Abstract
Kawasaki disease (KD) is often complicated by coronary artery lesions (CALs), including aneurysms. Because of the complications associated with KD, this disorder is the leading cause of acquired heart disease in children from developed countries. To identify genetic loci that confer a higher risk of developing CALs, we performed a case–control association study using previous genome-wide association study data for samples from KD cases only (n=186) by grouping KD patients without CALs (control: n=123) vs KD patients with extremely large aneurysms (diameter>5 mm) (case: n=17). Twelve loci with one or more sequence variants were found to be significantly associated with CALs (P<1 × 10−5). Of these, an SNP (rs17136627) in the potassium intermediate/small conductance calcium-activated channel, subfamily N, member 2 (KCNN2) at 5q22.3 was validated in 32 KD patients with large aneurysms (diameter>5 mm) and 191 KD patients without CALs (odds ratio (OR)=12.6, Pcombined=1.96 × 10−8). This result indicates that the KCNN2 gene can have an important role in the development of coronary artery aneurysms in KD.
Similar content being viewed by others
Introduction
Kawasaki disease (KD) is an acute, self-limited vasculitis that occurs predominantly in infants and young children.1 KD is often complicated by coronary artery lesions (CALs), with ∼15–25% of untreated children found to develop coronary artery aneurysms (CAAs),2 making this disease the leading cause of acquired heart disease among children in developed countries. Although treatment with high-dose intravenous immunoglobulin plus aspirin markedly reduces the incidence of CAAs, 3–5% of children with KD develop CAAs and 1% develop giant aneurysms.3, 4 According to a longitudinal study conducted over 10–21 years in Japanese children with CAAs, of the patients with giant aneurysms, roughly half developed stenosis or complete obstruction, which resulted in myocardial infarction in two-thirds of the patients.2 Hence, much effort has been directed towards decreasing the development of CAAs in KD patients.
Previously, we reported from a genome-wide association study (GWAS) of 186 KD children and 600 controls that SNPs in the DAB1 gene at chromosome 1p31 and PELI1 gene at chromosome 2p13.3 conferred a higher risk for KD or CALs.5 To identify additional risk loci for CAL formation, we have here reanalyzed our previous GWAS data for 186 children with KD only by categorizing a case–control group of KD patients without CALs (control group) vs KD patients with relatively large aneurysms (diameter>5 mm; case group).
Materials and methods
Subjects
Children with KD were recruited from 10 tertiary academic hospitals in Korea that participated in the Korean Kawasaki Disease Genetics Consortium. All KD patients were diagnosed by pediatricians according to the diagnostic criteria of the American Heart Association.6 Two-dimensional echocardiography results were interpreted by pediatric cardiologists, and coronary arteries were categorized as normal or abnormal (that is, showing dilation or aneurysm). The largest internal lumen diameter of coronary arteries was recorded, and aneurysms were classified as small (<5 mm internal diameter), medium (5–8 mm internal diameter) or giant (>8 mm internal diameter) according to the American Heart Association statement.6, 7
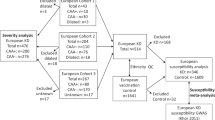
The samples used for the GWAS of CALs were obtained from our previous GWA study of KD.5 The study included 186 children with KD. According to the above criteria, 123 children had no CALs, 46 had small aneurysms, 12 had medium aneurysms and 5 had giant aneurysms. Among them, we selected children without CALs as controls, and children with medium or giant aneurysms (n=17) showing more severe phenotypes as cases instead of selecting all children with CALs including small aneurysms. A replication study was performed on 191 KD patients without CALs and 32 KD patients with medium or giant aneurysms. Our study protocol was approved by the Institutional Review Board of the involved institutions, and written informed consent was obtained from the parents of all KD patients.
