Abstract
Background:
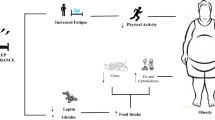
Sleep fragmentation (SF) increases food intake and the risk of obesity, and recruits macrophages to visceral white adipose tissue (VWAT) promoting tissue inflammation and insulin resistance. Administration of resveratrol (Resv) has been associated with significant improvements in high-fat diet-induced obesity, inflammation and insulin resistance.
Methods:
Male mice were subjected to SF or sleep control conditions for 8 weeks, and treated with either Resv or vehicle (Veh). Fasting plasma levels of glucose, insulin and leptin were obtained and VWAT insulin sensitivity tests were performed (phosphorylated AKT/total AKT), along with flow-cytometric assessments for VWAT macrophages (M1 and M2) and T-cell lymphocytes (CD4+, CD8+ and T regulatory cell (Treg)).
Results:
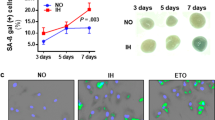
SF-Veh and SF-Resv mice showed increased food consumption and weight gain. However, although SF-Veh mice exhibited increased fasting insulin and leptin levels, and reduced VWAT p-AKT/AKT responses to insulin, such alterations were abrogated in SF-Resv-treated mice. Increases in M1, reduced M2 counts and increased tumor necrosis factor-α release emerged in SF-Veh macrophages compared with all other three groups. Similarly, increased CD8+ and reduced Treg lymphocyte counts were apparent in SF-Veh.
Conclusions:
Resveratrol does not reverse the SF-induced increases in food intake and weight gain, but markedly attenuates VWAT inflammation and insulin resistance, thereby providing a potentially useful adjunctive therapy in the context of sleep disorders manifesting metabolic morbidity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Wang Y, Carreras A, Lee SH, Hakim F, Zhang SXL, Nair D et al. Chronic fragmented sleep promotes obesity in mice. Obesity 2014; 22: 758–762.
Khalyfa A, Wang Y, Zhang SX, Qiao Z, Abdelkarim A, Gozal D . Sleep fragmentation in mice induces nicotinamide adenine dinucleotide phosphate oxidase 2-dependent mobilization, proliferation, and differentiation of adipocyte progenitors in visceral white adipose tissue. Sleep 2014; 37: 999–1009.
Zhang SX, Khalyfa A, Wang Y, Carreras A, Hakim F, Neel BA et al. Sleep fragmentation promotes NADPH oxidase 2-mediated adipose tissue inflammation leading to insulin resistance in mice. Int J Obes 2014; 38: 619–624.
Nair D, Zhang SX, Ramesh V, Hakim F, Kaushal N, Wang Y et al. Sleep fragmentation induces cognitive deficits via nicotinamide adenine dinucleotide phosphate oxidase-dependent pathways in mouse. Am J Resp Critic Care Med 2011; 184: 1305–1312.
Ramesh V, Nair D, Zhang SX, Hakim F, Kaushal N, Kayali F et al. Disrupted sleep without sleep curtailment induces sleepiness and cognitive dysfunction via the tumor necrosis factor-alpha pathway. J Neuroinflammation 2012; 9: 91.
Kaushal N, Ramesh V, Gozal D . TNF-α and temporal changes in sleep architecture in mice exposed to sleep fragmentation. PLoS One 2012; 7: e45610.
Möller-Levet CS, Archer SN, Bucca G, Laing EE, Slak A, Kabiljo R et al. Effects of insufficient sleep on circadian rhythmicity and expression amplitude of the human blood transcriptome. Proc Natl Acad Sci USA 2013; 110: E1132–E1141.
Stamatakis KA, Punjabi NM . Effects of sleep fragmentation on glucose metabolism in normal subjects. Chest 2010; 137: 95–101.
van den Berg SW, Jansen EH, Kruijshoop M, Beekhof PK, Blaak E, van der Kallen CJ et al. Paraoxonase 1 phenotype distribution and activity differs in subjects with newly diagnosed Type 2 diabetes (the CODAM Study). Diabet Med 2008; 25: 186–193.
van den Berg SW, Dollé ME, Imholz S, van der A DL, van 't Slot R, Wijmenga C et al. Genetic variations in regulatory pathways of fatty acid and glucose metabolism are associated with obesity phenotypes: a population-based cohort study. Int J Obes (Lond) 2009; 33: 1143–1152.
