease.1 Although the mechanism by which preeclampsia develops is not fully understood, some theories based in aberrant placental implantation and/or immune-mediated causes have led to investigations searching for the prevention and early detection strategies for this puzzling disease. The theory of abnormal placental implantation or reduced trophoblast invasion continues to link preeclampsia and intrauterine growth restriction (IUGR) as pregnancy disorders with a common pathogenesis.2 In fact, fetal IUGR has been traditionally included in the diagnostic criteria of severe preeclampsia regardless of other maternal manifestations of the disease.1 Historically, preeclampsia has been thought to lead to some of the most severe cases of IUGR.3
The impact of diagnosing severe preeclampsia after a certain gestational age is iatrogenic delivery, which often is preterm. Given the wide range of clinical phenotypes in preeclampsia, this raises the question of whether all the criteria that determine severity of preeclampsia should be managed similarly to optimize maternal and fetal outcome. Specifically, there is a lack of higher level evidence demonstrating that IUGR, in the absence of other severe maternal symptoms, should result in the diagnosis of severe disease and, therefore, impact clinical management.
Further confounding the relationship between preeclampsia and IUGR is that preexisting maternal co-morbid conditions, such as chronic hypertension (CHTN), have been associated with the development of IUGR, independent of preeclampsia.4, 5 Current theories suggest that the leading insult for IUGR in preeclampsia and in maternal preexisting CHTN is abnormal placental trophoblast invasion. If this theory is correct, one would expect that women with severe preeclampsia and those with CHTN with superimposed preeclampsia would have the highest risk of IUGR with the latter having the highest risk due to a ‘cumulative effect’.6 On the basis of this proposed pathogenesis, we would expect that women with mild preeclampsia compared with severe disease might be less likely to have fetuses affected by IUGR.
The aims of our study were (1) to describe the prevalence of IUGR in women with preeclampsia (with and without CHTN) compared with controls, (2) to investigate the relationship between IUGR and severity of preeclampsia, and (3) to elucidate the contribution of CHTN to the development of IUGR in women with and without preeclampsia.
Methods
After obtaining approval from the institutional review board, we performed a large case–control study, ‘Preeclampsia: Mechanisms and Consequences’ at the Hospital of the University of Pennsylvania. Cases and controls were collected prospectively and were frequency matched for race (African American vs other) given the baseline racial mix at our institution and the known predominance of preeclampsia among African American women.
All women admitted to Labor and Delivery with preeclampsia were eligible for enrollment. Cases were prospectively identified based solely on maternal criteria for preeclampsia. Classification of preeclampsia was based on maternal American College of Obstetrics and Gynecology guidelines. Mild preeclampsia included the diagnosis of gestational hypertension and was defined as blood pressure ⩾140/90 mm Hg on two measurements ⩾6 h apart and proteinuria (0 to 1+). Severe preeclampsia was defined as blood pressure ⩾140/90 mm Hg on two measurements ⩾6 h apart and >1+ proteinuria with any of the following: (1) platelets<120 K, (2) AST>45, (3) ALT>60, (4) creatinine ⩾1.0, (5) delivery before 37 weeks secondary to preeclampsia, (6) eclampsia, or (7) intravenous anti-hypertensive medications before delivery. Neither prenatal nor postnatal diagnosis of IUGR was included in our diagnostic criteria for preeclampsia. On the basis of these prespecified criteria, subclassification of preeclampsia into mild or severe categories was determined by the primary and senior author and not by physician diagnosis. Preterm preeclampsia was defined as those cases delivered at <34 weeks due to the diagnosis of preeclampsia. Controls were prospectively enrolled from women presenting for delivery at term (⩾37 weeks) either for scheduled induction of labor, scheduled cesarean section, spontaneous rupture of membranes, or term labor. Women with preexisting medical conditions or fetal anomalies were included in both the case and control groups.
Trained research nurses collected information on height, race, ethnicity, and family history by patient interview at the time of enrollment. Other history including obstetric, demographic, prenatal, delivery, and neonatal information were collected from prenatal and hospital chart abstraction by trained research nurse abstractors. The primary investigator reviewed all data sheets for completeness and consistency.