Genotyping
Genotyping methods and quality control steps for GWAS have been described in detail previously.5 Briefly, a total of 222 children with KD were genotyped using the Affymetrix Genome-Wide Human SNP array 6.0 (Affymetrix, Santa Clara, CA, USA). Samples with genotyping call rates of <97% were excluded (n=35). The sex of all study samples matched the recorded status of the patients. One pair of samples was identical based on an identity-by-state analysis. A total of 186 KD samples were available in subsequent analyses. To filter the SNP markers, we also excluded 62 645 SNP markers with missing call rates greater than 5%, 2510 markers with a Hardy−Weinberg equilibrium (P-value<0.0001), and 212 830 markers with a minor allele frequency (MAF)<0.01. After filtering, 652 397 SNPs were included in the GWAS analysis. Genotyping for the replication study was completed using the Sanger sequencing method (Applied Biosystems, Foster City, CA, USA) because the TaqMan probes failed to work.
Genotype imputation
Imputation was conducted for SNPs within the linkage disequilibrium (LD) block, which the most significant rs17136627 SNP belonged to using IMPUTE2 software based on the Asian (JPT, CHB, CHS) reference panels from the 1000 Genomes Project (February 2012 release).8, 9 Imputation quality was determined as the posterior probability for the best guessed genotypes and the info score. Markers info score⩾0.4 were included in the analysis and imputed genotypes with a posterior probability<0.9 were set to missing. The imputed data were used in association analysis. The functional motifs of the associated SNPs were investigated using HaploReg program (http://www.broadinstitute.org/mammals/haploreg/haploreg.php).
Exon resequencing of the KCNN2 gene
To identify causative variants, we resequenced the KCNN2 gene in 24 KD patients with CALs and 24 KD patients without CALs. Genomic regions for sequencing analysis were obtained from the GenBank database (http://www.ncbi.nlm.nih.gov/). PCR primers that amplified the coding regions and promoter regions (500 bp upstream from exon 1) of the gene were designed using Primer3 software (http://frodo.wi.mit.edu/primer3/).10 Each fragment amplified by PCR was sequenced with an ABI Prism 3730 sequencer (Applied Biosystems). DNA polymorphisms were identified using the PolyPhred program (http://droog.gs.washington.edu/polyphred/).11
Statistical analysis
Statistical analyses were performed using the PLINK (version 1.07) (http://pngu.mgh.harvard.edu/~purcell/plink/).12 To examine possible population stratification, P-value distribution was examined in Q–Q plot and genomic inflation factor was calculated. To test the association with CALs, we used a χ2-test to compare allele frequencies between the cases and the controls.
Results
Genome-wide association analysis and replication study of CALs in KD patients
To investigate the genetic loci that affect the development of CALs in KD, we first stratified our KD samples by the size of the CALs, that is, as small (<5 mm), medium (5−8 mm) or giant (>8 mm), according to the American Heart Association statement.6, 7 Next, we performed GWA analysis in 123 KD patients without CALs and 17 KD patients with medium or giant aneurysms that showed more extreme phenotypes (internal lumen diameter of coronary arteries>5 mm) (Table 1). Genomic control method showed no inflation of P-values (λ=1.078; Supplementary Figure 1). The initial genome-wide test results for CAL susceptibility are shown in Supplementary Figure 2. A total of 22 SNPs at 12 loci passed our arbitrary threshold (P<1 × 10−5; Supplementary Table 1). For validation, we selected 12 representative SNPs from among these 22 significant SNPs. To narrow down the number of candidate polymorphisms, we validated these SNPs by sequencing in 32 KD patients with medium or giant aneurysms and 191 KD patients without CALs. Only one SNP (rs17136627) located in the intron of the potassium intermediate/small conductance calcium-activated channel, subfamily N, member 2 (KCNN2) gene showed a significant association with CAL susceptibility (P=0.001144; Table 2). The combined P-value from joint analysis of GWAS and replication samples was 1.96 × 10−8 (OR=12.6, 95% confidence interval=4.03–38.5) and exceeded the threshold for genome-wide significance (P<5.0 × 10−8; Table 2 and Figure 1). Very interestingly, the risk genotype (AG or AA) of the significantly associated SNP rs17136627 in the KCNN2 gene was found to be enriched in the KD patients with large aneurysms, including both medium and giant aneurysms (Figure 2).
