Abstract
Objective:
To assess the association between the consumption of fast food (FF) and body mass index (BMI) of teenagers in a large UK birth cohort.
Methods:
A structural equation modelling (SEM) approach was chosen to allow direct statistical testing of a theoretical model. SEM is a combination of confirmatory factor and path analysis, which allows for the inclusion of latent (unmeasured) variables. This approach was used to build two models: the effect of FF outlet visits and food choices and the effect of FF exposure on consumption and BMI.
Results:
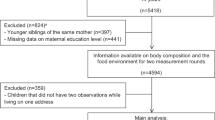
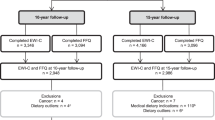
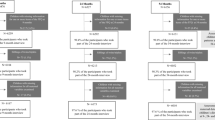
A total of 3620 participants had data for height and weight from the age 13 clinic and the frequency of FF outlet visits, and so were included in these analyses. This SEM model of food choices showed that increased frequency of eating at FF outlets is positively associated with higher consumption of unhealthy foods (β=0.29, P<0.001) and negatively associated with the consumption of healthy foods (β=−1.02, P<0.001). The SEM model of FF exposure and BMI showed that higher exposure to FF increases the frequency of visits to FF outlets (β=0.61, P<0.001), which is associated with higher body mass index standard deviation score (BMISDS; β=0.08, P<0.001). Deprivation was the largest contributing variable to the exposure (β=9.2, P<0.001).
Conclusions:
The teenagers who ate at FF restaurants consumed more unhealthy foods and were more likely to have higher BMISDS than those teenagers who did not eat frequently at FF restaurants. Teenagers who were exposed to more takeaway foods at home ate more frequently at FF restaurants and eating at FF restaurants was also associated with lower intakes of vegetables and raw fruit in this cohort.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Craig RS . Health survey for England 2007, 2008. Available from http://www.natcen.ac.uk/study/health-survey-for-england-2007.
Keynote. UK fast food and home delivery outlets, 2006.
DeMaria AN . Of fast food and franchises. J Am Coll Cardiol 2003; 41: 1227–1228.
Astrup A . Super-sized and diabetic by frequent fast-food consumption? Lancet 2005; 365: 4–5.
Brown K, McIlveen H, Strugnell C . Young consumers and the hospitality spectrum. Appetite 1998; 31: 403.
Harnack LJ, French SA, Oakes JM, Story MT, Jeffery RW, Rydell SA . Effects of calorie labeling and value size pricing on fast food meal choices: results from an experimental trial. Int J Behav Nutr Phys Act 2008; 5: 63.
Lewis LB, Sloane DC, Nascimento LM, Diamant AL, Guinyard JJ, Yancey AK et al. African Americans’ access to healthy food options in South Los Angeles restaurants. Am J Public Health 2005; 95: 668–673.
Paeratakul S, Ferdinand DP, Champagne CM, Ryan DH, Bray GA . Fast-food consumption among US adults and children: dietary and nutrient intake profile. J Am Diet Assoc 2003; 103: 1332–1338.
Schmidt M, Affenito SG, Striegel-Moore R, Khoury PR, Barton B, Crawford P et al. Fast-food intake and diet quality in black and white girls - the national heart, lung, and blood institute growth and health study. Arch Pediatr Adolesc Med 2005; 159: 626–631.
Bowman SA, Gortmaker SL, Ebbeling CB, Pereira MA, Ludwig DS . Effects of fast-food consumption on energy intake and diet quality among children in a national household survey. Pediatrics 2004; 113: 112–118.
Boutelle KN, Fulkerson JA, Neumark-Sztainer D, Story M, French SA . Fast food for family meals: relationships with parent and adolescent food intake, home food availability and weight status. Public Health Nutr 2007; 10: 16–23.
Duffey KJ, Gordon-Larsen P, Jacobs DR, Williams OD, Popkin BM . Differential associations of fast food and restaurant food consumption with 3-y change in body mass index: the Coronary Artery Risk Development in Young Adults Study. Am J Clin Nutr 2007; 85: 201–208.
Pereira MA, Kartashov AI, Ebbeling CB, Van Horn L, Slattery M, Jacobs DR et al. Fast-food habits, weight gain, and insulin resistance (the CARDIA study): 15-year prospective analysis. Lancet 2005; 365: 36–42.
Sutherland LA, MacKenzie T, Purvis LA, Dalton M . Prevalence of food and beverage brands in movies: 1996–2005. Pediatrics 2010; 125: 468–474.
Powell LM, Szczypka G, Chaloupka FJ . Trends in exposure to television food advertisements among children and adolescents in the United States. Arch Pediatr Adolesc Med 2010; 164: 794–802.
