Abstract
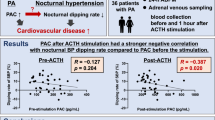
The pathophysiological mechanisms of arterial hypertension during hemodialysis (HD) in patients with end-stage renal disease (ESRD) are still poorly understood. The aim of this study is to investigate physiological, cardiovascular and neuroendocrine changes in patients with ESRD and its correlation with changes in blood pressure (BP) during the HD session. The present study included 21 patients with ESRD undergoing chronic HD treatment. Group A (study) consisted of patients who had BP increase and group B (control) consisted of those who had BP reduction during HD session. Echocardiograms were performed during the HD session to evaluate cardiac output (CO) and systemic vascular resistance (SVR). Before and after the HD session, blood samples were collected to measure brain natriuretic peptide (BNP), catecholamines, endothelin-1 (ET-1), nitric oxide (NO), electrolytes, hematocrit, albumin and nitrogen substances. The mean age of the studied patients was 43±4.9 years, and 54.6% were males. SVR significantly increased in group A (P<0.001). There were no differences in the values of BNP, NO, adrenalin, dopamin and noradrenalin, before and after dialysis, between the two groups. The mean value of ET-1, post HD, was 25.9 pg ml−1 in group A and 13.3 pg ml−1 in group B (P=<0.001). Patients with ESRD showed different hemodynamic patterns during the HD session, with significant BP increase in group A, caused by an increase in SVR possibly due to endothelial dysfunction, evidenced by an increase in serum ET-1 levels.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Agarwal R . Assessment of blood pressure in hemodialysis patients. Semin Dial 2002; 15: 299–304.
Lazar AE, Smith MC, Rahman M . Blood pressure measurement in hemodialysis patients. Semin Dial 2004; 17: 250–254.
Van Buren PN, Kim C, Toto R, Inrig JK . Intradialytic hypertension and the association with interdialytic ambulatory blood pressure. Clin J Am Soc Nephrol 2011; 6: 1684–1691.
Inrig JK, Patel UD, Toto RD, Szczech LA . Association of blood pressure increases during hemodialysis with 2-year mortality in incident hemodialysis patients: a secondary analysis of the Dialysis Morbidity and Mortality Wave 2 Study. Am J Kidney Dis 2009; 54: 881–890.
National High Blood Pressure Education Program. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. National Heart, Lung, and Blood Institute (US): Bethesda, MD, USA, 2004
Cheig JS, Milite C, Sullivan JF, Rubin AL, Stenzel KH . Hypertension is not adequately controlled in hemodialysis patients. Am J Kidny Dis 1992; 45: 453–459.
Agarwal R, Nissenson AR, Batlle D, Coyne DW . Prevalence, treatment and control of hypertension in chronic hemodialysis patientes in United States. Am J Med 2003; 115: 291–297.
Mees Douhort EJ . Rise in blood pressure during hemodialysis-ultrafiltration: a ‘paradoxical’ phenomenon? Int J Artif Organs 1996; 19: 569–570.
Cirit M, Akcicek F, Terzioglu E . Paradoxical rise in blood pressure in dialysis patients. Nephrol Dial Transplant 1994; 10: 1417–1419.
Hand MF, Haynes WG, Webb DJ . Hemodialysis and L-arginine but not D-arginine correct renal failure associated endothelial dysfunction. Kidney Int 1998; 53: 1068–1077.
Gunal AI, Karaca I, Celiker H, Ilkay E, Duman S . Paradoxical rise in blood pressure during ultrafiltration is caused by increased cardiac ouput. J Nephrol 2002; 15: 42–47.
Chou KJ, Lee PT, Chen CL, Chiou CW, Hsu CY, Chung HM et al. Physiological changes during hemodialysis in patients with intradialysis hypertension. Kidney Int 2006; 69: 1833–1888.
Weidman P, Maxwel MH, Lupu AN, Levin AJ, Massry SG . Plasma renin activity and blood pressure in terminal renal failure. N Engl J Med 1971; 285: 757–762.
Kuczera M, Hilgers KF, Lisson C, Ganten D, Hilgenfeldt U, Ritz E et al. Local angiotensin formation in hindlimbs of uremic hypertensive and renovascular hypertensive rats. J Hypertens 1991; 9: 41–48.
Converse JR, Jacobsen TN, Toto RD, Jost CM, Cosentino F, Fouad-Tarazi F et al. Sympathetic overactivity in patients with chronic renal failure. N Engl J Med 1995; 327: 1912–1918.
Amann K, Ritz E . Cardiovascular abnormalities in ageing and in uremia-only analogy or shared pathomecanism? Nephrol Dial Transplant 1998; 13: 6–11.
McGrath BP, Ledinham JGG, Benedict CR . Cathecolamines in peripheral venous plasma in patients on chronic hemodialysis. Clin Sci Mol Med 1978; 55: 89–96.
Gray DJ, Webb DJ . The endothelin system and is potential as therapeutic target in cardiovascular disease. Pharmacol Ther 1996; 72: 109–148.
Haynes WJ, Ferro CJ, O’Kane KP, Somerville D, Lomax CC, Webb DJ . Systemic endothelin receptor blockade decrease peripheral vascular resistance and blood pressure in humans. Circulation 1998; 93: 1860–1870.
Verhaar MC, Strachan FE, Newby DE, Cruden NL, Koomans HA, Rabelink TJ et al. Endothelin-A receptor antagonist-mediate vasodilation is attenuated by inhibition of nitric oxide synthesis and by endothelin-B receptor blockade. Circulation 1998; 97: 752–756.
Palmer RM, Ferrige AG, Moncada S . Nitric oxide release accounts for the biological activity of endotelium-derived relaxing factor. Nature 1987; 327: 524–526.
Baylis C, Wallance P . Nitric oxide and BP, Effects of NO deficiency. Curr Opin Nephrol Hypertens 1996; 5: 80–88.
Schmidt RJ, Domico J, Samsell LS, Yokota S, Tracy TS, Sorkin MI et al. Indices of activity of the nitric oxide system in hemodialysis patients. Am J Kidney Dis 1999; 34: 228–234.
Kielstein JT, Bögerrh RH, Bode-Böger SM, Schäfer J, Barbey M, Koch KM et al. Assymetric dimethylarginine plasma concentrations differ in patients with end-stage renal disease. Relationship to treatment method and atherosclerotic disease. J Am Soc Nephrol 1999; 10: 594–600.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Gutiérrez-Adrianzén, O., Moraes, M., Almeida, A. et al. Pathophysiological, cardiovascular and neuroendocrine changes in hypertensive patients during the hemodialysis session. J Hum Hypertens 29, 366–372 (2015). https://doi.org/10.1038/jhh.2014.93
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2014.93
This article is cited by
-
Time of hemodialysis and risk of intradialytic hypotension and intradialytic hypertension in maintenance hemodialysis
Journal of Human Hypertension (2023)
-
Negative Emotions in End-Stage Renal Disease: Are Anxiety Symptoms Related to Levels of Circulating Catecholamines?
Current Psychology (2020)
-
Hemodialysis patients with intradialytic rise in blood pressure display higher baseline aortic stiffness and negligible drop in augmentation index with dialysis
International Urology and Nephrology (2016)