Association plot for the KCNN2 gene region. Shown are a regional association plot, recombination rate and linkage disequilibrium (LD) for the KCNN2 region on chromosome 5q22.3, with gene annotations superimposed. Each SNP is plotted with respect to its chromosomal position (x axis) and its –log10 P-values (left, y axis) for the allelic test from the primary GWAS scan (red diamonds). The significance level of the replicated SNP rs17136627 in the combined analysis is also shown (large blue diamond). The estimated recombination rates (right y axis) based on the combined JPT and CHB samples from the HapMap Project are plotted in light blue. The color of each SNP symbol represents its LD (using the r2 algorithm) with the top SNP (large red diamond) within the association locus. The image above was generated using the SNAP program (http://www.broadinstitute.org/mpg/snap/ldplot.php).
The distribution of the risk genotype frequency of rs17136627 in the KCNN2 gene according to the size of the CALs. The genotypes of rs17136627 are shown on the top of the figure by CAL size. Non-CAL, normal; small, <5 mm internal diameter; medium, 5–8 mm internal diameter; giant, ⩾8 mm internal diameter.
Fine mapping and exon resequencing of the KCNN2 gene
For fine mapping, we constructed the LD map using the HapMap JPT and CHB group data in the most significant SNP (rs17136627) region and searched for genes within 100 kb of the significant marker SNP (Supplementary Figure 3). We found that the LD block contained only KCNN2 gene. Furthermore, KCNN2 gene was separated into two independent LD blocks. To further examine the LD block significantly associated with CALs, we imputed the genotypes of the SNPs within the LD block, which the most significant rs17136627 SNP belonged to using imputation method based on the Asian (JPT, CHB, CHS) reference panels from the 1000 Genomes Project and performed an association analysis. A total of 133 SNPs, including 15 genotyped SNPs were generated in 44 kb genomic region. Among them, 17 SNPs were significantly associated with CALs at P<0.05 (Supplementary Table 2). However, all imputed genotypes showed much less significance than rs17136627. In addition, although all the 17 SNPs were located in the non-coding region of the KCNN2 gene, 12 SNPs contained functional motifs including rs17136627 (Supplementary Table 2). These data suggest that those SNP sites may have a role for the expression and/or regulation of the KCNN2 gene.
To identify causative genetic variants, we resequenced promoter and exonic regions of the KCNN2 gene in 24 KD patients with CALs (diameter⩾5 mm) and 24 KD patients without CALs, focusing on functionally important regulatory SNPs, nonsynonymous SNPs (nsSNPs) and intronic SNPs in splice junction sites. Three nsSNPs (including two novel SNPs) and one repeat variant were identified in the coding regions of the KCNN2 gene and these SNPs were genotyped in 363 KD patients by sequencing (Table 3). The three nsSNPs were found to be extremely rare variants in KD patient samples and were detected in two, three and one KD patient without CAL from 363 KD samples for the R12W, I540T and S569F polymorphisms, respectively, whereas the GCC-repeat variant encoding four or five repeats of amino acid alanine (rs34838882) was relatively common in the KD patient samples (MAF=0.092). In association analysis, the GCC-repeat variant (encoding four repeats of alanine residue) located in different LD block was significantly associated with the development of CALs (OR=2.52; 95% confidence interval=1.36–4.66; P=0.0025) even though the significance of association was much lower than that of rs17136627 (Table 3 and Supplementary Figure 3).
Discussion
KD is a relatively rare disease, with an incidence in Korea of 113.1 per 100 000 children <5 years-old the second highest rate in the world.13 Coronary aneurysms develop in 15–25% of untreated children with KD, making this condition the leading cause of acquired childhood heart disease in developed countries. The cause of KD remains unknown and much effort has therefore been directed towards decreasing the development of CAAs in KD patients. We analyzed GWAS data of 123 KD patients without CALs and 17 KD patients with CALs in our current analyses to identify risk loci for CAL formation. We identified one CAL-associated locus, the rs17136627 SNP in the potassium intermediate/small conductance calcium-activated channel, subfamily N, member 2 (KCNN2) gene on chromosome 5q22.3.