The diagnosis of CHTN was defined by patient history, prior use of anti-hypertensive medications, or blood pressure >140/90 mm Hg before 20 weeks gestation. Diabetes mellitus was defined as the presence of pregestational or gestational diabetes. The standard definitions for IUGR <10% (IUGR10) or <5% (IUGR5) were based on the Alexander curve reference for fetal growth using gestational age at delivery and actual birth weight.7
Statistical methods
The prevalence of IUGR among women with preeclampsia and controls as well as by severity of disease among women with preeclampsia was evaluated using Pearson χ2 tests of association. Significant confounders (race, maternal age (>30), CHTN, diabetes, tobacco use, and early pregnancy (from first prenatal visit) body mass index (BMI) ⩾30) were controlled for using multivariable logistic regression. Parity was not considered a confounder as it was only associated with preeclampsia and not with IUGR. Because of the case/control design, the outcome in the logistic models was case/control status, or severe vs mild preeclampsia. Tests for effect modification/interaction between CHTN and IUGR were also evaluated using stratified analyses and tests of interaction within logistic regression models. All analyses were performed using STATA statistical software, version 9.0 Special Edition (College Station, TX, USA).
Results
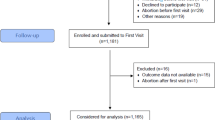
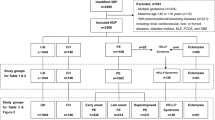
Over the study period from April 2005 to August 2007, approximately 10% of cases and 17% of controls approached declined participation. The total number of patients in our final analysis included 430 patients with preeclampsia (161 mild and 269 severe cases based on maternal criteria (Methods section) and 568 controls.
The demographic characteristics of our patients are presented in Table 1. Our controls represent a general obstetric population with approximate prevalence of 5% for CHTN and 4% for diabetes. There were no significant differences between patients with preeclampsia or controls with regard to tobacco use or mean gestational age of prenatal screening (14 vs 14.8 weeks). However, the proportion of African American women, women with a BMI⩾30 and primiparous women was slightly higher in the cases than in the controls.
Table 2 illustrates the prevalence of IUGR10 and IUGR5 by disease status. The prevalence of IUGR10 and IUGR5 was significantly different when the three groups (mild cases, severe cases, and controls) were compared. Table 3 shows the results of the multivariable logistic regression analyses comparing cases with controls. Women with preeclampsia have a 2.7 ((1.94 to 3.86)) and 4.3 ((2.58 to 7.17)) times increased odds of having a fetus with IUGR10 and IUGR5 compared with controls after controlling for confounders including race, maternal age (dichotomized at age >30), obesity (BMI⩾30), diabetes, CHTN, and tobacco use. Within the cases only, after controlling for these same confounders, there was an increased odds for IUGR10 (AOR=1.82, (1.11 to 2.97)) but not IUGR5 (AOR=1.56, (0.85 to 2.86)) among severe cases compared with mild cases. When cases delivered preterm (<34 weeks) were compared with cases delivered ⩾34 weeks, an increased odds of IUGR10 among the preterm cases was evident (AOR=1.7 (1 to 3), P=0.05).
Table 4 explores the prevalence of IUGR in women with and without CHTN in cases vs controls. Women who delivered with preeclampsia but without CHTN had the highest prevalence of IUGR. Although the total number of women with CHTN was small, there was significant effect modification/interaction between CHTN and IUGR10 (interaction P-value 0.04) after controlling for race, age>30, diabetes, BMI ⩾30, and tobacco use. Given this significant interaction, in women without CHTN, the odds of IUGR10 was 3.03 ((2.11 to 4.34), P=<0.001) times higher in the cases compared with controls. However, in women with CHTN, the odds of IUGR10 was similar between the cases and controls (OR=0.92, (0.30 to 2.82), P=0.88). The interaction between IUGR5 and CHTN was not significant (interaction P-value=0.62).
Discussion
As preeclampsia has a prevalence of approximately 5 to 7%, prospective studies are limited in their ability to study the prevalence of IUGR in women with preeclampsia and to assess the validity of incorporating IUGR in the definition of severe preeclampsia. With our case/control design and the fact that severe preeclampsia was defined in our study by maternal—not fetal—criteria, we were able to evaluate (1) the prevalence of IUGR in women with and without preeclampsia, (2) the relationship between IUGR and the severity of preeclampsia, and (3) the interaction between IUGR and CHTN. In our study, women with preeclampsia did have a higher prevalence of IUGR10 and IUGR5 when compared with controls, as earlier studies have demonstrated.4 There was a moderate increased prevalence of IUGR10 in severe cases when compared with mild cases of preeclampsia. However, one would have expected a much larger effect size difference when comparing both mild-to-severe cases and ⩽34-week cases to >34-week cases, given the current inclusion of IUGR into the diagnostic criteria for severe diseases. Further, although CHTN is an independent risk factor for IUGR and is independently associated with the development of preeclampsia, the mechanism by which these pregnancies develop IUGR seems to be more complicated. Our findings suggest that there may be disparate mechanisms by which IUGR occurs in patients with CHTN and superimposed preeclampsia, patients with only CHTN, and patients with preeclampsia alone. In patients with CHTN and superimposed preeclampsia, the pathogenesis of IUGR may be related by a variety of factors including the use of medications, aggressiveness of treatment of hypertension, or willingness to deliver at a clinically earlier stage in the disease process. Our findings emphasize that preeclampsia is associated with IUGR independent of CHTN. The lack of synergy between preeclampsia and CHTN in the development of IUGR (as these patients did not have the highest rates of IUGR) suggests that the pathways leading to the development of IUGR may be disparate and not all IUGR develops from the same mechanistic pathways.