Hubbard BP, Sinclair DA . Small molecule SIRT1 activators for the treatment of aging and age-related diseases. Trends Pharmacol Sci. 2014; 35: 146–154.
Hausenblas HA, Schoulda JA, Smoliga JM . Resveratrol treatment as an adjunct to pharmacological management in Type 2 diabetes mellitus - systematic review and meta-analysis. Mol Nutr Food Res 2014.
Pearson KJ, Baur JA, Lewis KN, Peshkin L, Price NL, Labinskyy N et al. Resveratrol delays age-related deterioration and mimics transcriptional aspects of dietary restriction without extending life span. Cell Metab 2008; 8: 157–168.
Baur JA, Pearson KJ, Price NL, Jamieson HA, Lerin C, Kalra A et al. Resveratrol improves health and survival of mice on a high-calorie diet. Nature 2006; 444: 337–342.
Lagouge M, Argmann C, Gerhart-Hines Z, Meziane H, Lerin C, Daussin F et al. Resveratrol improves mitochondrial function and protects against metabolic disease by activating SIRT1 and PGC-1alpha. Cell 2006; 127: 1109–1122.
Ramesh V, Kaushal N, Gozal D . Sleep fragmentation differentially modifies EEG delta power during slow wave sleep in socially isolated and paired mice. Sleep Sci 2009; 2: 64–75.
Sargis RM, Neel BA, Brock CO, Lin Y, Hickey AT, Carlton DA et al. The novel endocrine disruptor tolylfluanid impairs insulin signaling in primary rodent and human adipocytes through a reduction in insulin receptor substrate-1levels. Biochim Biophys Acta 2012; 1822: 952–960.
Hakim F, Wang Y, Carreras A, Hirotsu C, Zhang J, Peris E et al. Chronic sleep disruption during the sleep period induces hypothalamic endoplasmic reticulum stress and PTP1b-mediated leptin resistance in mice. Sleep 2014 (in press).
Zhu J, Yong W, Wu X, Yu Y, Lv J, Liu C et al. Anti-inflammatory effect of resveratrol on TNF-alpha-induced MCP-1 expression in adipocytes. Biochem Biophys Res Commun. 2008; 369: 471–477.
Gonzales AM, Orlando RA . Curcumin and resveratrol inhibit nuclear factor-kappaB-mediated cytokine expression in adipocytes. Nutr Metab (Lond) 2008; 5: 17.
Olholm J, Paulsen SK, Cullberg KB, Richelsen B, Pedersen SB . Anti-inflammatory effect of resveratrol on adipokine expression and secretion in human adipose tissue explants. Int J Obes (Lond) 2010; 34: 1546–1553.
Jimenez-Gomez Y, Mattison JA, Pearson KJ, Martin-Montalvo A, Palacios HH, Sossong AM et al. Resveratrol improves adipose insulin signaling and reduces the inflammatory response in adipose tissue of rhesus monkeys on high-fat, high-sugar diet. Cell Metab 2013; 18: 533–545.
Wright DC . Exercise- and resveratrol-mediated alterations in adipose tissue metabolism. Appl Physiol Nutr Metab 2014; 39: 109–116.
Schneider Y, Duranton B, Gossé F, Schleiffer R, Seiler N, Raul F . Resveratrol inhibits intestinal tumorigenesis and modulates host-defense-related gene expression in an animal model of human familial adenomatous polyposis. Nutr Cancer 2001; 39: 102–107.
Norata GD, Marchesi P, Passamonti S, Pirillo A, Violi F, Catapano AL . Anti-inflammatory and anti-atherogenic effects of cathechin, caffeic acid and trans-resveratrol in apolipoprotein E deficient mice. Atherosclerosis 2007; 191: 265–271.
Qureshi AA, Guan XQ, Reis JC, Papasian CJ, Jabre S, Morrison DC et al. Inhibition of nitric oxide and inflammatory cytokines in LPS-stimulated murine macrophages by resveratrol, a potent proteasome inhibitor. Lipids Health Dis 2012; 11: 76.
Cho SJ, Jung UJ, Choi MS . Differential effects of low-dose resveratrol on adiposity and hepatic steatosis in diet-induced obese mice. Br J Nutr 2012; 108: 2166–2175.