In our previous GWAS study,5 we performed case–control association analysis for KD susceptibility and CAL formation using KD patients and general population samples as a control. In this design setting, we could not rule out the inclusion of genetic susceptibility variants in the control samples, especially if these samples were not exposed to common pathogenic agents. In our current study, to identify CAL-associated loci, we reanalyzed our previous GWAS data using only KD patient sample data for the KD subphenotype (CAL formation). Furthermore, we selected patients with medium or giant aneurysms showing more severe phenotypes for analysis instead of selecting all patients with CALs that had a small aneurysm (diameter<5 mm). This made our sample size smaller, but it provided great statistical power for detecting CAL risk loci that have a large effect. Thus, we could identify an SNP with a genome-wide significant P-value (OR=12.6; Pcombined=1.96 × 10−8) using a smaller sample size (49 cases and 314 controls in the joint analysis). In contrast, our previous GWAS study for CAL formation identified one SNP by using a much large sample size (149 cases and 1200 controls in the joint analysis) with less significance (OR=2.90; Pcombined=1.46 × 10−6). These results indicate that grouping of case–controls with an extreme subphenotype in patients is powerful method for detecting genes with a very strong effect. The associated SNP (rs17136627) in the KCNN2 gene was found to be associated with a 12.6-fold increased risk for CAL formation in KD patients with severe coronary aneurysms (diameter⩾5 mm).
The KCNN2 gene is a member of the KCNN family of potassium channel genes. Calcium-activated potassium channels (KCa channels) respond to changes in intracellular calcium concentration, and couple calcium metabolism to potassium flux and membrane excitability. Based on their electrophysiological properties, KCa channels are classified as large conductance, calcium- and voltage-gated channels (BK), intermediate conductance, voltage-independent channels (IK) and small conductance, voltage-independent channels (SK). SK channels are encoded by three genes, KCNN1 (SK1), KCNN2 (SK2) and KCNN3 (SK3).14 SK channels have been extensively studied in the central and peripheral nervous system, but according to recent reports are highly expressed and have important functional roles in atrial myocytes.15, 18 In particular, genetic ablation of KCNN2 channels in a mouse model results in atrial action potential prolongation and atrial arrhythmias.18 The overexpression of KCNN2 channels in transgenic mouse models results in the shortening of the spontaneous action potentials of the atrioventricular node cells and an increase in the firing frequency.19 These previous results indicate that the KCNN2 gene is highly expressed in atrial myocytes and associated with heart disease such as arrhythmias. However, although we found KCNN2 gene as susceptibility gene for CAA in Kawasaki disease, the biological role of KCNN2 gene in the formation of CAL in KD patients remains to be elucidated in the future.
To further examine the LD block significantly associated with CALs, we imputed the genotypes of the SNPs within the 44-kb genomic LD block, which the most significant rs17136627 SNP belonged to using imputation method based on the Asian (JPT, CHB, CHS) reference panels from the 1000 Genomes Project and performed an association analysis. We found that 17 SNPs, all located in the non-coding region, were significantly associated with CALs at P<0.05 (Supplementary Table 2). However, all imputed genotypes showed much less significance (P-value ranges: 0.008019–0.0001347) than rs17136627. Among 17 SNPs, 12 SNPs contained functional motifs including rs17136627 (Supplementary Table 2), suggesting that those SNP sites may have a role for the expression and/or regulation of the KCNN2 gene.
To identify causal variant(s) in the KCNN2 gene, we resequenced its promoter and exonic regions in 48 KD patient samples. We thereby identified three nonsynonymous SNPs (including two novel SNPs) and one repeat variant encoding four or five repeats of the amino acid alanine in the KCNN2 coding regions. However, when we genotyped these SNPs in all KD patients, the MAFs of three nonsynonymous SNPs were found to be extremely rare (MAF=0.001−0.003) and a genetic association test was therefore not possible. Furthermore, the rare nonsynonymous SNPs were detected only in the KD patients without CALs (Table 3), indicating that they are not likely to be involved in CAL formation in these cases. However, the common coding variant (rs34838882), a GCC-repeat variant encoding alanine, showed significant association with CALs (OR=2.52; P=0.0025), although this P-value is less significant in comparison with the SNP rs17136627 identified by GWAS. Furthermore, the GCC-repeat variant was located in the different block from the block which rs17136627 SNP belongs to. Therefore, the role of GCC repeat in the KCNN2 gene for the development of CAL formation is still not sure. Further studies, for example, resequencing of the KCNN2 gene and validation of association using a larger KD patient cohort will be necessary to identify functional variants that influence CAL formation in KD patients.