Before developing strategies on prevention and treatment for the preeclampsia syndrome, the mechanisms by which IUGR occurs in the presence and absence of preeclampsia and further in the presence or absence of CHTN need to be further elucidated. Ness and Sibai8 suggest that the subset of women with both preeclampsia and IUGR result from a maternal predisposition to endothelial dysfunction leading to shallow placental implantation. Although this theory is plausible, the interaction between CHTN and IUGR that we observed, and its relationship to the development of preeclampsia, may suggest a separate mechanism.
In the WHO Antenatal Care Trial, Villar et al.9 suggest that unexplained IUGR, although presumed to share a similar etiology with preeclampsia, actually seems to be biologically separate. Other factors suggesting possible mechanistic differences between the development of preeclampsia and the development of IUGR are the disparate risk factors between the two processes. Diabetes, obesity, and CHTN have all been associated with the development of preeclampsia.4, 5, 10 However, IUGR is more common in women with lower BMI.11 Diabetes is often more likely to result in macrosomic rather than IUGR fetuses except in cases of long-standing diabetes with vascular complications.12 Further, tobacco use demonstrates this paradox with a strong association with IUGR but a protective effect in the development of preeclampsia.13, 14
The study design used for this investigation, a prospective case–control study, has several important advantages. First, we have a large number of cases including severe cases whose diagnosis was based solely on maternal criteria, allowing us to assess the independent association of the fetal condition with severe maternal disease. Second, these data were prospectively collected and are robust with information on clinically relevant exposure, outcome, and confounding variables that were strictly defined, with a small amount of missing data (<10%). Third, the prevalence of CHTN, diabetes, and IUGR in our control population and IUGR in our cases (28%) is similar to that reported in the literature, imparting validity to our results.4, 15, 16, 17
Although there are several strengths, we must also explicitly state the limitations of our study. The mean gestational ages of the cases and controls are different given our protocol for control selection. Second, there is potential for misclassification bias of exposure variables, particularly CHTN. Some women may have CHTN who were not classified as such due to lack of prior diagnosis secondary to lack of health care or late entry into prenatal care (⩾20 weeks). However, the comparability in the mean gestational age at screening of our cases and controls and the prevalence of CHTN in our controls makes this less of a concern. Third, with differences in provider threshold for delivery of women with preeclampsia (confounding by indication), some mild cases may have been misclassified as severe if women were delivered before the 37th week of gestation. However, this is not the standard practice at our institution. We also examined preterm cases (<34 weeks at delivery) to evaluate the most severe cases. Fourth, in this type of study design there is always the possibility that the assessment of the exposure status may have been influenced by our disease state. In this study, this is an unlikely limitation as the presence or absence of IUGR was based on actual birth weight and a standard curve, and the prevalence of IUGR in the cases and the controls correlates with earlier reports.
Our results suggest that the diagnosis of preeclampsia is significantly associated with IUGR. Interestingly, the development of IUGR in women with preeclampsia with and without CHTN may be disparate. Given these findings, further study is warranted to elucidate the potentially divergent pathogenesis leading to the development of preeclampsia and IUGR in women with CHTN vs those without. Further, the association between IUGR10 in mild and severe cases and preterm and non-preterm cases was present but there was only a mild-to-moderate association (<2-fold odds). Although severe disease is associated with IUGR10, it remains unclear if IUGR should be included in the diagnostic criteria for severe disease. The current inclusion of IUGR in the diagnostic criteria affects clinical management as some cases of IUGR occur in patients who would otherwise be deemed to have mild disease. It remains unclear whether delivery is the optimal management strategy in these women. Recent data reveal the morbidity associated with late preterm delivery.18, 19 Development of ultrasound testing and technology allows for more sophisticated methods to monitor fetuses affected by IUGR thereby allowing more conservative management. These modalities include umbilical artery and ductus venosus doppler studies. As the inclusion of IUGR in the diagnosis of severe disease currently suggests delivery, even in the absence of other maternal indications of severe disease, it is time to re-evaluate whether this is the optimal management strategy.
Conflict of interest
The authors declare no conflict of interest.
