Abstract
Background:
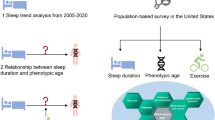
Sleep plays a vital role in maintaining homeostasis and promoting health. Previous studies show that shorter sleep duration is associated with elevated body mass index (BMI) and other cardiovascular risk factors. The goal of this study was to investigate the effects of habitual sleep duration and nightly sleep duration variation based on daily device-recorded data on BMI and obesity-related biomarkers.
Methods:
In all, 748 individuals (50.6% females, 85.4% European-Americans, average age: 49.7 years old) participated in a commercial lifestyle coaching program beginning in July 2015. Daily sleep data were recorded by Fitbit Charge HR wristbands. Clinical laboratory blood tests were measured up to three times over a 12-month period. Linear regression models were used for cross-sectional analyses, and generalized estimating equations for longitudinal analyses. All models were adjusted for age, sex, geographic location, season, genetic ancestry inferred from whole genome sequencing data, and BMI (if applicable). Multiple testing issues were corrected by false discovery rate.
Results:
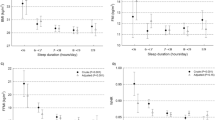
We calculated habitual sleep duration and nightly sleep duration variation. In general, females slept 15-min longer on average than males. A negative correlation was found between habitual sleep duration and BMI (β=−1.12, standard error=0.25, P<0.001). Moreover, we identified a positive correlation between sleep duration variation and BMI (β=2.97, standard error=0.79, P<0.001) while controlling for sleep duration, indicating that larger sleep duration variation is significantly and independently associated with increased BMI.
Conclusions:
We explored the impact of habitual sleep duration and sleep duration variation, and identified that shorter habitual sleep duration and larger duration variation were independently associated with increased BMI.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
St-Onge M-P, Grandner MA, Brown D, Conroy MB, Jean-Louis G, Coons M et al. Sleep duration and quality: impact on lifestyle behaviors and cardiometabolic health: a scientific statement from the American Heart Association. Circulation 2016; 134: e367–e386.
Ferranti R, Marventano S, Castellano S, Giogianni G, Nolfo F, Rametta S et al. Sleep quality and duration is related with diet and obesity in young adolescent living in Sicily, Southern Italy. Sleep Sci 2016; 9: 117–122.
Hirshkowitz M, Whiton K, M Albert S, Alessi C, Bruni O, DonCarlos L et al. National Sleep Foundation’s updated sleep duration recommendations: final report. SLEH 2015; 1: 233–243.
Moraes W, Poyares D, Zalcman I, de Mello MT, Bittencourt LR, Santos-Silva R et al. Association between body mass index and sleep duration assessed by objective methods in a representative sample of the adult population. Sleep Med 2013; 14: 312–318.
Silva AAD, Mello RGB de, Schaan CW, Fuchs FD, Redline S, Fuchs SC . Sleep duration and mortality in the elderly: a systematic review with meta-analysis. BMJ Open 2016; 6: e008119.
Tatone-tokuda F, Dubois L, Ramsay T, Girard M, Touchette E, Petit D et al. Sex differences in the association between sleep duration, diet and body mass index: a birth cohort study. J Sleep Res 2011; 21: 448–460.
Jean-Louis G, Williams NJ, Sarpong D, Pandey A, Youngstedt S, Zizi F et al. Associations between inadequate sleep and obesity in the US adult population: analysis of the national health interview survey (1977-2009). BMC Public Health 2014; 14: 290.
Zizi F, Pandey A, Murrray-Bachmann R, Vincent M, McFarlane S, Ogedegbe G et al. Race/ethnicity, sleep duration, and diabetes mellitus: analysis of the National Health Interview Survey. Am J Med 2012; 125: 162–167.
Bin YS, Marshall NS, Glozier N . Sleeping at the limits: the changing prevalence of short and long sleep durations in 10 countries. Am J Epidemiol 2013; 177: 826–833.