In summary, we have here identified KCNN2 as a new risk locus for coronary aneurysms in KD. This result may provide new insight into the pathophysiology of the development of CALs in this disease. Further studies are required to determine the relationship between this locus and the functional consequences that lead to CAL formation.
References
Burns, J. C. & Glodé, M. P. Kawasaki syndrome. Lancet 364, 533–554 (2004).
Kato, H., Sugimura, T., Akagi, T., Sato, N., Hashino, K., Maeno, Y. et al. Long-term consequences of Kawasaki disease. A 10- to 21-year follow-up study of 594 patients. Circulation 94, 1379–1385 (1996).
Newburger, J. W., Takahashi, M., Burns, J. C., Beiser, A. S., Chung, K. J., Duffy, C. E. et al. The treatment of Kawasaki syndrome with intravenous gamma globulin. N. Engl. J. Med. 315, 341–347 (1986).
Durongpisitkul, K., Gururaj, V. J., Park, J. M. & Martin, C. F. The prevention of coronary artery aneurysm in Kawasaki disease: a meta-analysis on the efficacy of aspirin and immunoglobulin treatment. Pediatrics 96, 1057–1061 (1995).
Kim, J. J., Hong, Y. M., Sohn, S., Jang, G. Y., Ha, K. S., Yun, S. W. et al. A genome-wide association analysis reveals 1p31 and 2p13.3 as susceptibility loci for Kawasaki disease. Hum. Genet. 129, 487–495 (2011).
Newburger, J. W., Takahashi, M., Gerber, M. A., Gewitz, M. H., Tani, L. Y., Burns, J. C. et al. Diagnosis, treatment, and long-term management of Kawasaki disease: a statement for health professionals from the Committee on Rheumatic Fever, Endocarditis and Kawasaki Disease, Council on Cardiovascular Disease in the Young, American Heart Association. Circulation 110, 2747–2771 (2004).
Dajani, A. S., Taubert, K. A., Takahashi, M., Bierman, F. Z., Freed, M. D., Ferrieri, P. et al. Guidelines for long-term management of patients with Kawasaki disease. Report from the Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease, Council on Cardiovascular Disease in the Young, American Heart Association. Circulation 89, 916–922 (1994).
Howie, B. N., Donnelly, P. & Marchini, J. A flexible and accurate genotype imputation method for the next generation of genome-wide association studies. PLoS Genet. 5, e1000529 (2009).
Howie, B., Marchini, J. & Stephens, M. Genotype imputation with thousands of genomes. G3. 1, 457–470 (2011).
Rozen, S. & Skaletsky, H. Primer3 on the WWW for general users and for biologist programmers. Methods Mol. Biol. 132, 365–386 (2000).
Nickerson, D. A., Tobe, V. O. & Taylor, S. L. PolyPhred: automating the detection and genotyping of single nucleotide substitutions using fluorescence-based resequencing. Nucleic Acids Res. 25, 2745–2751 (1997).
Purcell, S., Neale, B., Todd-Brown, K., Thomas, L., Ferreira, M. A., Bender, D. et al. PLINK: a tool set for whole-genome association and population-based linkage analyses. Am. J. Hum. Genet. 81, 559–575 (2007).
Park, Y. W., Han, J. W., Hong, Y. M., Ma, J. S., Cha, S. H., Kwon, T. C. et al. Epidemiological features of Kawasaki disease in Korea, 2006-2008. Pediatr. Int. 53, 36–39 (2010).
Köhler, M., Hirschberg, B., Bond, C. T., Kinzie, J. M., Marrion, N. V., Maylie, J. et al. Small-conductance, calcium-activated potassium channels from mammalian brain. Science 273, 1709–1714 (1996).
Xu, Y., Tuteja, D., Zhang, Z., Xu, D., Zhang, Y., Rodriguez, J. et al. Molecular identification and functional roles of a Ca2+-activated K+ channel in human and mouse hearts. J. Biol. Chem. 278, 49085–49094 (2003).