Bakker GC, van Erk MJ, Pellis L, Wopereis S, Rubingh CM, Cnubben NH et al. An antiinflammatory dietary mix modulates inflammation and oxidative and metabolic stress in overweight men: a nutrigenomics approach. Am J Clin Nutr 2010; 91: 1044–1059.
Weisberg SP, McCann D, Desai M, Rosenbaum M, Leibel RL, Ferrante AW Jr . Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest 2003; 112: 1796–1808.
Di Gregorio GB, Yao-Borengasser A, Rasouli N, Varma V, Lu T, Miles LM et al. Expression of CD68 and macrophage chemoattractant protein-1 genes in human adipose and muscle tissues: association with cytokine expression, insulin resistance, and reduction by pioglitazone. Diabetes 2005; 54: 2305–2313.
Hernandez ED, Lee SJ, Kim JY, Duran A, Linares JF, Yajima T et al. A Macrophage NBR1-MEKK3 Complex Triggers JNK-Mediated Adipose Tissue Inflammation in Obesity. Cell Metab 2014; 20: 499–511.
Cipolletta D . Adipose tissue-resident regulatory T cells: phenotypic specialization, functions and therapeutic potential. Immunology 2014; 142: 517–525.
Garg SK, Delaney C, Shi H, Yung R . Changes in adipose tissue macrophages and T cells during aging. Crit Rev Immunol 2014; 34: 1–14.
Lee BC, Lee J . Cellular and molecular players in adipose tissue inflammation in the development of obesity-induced insulin resistance. Biochim Biophys Acta. 2014; 1842: 446–462.
Lal G, Bromberg JS . Epigenetic mechanisms of regulation of Foxp3 expression. Blood 2009; 114: 3727–3735.
Akasheh RT, Pang J, York JM, Fantuzzi G . New pathways to control inflammatory responses in adipose tissue. Curr Opin Pharmacol 2013; 13: 613–617.
Farghali H, Kutinová Canová N, Lekić N . Resveratrol and related compounds as antioxidants with an allosteric mechanism of action in epigenetic drug targets. Physiol Res 2013; 62: 1–13.
Qin W, Zhang K, Clarke K, Weiland T, Sauter ER . Methylation and miRNA effects of resveratrol on mammary tumors vs normal tissue. Nutr Cancer 2014; 66: 270–277.
Kim J, Bhattacharjee R, Khalyfa A, Kheirandish-Gozal L, Capdevila OS, Wang Y et al. DNA methylation in inflammatory genes among children with obstructive sleep apnea. Am J Respir Crit Care Med 2012; 185: 330–338.
Tan HL, Gozal D, Wang Y, Bandla HP, Bhattacharjee R, Kulkarni R et al. Alterations in circulating T-cell lymphocyte populations in children with obstructive sleep apnea. Sleep 2013; 36: 913–922.
Acknowledgements
This work was supported by the Herbert T. Abelson Endowed Chair in Pediatrics to DG.
Author Contributions
AC participated in the conceptual framework of the project, performed experiments, analyzed data and drafted components of the manuscript. SXZ, EP, ZQ, IA performed experiments. YW analyzed data and served as blinded observer. DG conceptualized the project, provided critical input in all phases of the experiments, analyzed data, drafted the ulterior versions of the manuscript and is responsible for the financial support of the project and the manuscript content. All authors have reviewed and approved the final version of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Carreras, A., Zhang, S., Peris, E. et al. Effect of resveratrol on visceral white adipose tissue inflammation and insulin sensitivity in a mouse model of sleep apnea. Int J Obes 39, 418–423 (2015). https://doi.org/10.1038/ijo.2014.181
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2014.181
This article is cited by
-
A long-term anti-inflammation markedly alleviated high-fat diet-induced obesity by repeated administrations of overexpressing IL10 human umbilical cord-derived mesenchymal stromal cells
Stem Cell Research & Therapy (2022)
-
Resveratrol alleviates obesity-induced skeletal muscle inflammation via decreasing M1 macrophage polarization and increasing the regulatory T cell population
Scientific Reports (2020)
-
Baroreflex Control of Heart Rate in Mice Overexpressing Human SOD1: Functional Changes in Central and Vagal Efferent Components
Neuroscience Bulletin (2019)
-
Sleep-disordered breathing, circulating exosomes, and insulin sensitivity in adipocytes
International Journal of Obesity (2018)
-
Biological plausibility linking sleep apnoea and metabolic dysfunction
Nature Reviews Endocrinology (2016)