Prather AA, Vogelzangs N . Penninx BWJH. Sleep duration, insomnia, and markers of systemic inflammation: results from the Netherlands Study of Depression and Anxiety (NESDA). J Psychiatr Res 2015; 60: 95–102.
Lawman HG, D Fryar C, Gu Q, Ogden CL . The role of prescription medications in the association of self-reported sleep duration and obesity in US adults, 2007-2012. Obesity 2016; 24: 2210–2216.
Guo X, Zheng L, Wang J, Zhang X, Zhang X, Li J et al. Epidemiological evidence for the link between sleep duration and high blood pressure: a systematic review and meta-analysis. Sleep Med 2013; 14: 324–332.
Ohkuma T, Fujii H, Iwase M, Ogata-Kaizu S, Ide H, Kikuchi Y et al. U-shaped association of sleep duration with metabolic syndrome and insulin resistance in patients with type 2 diabetes: the Fukuoka Diabetes Registry. Metab Clin Exp 2014; 63: 484–491.
Kurina LM, McClintock MK, Chen J-H, Waite LJ, Thisted RA, Lauderdale DS . Sleep duration and all-cause mortality: a critical review of measurement and associations. Ann Epidemiol 2013; 23: 361–370.
Cappuccio FP, Taggart FM, Kandala N-B, Currie A, Peile E, Stranges S et al. Meta-analysis of short sleep duration and obesity in children and adults. Sleep 2008; 31: 619–626.
Lemola S, Ledermann T, Friedman EM . Variability of sleep duration is related to subjective sleep quality and subjective well-being: an actigraphy study. PLoS One 2013; 8: e71292.
Haus EL, Smolensky MH . Shift work and cancer risk: potential mechanistic roles of circadian disruption, light at night, and sleep deprivation. Sleep Med Rev 2013; 17: 273–284.
Poirier A, Corkum P . Night-to-night variability of sleep in children with ADHD and typically developing controls. J Atten Disord 2015; e-pub ahead of print 18 March 2015; pii: 1087054715575065.
Suh S, Nowakowski S, Bernert RA, Ong JC, Siebern AT, Dowdle CL et al. Clinical significance of night-to-night sleep variability in insomnia. Sleep Med 2012; 13: 469–475.
de Zambotti M, Baker FC, Willoughby AR, Godino JG, Wing D, Patrick K et al. Measures of sleep and cardiac functioning during sleep using a multi-sensory commercially-available wristband in adolescents. Physiol Behav 2016; 158: 143–149.
Benjamini Y, Hochberg Y . Controlling the false discovery rate: a practical and powerful approach to multiple testing. J r stat soc Ser B 1995; 57: 289–300.
Conomos MP, Miller MB, Thornton TA . Robust inference of population structure for ancestry prediction and correction of stratification in the presence of relatedness. Genet Epidemiol 2015; 39: 276–293.
Hanley JA, Negassa A, Edwardes MDD, Forrester JE . Statistical analysis of correlated data using generalized estimating equations: an orientation. Am J Epidemiol 2003; 157: 364–375.
Yetish G, Kaplan H, Gurven M, Wood B, Pontzer H, Manger PR et al. Natural sleep and its seasonal variations in three pre-industrial societies. Curr Biol 2015; 25: 2862–2868.
Allebrandt KV, Teder-Laving M, Kantermann T, Peters A, Campbell H, Rudan I et al. Chronotype and sleep duration: the influence of season of assessment. Chronobiol Int 2014; 31: 731–740.
Lo JC, Leong RLF, Loh K-K, Dijk D-J, Chee MWL . Young adults’ sleep duration on work days: differences between east and west. Front Neurol 2014; 5: 81.
Buysse DJ, Cheng Y, Germain A, Moul DE, Franzen PL, Fletcher M et al. Night-to-night sleep variability in older adults with and without chronic insomnia. Sleep Med 2010; 11: 56–64.
Kim M, Sasai H, Kojima N, Kim H . Objectively measured night-to-night sleep variations are associated with body composition in very elderly women. J Sleep Res 2015; 24: 639–647.
