Abstract
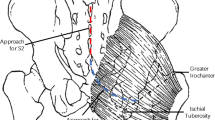
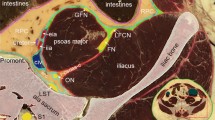
Dissection of the pudendal nerve (PN) and its branches in 71 cadavers revealed anatomic variations not previously described. Knowledge of this variation is necessary to prevent nerve injury resulting in sexual of sensory dysfunction. Because descriptions vary, this study re-evaluated the anatomy of the PN as implicated in perineal procedures in South Africans. The course of the PN from the gluteal region into the perineum was dissected in an adult sample of both sexes and of African and European ancestry. Distances between PN and branches to applicable landmarks were measured. Basic descriptive statistics and comparisons were carried out between groups. In 5/13 African females, the inferior rectal nerve (IRN) entered the gluteal region separately and in 12/13 cases it passed medial to the ischial spine with the PN. The dorsal nerve of the clitoris or penis (DNC/DNP) was closer to the bony frame in those of European ancestry. The IRN branches were more superficial in females, but deeper in males of European ancestry. In African females, a PN block and Richter stitch should be placed more medial. Outside-in transobturator tape procedures might endanger the DNC/DNP in obese individuals. In females of European ancestry the IRN branches are compromised during ischioanal abscess drainage. In males of European ancestry, the dorsal penile nerve block might be less effective. Predictions should be verified clinically.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Barksdale P, Gasser R, Gauthier C, Elkins T, Wall L . Intraligamentous nerves as a potential source of pain after sacrospinous ligament fixation of the vaginal apex. Int Urogynecol J Pelvic Floor Dysfunct 1997; 8: 121–125.
Braverman F Labor pain management In: Vadivelu N, Urman RD, Hines RL (eds) Essentials of Pain Management. Springer: New York, NY, USA, 2006 pp 506.
Cho MK, Kang WD, Kim JW, Kim SM, Kim YH . Complications following outside-in and inside-out transobturator-tape procedures with concomitant gynecologic operations. Chonnam Med J 2011; 47: 165–169.
Rigaud J, Pothin P, Labat JJ, Riant T, Guerineau M, Normand LL et al. Functional results after tape removal for chronic pelvic pain following tension-free vaginal tape or transobturator tape. J Urol 2010; 184: 610–615.
Mahakkanukrauh P, Surin P, Vaidhayakarn P . Anatomical study of the pudendal nerve adjacent to the sacrospinous ligament. Clin Anat 2005; 18: 200–205.
Schraffordt SE, Tjandra JJ, Eizenberg N, Dwyer PL . Anatomy of the pudendal nerve and its terminal branches: a cadaver study. ANZ J Surg 2004; 74: 23–26.
Shafik A, El-Sherif M, Youssef A, Olfat ES . Surgical anatomy of the pudendal nerve and its clinical implications. Clin Anat 1995; 8: 110–115.
Moore KL, Dalley AF . Clinically Orientated Anatomy 5th edn Lippincott Williams and Wilkins: Baltimore, MD, USA, 2006 pp 444.
Nakanishi T . Study on the pudendal nerve, part I: a macroscopical observation of the pudendal nerve in man. Acta Anat Nippon 1967; 42: 223–239.
Takahasi M . [Morphological analysis of the pudendal nerve (author’s transl)]. Kaibogaku Zasshi 1980; 55: 23–44.
Takahashi M, Sato T . Innervation of the anterior perineal muscles and its morphological consideration. Anat Anz 1985; 158: 65–78.
Lazarou G, Grigorescu BA, Olson TR, Downie SA, Powers K, Mikhail MS . Anatomic variations of the pelvic floor nerves adjacent to the sacrospinous ligament: a female cadaver study. Int Urogynecol J 2008; 19: 649–654.
Pirro N, Sielezneff I, Le Corroller T, Ouaissi M, Sastre B, Champsaur P . Surgical anatomy of the extrapelvic part of the pudendal nerve and its applications for clinical practice. Surg Radiol Anat 2009; 31: 769–773.
