Abstract
OBJECTIVE:
To examine the long-term relationship between changes in water and beverage intake and weight change.
SUBJECTS:
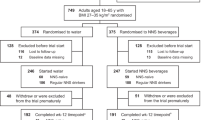
Prospective cohort studies of 50 013 women aged 40–64 years in the Nurses’ Health Study (NHS, 1986–2006), 52 987 women aged 27–44 years in the NHS II (1991–2007) and 21 988 men aged 40–64 years in the Health Professionals Follow-up Study (1986–2006) without obesity and chronic diseases at baseline.
MEASURES:
We assessed the association of weight change within each 4-year interval, with changes in beverage intakes and other lifestyle behaviors during the same period. Multivariate linear regression with robust variance and accounting for within-person repeated measures were used to evaluate the association. Results across the three cohorts were pooled by an inverse-variance-weighted meta-analysis.
RESULTS:
Participants gained an average of 1.45 kg (5th to 95th percentile: −1.87 to 5.46) within each 4-year period. After controlling for age, baseline body mass index and changes in other lifestyle behaviors (diet, smoking habits, exercise, alcohol, sleep duration, TV watching), each 1 cup per day increment of water intake was inversely associated with weight gain within each 4-year period (−0.13 kg; 95% confidence interval (CI): −0.17 to −0.08). The associations for other beverages were: sugar-sweetened beverages (SSBs) (0.36 kg; 95% CI: 0.24–0.48), fruit juice (0.22 kg; 95% CI: 0.15–0.28), coffee (−0.14 kg; 95% CI: −0.19 to −0.09), tea (−0.03 kg; 95% CI: −0.05 to −0.01), diet beverages (−0.10 kg; 95% CI: −0.14 to −0.06), low-fat milk (0.02 kg; 95% CI: −0.04 to 0.09) and whole milk (0.02 kg; 95% CI: −0.06 to 0.10). We estimated that replacement of 1 serving per day of SSBs by 1 cup per day of water was associated with 0.49 kg (95% CI: 0.32–0.65) less weight gain over each 4-year period, and the replacement estimate of fruit juices by water was 0.35 kg (95% CI: 0.23–0.46). Substitution of SSBs or fruit juices by other beverages (coffee, tea, diet beverages, low-fat and whole milk) were all significantly and inversely associated with weight gain.
CONCLUSION:
Our results suggest that increasing water intake in place of SSBs or fruit juices is associated with lower long-term weight gain.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Wolf A, Bray GA, Popkin BM . A short history of beverages and how our body treats them. Obes Rev 2008; 9: 151–164.
Nielsen SJ, Popkin BM . Changes in beverage intake between 1977 and 2001. Am J Prev Med 2004; 27: 205–210.
Bleich SN, Wang YC, Wang Y, Gortmaker SL . Increasing consumption of sugar-sweetened beverages among US adults: 1988–1994 to 1999–2004. Am J Clin Nutr 2009; 89: 372–381.
Malik VS, Schulze MB, Hu FB . Intake of sugar-sweetened beverages and weight gain: a systematic review. Am J Clin Nutr 2006; 84: 274–288.
Olsen NJ, Heitmann BL . Intake of calorically sweetened beverages and obesity. Obes Rev 2009; 10: 68–75.
Daniels MC, Popkin BM . Impact of water intake on energy intake and weight status: a systematic review. Nutr Rev 2010; 68: 505–521.
Dennis EA, Dengo AL, Comber DL, Flack KD, Savla J, Davy KP et al. Water consumption increases weight loss during a hypocaloric diet intervention in middle-aged and older adults. Obesity 2010; 18: 300–307.
Stookey JD, Constant F, Popkin BM, Gardner CD . Drinking water is associated with weight loss in overweight dieting women independent of diet and activity. Obesity 2008; 16: 2481–2488.
Lopez-Garcia E, van Dam RM, Rajpathak S, Willett WC, Manson JE, Hu FB . Changes in caffeine intake and long-term weight change in men and women. Am J Clin Nutr 2006; 83: 674–680.
Mozaffarian D, Hao T, Rimm EB, Willett WC, Hu FB . Changes in diet and lifestyle and long-term weight gain in women and men. N Engl J Med 2011; 364: 2392–2404.