Tuteja, D., Xu, D., Timofeyev, V., Lu, L., Sharma, D., Zhang, Z. et al. Differential expression of small-conductance Ca2+-activated K+ channels SK1, SK2, and SK3 in mouse atrial and ventricular myocytes. Am. J. Physiol. Heart Circ. Physiol. 289, H2714–H2723 (2005).
Lu, L., Zhang, Q., Timofeyev, V., Zhang, Z., Young, J. N., Shin, H. S. et al. Molecular coupling of a Ca2+-activated K+ channel to L-type Ca2+ channels via alpha-actinin2. Circ. Res. 100, 112–120 (2007).
Li, N., Timofeyev, V., Tuteja, D., Xu, D., Lu, L., Zhang, Q. et al. Ablation of a Ca2+-activated K+ channel (SK2 channel) results in action potential prolongation in atrial myocytes and atrial fibrillation. J. Physiol. 587, 1087–1100 (2009).
Zhang, Q., Timofeyev, V., Lu, L., Li, N., Singapuri, A., Long, M. K. et al. Functional roles of a Ca2+-activated K+ channel in atrioventricular nodes. Circ. Res. 102, 465–471 (2008).
Acknowledgements
We thank each of the patients analyzed and their families for agreeing to participate in this study. This work was supported by a grant from the Korean Health Technology R&D Project, Ministry of Health and Welfare, Republic of Korea (A111517) and a grant (No. 2012-419) from the Asan Institute for Life Sciences, Seoul, Korea.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Supplementary Information accompanies the paper on Journal of Human Genetics website
Supplementary information
Appendix
Appendix
Korean Kawasaki Disease Genetics Consortium: In-Sook Park, Jeong-Jin Yoo, Soo-Jong Hong, Kwi-Joo Kim (Department of Pediatrics, Asan Medical Center, Seoul, Korea); Jong-Keuk Lee, Jae-Jung Kim, Young-Mi Park (Asan Institute for Life Sciences, University of Ulsan College of Medicine, Seoul, Korea); Young Mi Hong, Saejung Sohn (Department of Pediatrics, Ewha Womans University Hospital, Seoul, Korea); Gi Young Jang, Kee-Soo Ha, Hyo-Kyoung Nam, Jung-Hye Byeon (Department of Pediatrics, Korea University Hospital, Seoul, Korea); Sin Weon Yun (Department of Pediatrics, Chung-Ang University Hospital, Seoul, Korea); Myung Ki Han (Department of Pediatrics, University of Ulsan, Gangneung Asan Hospital, Gangneung, Korea); Kyung-Yil Lee, Ja-Young Hwang, Jung-Woo Rhim (Department of Pediatrics, The Catholic University of Korea, Daejeon St. Mary’s Hospital, Daejeon, Korea); Min Seob Song (Department of Pediatrics, Inje University Paik Hospital, Busan, Korea); Hyoung Doo Lee (Department of Pediatrics, Pusan National University Hospital, Busan, Korea); Dong Soo Kim (Department of Pediatrics, Yonsei University College of Medicine, Severance Children’s Hospital, Seoul, Korea); Jae-Moo Lee (Seoul Clinical Laboratories, Seoul, Korea).
Rights and permissions
About this article
Cite this article
Kim, JJ., Park, YM., Yoon, D. et al. Identification of KCNN2 as a susceptibility locus for coronary artery aneurysms in Kawasaki disease using genome-wide association analysis. J Hum Genet 58, 521–525 (2013). https://doi.org/10.1038/jhg.2013.43
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2013.43
Keywords
This article is cited by
-
Multisystem inflammatory syndrome in children and Kawasaki disease: a critical comparison
Nature Reviews Rheumatology (2021)
-
Identification of novel locus associated with coronary artery aneurysms and validation of loci for susceptibility to Kawasaki disease
European Journal of Human Genetics (2021)
-
Immunogenetics of Kawasaki disease
Clinical Reviews in Allergy & Immunology (2020)
-
Cardioprotective mechanisms of salvianic acid A sodium in rats with myocardial infarction based on proteome and transcriptome analysis
Acta Pharmacologica Sinica (2019)
-
Identification of the TIFAB Gene as a Susceptibility Locus for Coronary Artery Aneurysm in Patients with Kawasaki Disease
Pediatric Cardiology (2019)