Abstract
Objective:
This study assessed longitudinal changes in body composition, fat distribution and energy balance in perimenopausal women. We hypothesized that total fat and abdominal body fat would increase at menopause due to decreased energy expenditure (EE) and declining estrogen, respectively.
Design:
Observational, longitudinal study with annual measurements for 4 years.
Subjects:
Healthy women (103 Caucasian; 53 African-American), initially premenopausal. During follow-up, lack of menstruation for 1 year and follicle-stimulating hormone >30 mIU ml−1 defined a subject as postmenopausal.
Measurements:
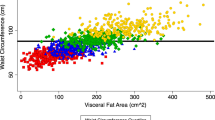
Fat and lean mass (dual-energy X-ray absorptiometry), visceral (VAT) and subcutaneous abdominal fat (SAT) (computed tomography), dietary intake (4-day food record), serum sex hormones and physical activity (tri-axial accelerometry). Twenty-four hour EE was measured by whole-room calorimeter in a subset of 34 women at baseline and at year 4.
Results:
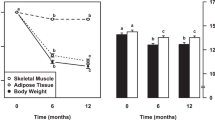
Body fat and weight increased significantly over time only in those women who became postmenopausal by year 4 (n=51). All women gained SAT over time; however, only those who became postmenopausal had a significant increase in VAT. The postmenopausal group also exhibited a significant decrease in serum estradiol. Physical activity decreased significantly 2 years before menopause and remained low. Dietary energy, protein, carbohydrate and fiber intake were significantly higher 3–4 years before the onset of menopause compared with menopause onset. Twenty-four hour EE and sleeping EE decreased significantly with age; however, the decrease in sleeping EE was 1.5-fold greater in women who became postmenopausal compared with premenopausal controls (−7.9 vs −5.3%). Fat oxidation decreased by 32% in women who became postmenopausal (P<0.05), but did not change in those who remained premenopausal.
Conclusion:
Middle-aged women gained SAT with age, whereas menopause per se was associated with an increase in total body fat and VAT. Menopause onset is associated with decreased EE and fat oxidation that can predispose to obesity if lifestyle changes are not made.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
WHO. Obesity: preventing and managing the global epidemic. Report of a WHO Consultation. WHO Technical Report Series 894 World Health Organization: Geneva, 2000.
Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, Flegal KM . Prevalence of overweight and obesity in the United States, 1999–2004. JAMA 2006; 295: 1549–1555.
Wing RR, Matthews KA, Kuller LH, Meilahn EN, Plantinga PL . Weight gain at the time of menopause. Arch Intern Med 1991; 151: 97–102.
Matthews KA, Abrams B, Crawford S, Miles T, Neer R, Powell LH et al. Body mass index in mid-life women: relative influence of menopause, hormone use, and ethnicity. Int J Obes Relat Metab Disord 2001; 25: 863–873.
Sowers M, Zheng H, Tomey K, Karvonen-Gutierrez C, Jannausch M, Li X et al. Changes in body composition in women over six years at midlife: ovarian and chronological aging. J Clin Endocrinol Metab 2007; 92: 895–901.
Espeland MA, Stefanick ML, Kritz-Silverstein D, Fineberg SW, Waclawiw MA, James MK et al. Effect of postmenopausal hormone therapy on body weight and waist and hip girths. J Clin Endocrinol Metab 1997; 82: 1549–1556.
Munoz J, Derstine A, Gower BA . Fat distribution and insulin sensitivity in postmenopausal women: influence of hormone replacement. Obes Res 2002; 10: 424–431.
Kanaley JA, Sames C, Swisher L, Swick LL, Ploutz-Snyder CM, Steppan KS et al. Abdominal fat distribution in pre- and postmenopausal women: the impact of physical activity, age and menopausal status. Metabolism 2001; 50: 976–982.
Douchi T, Yamamoto S, Yoshimitsu N, Andoh T, Matsuo T, Nagata Y . Relative contribution of aging and menopause to changes in lean and fat mass in segmental regions. Maturitas 2002; 42: 301–306.