Salvini S, Hunter DJ, Sampson L, Stampfer MJ, Colditz GA, Rosner B et al. Food-based validation of a dietary questionnaire: the effects of week-to-week variation in food consumption. Int J Epidemiol 1989; 18: 858–867.
Feskanich D, Rimm EB, Giovannucci EL, Colditz GA, Stampfer MJ, Litin LB et al. Reproducibility and validity of food intake measurements from a semiquantitative food frequency questionnaire. J Am Diet Assoc 1993; 93: 790–796.
Manson JE, Willett WC, Stampfer MJ, Colditz GA, Hunter DJ, Hankinson SE et al. Body weight and mortality among women. N Engl J Med 1995; 333: 677–685.
Hu FB, Stampfer MJ, Rimm E, Ascherio A, Rosner BA, Spiegelman D et al. Dietary fat and coronary heart disease: a comparison of approaches for adjusting for total energy intake and modeling repeated dietary measurements. Am J Epidemiol 1999; 149: 531–540.
Boschmann M, Steiniger J, Hille U, Tank J, Adams F, Sharma AM et al. Water-induced thermogenesis. J Clin Endocrinol Metab 2003; 88: 6015–6019.
Boschmann M, Steiniger J, Franke G, Birkenfeld AL, Luft FC, Jordan J . Water drinking induces thermogenesis through osmosensitive mechanisms. J Clin Endocrinol Metab 2007; 92: 3334–3337.
Brown CM, Dulloo AG, Montani JP . Water-induced thermogenesis reconsidered: the effects of osmolality and water temperature on energy expenditure after drinking. J Clin Endocrinol Metab 2006; 91: 3598–3602.
Davy BM, Dennis EA, Dengo AL, Wilson KL, Davy KP . Water consumption reduces energy intake at a breakfast meal in obese older adults. J Am Diet Assoc 2008; 108: 1236–1239.
Van Walleghen EL, Orr JS, Gentile CL, Davy BM . Pre-meal water consumption reduces meal energy intake in older but not younger subjects. Obesity 2007; 15: 93–99.
Rolls BJ, Kim S, Fedoroff IC . Effects of drinks sweetened with sucrose or aspartame on hunger, thirst and food intake in men. Physiol Behav 1990; 48: 19–26.
DellaValle DM, Roe LS, Rolls BJ . Does the consumption of caloric and non-caloric beverages with a meal affect energy intake? Appetite 2005; 44: 187–193.
Astrup A, Toubro S, Cannon S, Hein P, Breum L, Madsen J . Caffeine: a double-blind, placebo-controlled study of its thermogenic, metabolic, and cardiovascular effects in healthy volunteers. Am J Clin Nutr 1990; 51: 759–767.
Acheson KJ, Gremaud G, Meirim I, Montigon F, Krebs Y, Fay LB et al. Metabolic effects of caffeine in humans: lipid oxidation or futile cycling? Am J Clin Nutr 2004; 79: 40–46.
Hursel R, Viechtbauer W, Westerterp-Plantenga MS . The effects of green tea on weight loss and weight maintenance: a meta-analysis. Int J Obes 2009; 33: 956–961.
Phung OJ, Baker WL, Matthews LJ, Lanosa M, Thorne A, Coleman CI . Effect of green tea catechins with or without caffeine on anthropometric measures: a systematic review and meta-analysis. Am J Clin Nutr 2010; 91: 73–81.
Pepino MY, Bourne C . Non-nutritive sweeteners, energy balance, and glucose homeostasis. Curr Opin Clin Nutr Metab Care 2011; 14: 391–395.
Mattes RD, Shikany JM, Kaiser KA, Allison DB . Nutritively sweetened beverage consumption and body weight: a systematic review and meta-analysis of randomized experiments. Obes Rev 2011; 12: 346–365.
Rajpathak SN, Rimm EB, Rosner B, Willett WC, Hu FB . Calcium and dairy intakes in relation to long-term weight gain in US men. Am J Clin Nutr 2006; 83: 559–566.