References
American College of Obstetrics and Gynecology Practice Bulletin 33. Diagnosis and Management of Preeclampsia and Eclampsia. January 2002.
Kaufman P, Black S, Huppertz B . Endovascular trophoblast invasion: implications for the pathogenesis of intrauterine growth retardation and preeclampsia. Biol Reprod 2003; 69: 1–7.
Ounsted M, Moar V, Scott WA . Perinatal morbidity and mortality in small-for-dates babies: the relative importance of some maternal factors. Early Hum Dev 1981; 5: 367–375.
American College of Obstetrics and Gynecology Practice Bulletin 12. Intrauterine Growth Restriction. January 2000.
Catov JM, Ness RB, Kip KE, Olsen J . Risk of early or severe preeclampsia related to pre-existing conditions. Int J Epidemiol. Oxford University Press: Oxford, UK, 2007; 36 (2): 412–419.
Sibai BM, Abdella TN, Anderson GD . Pregnancy outcome in 211 with mild chronic hypertension. Obstet Gynecol 1983; 61: 571–576.
Alexander GR, Himes JH, Kaufman RB, Mor J, Kogan M . A United States national reference for fetal growth. Obstet Gynecol 1996; 87 (2): 163–168.
Ness RB, Sibai BM . Shared and disparate components of the pathophysiologies of fetal growth restriction and preeclampsia. Am J Obstet Gynecol 2006; 195: 40–49.
Villar J, Carroli G, Wojdyla D, Abalos E, Giordano D, Ba'aqeel H et al. Preeclampsia, gestational hypertension and intrauterine growth restriction, related or independent conditions? Am J Obstet Gynecol 2006; 194: 921–931.
Sibai BM, Ewell M, Levine RJ, Klebanoff MA, Esterlitz J, Catalano PM et al. Risk factors associated with preeclampsia in healthy nulliparous women. The calcium for Preeclampsia Prevention (CPEP) Study Group. Am J Obstet Gynecol 1997; 177: 1003–1010.
Bernstein PS, Divon MY . Etiologies of fetal growth restriction. Clin Obstet Gynecol 1997; 40: 723–729.
Bradley RJ, Nicolaides KH, Brudenell JM . Are all infants of diabetic mothers ‘macrosomic’? BMJ 1998; 297: 1583–1584.
McDonald AD, Armstrong BJ, Sloan M . Cigarette, alcohol and coffee consumption and prematurity. Am J Public Health 1992; 82: 87–90.
Conde-Agudelo A, Althabe F, Belizan J, Kafury-Goeta A . Cigarette smoking during pregnancy and risk of preeclampsia: a systematic review. Am J Obstet Gynecol 1999; 181: 1026–1035.
American College of Obstetrics and Gynecology Practice Bulletin 29. Chronic Hypertension in Pregnancy. July 2001.
American College of Obstetrics and Gynecology Practice Bulletin 30. Gestational Diabetes. September 2001.
Walker JJ . Pre-eclampsia. Lancet 2000; 356: 1260–1265.
Raju TN, Higgins RD, Stark AR, Leveno KJ . Optimizing care and outcome for late-preterm (near-term) infants: a summary of the workshop sponsored by the National Institute of Child Health and Human Development. Pediatrics 2006; 118 (3): 1207–1214.
McIntire DD, Leveno KJ . Neonatal mortality and morbidity rates in late preterm births compared with births at term. Obstet Gynecol 2008; 111 (1): 35–41.
Acknowledgements
Part of this research was supported by a University of Pennsylvania Research Foundation Grant.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Srinivas, S., Edlow, A., Neff, P. et al. Rethinking IUGR in preeclampsia: dependent or independent of maternal hypertension?. J Perinatol 29, 680–684 (2009). https://doi.org/10.1038/jp.2009.83
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2009.83
Keywords
This article is cited by
-
Challenges in Conducting Clinical Trials for Preeclampsia
Current Hypertension Reports (2024)
-
Evaluating the predictive value of fetal Doppler indices and neonatal outcome in late-onset preeclampsia with severe features: a cross-sectional study in a resource-limited setting
BMC Pregnancy and Childbirth (2022)
-
The Association of Pregnancy-induced Hypertension with Bronchopulmonary Dysplasia – A Retrospective Study Based on the Korean Neonatal Network database
Scientific Reports (2020)
-
FOXD1 mutations are related to repeated implantation failure, intra-uterine growth restriction and preeclampsia
Molecular Medicine (2019)
-
Hypertensive disorders during pregnancy are associated with reduced severe intraventricular hemorrhage in very-low-birth-weight infants
Journal of Perinatology (2019)