Hillier A, Cole BL, Smith TE, Yancey AK, Williams JD, Grier SA et al. Clustering of unhealthy outdoor advertisements around child-serving institutions: a comparison of three cities. Health Place 2009; 15: 935–945.
Lingas EO, Dorfman L, Bukofzer E . Nutrition content of food and beverage products on Web sites popular with children. Am J Public Health 2009; 99 (Suppl 3): S587–S592.
Robinson TN, Borzekowski DLG, Matheson DM, Kraemer HC . Effects of fast food branding on young children's taste preferences. Arch Pediatr Adolesc Med 2007; 161: 792–797.
Cummins SCJ, McKay L, MacIntyre S . McDonald's restaurants and neighborhood deprivation in Scotland and England. Am J Prev Med 2005; 29: 308–310.
Fraser LK, Edwards KL . The association between the geography of fast food outlets and childhood obesity rates in Leeds, UK. Health Place 2010; 16: 1124–1128.
Macdonald L, Cummins S, Macintyre S . Neighbourhood fast food environment and area deprivation-substitution or concentration? Appetite 2007; 49: 251–254.
Neckerman KM, Bader MDM, Richards CA, Purciel M, Quinn JW, Thomas JS et al. Disparities in the food environments of New York City public schools. A J Prev Med 2010; 39: 195–202.
Davis B, Carpenter C . Proximity of fast-food restaurants to schools and adolescent obesity. Am J Public Health 2009; 99: 505–510.
Seliske LM, Pickett W, Boyce WF, Janssen I . Density and type of food retailers surrounding Canadian schools: variations across socioeconomic status. Health Place 2009; 15: 903–907.
Stender S, Dyerberg J, Astrup A . Fast food: unfriendly and unhealthy. Int J Obes 2007; 31: 887–890.
Golding J, Pembrey M, Jones R, Team AS . ALSPAC-The Avon Longitudinal Study of Parents and Children – I. Study methodology. Paediatr Perinat Epidemiol 2001; 15: 74–87.
Cole TJ, Freeman JV, Preece MA . Body-mass index reference curves for the UK, 1990. Arch DisChild 1995; 73: 25–29.
Riddoch CJ, Leary SD, Ness AR, Blair SN, Deere K, Mattocks C et al. Prospective associations between objective measures of physical activity and fat mass in 12–14 year old children: the Avon Longitudinal Study of Parents and Children (ALSPAC). Br Med J 2009; 339: b4544.
Index of Multiple Deprivation 2007 (IMD 2007).
Kline R (ed) Principles and Practice of Structural Equation Modeling. The Guildford Press: New York, 2005.
Tomarken AJ, Waller NG . Structural equation modeling: strengths, limitations, and misconceptions. Annu Rev Clinic Psychol 2005; 1: 31–65.
Byrne BM (ed). Structural Equation Modelling with AMOS. Lawrence Erbaum Associates: London, 2001.
Astrup A, Dyerberg J, Selleck M, Stender S . Nutrition transition and its relationship to the development of obesity and related chronic diseases. Obes Rev 2008; 9: 48–52.
Taveras EM, Berkey CS, Rifas-Shiman SL, Ludwig DS, Rockett HRH, Field AE et al. Association of consumption of fried food away from home with body mass index and diet quality in older children and adolescents. Pediatrics 2005; 116: E518–E524.
Fraser LK, Edwards KL, Cade J, Clarke GP . The geography of fast food outlets: a review. Int J Environ Res Public Health 2010; 7: 2290–2308.
Powell LM . Fast food costs and adolescent body mass index: evidence from panel data. J Health Econ 2009; 28: 963–970.
Dunford E, Webster J, Barzi F, Neal B . Nutrient content of products served by leading Australian fast food chains. Appetite 2010; 55: 484–489.
Acknowledgements
We are extremely grateful to all the families who took part in this study, the midwives for their help in recruiting and the whole ALSPAC team, which include interviewers, computer and laboratory technicians, clerical workers, research scientists, volunteers, managers, receptionists and nurses. The UK Medical Research Council (grant ref: 74882), The Wellcome Trust (grant ref: 076467) and the University of Bristol provide core support for ALSPAC. LKF was funded by ESRC/MRC studentship.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Fraser, L., Edwards, K., Cade, J. et al. Fast food, other food choices and body mass index in teenagers in the United Kingdom (ALSPAC): a structural equation modelling approach. Int J Obes 35, 1325–1330 (2011). https://doi.org/10.1038/ijo.2011.120
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2011.120
Keywords
This article is cited by
-
Food Away from Home and Childhood Obesity
Current Obesity Reports (2014)
-
Modern Sedentary Behaviors Favor Energy Consumption in Children and Adolescents
Current Obesity Reports (2013)