Smith SR, Lovejoy JC, Greenway F, Ryan D, Dejonge L, De La Bretonne J et al. Contributions of total body fat, abdominal subcutaneous adipose tissue compartments, and visceral adipose tissue to the metabolic complications of obesity. Metabolism 2001; 50: 425–435.
Westerterp KR . Physical activity assessment with accelerometers. Int J Obes Relat Metab Disord 1999; 23 (Suppl 3): S45–S49.
Nguyen T, de Jonge L, Smith SR, Bray GA . Chamber for indirect calorimetry with accurate measurement and time discrimination of metabolic plateaus of over 20 min. Med Biol Eng Comput 2003; 41: 572–578.
Elia S, Livesey G . Energy expenditure and fuel selection in biological systems: the theory and practice of calculations based on indirect calorimetry and tracer methods. In: Simopoulus AP (ed). Metabolic Control of Eating, Energy Expenditure and the Bioenergetics of Obesity World Review on Nutrition and Diet. Karger: Basel, 1992, pp 68–131.
Katz A, Nambi SS, Mather K, Baron AD, Follmann DA, Sullivan G et al. Quantitative insulin sensitivity check index: a simple, accurate method for assessing insulin sensitivity in humans. J Clin Endocrinol Metab 2000; 85: 2402–2410.
Lovejoy JC, Smith SR, Rood JC . Comparison of regional fat distribution and health risk factors in middle-aged white and African American women: the Healthy Transitions Study. Obes Res 2001; 9: 10–16.
Rebuffe-Scrive M, Eldh J, Hafstrom LO, Bjorntorp P . Metabolism of mammary, abdominal, and femoral adipocytes in women before and after menopause. Metabolism 1986; 35: 792–797.
Price TM, O'Brien SN, Welter BH, George R, Anandjiwala J, Kilgore M . Estrogen regulation of adipose tissue lipoprotein lipase—possible mechanism of body fat distribution. Am J Obstet Gynecol 1998; 178: 101–107.
Elbers JM, de Jong S, Teerlink T, Asscheman H, Seidell JC, Gooren LJ . Changes in fat cell size and in vitro lipolytic activity of abdominal and gluteal adipocytes after a one-year cross-sex hormone administration in transsexuals. Metabolism 1999; 48: 1371–1377.
Lindberg UB, Crona N, Silfverstolpe G, Bjorntorp P, Rebuffe-Scrive M . Regional adipose tissue metabolism in postmenopausal women after treatment with exogenous sex steroids. Horm Metab Res 1990; 22: 345–351.
Pedersen SB, Kristensen K, Hermann PA, Katzenellenbogen JA, Richelsen B . Estrogen controls lipolysis by up-regulating α2A-adrenergic receptors directly in human adipose tissue through the estrogen receptor α. Implications for the female fat distribution. J Clin Endocrinol Metab 2004; 89: 1869–1878.
Heymsfield SB, Gallagher D, Poehlman ET, Wolper C, Nonas K, Nelson D et al. Menopausal changes in body composition and energy expenditure. Exp Gerontol 1994; 29: 377–389.
Ogawa S, Chan J, Gustafsson J-A, Korach KS, Pfaff DW . Estrogen increases locomotor activity in mice through estrogen receptor α: specificity for the type of activity. Endocrinology 2003; 144: 230–239.
Ross R, Janssen I, Dawson J, Kungl AM, Kuk JL, Wong SL et al. Exercise-induced reduction in obesity and insulin resistance in women: a randomized controlled trial. Obes Res 2004; 12: 789–798.
Geiselman PJ, Smith SR . Estrogen's role in the regulation of appetite and body fat. In: Kohlstadt I (ed). Scientific Evidence for Musculoskeletal, Bariatric, and Sports Nutrition. CRC Press, an imprint of Taylor and Francis Group, LLC: Boca Raton, London, and New York, 2006, pp 231–251.
