Abstract
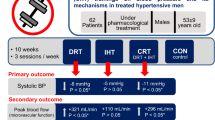
Post-exercise hypotension (PEH), the reduction of blood pressure (BP) after a single bout of exercise, is of great clinical relevance. As the magnitude of this phenomenon seems to be dependent on pre-exercise BP values and chronic exercise training in hypertensive individuals leads to BP reduction; PEH could be attenuated in this context. Therefore, the aim of the present study was to investigate whether PEH remains constant after resistance exercise training. Fifteen hypertensive individuals (46±8 years; 88±16 kg; 30±6% body fat; 150±13/93±5 mm Hg systolic/diastolic BP, SBP/DBP) were withdrawn from medication and performed 12 weeks of moderate-intensity resistance training. Parameters of cardiovascular function were evaluated before and after the training period. Before the training program, hypertensive volunteers showed significant PEH. After an acute moderate-intensity resistance exercise session with three sets of 12 repetitions (60% of one repetition maximum) and a total of seven exercises, BP was reduced post-exercise (45–60 min) by an average of aproximately −22 mm Hg for SBP, −8 mm Hg for DBP and −13 mm Hg for mean arterial pressure (P<0.05). However, this acute hypotensive effect did not occur after the 12 weeks of training (P>0.05). In conclusion, our data demonstrate that PEH, following an acute exercise session, can indeed be attenuated after 12 weeks of training in hypertensive stage 1 patients not using antihypertensive medication.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Kenney MJ, Seals DR . Postexercise hypotension. Key features, mechanisms, and clinical significance. Hypertension 1993; 22: 653–664.
MacDonald JR . Potential causes, mechanisms, and implications of post exercise hypotension. J Hum Hypertens 2002; 16: 225–236.
Motta DF, Lima LC, Arsa G, Russo PS, Sales MM, Moreira SR et al. Effect of type 2 diabetes on plasma kallikrein activity after physical exercise and its relationship to post-exercise hypotension. Diabetes Metab 2010; 36: 363–368.
Pontes Jr FL, Bacurau RF, Moraes MR, Navarro F, Casarini DE, Pesquero JL et al. Kallikrein kinin system activation in post-exercise hypotension in water running of hypertensive volunteers. Int Immunopharmacol 2008; 8: 261–266.
Pescatello LS, Franklin BA, Fagard R, Farquhar WB, Kelley GA, Ray CA . American College of Sports Medicine position stand. Exercise and hypertension. American College of Sports Medicine. Med Sci Sports Exerc 2004; 36: 533–553.
Cornelissen VA, Fagard RH . Effect of resistance training on resting blood pressure: a meta-analysis of randomized controlled trials. J Hypertens 2005; 23: 251–259.
Collier SR, Kanaley JA, Carhart Jr R, Frechette V, Tobin MM, Hall AK et al. Effect of 4 weeks of aerobic or resistance exercise training on arterial stiffness, blood flow and blood pressure in pre- and stage-1 hypertensives. J Hum Hypertens 2008; 22: 678–686.
Williams MA, Haskell WL, Ades PA, Amsterdam EA, Bittner V, Franklin BA et al. Resistance exercise in individuals with and without cardiovascular disease: 2007 update: a scientific statement from the American Heart Association Council on Clinical Cardiology and Council on Nutrition, Physical Activity, and Metabolism. Circulation 2007; 116: 572–584.
Moraes MR, Bacurau RFP, Ramalho JD, Reis FC, Casarini DE, Chagas JR et al. Increase in kinins on post-exercise hypotension in normotensive and hypertensive volunteers. Biol Chem 2007; 388: 533–540.
Mota MR, Pardono E, Lima LC, Arsa G, Bottaro M, Campbell CS et al. Effects of treadmill running and resistance exercises on lowering blood pressure during the daily work of hypertensive subjects. J Strength Cond Res 2009; 23: 2331–2338.
Melo CM, Alencar Filho AC, Tinucci T, Mion Jr D, Forjaz CL . Postexercise hypotension induced by low-intensity resistance exercise in hypertensive women receiving captopril. Blood Press Monit 2006; 11: 183–189.
Hamer M . The anti-hypertensive effects of exercise: integrating acute and chronic mechanisms. Sports Med 2006; 36: 109–116.
Atkinson G, Cable NT, George K . The relationship between baseline blood pressure and magnitude of postexercise hypotension. J Hypertens 2005; 23: 1271–1272.
