Abstract
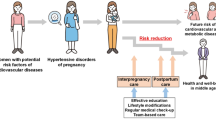
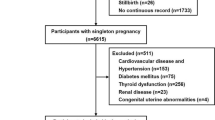
Previous studies in general people indicated that hypertensive disorders of pregnancy (HDP) increased the risk of subsequent hypertension after delivery. Some studies found that women with gestational diabetes mellitus (GDM) had an increased risk of HDP. However, very few studies have assessed the association between HDP and the risk of postpartum hypertension among GDM women. To evaluate the association between HDP and the risk of postpartum hypertension among GDM women, a retrospective cohort study was conducted in 1261 women with prior GDM at their postpartum 1–5 years using the baseline data from Tianjin Gestational Diabetes Mellitus Prevention Program. Cox regression models were applied to assess the single and joint associations of having a history of HDP, maternal pre-pregnancy Body mass index (BMI) (normal weight, overweight and obesity), and weight change from preconception to post-delivery with the risk of subsequent hypertension among the GDM women. We found that GDM women with a history of HDP, high pre-pregnancy BMI and weight gain >7 kg from preconception to post-delivery had an increased risk of postpartum hypertension. Joint effects analysis revealed that the positive association between a history of HDP in the index pregnancy and the risk of postpartum hypertension was consistent in GDM women with different levels of pre-pregnancy BMI or weight gain from preconception to post-delivery. In conclusion, a history of HDP, high pre-pregnancy BMI and weight gain >7 kg from preconception to post-delivery increase the risk of subsequent hypertension in postpartum 1–5 years among GDM women.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
WHO. WHO Recommendations for Prevention and Treatment of Pre-Eclampsia and Eclampsia. Geneva, 2011.
Kurabayashia T, Mizunuma H, Kubota T, Kiyohara Y, Nagai K, Hayashi K . Pregnancy-induced hypertension is associated with maternal history and a risk of cardiovascular disease in later life: a Japanese cross-sectional study. Maturitas 2013; 75 (3): 227–231.
Wilson BJ, Watson MS, Prescott GJ, Sunderland S, Campbell DM, Hannaford P et al. Hypertensive diseases of pregnancy and risk of hypertension and stroke in later life: results from cohort study. BMJ 2003; 326 (7394): 845.
Mannisto T, Mendola P, Vaarasmaki M, Jarvelin MR, Hartikainen AL, Pouta A et al. Elevated blood pressure in pregnancy and subsequent chronic disease risk. Circulation 2013; 127 (6): 681–690.
Lykke JA, Langhoff-Roos J, Sibai BM, Funai EF, Triche EW, Paidas MJ . Hypertensive pregnancy disorders and subsequent cardiovascular morbidity and type 2 diabetes mellitus in the mother. Hypertension 2009; 53 (6): 944–951.
Suzuki H, Watanabe Y, Arima H, Kobayashi K, Ohno Y, Kanno Y . Short- and long-term prognosis of blood pressure and kidney disease in women with a past history of preeclampsia. Clin Exp Nephrol 2008; 12 (2): 102–109.
Callaway LK, Mamun A, McIntyre HD, Williams GM, Najman JM, Nitert MD et al. Does a history of hypertensive disorders of pregnancy help predict future essential hypertension? Findings from a prospective pregnancy cohort study. J Hum Hypertens 2013; 27 (5): 309–314.
Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists' Task Force on Hypertension in Pregnancy. Obstet Gynecol 2013; 122 (5): 1122–1131.
Wallis AB, Saftlas AF, Hsia J, Atrash HK . Secular trends in the rates of preeclampsia, eclampsia, and gestational hypertension, United States, 1987-2004. Am J Hypertens 2008; 21 (5): 521–526.
Bryson CL, Ioannou GN, Rulyak SJ, Critchlow C . Association between gestational diabetes and pregnancy-induced hypertension. Am J Epidemiol 2003; 158 (12): 1148–1153.
Metzger BE, Coustan DR . Summary and recommendations of the Fourth International Workshop-Conference on Gestational Diabetes Mellitus. The Organizing Committee. Diabetes Care 1998; 21 (Suppl 2): B161–B167.
Bellamy L, Casas JP, Hingorani AD, Williams D . Type 2 diabetes mellitus after gestational diabetes: a systematic review and meta-analysis. Lancet 2009; 373 (9677): 1773–1779.
Contreras F, Rivera M, Vasquez J, De la Parte MA, Velasco M . Diabetes and hypertension physiopathology and therapeutics. J Hum Hypertens 2000; 14 (Suppl 1): S26–S31.
Carpenter MW . Gestational diabetes, pregnancy hypertension, and late vascular disease. Diabetes care 2007; 30: S246–S250.
Kaaja R, Gordin D . Health after pregnancy in the mother with diabetes. Womens Health 2015; 11 (4): 471–476.
Li W, Liu H, Qiao Y, Lv F, Zhang S, Wang L et al. Metabolic syndrome of weight change from pre-pregnancy to 1-5 years post-partum among Chinese women with prior gestational diabetes. Diabet Med 2015; 32 (11): 1492–1499.
WHO ConsultationDefinition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus. World Health Organisation: Geneva, 1999.
Hu G, Tian H, Zhang F, Liu H, Zhang C, Zhang S et al. Tianjin Gestational Diabetes Mellitus Prevention Program: study design, methods, and 1-year interim report on the feasibility of lifestyle intervention program. Diabetes Res Clin Pract 2012; 98 (3): 508–517.