Case MA, Burwick HA, Volpp KG, Patel MS . Accuracy of smartphone applications and wearable devices for tracking physical activity data. JAMA 2015; 313: 625–626.
Greer SM, Goldstein AN, Walker MP . The impact of sleep deprivation on food desire in the human brain. Nat Commun 2013; 4: 2259.
St-Onge M-P . The role of sleep duration in the regulation of energy balance: effects on energy intakes and expenditure. J Clin Sleep Med 2013; 9: 73–80.
Kjeldsen JS, Hjorth MF, Andersen R, Michaelsen KF, Tetens I, Astrup A et al. Short sleep duration and large variability in sleep duration are independently associated with dietary risk factors for obesity in Danish school children. Int J Obes 2013; 38: 32–39.
He F, Bixler EO, Liao J, Berg A, Imamura Kawasawa Y, Fernandez-Mendoza J et al. Habitual sleep variability, mediated by nutrition intake, is associated with abdominal obesity in adolescents. Sleep Med 2015; 16: 1489–1494.
García-García F, Juárez-Aguilar E, Santiago-García J, Cardinali DP . Ghrelin and its interactions with growth hormone, leptin and orexins: implications for the sleep-wake cycle and metabolism. Sleep Med Rev 2014; 18: 89–97.
Cappuccio FP, D'Elia L, Strazzullo P, Miller MA . Quantity and quality of sleep and incidence of type 2 diabetes. Diabetes Care 2010; 33: 414–420.
Ford ES, Wheaton AG, Chapman DP, Li C, Perry GS, Croft JB . Associations between self-reported sleep duration and sleeping disorder with concentrations of fasting and 2-h glucose, insulin, and glycosylated hemoglobin among adults without diagnosed diabetes. J Diabetes 2013; 6: 338–350.
McCanlies EC, Slaven JE, Smith LM, Andrew ME, Charles LE, Burchfiel CM et al. Metabolic syndrome and sleep duration in police officers. Work 2012; 43: 133–139.
Wang Q, Xi B, Liu M, Zhang Y, Fu M . Short sleep duration is associated with hypertension risk among adults: a systematic review and meta-analysis. Hypertens Res 2012; 35: 1012–1018.
Cappuccio FP, Cooper D, D'Elia L, Strazzullo P, Miller MA . Sleep duration predicts cardiovascular outcomes: a systematic review and meta-analysis of prospective studies. Eur Heart J 2011; 32: 1484–1492.
Fatima Y, Doi SAR, Mamun AA . Sleep quality and obesity in young subjects: a meta-analysis. Obes Rev 2016; 17: 1154–1166.
Lee SWH, Ng KY, Chin WK . The impact of sleep amount and sleep quality on glycemic control in type 2 diabetes: a systematic review and meta-analysis. Sleep Med Rev 2017; 31: 91–101.
Leng Y, Cappuccio FP, Surtees PG, Luben R, Brayne C, Khaw KT . Daytime napping, sleep duration and increased 8-year risk of type 2 diabetes in a British population. Nutr Metab Cardiovasc Dis 2016; 26: 996–1003.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
All authors are employees of Arivale Inc. and have stock options in the company.
Additional information
Supplementary Information accompanies this paper on International Journal of Obesity website
Supplementary information
Rights and permissions
About this article
Cite this article
Xu, X., Conomos, M., Manor, O. et al. Habitual sleep duration and sleep duration variation are independently associated with body mass index. Int J Obes 42, 794–800 (2018). https://doi.org/10.1038/ijo.2017.223
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2017.223
This article is cited by
-
Multiomic signatures of body mass index identify heterogeneous health phenotypes and responses to a lifestyle intervention
Nature Medicine (2023)
-
Manifestations of Alzheimer’s disease genetic risk in the blood are evident in a multiomic analysis in healthy adults aged 18 to 90
Scientific Reports (2022)
-
Digital phenotyping by consumer wearables identifies sleep-associated markers of cardiovascular disease risk and biological aging
Communications Biology (2019)
-
Reply to "Precision medicine in the clouds"
Nature Biotechnology (2018)