Taylor CE, Jones H, Zaregarizi M, Cable NT, George KP, Atkinson G . Blood pressure status and post-exercise hypotension: an example of a spurious correlation in hypertension research? J Hum Hypertens 2010; 24: 585–592.
Nobrega AC . The subacute effects of exercise: concept, characteristics, and clinical implications. Exerc Sport Sci Rev 2005; 33: 84–87.
MacDonald JR, MacDougall JD, Interisano SA, Smith KM, McCartney N, Moroz JS et al. Hypotension following mild bouts of resistance exercise and submaximal dynamic exercise. Eur J Appl Physiol Occup Physiol 1999; 79: 148–154.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL et al. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA 2003; 289: 2560–2572.
Pickering TG, Hall JE, Appel LJ, Falkner BE, Graves J, Hill MN et al. Recommendations for blood pressure measurement in humans and experimental animals: part 1: blood pressure measurement in humans: a statement for professionals from the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research. Circulation 2005; 111: 697–716.
Josephson RA, Shefrin E, Lakatta EG, Brant LJ, Fleg JL . Can serial exercise testing improve the prediction of coronary events in asymptomatic individuals? Circulation 1990; 81: 21–24.
Pollock ML, Jackson AS . Research progress in validation of clinical methods of assessing body composition. Med Sci Sports Exerc 1984; 16: 606–615.
Armstrong LE, Whaley MH, Brubaker PH, Otto R . Health-related physical fitness testing and interpretation. In: Whaley MH, Brubaker PH, Otto RM (eds). ACSM's Guidelines for Exercise Testing and Prescription. 7th edn. Lippincott Williams & Wilkins: Philadelphia, PA, 2006, pp 62–64.
American College of Sports Medicine. American College of Sports Medicine position stand. Progression models in resistance training for healthy adults. Med Sci Sports Exerc 2009; 41: 687–708.
Topouchian JA, El Assaad MA, Orobinskaia LV, El Feghali RN, Asmar RG . Validation of two devices for self-measurement of brachial blood pressure according to the International Protocol of the European Society of Hypertension: the SEINEX SE-9400 and the Microlife BP 3AC1-1. Blood Press Monit 2005; 10: 325–331.
Halliwill JR . Mechanisms and clinical implications of post-exercise hypotension in humans. Exerc Sport Sci Rev 2001; 29: 65–70.
Okamoto T, Masuhara M, Ikuta K . Effect of low-intensity resistance training on arterial function. Eur J Appl Physiol 2010; 111: 743–748.
White WB . Heart rate and the rate-pressure product as determinants of cardiovascular risk in patients with hypertension. Am J Hypertens 1999; 12: 50S–55S.
MacDonald JR, MacDougall JD, Hogben CD . The effects of exercising muscle mass on post exercise hypotension. J Hum Hypertens 2000; 14: 317–320.
Senitko AN, Charkoudian N, Halliwill JR . Influence of endurance exercise training status and gender on postexercise hypotension. J Appl Physiol 2002; 92: 2368–2374.
Thompson PD, Crouse SF, Goodpaster B, Kelley D, Moyna N, Pescatello L . The acute versus the chronic response to exercise. Med Sci Sports Exerc 2001; 33: S438–S445.
Acknowledgements
We thank cardiologists Dr Ricardo Harada and Dr Manoel Leitão Neto for assistance. We additionally acknowledge the Salvape and the Trainer Gym, Mogi das Cruzes. This study was supported by grants from Fundação de Amparo à Pesquisa do Estado de São Paulo-FAPESP (06/59081-6) and Conselho Nacional de Pesquisa e Tecnologia-CNPq.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Moraes, M., Bacurau, R., Simões, H. et al. Effect of 12 weeks of resistance exercise on post-exercise hypotension in stage 1 hypertensive individuals. J Hum Hypertens 26, 533–539 (2012). https://doi.org/10.1038/jhh.2011.67
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2011.67
Keywords
This article is cited by
-
Can postexercise hypotension also be observed in African and Asian populations: a systematic review and meta-analysis of randomized controlled trials
Journal of Human Hypertension (2023)
-
Pathophysiology of Noncardiac Syncope in Athletes
Sports Medicine (2018)
-
Different training programs decrease blood pressure during submaximal exercise
European Journal of Applied Physiology (2017)
-
Chronic resistance training does not affect post-exercise blood pressure in normotensive older women: a randomized controlled trial
AGE (2015)
-
Exercise, the Brain, and Hypertension
Current Hypertension Reports (2015)