Robert R, Prat-Pradal D, Labat J, Bensignor M, Raoul S, Rebai R et al. Anatomic basis of chronic perineal pain: role of the pudendal nerve. Surg Radiol Anat 1998; 20: 93–98.
Shafik A, Doss S . Surgical anatomy of the somatic terminal innervation to the anal and urethral sphincters: role in anal and urethral surgery. J Urol 1999; 161: 85–89.
Krissi H, Stanton SL . Bilateral iliococcygeus fixation technicque for enterocele and vaginal vault prolapse repair. Pelviperineology 2010; 29: 11–14.
Uzoma A, Farag K . Vaginal vault prolapse. Obstet Gynecol Int 2009; 2009: 1–9.
Goldberg RP . Sacrospinous ligament suspension using the CapioTM suture capture technique. J Eur Genitourninary Dis 2007; 74–81.
Verdeja AM, Elkins TE, Odoi A, Gasser R, Lamoutte C . Transvaginal sacrospinous colpopexy: anatomic landmarks to be aware of to minimize complications. Am J Obstet Gynecol 1995; 173: 1468–1469.
De Leval J . Novel surgical technique for the treatment of female stress urinary incontinence: transobturator vaginal tape inside-out. Eur Urol 2003; 44: 724–730.
Ulmsten U, Falconer C, Johnson P, Jomaa M, Lanner L, Nilsson C et al. A multicenter study of tension-free vaginal tape (TVT) for surgical treatment of stress urinary incontinence. Int Urogynecol J 1998; 9: 210–213.
Ulmsten U, Hendriksson L, Johnson P, Varhos G . An ambulatory surgical procedure under local anesthesia for treatment for female urinary incontinence. Int Urogynecol J 1996; 7: 81–86.
Sagsoz N, Ersoy M, Kamaci M, Tekdemir I . Anatomical landmarks regarding sacrospinous colpopexy operations performed for vaginal vault prolapse. Euro J Obstet Gynecol Reprod Biol 2002; 101: 74–78.
Delmas V . Anatomical risks of transobturator suburethral tape in the treatment of female stress urinary incontinence. Eur Urol 2005; 48: 793–798.
Delorme E . Transobturator urethral suspension: mini-invasive procedure in the treatment of stress urinary incontinence in women. Prog Urol 2001; 11: 1306.
Dellon AL, Coady D, Harris D . Pelvic pain of pudendal nerve origin: Surgical outcomes and learning curve lessons. J Reconstr Microsurg 2015 1 31: 283–290.
Kessler TM, Burkhard FC, Perimenis P, Danuser H, Thalmann GN, Hochreiter WW et al. Atrempted nerve sparing surgery and age have a significant effect on urinary continence and erectile function after radical cystoprostatectomy and ilial orthotopic bladder substitusion. J Urol 2004; 172: 1323–1327.
Hollabaugh RS, Dmochowski RR, Kneib TG, Steiner MS . Preservation of putative continence nerves during radical retropubic prostatectomy leads to more rapid return of urinary continence. Urol 1998; 51: 960–967.
Tomita R, Igarashi S, Ikeda T, Koshinaga T, Fujisaki S, Tanjoh K . Pudendal nerve terminal motor latency in patients with or without soiling 5 years or more after low anterior resection for lower rectal cancer. World J Surg 2007; 31: 403–408.
Calpista A, Lai S, Agostini A, Mancini M, Artibani W . Functional urological complications after colo-rectal cancer surgery. Pelviperineology 2007; 26: 38–40.
Acknowledgements
We acknowledge Professor PJ Becker from the Medical Research Council of South Africa for data handling and statistical analysis performed. Barbara English from the research office at the University of Pretoria’s Faculty of Health Sciences is acknowledged for her language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
van der Walt, S., Oettlé, A. & Patel, H. Surgical anatomy of the pudendal nerve and its branches in South Africans. Int J Impot Res 27, 128–132 (2015). https://doi.org/10.1038/ijir.2015.10
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijir.2015.10
This article is cited by
-
Electrical stimulation enhances neuronal cell activity mediated by Schwann cell derived exosomes
Scientific Reports (2019)