Louie JC, Flood VM, Hector DJ, Rangan AM, Gill TP . Dairy consumption and overweight and obesity: a systematic review of prospective cohort studies. Obes Rev 2011; 12: e582–e592.
Chen M, Pan A, Malik V, Hu FB . Dairy intake and body weight: a meta-analysis of randomized controlled trials. Am J Clin Nutr 2012; 96: 735–747.
Libuda L, Alexy U, Sichert-Hellert W, Stehle P, Karaolis-Danckert N, Buyken AE et al. Pattern of beverage consumption and long-term association with body-weight status in German adolescents—results from the DONALD study. Br J Nutr 2008; 99: 1370–1379.
Chen L, Appel LJ, Loria C, Lin PH, Champagne CM, Elmer PJ et al. Reduction in consumption of sugar-sweetened beverages is associated with weight loss: the PREMIER trial. Am J Clin Nutr 2009; 89: 1299–1306.
Tordoff MG, Alleva AM . Effect of drinking soda sweetened with aspartame or high-fructose corn syrup on food intake and body weight. Am J Clin Nutr 1990; 51: 963–969.
DiMeglio DP, Mattes RD . Liquid versus solid carbohydrate: effects on food intake and body weight. Int J Obes Relat Metab Disord 2000; 24: 794–800.
Raben A, Vasilaras TH, Moller AC, Astrup A . Sucrose compared with artificial sweeteners: different effects on ad libitum food intake and body weight after 10 wk of supplementation in overweight subjects. Am J Clin Nutr 2002; 76: 721–729.
Stookey JD, Constant F, Gardner CD, Popkin BM . Replacing sweetened caloric beverages with drinking water is associated with lower energy intake. Obesity 2007; 15: 3013–3022.
Tate DF, Turner-McGrievy G, Lyons E, Stevens J, Erickson K, Polzien K et al. Replacing caloric beverages with water or diet beverages for weight loss in adults: main results of the Choose Healthy Options Consciously Everyday (CHOICE) randomized clinical trial. Am J Clin Nutr 2012; 95: 555–563.
Pan A, Malik VS, Schulze MB, Manson JE, Willett WC, Hu FB . Plain-water intake and risk of type 2 diabetes in young and middle-aged women. Am J Clin Nutr 2012; 95: 1454–1460.
Flegal KM, Carroll MD, Kit BK, Ogden CL . Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999–2010. JAMA 2012; 307: 491–497.
Acknowledgements
We are indebted to the participants in the Nurses’ Health Study, Nurses’ Health Study II and HPFS for their continuing outstanding support and colleagues working in these studies for their valuable help. The study was supported by the National Institutes of Health Grants (P01CA087969, R01CA050385, U19CA055075, R01DK058845, P30DK046200 and U54CA155626). The study sponsors were not involved in the study design and the collection, analysis and interpretation of data, nor the writing of the article or the decision to submit it for publication. The authors were independent from the study sponsors.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on International Journal of Obesity website
Supplementary information
Rights and permissions
About this article
Cite this article
Pan, A., Malik, V., Hao, T. et al. Changes in water and beverage intake and long-term weight changes: results from three prospective cohort studies. Int J Obes 37, 1378–1385 (2013). https://doi.org/10.1038/ijo.2012.225
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2012.225
Keywords
This article is cited by
-
Substitution of animal-based with plant-based foods on cardiometabolic health and all-cause mortality: a systematic review and meta-analysis of prospective studies
BMC Medicine (2023)
-
Relation of fruit juice with adiposity and diabetes depends on how fruit juice is defined: a re-analysis of the EFSA draft scientific opinion on the tolerable upper intake level for dietary sugars
European Journal of Clinical Nutrition (2023)
-
Sugar and low/no-calorie-sweetened beverage consumption and associations with body weight and waist circumference changes in five European cohort studies: the SWEET project
European Journal of Nutrition (2023)
-
Association of health behaviors, dietary habits, and oral health with weight gain after 20 years of age in community-dwelling Japanese individuals aged 40 years and older: a cross-sectional study
Clinical Oral Investigations (2023)
-
Association between dietary behaviors and depression in adolescent girls
BMC Public Health (2022)