Li YP, He YN, Zhai FY, Yang XG, Hu XQ, Zhao WH et al. Comparison of assessment of food intakes by using 3 dietary survey methods. Zhonghua Yu Fang Yi Xue Za Zhi 2006; 40 (4): 273–280.
Ma G, Luan D, Li Y, Liu A, Hu X, Cui Z et al. Physical activity level and its association with metabolic syndrome among an employed population in China. Obes Rev 2008; 9 (Suppl 1): 113–118.
Yuan X, Liu H, Wang L, Zhang S, Zhang C, Leng J et al. Gestational hypertension and chronic hypertension on the risk of diabetes among gestational diabetes women. J Diabetes Complications 2016; 30 (7): 1269–1274.
Zhou B . Predictive values of body mass index and waist circumference to risk factors of related diseases in Chinese adult population. Zhonghua liu xing bing xue za zhi 2002; 23 (1): 5–10.
Mansia G, De Backer G, Dominiczak A, Cifkova R, Fagard R, Germano G et al. ESH-ESC Guidelines for the management of arterial hypertension: the task force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Blood Press 2007; 16 (3): 135–232.
Bellamy L, Casas JP, Hingorani AD, Williams DJ . Pre-eclampsia and risk of cardiovascular disease and cancer in later life: systematic review and meta-analysis. BMJ 2007; 335 (7627): 974.
Hwang JW, Park SJ, Oh SY, Chang SA, Lee SC, Park SW et al. The risk factors that predict chronic hypertension after delivery in women with a history of hypertensive disorders of pregnancy. Medicine 2015; 94 (42): e1747.
Colatrella A, Loguercio V, Mattei L, Trappolini M, Festa C, Stoppo M et al. Hypertension in diabetic pregnancy: impact and long-term outlook. Best pract Res Clin Endocrinol Metab 2010; 24 (4): 635–651.
Tobias DK, Hu FB, Forman JP, Chavarro J, Zhang C . Increased risk of hypertension after gestational diabetes mellitus: findings from a large prospective cohort study. Diabetes care 2011; 34 (7): 1582–1584.
Heida KY, Franx A, van Rijn BB, Eijkemans MJ, Boer JM, Verschuren MW et al. Earlier age of onset of chronic hypertension and type 2 diabetes mellitus after a hypertensive disorder of pregnancy or gestational diabetes mellitus. Hypertension 2015; 66 (6): 1116–1122.
Pirkola J, Pouta A, Bloigu A, Miettola S, Hartikainen AL, Jarvelin MR et al. Prepregnancy overweight and gestational diabetes as determinants of subsequent diabetes and hypertension after 20-year follow-up. J Clin Endocrinol Metab 2010; 95 (2): 772–778.
Solomon CG, Seely EW . Brief review: hypertension in pregnancy: a manifestation of the insulin resistance syndrome? Hypertension 2001; 37 (2): 232–239.
Hermes W, Franx A, van Pampus MG, Bloemenkamp KW, van der Post JA, Porath M et al. 10-Year cardiovascular event risks for women who experienced hypertensive disorders in late pregnancy: the HyRAS study. BMC Pregnancy Childbirth 2010; 10: 28.
Dietz P, Bombard J, Mulready-Ward C, Gauthier J, Sackoff J, Brozicevic P et al. Validation of self-reported maternal and infant health indicators in the Pregnancy Risk Assessment Monitoring System. Matern Child Health J 2014; 18 (10): 2489–2498.
Roberts CL, Bell JC, Ford JB, Hadfield RM, Algert CS, Morris JM . The accuracy of reporting of the hypertensive disorders of pregnancy in population health data. Hypertens Pregnancy 2008; 27 (3): 285–297.
Thomopoulos C, Salamalekis G, Kintis K, Andrianopoulou I, Michalopoulou H, Skalis G et al. Risk of hypertensive disorders in pregnancy following assisted reproductive technology: overview and meta-analysis. J Clin Hypertens (Greenwich) 2017; 19 (2): 173–183.
Ip MSM, Lam B, Ng MMT, Lam WK, Tsang KWT, Lam KSL . Obstructive sleep apnea is independently associated with insulin resistance. Am J Respir Crit Care Med 2002; 165 (5): 670–676.
Acknowledgements
This work is supported by the grant from European Foundation for the Study of Diabetes (EFSD)/Chinese Diabetes Society (CDS)/Lilly programme for Collaborative Research between China and Europe, Tianjin Women’s and Children’s Health Center and Tianjin Public Health Bureau. Dr GH was supported by grant from National Institute of Diabetes and Digestive and Kidney Diseases of the National Institutes of Health under Award Number R01DK100790. We would also like to appreciate all families for participating in Tianjin Gestational Diabetes Mellitus Prevention Programme. We would also like to appreciate all families for participating in Tianjin Gestational Diabetes Mellitus Prevention Program.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Wang, L., Leng, J., Liu, H. et al. Association between hypertensive disorders of pregnancy and the risk of postpartum hypertension: a cohort study in women with gestational diabetes. J Hum Hypertens 31, 725–730 (2017). https://doi.org/10.1038/jhh.2017.46
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2017.46
This article is cited by
-
Glycated albumin in pregnancy: reference intervals establishment and its predictive value in adverse pregnancy outcomes
BMC Pregnancy and Childbirth (2020)