Abstract
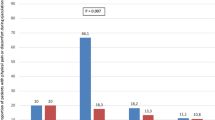
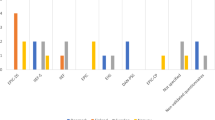
Prostate cancer screening has led to the diagnosis of localized prostate cancer in increasingly young and sexually active men. Accordingly, the impact of cancer treatment on sexual function is gaining more attention. To prospectively evaluate the impact of radical prostatectomy (RP) on male, female and conjugal sexual function. Patients were prospectively assessed by an urologist and a sexologist before and 6 months after robot-assisted laparoscopic RP (RALP). RALP was performed with uni- or bilateral neurovascular bundle preservation by a single surgeon. Postoperatively, all patients were prescribed tadalafil 20 mg, 3 times a week during 6 months. Male and female sexual functions were evaluated by using the International Index of Erectile Function (IIEF-5), the Female Sexual Function Index (FSFI) and the Lock-Wallace Marital Adjustment Test (MAT). Continuous variables were analyzed with rank-sum and t-tests, as needed, and categorical variables with chi-squared tests. All tests were two-sided, with a P-value⩽0.05 considered significant. Twenty-one couples were included. Mean patient male and female age was 62.4 and 60.7 years, respectively. Bilateral nerve sparing was performed in 12/21 (57%) patients. Median preoperative IIEF-5 was 20/25, corresponding to mild erectile dysfunction (ED). Median preoperative FSFI and MAT were both within normal range (28/36 and 114/158, respectively). Six months following surgery, both IIEF-5 (11/25) and FSFI (25/36) had significantly dropped (P=0.007 and 0.003, respectively). Postoperative decreases in IIEF-5 and FSFI scores were associated within couples. MAT scores (115/158), however, remained unaffected by RALP, showing an unmodified relationship satisfaction postoperatively. Finally, bilateral nerve sparing surgery preserved not only male but also female sexual function. This study shows that the expected short-term post-RALP ED is associated with a worsening of female sexual function, whereas nerve sparing surgery has a protective effect on both the patient’s and his partner’s sexual function with a significant effect of bilateral over unilateral neurovascular bundle preservation. Furthermore, we found that conjugal complicity remains stable throughout the first semestrial postoperative period despite the decrease in sexual function.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Sanders S, Pedro LW, Bantum EO, Galbraith ME . Couples surviving prostate cancer: Long-term intimacy needs and concerns following treatment. Clin J Oncol Nurs 2006; 10: 503–508.
Street AF, Couper JW, Love AW, Bloch S, Kissane DW, Street BC . Psychosocial adaptation in female partners of men with prostate cancer. Eur J Cancer Care (Engl) 2010; 19: 234–242.
Kaul S, Savera A, Badani K, Fumo M, Bhandari A, Menon M . Functional outcomes and oncological efficacy of Vattikuti Institute prostatectomy with Veil of Aphrodite nerve-sparing: an analysis of 154 consecutive patients. BJU Int 2006; 97: 467–472.
Ahlering TE, Skarecky D, Borin J . Impact of cautery versus cautery-free preservation of neurovascular bundles on early return of potency. J Endourol 2006; 20: 586–589.
Crowe H, Costello AJ . Prostate cancer: perspectives on quality of life and impact of treatment on patients and their partners. Urol Nurs 2003; 23: 279–285.
Rosen RC, Cappelleri JC, Smith MD, Lipsky J, Peña BM . Development and evaluation of an abridged, 5-item version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile dysfunction. Int J Impot Res 1999; 11: 319–326.
Wiegel M, Meston C, Rosen R . The female sexual function index (FSFI): cross-validation and development of clinical cutoff scores. J Sex Marital Ther 2005; 31: 1–20.
Birchler GR, Weiss RL, Vincent JP . Multimethod analysis of social reinforcement exchange between maritally distressed and nondistressed spouse and stranger dyads. Journal of Personality and Social Psychology 1975; 31: 349–360.
Birchler GR, Webb LJ . Discriminating interaction behaviors in happy and unhappy marriages. J Consult Clin Psychol 1977; 45: 494–495.
Vincent JP, Weiss Rl, Birchler GR . A behavioral analysis of problem solving in distressed and nondistressed married and stranger dyads. Behavior Therapy 1975; 6: 475–487.
Coelho RF, Palmer KJ, Rocco B, Moniz RR, Chauhan S, Orvieto MA et al. Early complication rates in a single-surgeon series of 2500 robotic-assisted radical prostatectomies: report applying a standardized grading system. Eur Urol 2010; 57: 945–952.
Deho F, Gallina A, Salonia A, Briganti A, Suardi N, Zanni G et al. Prophylaxis of erectile function after radical prostatectomy with phosphodiesterase type 5 inhibitors. Curr Pharm Des 2009; 15: 3496–3501.
Lee DJ, Cheetham P, Badani KK . Penile rehabilitation protocol after robot-assisted radical prostatectomy: assessment of compliance with phosphodiesterase type 5 inhibitor therapy and effect on early potency. BJU Int 2010; 105: 382–388.
Glickman L, Godoy G, Lepor H . Changes in continence and erectile function between 2 and 4 years after radical prostatectomy. J Urol 2009; 181: 731–735.
Shindel A, Quayle S, Yan Y, Husain A, Naughton C . Sexual dysfunction in female partners of men who have undergone radical prostatectomy correlates with sexual dysfunction of the male partner. J Sex Med 2005; 2: 833–841.
Tsivian M, Mayes JM, Krupski TL, Mouraviev V, Donatucci CF, Polascik TJ . Altered male physiologic function after surgery for prostate cancer: couple perspective. Int Braz J Urol 2009; 35: 673–682.
Johansson E, Steineck G, Holmberg L, Johansson JE, Nyberg T, Ruutu M et al. Long-term quality-of-life outcomes after radical prostatectomy or watchful waiting: the Scandinavian Prostate Cancer Group-4 randomised trial. Lancet Oncol 2011; 12: 891–899.
Abbani F, Schiff J, Piecuch M, Yunis LH, Eastham JA, Scardino PT et al. Time course of recovery of erectile function after radical retropubic prostatectomy: does anyone recover after 2 years? J Sex Med 2010; 7: 3984–3990.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Tran, SN., Wirth, G., Mayor, G. et al. Prospective evaluation of early postoperative male and female sexual function after radical prostatectomy with erectile nerves preservation. Int J Impot Res 27, 69–74 (2015). https://doi.org/10.1038/ijir.2014.36
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijir.2014.36
This article is cited by
-
Psychosocial contributors to patients’ and partners’ postprostate cancer sexual recovery: 10 evidence-based and practical considerations
International Journal of Impotence Research (2021)
-
Erectile dysfunction
Nature Reviews Disease Primers (2016)