Abstract
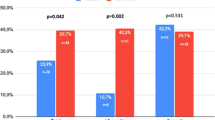
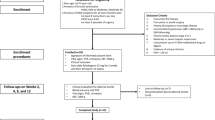
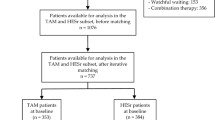
Saffron (Crocus sativus Linn.) have been perceived by the public as a strong aphrodisiac herbal product. However, studies addressing the potential beneficial effects of saffron on erectile function (EF) in men with ED are lacking. Our aim was to evaluate the efficacy and safety of saffron administration on EF in men with ED. After a 4-week baseline assessment, 346 men with ED (mean age 46.6±8.4 years) were randomized to receive on-demand sildenafil for 12 weeks followed by 30 mg saffron twice daily for another 12 weeks or vice versa, separated by a 2-week washout period. To determine the type of ED, penile color duplex Doppler ultrasonography before and after intracavernosal injection with 20 μg prostaglandin E1, pudendal nerve conduction tests and impaired sensory-evoked potential studies were performed. Subjects were assessed with an International Index of Erectile Function (IIEF) questionnaire, Sexual Encounter Profile (SEP) diary questions, patient and partner versions of the Erectile Dysfunction Inventory of Treatment Satisfaction (EDITS) questionnaire and the Global Efficacy Question (GEQ) ‘Has the medication you have been taking improved your erections?’ No significant improvements were observed with regard to the IIEF sexual function domains, SEP questions and EDITS scores with saffron administration. The mean changes from baseline values in IIEF-EF domain were +87.6% and +9.8% in sildenafil and placebo groups, respectively (P=0.08). We did not observe any improvement in 15 individual IIEF questions in patients while taking saffron. Treatment satisfaction as assessed by partner versions of EDITS was found to be very low in saffron patients (72.4 vs 25.4, P=0.001). Mean per patient ‘yes’ responses to GEQ was 91.2 and 4.2% for sildenafil and saffron, respectively (P=0.0001). These findings do not support a beneficial effect of saffron administration in men with ED.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
NIH Consensus Conference Impotence NIH Consensus Development Panel on Impotence. JAMA 1993; 270: 83–90.
Tiefer L . The medicalization of impotence: normalizing phallocentrism. Gend Soc 1994; 8: 363–377.
Moyad M . Dietary supplements and other alternative medicines for erectile dysfunction. What do I tell my patients? Urol Clin N Am 2002; 29: 11–22.
Rios JL, Recio MC, Giner RM, Manez S . An update review of saffron and its active compounds. Phytotherap Res 1996; 10: 189–193.
Fernandez JA . Biology, biotechnology and biomedicine of saffron. Recent Res Develop Plant Sci 2004; 2: 127–159.
Negbi M . Saffron cultivation: Past, present and future prospects. In: M Negbi (ed.). Saffron Crocus sativus L. Harwood Academic Publishers: Amsterdam, 1999, pp 1–17.
Carmona M, Zalacain A, Sanchez AM, Novella JL, Alonso GL . Crocetin esters, picrocrocin and its related compounds present in Crocus sativus stigmas and Gardenia jasminoides fruits.Tentative identification of seven new compounds by LC-ESI-MS. J Agric Food Chem 2006; 54: 973–979.
Lozano P, Castellar MR, Simancas MJ, Iborra JL . Quantitative high performance liquid chromatographic method to analyse commercial saffron (Crocus sativus L.) products. J Chromatogr A 1999; 830: 477–483.
Abdullaev FI . Cancer chemopreventive and tumoricidal properties of saffron (Crocus sativus). Exp Biol Med 2002; 227: 20–25.
Verma SK, Bordia A . Antioxidant property of saffron in man. Ind J Med Sci 1998; 52: 205–207.
Abdullaev FI, Espinosa-Aguirre JJ . Biomedical properties of saffron and its potential use in cancer therapy and chemoprevention trials. Cancer Detect Pre 2004; 28: 426–432.
Madan CL, Kapur BM, Gupta US . Saffron. Econ Bot 1966; 20: 377.
Hosseinzadeh H, Ziaee T, Sadeghi A . The effect of saffron, Crocus sativus stigma, extract and its constituents, safranal and crocin on sexual behaviors in normal male rats. Phytomedicine 2008; 15: 491–495.
Shamsa A, Hosseinzadeh H, Molaei M, Shakeri MT, Rajabi O . Evaluation of Crocus sativus L (saffron) on male erectile dysfunction: a pilot study. Phytomedicine 2009; 16: 690–693.
Akhondzadeh S, Tahmacebi-Pour N, Noorbala AA, Amini H, Fallah-Pour H et al. Crocus sativus L in the treatment of mild to moderate depression: a double-blind, randomized and placebo-controlled trial. Phytother Res 2005; 19: 148–151.
Rosen RC, Riley A, Wagner G, Osterloh H, Kirkpatrick J, Mishra A . The International Index of Erectile Function (IIEF): a multidimensional scale for the assessment of erectile dysfunction. Urology 1997; 49: 822–829.
Cappelleri JC, Rosen RC, Smith MD, Mishra A, Osterloh IH . Diagnostic evaluation of the erectile function domain of the International Index of Erectile Function. Urology 1999; 54: 346–351.
Althof SE, Corty EW, Levine SB, Levine F, Burnett AL, McVary K et al. EDITS: development of questionnaires for evaluating satisfaction with treatment for erectile dysfunction. Urology 1999; 53: 793–799.
Adimoelja A . Phytochemicals and the breakthrough of traditional herbs in the management of sexual dysfunction. Int J Androl 2000; 23: 82–84.
Montorsi F, Althof SE . Partner responses to sildenafil citrate (Viagra) treatment of erectile dysfunction. Urology 2004; 63: 762–766.
Cherdshewasart W, Nimsakul N . Clinical trial of Butea Superba, an alternative herbal treatment for erectile dysfunction. Asian J Androl 2003; 5: 243–246.
Jordan SA, Cunningham DG, Marles RJ . Assessment of herbal medicinal products: Challenges, and opportunities to increase the knowledge base for safety assessment. Toxicol Appl Pharmacol 2009; e-pub ahead of print 16 December 2009.
Souverein PC, Egberts AC, Meuleman EJ, Urquhart J, Leufkens HG . Incidence determinants of sildenafil (dis) continuation: the Dutch cohort of sildenafil users. Int J Impot Res 2002; 14: 256–259.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflicts of interest.
Rights and permissions
About this article
Cite this article
Safarinejad, M., Shafiei, N. & Safarinejad, S. An open label, randomized, fixed-dose, crossover study comparing efficacy and safety of sildenafil citrate and saffron (Crocus sativus Linn.) for treating erectile dysfunction in men naïve to treatment. Int J Impot Res 22, 240–250 (2010). https://doi.org/10.1038/ijir.2010.10
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijir.2010.10
Keywords
This article is cited by
-
Toxicology of natural and synthetic aphrodisiacs
Rechtsmedizin (2020)
-
The effects of crocin on psychological parameters in patients under methadone maintenance treatment: a randomized clinical trial
Substance Abuse Treatment, Prevention, and Policy (2019)
-
Herbal Dietary Supplements for Erectile Dysfunction: A Systematic Review and Meta-Analysis
Drugs (2018)