Geiselman PJ, Martin JR, Vanderweele DA, Novin D . Dietary self-selection in cycling and neonatally ovariectomized rats. Appetite 1981; 2: 87–101.
Lovejoy JC, Champagne CM, Smith SR, de Jonge L, Xie H . Ethnic differences in dietary intakes, physical activity, and energy expenditure in middle-aged, premenopausal women: the Healthy Transitions Study. Am J Clin Nutr 2001; 74: 90–95.
Despres JP . The insulin resistance-dyslipidemic syndrome of visceral obesity: effect on patients' risk. Obes Res 1998; 6 (Suppl 1): 8S–17S.
Ryan AS, Nicklas BJ, Berman DM . Hormone replacement therapy, insulin sensitivity, and abdominal obesity in postmenopausal women. Diabetes Care 2002; 25: 127–133.
Wilcox JG, Hwang J, Hodis HN, Sevanian A, Stanczyk FZ, Lobo RA . Cardioprotective effects of individual conjugate equine estrogens through their possible modulation of insulin resistance and oxidation of low-density lipoprotein. Fertil Steril 1997; 67: 57–62.
Spencer CP, Godsland IF, Cooper AJ, Ross D, Whitehead MI, Stevenson JC . Effects of oral and transdermal 17β-estradiol with cyclical oral norethindrone acetate on insulin sensitivity, secretion and elimination in postmenopausal women. Metabolism 2000; 49: 742–747.
O'Sullivan AJ, Ho KKY . A comparison of the effects of oral and transdermal estrogen replacement on insulin sensitivity in postmenopausal women. J Clin Endocrinol Metab 1995; 80: 1783–1788.
Cagnacci A, Soldani R, Carriero PL, Paoletti AM, Fioretti P, Melis GB . Effects of low doses of transdermal 17β-estradiol on carbohydrate metabolism in postmenopausal women. J Clin Endocinol Metab 1992; 74: 1396–1400.
Salpeter SR, Walsh JM, Ormiston TM, Greyber E, Buckley NS, Salpeter EE . Meta-analysis: effect of hormone replacement therapy on components of the metabolic syndrome in postmenopausal women. Diabetes Obes Metab 2006; 8: 538–554.
Wing RR, Matthews KA, Kuller LH, Smith D, Becker D, Plantinga PL et al. Environmental and familial contributions to insulin levels and change in insulin levels in middle-aged women. JAMA 1992; 268: 1890–1895.
Toth MJ, Sites CK, Eltabbakh GH, Poehlman ET . Effect of menopausal status on insulin stimulated glucose disposal. Diabetes Care 2000; 23: 801–806.
Acknowledgements
We thank the study participants and their families for their support during this study. We also thank the staff at the Pennington Biomedical Research Center clinic and the inpatient unit for assistance with all aspects of the study, Mr Tuong Nguyen, BSE, for expert maintenance of the metabolic chambers and the case managers who helped retain so many participants in the study. This study was funded by the National Institutes of Health (DK 2 R01 DK050736). All authors do not have conflicts of interest, including specific financial interests and relationships and affiliations relevant to the subject of this work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lovejoy, J., Champagne, C., de Jonge, L. et al. Increased visceral fat and decreased energy expenditure during the menopausal transition. Int J Obes 32, 949–958 (2008). https://doi.org/10.1038/ijo.2008.25
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2008.25
Keywords
This article is cited by
-
Association of the triglyceride glucose-body mass index with the extent of coronary artery disease in patients with acute coronary syndromes
Cardiovascular Diabetology (2024)
-
Alzheimer’s disease risk reduction in clinical practice: a priority in the emerging field of preventive neurology
Nature Mental Health (2024)
-
Menopause und Sport
Journal für Gynäkologische Endokrinologie/Schweiz (2024)
-
Menopausal Hormone Therapy in Women with Type 2 Diabetes Mellitus: An Updated Review
Diabetes Therapy (2024)
-
Dynamics of serum exosome microRNA profile altered by chemically induced estropause and rescued by estrogen therapy in female mice
GeroScience (2024)